Continuing Education Activity
Plantar heel pain is a pervasive issue that afflicts numerous adults and significantly hampers their quality of life. With diverse causative factors, ranging from common plantar fasciitis to more complex etiologies such as S1 radiculopathy and seronegative spondyloarthropathies, this activity comprehensively explores the condition. This condition underscores the pivotal role of an interprofessional team in recognizing and managing plantar heel pain effectively. The program facilitates a practical approach to identifying the underlying cause through comprehensive history-taking and physical examination, which form the foundation of accurate diagnosis. The activity discusses evidence-based management strategies, encompassing lifestyle modifications, nonsteroidal anti-inflammatory drugs, rehabilitation, local injections, and surgical interventions. By participating in this activity, learners will be better prepared to address the challenges posed by plantar heel pain and improve patient outcomes through a comprehensive and interdisciplinary approach.
Objectives:
Apply lifestyle modifications, non-steroidal anti-inflammatory drugs, rehabilitation, local injections, and surgical interventions as appropriate.
Evaluate the effectiveness of selected management strategies through ongoing assessment.
Recognize common conditions such as plantar fasciitis and complex etiologies like S1 radiculopathy and seronegative spondyloarthropathies.
Identify interprofessional team strategies to improve care coordination and communication to enhance outcomes for patients affected by plantar heel pain.
Introduction
As a common problem among adults, plantar heel pain can lead to significant disability and impairment of activities of daily living. Plantar heel pain can be due to local causes, which include plantar fasciitis, referred causes like S1 radiculopathy or systemic illnesses, such as seronegative spondyloarthropathies. The most common causes of plantar heel pain are plantar fasciitis, heel fat pad atrophy, calcaneal stress fracture, or entrapment of the tibial nerve, medial calcaneal nerve, or the first branch of the lateral plantar nerve (Baxter nerve). History taking and physical examination are crucial for correct diagnosis. Laboratory studies can help diagnose systemic causes of plantar heel pain. Plain radiographs and computed tomography can confirm the diagnosis of the stress fractures of the calcaneus and bone tumors. High-resolution ultrasound confirms the diagnosis of plantar fasciitis, heel fat pad atrophy, or entrapment neuropathies. Electrophysiological studies are required to investigate neurogenic causes of plantar heel pain. Magnetic resonance imaging can also help diagnose soft tissue pathologies and may be better than ultrasound for investigating bony disorders. Treatments include lifestyle modification, non-steroidal anti-inflammatory drugs, rehabilitation, local injection, and surgery.[1][2][3]
Etiology
Local Causes
- Mechanical: Plantar fasciitis
- Traumatic: Calcaneal stress fractures
- Neurologic: Entrapment of the tibial nerve (posterior tarsal tunnel syndrome), medial calcaneal nerve, and Baxter nerve
- Other: Tumors, osteomyelitis, plantar warts, or plantar heel fat pad atrophy
Referred Causes
Systemic Causes
- Rheumatoid arthritis
- Seronegative spondyloarthropathies
Risk Factors
- Obesity
- Prolonged standing
- Inappropriate footwear
Epidemiology
In the United States, people visit the physician more than 1 million times yearly because of plantar heel pain.[4] Patients include athletes and sedentary individuals. Men and Women are affected equally. The most frequent cause of plantar heel pain is plantar fasciitis, affecting approximately 2 million Americans each year.[4]This condition affects almost 10% of the population over a lifetime.[5] Calcaneal stress fractures account for 20% of lower extremity stress fractures in 109,296 soldiers, reported from a 4-year study conducted by Pester et al, 16% of patients with heel pain have a systemic illness like rheumatoid arthritis. The estimated prevalence of neurogenic causes of plantar heel pain is unclear.[6]
Pathophysiology
Plantar Fasciitis
The plantar fascia (plantar aponeurosis) includes medial, central, and lateral bands that extend across the forefoot into the calcaneus.[7] Repetitive microtrauma is the classic cause of plantar fasciitis and can be exacerbated by obesity, prolonged standing, pes planus, soleus-gastrocnemius complex dysfunction, and ankle instability.[8] The windlass mechanism describes how, when under tension, the plantar fascia pulls the midtarsal bones together into a stable, longitudinal arch that locks the midfoot and supports the axial load. Failure of this relationship, from repetitive microtrauma or excessive load, can result in a collapsed arch and variable foot pain.[9] Furthermore, aging leads to a reduction in the elasticity of the plantar fascia.[4] These factors may contribute to the progressive degeneration of the soft tissue and failure of the windlass mechanism.
