Introduction
Back pain is one of the most common reasons for primary- and emergency-care consultations. An estimated $200 billion is spent annually on managing back pain. Additionally, work hours, productivity, and workers' compensation are greatly reduced due to this condition.[1]
Back pain arises from a broad range of causes in adults and children, though most are mechanical in nature or have a nonspecific origin. Mechanical back pain comprises 90% of cases, so health providers can easily miss rare causes while focusing on common etiologies.[2][3]
Identifying red flags and determining the appropriate treatment are the most important aspects of back pain management. Most cases can be managed conservatively. Association with nerve dysfunction and other alarming signs warrants a thorough investigation and a multidisciplinary approach.[4]
Pharmacological treatments include pain relievers targeting peripheral and central neurologic pathways and muscle relaxants.[5] Various forms of physical therapy are available for individuals who prefer nonpharmacological approaches or recovering from injuries.[6] Acupuncture is an alternative therapy shown to improve back pain moderately. Surgery is reserved when the symptom is accompanied by severe nerve dysfunction or is due to serious causes like malignancy.[7][8] Back pain that does not resolve 6 weeks after acute injury warrants imaging by radiography, computed tomography (CT), or magnetic resonance imaging (MRI).
A thorough evaluation helps determine the cause of back pain and develop a tailored therapeutic plan. Eliminating the cause of this symptom profoundly improves patients' functional capacity and quality of life.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Back pain arises from various conditions, which can be classified into the following:[9]
- Traumatic: Back pain commonly results from direct or indirect contact with an external force. Examples are whiplash injury, strain, and traumatic fractures.
- Degenerative: Musculoskeletal structures can weaken over time due to aging, overuse, or pre-existing pathology. Conditions like intervertebral disk herniation and degenerative disk disease fall into this class.
- Oncologic: Anatomic structures of the back can develop primary or secondary malignant lesions. Pathologic fractures of the axial skeleton can arise as a complication.
- Infectious: Infections of the musculoskeletal structures in this region can arise from direct inoculation or spread from another source.
- Inflammatory: This category includes inflammatory conditions not caused by infection or malignancy. Examples are ankylosing spondylitis and sacroiliitis. Chronic inflammation can give rise to spinal arthritis.
- Metabolic: Calcium and bone metabolism can cause the symptoms. Osteoporosis and osteosclerosis are examples.
- Referred pain: Visceral organ inflammation can cause referred back pain. Examples are biliary colic, lung disease, and aortic or vertebral artery pathology.
- Postural: Spending long hours in an upright position can cause back pain. Pregnancy and certain occupations can predispose people to postural back pain.
- Congenital: Inborn conditions of the axial skeleton can cause the symptoms. Examples are kyphoscoliosis and tethered spinal cord.
- Psychiatric: Back pain may also present in patients with chronic pain syndromes and other mental health conditions. Malingering individuals may also claim to have back pain.
The problem's duration must also be considered, as acute back pain often has different sources from chronic back pain. Thorough clinical evaluation and appropriate diagnostic examination are usually enough to determine the exact cause of this symptom. Depending on the findings, referral to specialists such as orthopedic surgeons, neurologists, rheumatologists, or pain management specialists may be necessary for further evaluation and treatment planning.
Epidemiology
Back pain is widespread among adults. Studies show that up to 23% of adults worldwide suffer from chronic low back pain, with one-year recurrence rates reaching 24% to 80%.[10][11]. Lifetime back pain prevalence is as high as 84% in adults.[12]
Back pain is less prevalent among pediatric patients than in adults. One Scandinavian study revealed that the point prevalence of back pain was approximately 1% for 12-year-olds and 5% for 15-year-olds. By age 18 for girls and age 20 for boys, 50% would have already experienced at least one episode of back pain.[13] The lifetime prevalence of back pain in adolescents increases steadily with age until it approximates adult levels by 18 years.[14]
History and Physical
Determining the cause of back pain starts with a thorough history and physical examination. The onset of the pain must be established early. Acute back pain, which lasts less than 6 weeks, is usually precipitated by trauma or sudden changes in the course of a chronic illness like malignancy. Chronic cases, which last longer than 12 weeks, may be mechanically related or due to longstanding conditions.