Heel Fat Pad Atrophy
The heel pad comprises closely packed fat chambers surrounded by tough circular or cone-shaped collagenous septa and elastin fibers. Reduction in fat chambers may be due to micro-trauma or repeated corticosteroid injections leading to decreased shock-absorbing properties and the development of pain.[10] A decrease in the height of the fat pad may contribute to heel pain.[11][8]
Calcaneal Stress Fractures
Normal weight-bearing stress is less than the threshold to cause a calcaneal fracture. Stress fractures are most commonly found posterior and inferior to the posterior facet of the subtalar joint.[12] Patients with osteopenia or who play a sport with repetitive jumping or running are at higher risk for this injury.[13] Abnormal mechanical stress results in inadequate bone healing, osteoclast activation, and thus stress fracture. Other relevant factors include starting a new activity (running) and increased intensity or duration of previous activities (prolonged running and standing), obesity, inappropriate footwear, flat feet, and rheumatoid arthritis.[14] Aside from mechanical load, intrinsic factors of bone secondary to bone tumors (Ewing sarcoma) or metastatic disease (endometrial adenocarcinoma, bronchogenic carcinoma, bladder cancer, and gastric cancer) can result in a pathologic calcaneal fracture.[13]
Entrapment Neuropathies
Tarsal tunnel syndrome is due to the entrapment of the tibial nerve underneath the flexor retinaculum on the medial side of the ankle. Entrapment may be due to direct nerve compression from any space-occupying lesion, including an accessory flexor digitorum longus, a soft tissue mass such as a ganglion cyst, or fibrous scar tissue from prior surgery.[15] The cause may be more elusive and result from systemic inflammation in diabetes mellitus and rheumatoid arthritis or be idiopathic.[16]
The medial calcaneal nerve commonly arises from the tibial nerve above the level of the flexor retinaculum of the ankle. This nerve carries sensory information from the skin over the plantar surface of the calcaneus and subcutaneous fat. The entrapment of this nerve might be due to tight fascia, varicosities, or scars from previous surgical procedures.
The Baxter nerve is the first branch of the lateral plantar nerve. This nerve provides motor innervation to the quadratus plantae, flexor digitorum brevis, and abductor digiti minimi muscles. This nerve also carries sensory information from the calcaneal periosteum and the long plantar ligament. Baxter nerve can be entrapped distally due to tight fascial planes, muscle hypertrophy, or compression secondary to foot biomechanics.[17]
History and Physical
Plantar Fasciitis
Patients typically complain of heel pain accompanying the first steps after getting up in the morning. Others report heel pain after standing for a prolonged time in a sitting position (ie, sitting at a desk or in a car). In long-standing cases, the pain might persist throughout walking and rest.[7] Tenderness is usually elicited inferiorly over the medial calcaneal tubercle.
Heel Fat Pad Atrophy
Patients present with diffuse central plantar heel pain often precipitated by barefoot walking on hard surfaces. Tenderness can be elicited on the central part of the calcaneus. Calcaneal fat pad height seen on lateral radiographs or sagittal magnetic resonance imaging views may support this diagnosis.[8]
Calcaneal Stress Fractures
Patients present with diffuse heel pain and a positive squeeze test (tenderness on medial and lateral compression of the calcaneus). Pain will worsen with activity and, without treatment, may progress to pain at rest.[18] Significant bruising is often seen pooling at the lateral foot or across the bottom of the arch.