Information about what provokes or alleviates the pain must be elicited. Besides providing additional clues to the diagnosis, knowing these factors guides the clinician in determining the appropriate pain control measures for the patient.
The pain quality helps the provider distinguish between visceral and non-visceral pain. Well-localized pain is often an indicator of an organic process. Any associated symptoms can serve as further clues about the source of back pain.
Other pertinent information may be obtained from the patient's medical, family, occupational, and social history. For example, a history of previous cancer chemotherapy should raise suspicion of metastasis or a secondary tumor. Some autoimmune arthritides have a hereditary component. Pott disease or spinal tuberculosis can result from tuberculosis exposure while traveling to a location where the infection is endemic. Spending long hours in a sitting position at work can cause acute and chronic back pain.
A focused physical examination should include inspection, auscultation, palpation, and provocative maneuvers. Visual back inspection may not reveal the cause of the problem unless deformity, inflammation signs, and skin lesions are present. Auscultation is valuable when the back pain may be secondary to a pulmonary pathology. Palpation can elicit localized musculoskeletal tenderness.
Some provocative exercises can help provide clues about the cause of back pain. One is the straight-leg-raising (SLR) test, which is useful for diagnosing lumbar disk herniation. The test is performed by raising the patient’s leg to 30° to 70°. The result is positive if ipsilateral leg pain develops at less than 60°. A crossed SLR test raises the leg contralateral to the side of disk herniation. A positive crossed SLR test result is even more specific than a positive SLR test.[15][16]
The Stork test, which tests for spondylolysis, is another maneuver used clinically to investigate the cause of back pain. The examiner supports the patient while having them stand on one leg and hyperextending the back. The maneuver is repeated on the other side. The test result is positive if the patient experiences pain during hypertension.
The Adam test aids in evaluating for scoliosis. The patient bends over with the feet together, arms extended, and palms together. An examiner standing in front can appreciate a thoracic lump in patients with scoliosis.[17]
Testing the range of motion, limb strength, deep tendon reflex, and sensation helps assess the integrity of both the musculoskeletal and neurologic systems.
Red flags on history or physical exam warrant imaging and other diagnostic tests. Listed below are the signs to watch out for in each group:
- Malignancy:
- History: History of metastatic cancer, unexplained weight loss
- Physical exam: Focal tenderness to palpation in the setting of risk factors
- Infection:
- History: Spinal procedure within the last 12 months, intravenous drug use, immunosuppression, prior lumbar spine surgery
- Physical exam: Fever, wound in the spinal region, localized pain, tenderness
- Fracture:
- History: Significant trauma (relative to age), prolonged corticosteroid use, osteoporosis, and age older than 70 years
- Physical exam: Contusions, abrasions, tenderness to palpation over spinous processes
- Neurologic:
- History: Progressive motor or sensory loss, new urinary retention or incontinence, new fecal incontinence
- Physical exam: Saddle anesthesia, anal sphincter atony, significant motor deficits of multiple myotomes
In pediatric patients:[20][21]