Tarsal Tunnel Syndrome/Tibial Nerve Entrapment
A biomechanical exam with attention to hindfoot position and alignment is key for this diagnosis, as rearfoot varus or valgus foot position may contribute to tibial nerve compression. Patients often present with pain along the inside of the ankle or arch and may have tingling or paresthesia along the plantar surface of the foot. Suppose deliberate tapping along the course of the tibial nerve elicits tingling or pain in the foot. In that case, this is a positive Tinel sign and a strong suggestion of tarsal tunnel entrapment. Reproducing nerve compression can also be done by placing the foot in maximum dorsiflexion and eversion or maximum plantar flexion and inversion (Phalen test) and holding this for 10 seconds. Numbness or pain with either of these positions supports the diagnosis of tarsal tunnel syndrome.[17]
Medial Calcaneal Nerve Entrapment
The medial plantar nerve branches from the tibial nerve just beyond the tarsal tunnel and courses deep to the abductor hallucis muscle.[19] Diagnosis of this nerve entrapment may be challenging due to variation in branching patterns (bifurcation occurs before the tarsal tunnel in 5% of patients), but compression of this nerve will typically cause heel pain at the anterior medial portion of the heel.[17] Patients will present with burning pain and paresthesia on the skin over the calcaneus. Pain does not radiate distally as in cases of the entrapment of the tibial nerve or Baxter nerve. Tinel sign might be positive but localized to the medial surface of the calcaneal bone.
Baxter Nerve Entrapment
As the first branch of the lateral plantar nerve, the Baxter nerve lies deep to the abductor hallucis and flexor digitorum brevis muscles and superficial to the quadratus plantae.[19] Compression of this nerve is often found just anterior to the medial calcaneal tuberosity or at the deep margin of the abductor hallucis muscle due to a tight fascial plane.[20] Patients often have sharp, radiating pain along the Baxter nerve. Pain is worse after activities (ie, walking) and at night. A positive Tinel sign and maximal tenderness of nerve entrapment can be elicited at the two points mentioned above. As discussed above, examining these nerve entrapments should include a biomechanical exam to evaluate the contribution of hindfoot varus/valgus position, equinus, or pes planus.
S1 Radiculopathy
Patients with heel pain may have a history of chronic lower back pain. Clinically, radicular involvement will present as pain and numbness radiating from the lower back down to the heel of the foot. Patients may have decreased sensation over the skin of the sole, heel, or lateral foot and weakness of the gastrocnemius, gluteus maximus, hamstring, peroneal, and foot muscles with a diminished ankle reflex. Perform the positive straight leg raise test (Lasègue test) with the patient in the supine position. Pain with passive hip flexion while lifting the leg suggests stretching the lower lumbar and sacral roots.[21] Perform a crossed straight leg raise test, eliciting pain on the contralateral side with the same motion. Results from new studies suggest that these exams may not be as reliable as we once thought.[22]
Systemic Causes
Screen for symmetric or asymmetric polyarthritis, uveitis, psoriasis, lower gastrointestinal symptoms, enthesitis, balanitis, dactylitis, sacroiliitis, and spondylitis.
Evaluation
Most heel pain causes can be diagnosed clinically.[23][24][25][26]
Laboratory
The laboratory tests include acute phase reactants, rheumatoid factor, anti-cyclic citrullinated peptide antibodies, and HLA-B27 for systemic causes of plantar heel pain.
Plain Radiographs and Computed Tomography
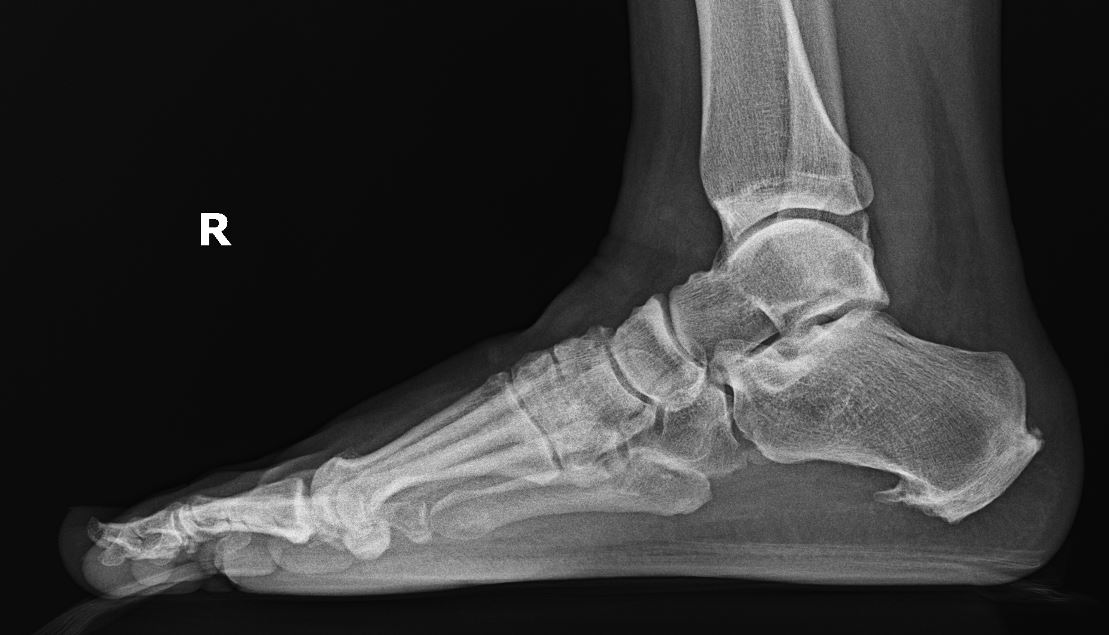
Radiographs are best used to evaluate bony changes such as plantar calcaneal spurs, tumors, bone cysts, or stress fractures (see Image. Plantar Heel Pain). Plantar heel spurs seen on imaging suggest that a tight plantar fascia has been present for at least 6 to 12 months, regardless of clinical symptoms.[8] Spurs are present in 45% to 85% of patients with plantar fasciitis.[27] Over 15% of the general population has a radiologically asymptomatic spur.[28] Even with a clinical exam and radiographs, computed tomography imaging may be helpful when a diagnosis is unclear.
Musculoskeletal Ultrasound
Ultrasound can be a powerful tool for differentiating the root cause of heel pain in the office. If the plantar fascia is measured as greater than 4 mm at its insertion onto the medial calcaneal tuberosity with associated pain, this supports a diagnosis of plantar fasciitis.[29] An increase in vascularity under power Doppler ultrasound is not a common finding in plantar fasciitis. A diagnosis of heel fat pad atrophy can be more nuanced. Results from studies have found that a healthy heel fat pad thickness can range from 12 mm to 28 mm.[30] Literature supporting a definitive measurement for fat pad atrophy is sparse. Some studies have referenced measurements as low as 3 mm.[31] Since heel fat pad-related pain is often the result of a loss in elasticity, US imaging comparing weight-bearing versus non-weight-bearing measurements of fat pad height should be taken.[10] Ultrasound can also detect sub-entheseal erosions, enthesitis, and enthesophytes at the plantar fascia's attachment to the calcaneus, which are suggestive of spondyloarthropathy.