- Malignancy:
- History: Age younger than 4 years, nighttime pain
- Physical exam: Focal tenderness to palpation in the setting of risk factors
- Infectious:
- History: Age younger than 4 years, nighttime pain, history of tuberculosis exposure
- Physical exam: Fever, wound in the spinal region, localized pain, and tenderness
- Inflammatory:
- History: Age younger than 4 years, morning stiffness lasting longer than 30 minutes, improving with activity or hot showers
- Physical exam: Limited range of motion, localized pain, and tenderness
- Fracture:
- History: Activities with repetitive lumbar hyperextension (as in sports activities like cheerleading, gymnastics, wrestling, and football)
- Physical exam: Tenderness to palpation over spinous process, positive Stork test
Evaluation
History and physical examination are enough to determine the cause of back pain in most cases. Early imaging in the adult population correlates with worse outcomes, as it tends to result in more invasive treatments that provide little benefit to patients.[22][23] The same is true in the pediatric population. However, the presence of concerning signs warrants diagnostic testing. In adults, back pain persisting longer than 6 weeks despite appropriate conservative management is also an indication for imaging. In the pediatric population, the recommendation is to perform imaging tests for continuous pain lasting more than 4 weeks.[91]
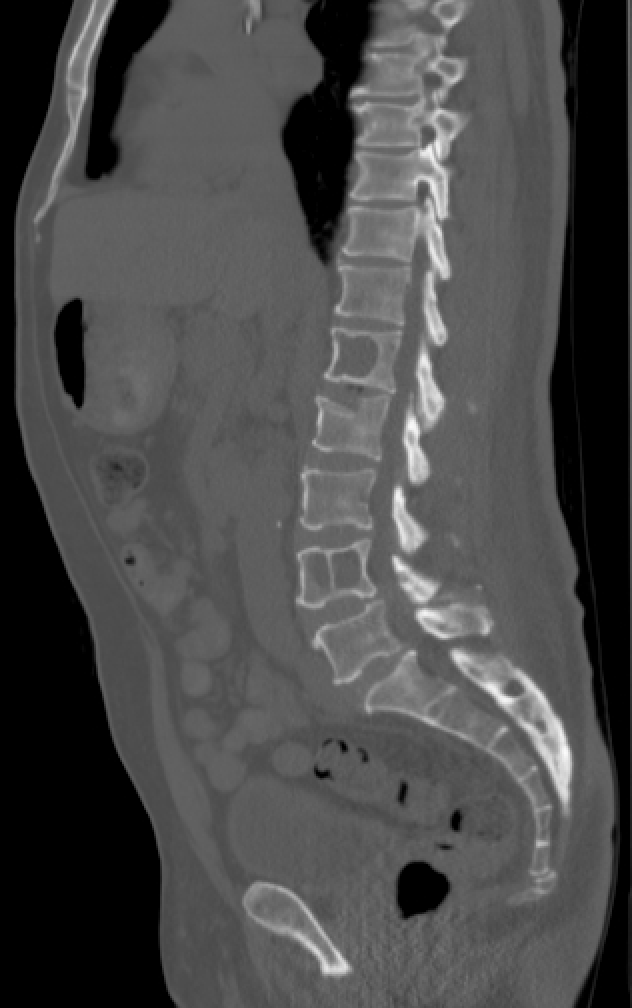
Plain anteroposterior and lateral (APL) films of the axial skeleton can detect bone pathology (see Image. Multiple Myeloma Involving the Spine). Magnetic resonance imaging (MRI) is indicated for evaluating soft tissue lesions, such as the nerves, intervertebral disks, and tendons. Both imaging modalities can detect signs of malignancy and inflammation, but MRI is preferable when the soft tissues are involved.[24][25] Bone scans may show osteomyelitis, diskitis, and stress reactions but remain inferior to MRI in evaluating these conditions.[26]
Adolescents with MRI evidence of disk herniation need a computed tomogram (CT) to confirm or rule out apophyseal ring separation, which occurs in 5.7% of these patients.[27]
Electromyography (EMG) or nerve conduction studies are indicated in patients with prior spinal surgery who may be experiencing radiculopathy or plexopathy as a complication. Image-guided diagnostic injection can help confirm sacroiliac joint injury.[92]
Laboratory tests may be necessary in some cases of back pain. Rheumatologic assays such as HLA-B27, antinuclear antibody (ANA), rheumatoid factor (RF), and Lyme antibodies are typically not helpful, being nonspecific for back pain.[28][29] However, the inflammatory markers C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) can be useful.[30] A complete blood count (CBC) and blood cultures may aid in diagnosing inflammatory, infectious, or malignant etiologies. High lactate dehydrogenase (LDH) and uric acid levels are commonly found in conditions associated with rapid marrow turnover like leukemia.[31]
Treatment / Management
Adult and pediatric back pain require different management approaches. Many cases have an unidentifiable cause, although degenerative disease and musculoskeletal injury are more common in adults than children. By comparison, overuse and muscle strain typically precipitate back pain in children and adolescents. Rare causes like malignancy and metabolic conditions also present differently in various age groups. Therefore, treatments must be appropriate for both the condition and the patient's age.