For patients with nonspecific nerve pain or paresthesia, ultrasound can be used to visualize the size of nerves. The cross-sectional area of the tibial nerve is roughly 11 to 13 mm2 at the superior posterior medial malleolus.[32][33] A study by Fanino et al in France found that a tibial nerve size of 15 mm2 had a 74% sensitivity and 100% specificity for diagnosing tarsal tunnel syndrome. The medial calcaneal and Baxter nerves are roughly 3 mm and 2 mm, respectively. To confirm the diagnosis of the medial calcaneal and Baxter nerve entrapment, clinicians should compare the symptomatic side with the asymptomatic side or perform ultrasound-guided diagnostic blocks. Reduced muscle size in the quadratus plantae, flexor digitorum brevis, or abductor digiti minimi may also support a diagnosis of Baxter nerve entrapment. Ultrasound may also rule out nerve entrapment secondary to mass effect from a soft tissue lesion or ganglion cyst.[17]
General ultrasound criteria for entrapment neuropathies include
- The cross-sectional area is more than 2 standard deviations above the mean reference value
- Change in the echotexture of the affected nerve, like being hypoechoic
- Notching and flattening of the nerve at the entrapment site
- Change in the fascicle size (enlargement of fascicles within the affected nerve)
Despite ultrasound's ability to evaluate several factors that may contribute to heel pain, the 2014 Clinical Practice Guidelines do not recommend using ultrasound for individuals with heel pain or plantar fasciitis due to a low level of supporting evidence.[34]
Electrophysiologic Studies
Electromyographic studies and nerve conduction velocities can help rule in the specific location of nerve entrapment and rule out differentials such as peripheral neuropathy and lumbosacral radiculopathy.[17] However, they have poor diagnostic sensitivity, and a thorough history and physical may be more reliable.[16]
Magnetic Resonance Imaging
Magnetic resonance imaging (MRI) is often the next best imaging modality for evaluating the surrounding soft tissue structures when radiographs are negative. MRI helps to visualize and assess the thickening of the fascia, nerve entrapment, soft tissue masses, infection, bony tumors, or muscle/fat atrophy.[13] MRI may reveal bone marrow edema associated with a calcaneal stress fracture when radiographs are negative in a positive calcaneal squeeze test setting.[14]
Treatment / Management
Plantar Fasciitis
The first-line treatment for plantar fasciitis should be conservative. The following components of care are a combined summary of the recommendations made by the 2010 Clinical Practice Guideline from the Journal of Foot and Ankle Surgery and the 2014 Clinical Guidelines from The Orthopedic Section of the American Physical Therapy Association.[34][8] There are no recent updates to these guidelines. Treatment should always target the primary cause of heel pain (neurologic, arthritic, mechanical, traumatic, or other).
Initial Therapy - for 6 weeks
- Manual therapy or soft tissue massage may improve soft tissue flexibility or joint mobility.
- Gastroc/soleus muscle and plantar fascia stretching may relieve pain between 1 week and 4 months. There is no recommendation on how long or how often.
- Low-dye or calcaneal taping may provide up to 3 weeks of temporary pain relief, and elastic therapeutic taping may reduce pain in the gastroc-soleus complex and fascia for 1 week.
- Custom or prefabricated orthotics can improve pain for as little as 2 weeks but do not provide significant benefits after 1 year. People who respond well to taping often have the best outcomes with orthotics.
- The best shoes for plantar fasciitis have a rocker bottom sole and should be combined with an orthosis. Patients may also benefit from shoe-style rotation throughout the week.
- These should be combined with cryotherapy, oral anti-inflammatories, limitations to provoking activity, avoidance of barefoot walking, and weight loss consultation.
Tier 2 Therapies - for 6 months
- For patients with persistent pain first thing in the morning, a night splint should be used every night for 1 to 3 months.
- Corticosteroid injections are not superior to conservative options as a first-line therapy.
- Physical therapy may help keep patients on a schedule or provide more targeted therapy.
- Electrotherapy (iontophoresis) may provide 2 to 4 weeks of pain relief but should not be performed until failure of the treatments as mentioned above.
- Low-level laser therapy and phonophoresis may provide some pain relief.
- Ultrasonic therapy is not recommended.
- Dry needling is not recommended.
Tier 3 Therapies
- Extracorporeal shockwave therapy does not have superior outcomes to the above-mentioned conservative options and comes with more significant risks.
- Consider surgery for plantar fasciotomy with or without heel spur resection at this time.
- These reviews did not discuss autologous blood-derived products such as platelet-rich plasma.
Surgery is indicated for patients who have failed at least 6 months of conservative care.[13] Intervention includes releasing the medial and central bands of the plantar fascia, which can be done with an open incision or by endoscopy. Endoscopy is favored due to the small incision and relatively quick return to work. An open incision allows for better visualization of the fascial release and access to the plantar calcaneal spur. However, results from studies show that spur removal does not correlate with more successful surgical outcomes.[8] Gastrocnemius contracture has been associated with a tight plantar fascia, and select patients may also benefit from a gastrocnemius recession.[13]
Heel Fat Pad Atrophy
Treatment for heel fat pad atrophy is focused on relieving symptoms. Recommend first-line pain treatment for heel fat pad atrophy, including rest, ice, nonsteroidal anti-inflammatory drugs, silicone heel cups, low-dye arch taping, cushioned and supportive footwear, and avoidance of high-impact activities.[31] Using a cup-shaped silicone heel has been found to provide the most relief.[10] There is limited evidence or reports on the use of platelet-rich plasma injections or surgery. Nevertheless, only consider these as a last-line option.
Calcaneal Stress Fractures
Conservative care is the current protocol for calcaneal stress fracture management. Patients should stop the activity and be placed in a non-weight-bearing, controlled ankle motion boot for at least 4 weeks. They may then transition to partial weight bearing over the next 4 weeks and slowly return to full weight bearing and light exercise. Nonsteriod and cryotherapy may aid with swelling and pain control. Labs and vitamin D supplementation should be considered for patients with delayed healing. Surgery should only be considered after failed conservative care.[12]
Entrapment Neuropathies
Nonsteroidal anti-inflammatory drugs and anticonvulsants can help reduce symptoms. Non-responders can benefit from ultrasound-guided corticosteroid injection, hydro dissection using dextrose 5%, radiofrequency, or cryoablation. Recalcitrant cases or severe cases might need surgical decompression.[17] Surgical tarsal tunnel release decompresses the entire tibial nerve and its branches through an open incision or a minimally invasive technique.[35] Ultrasound guidance in the operating room can help localize the nerve and avoid extensive dissection, which is invaluable for vascular or diabetic patients.[16] An endoscopic release is an option for these patients. Few studies have looked into using pulsed radiofrequency for treatment, but there has yet to be a consensus on this therapy.
Differential Diagnosis
Differential diagnoses to consider include the following:
Prognosis
Plantar fasciitis has a positive long-term prognosis.[36] Results from studies have found that the average duration of chronic heel pain can persist for just over one year. However, up to 90% of patients will recover with conservative care.[34][7] Patients with heel fat pad atrophy often have the most significant improvement with a simple silicone heel cup; in contrast, patients who undergo surgery may experience residual pain from scarring.[10] Tarsal tunnel syndrome is a more challenging pathology due to its often idiopathic nature and insidious progression of symptoms.[17] Patient outcomes optimize when the cause or location of entrapment can be clearly identified. The prognosis for a calcaneal stress fracture is favorable, with most patients recovering with activity modification and a period of immobilization.[14]
Complications
Conservative treatment options for heel pain have resulted in minimal reported complications. Corticosteroid injection poses a mild risk of fat pad atrophy or plantar fascia rupture due to the local reaction of steroids with soft tissue.[37] Complications after a plantar fascia release may include insufficient fascia release, poor hemostasis, or nerve damage. Complications after a tarsal tunnel release may be related to an inaccurate diagnosis, incomplete release, neuroma formation, poor technique, poor hemostasis, or intrinsic nerve damage.[35] In this case, an extensile tarsal tunnel release with or without autogenous vein or collagen nerve wrapping may be performed.[35] If a calcaneal stress fracture fails to heal, patients should be medically optimized. Surgical repair may include drilling of the fracture site with or without graft. Surgery carries the most significant risk of any treatment, which includes swelling, pain, infection, bleeding, nerve damage, wound dehiscence, over or under-correction, need for further surgery, or blood clots.
Postoperative and Rehabilitation Care
Reserve surgery for patients who have exhausted all conservative options. Modify postoperative and rehabilitation protocols for the specific procedure and patient goals. Remove sutures routinely at 2 weeks unless delayed healing signs or patient comorbidities might impede recovery. In the case of revision surgery, patients may be non-weight-bearing for up to 4 weeks.[35] Physical therapy is recommended to reduce swelling and pain and improve postoperative strength and proprioception.
Consultations
For patients who have not improved with first-line therapy for heel pain, referral should be considered. Patients with neurologic heel pain should be referred to a pain management and rehabilitation physician or a neurologist for an electromyography or a nerve conduction velocity exam.[8] Although rare, a tumor found on advanced imaging warrants a referral to oncology. Clinicians can assist with exercise and diet counseling to maintain a healthy weight.[34] For recurrent joint pain or unimproved pain with conservative care in the setting of a family history of rheumatologic disease, there should be a low threshold for referral to a rheumatologist.
Deterrence and Patient Education
Patient education is one of the mainstays of treatment. The primary cause of each patient’s pain, the impact of comorbidities (ie, weight gain), the prognosis, and the value of self-management should be thoroughly discussed to set realistic expectations about recovery. Patients who understand the primary pain driver and the meaning of pain throughout their recovery may be more inclined to commit to conservative protocols.[36]
Plantar fasciitis, also sometimes called heel spur syndrome, is often the leading cause of heel pain. Causes of heel pain include unsupportive footwear, overuse such as prolonged standing, and flat feet. Typical symptoms of heel pain include discomfort when taking the initial step out of bed in the morning or upon standing after an extended rest period. Podiatrists typically order radiographs of the feet to diagnose and distinguish different types of heel pain. Treatment can include surgical and non-surgical methods. Non-surgical treatments include physical therapy, medications, injections, splints, and arch supports. Treatment can include surgery and non-surgical methods (eg, physical therapy, medications, injections, splints, and arch supports).
Pearls and Other Issues
Key facts to keep in mind when considering plantar heel pain include the following:
- The plantar calcaneal spurs are not a common cause of plantar heel pain. Spurs are present in 50% of patients with plantar fasciitis. Over 15% of the general population has a radiologically asymptomatic spur.
- Repeated corticosteroid injection to treat plantar fasciitis can lead to heel fat pad atrophy and rupture of the plantar fascia due to attenuation.
- Clinicians should treat the underlying cause of the plantar fasciitis, such as flat feet and ankle instability; otherwise, symptoms will recur.
Enhancing Healthcare Team Outcomes
Heel pain includes a wide range of differential diagnoses, which may be as simple as a biomechanical malalignment or as complex as neurologic insufficiency secondary to a rheumatologic disease. Diagnosis requires a thorough history and physical exam to evaluate the true source of pain, and treatment may require coordination between several different medical specialties. Improving understanding of promptly evaluating and treating this condition is crucial for achieving better patient outcomes.
With over 1 million patient visits yearly for heel pain, proper diagnosis and management can impact many patients’ quality of life. Long-term physical effects can include recurrent symptoms, diminished activity, challenges performing physical labor, or a lassitude for performing activities of daily living. Healthcare practitioners should thoroughly counsel patients with heel pain so that they can make informed decisions about their treatment.
Practitioners should recognize that further evaluation is warranted when patients fail the initial 6 weeks of conservative therapy. This may include advanced imaging, more invasive treatment therapies, medical optimization by their clinician, or referral to a physical therapist, neurologist, pain management and rehab specialist, or rheumatologist. Improved recognition of potential abnormalities will guide treatment strategies and enhance patient outcomes.