Management of Back Pain in Adults
For acute back pain in adults, serious conditions must first be ruled out. If there are no indications for further testing, the patient must be given reassurance about the condition and symptomatic relief. The first-line treatments are nonpharmacological and include the following:[93]
- Early return to normal routines, except for heavy labor
- Avoidance of activities that precipitate the pain
- Patient education
Second-line options that may be offered to the patient include nonsteroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, opioids, spinal manipulation, physical therapy, superficial heat application, and alternative treatments like acupuncture and massage. Education about the possible causes of back pain must be tailored to each patient's circumstances. Patient education is crucial in preventing back pain aggravation or recurrence. The patient may be advised to follow up after 2 weeks. Resumption of normal routines must be recommended if asymptomatic during follow-up.
For adult patients with acute radicular back pain, NSAID intake, exercise, traction, and spinal manipulation may be advised. Diazepam and systemic steroids have no added benefit.
Diagnostics tests are necessary if serious conditions cannot be ruled out. Referral to other specialists for other tests and treatments must be considered.
The management approach to chronic back pain is similar. Start by ruling out serious conditions. If the cause is nonspecific, advise the patient to remain active and avoid precipitating factors. Exercise therapy and cognitive behavioral therapy are also considered first-line treatments.[32][33] Second-line treatments include spinal manipulation, massage, acupuncture, yoga, stress reduction, NSAIDs, selective norepinephrine reuptake inhibitors (SNRIs), and interdisciplinary rehabilitation.[34][35][36](A1)
The role of anticonvulsants like gabapentin and topiramate in managing back pain is uncertain.[37][38] Transcutaneous electrical nerve stimulation (TENS) units do not appear more effective than placebo in managing chronic back pain.[39](A1)
The American Pain Society recommends that surgical referral be reserved for patients with disabling low-back pain lasting longer than 1 year.[40] However, evidence is mixed for some of the most commonly performed invasive procedures, including epidural space injection therapy and lumbar disk replacement.[41][42](A1)
Management of Back Pain in Children and Adolescents
Pediatric back pain treatments are less widely studied. However, activity modification, physical therapy, and NSAIDs have broad support as first-line therapies. If serious pathology is present, the treatment is based on the standard of care for that condition. Spondylolysis resulting from repetitive spinal stress may be managed conservatively as in adults. However, some young patients actively engaged in sports may need a referral for surgical intervention.[43][44] Symptoms persisting beyond 6 months of conservative therapy or Grade III or IV spondylolisthesis may be referred to a pediatric spine surgeon for further evaluation.[45][46](B2)
Patients with Scheuermann's kyphosis may be conservatively managed with physical therapy and guided exercise if the spinal curvature is less than 60°. Bracing may be added to these treatments for patients with curvature between 60° and 70°. Surgical correction is indicated for spinal curvature greater than 75°, especially if conservative measures have failed and the patient's skeleton is mature.[47][48] Spinal curvature of 20° or greater during peak growth, significant scoliosis, progressive curvature, and atypical scoliosis are all indications for a surgical referral.[49](B2)
Differential Diagnosis
Listed below are adult and pediatric conditions presenting with back pain. The associated symptoms and physical examination findings are also described. This list is not comprehensive, though it includes the most common or serious conditions producing this symptom.
Differential Diagnosis of Back Pain in Adults
- Lumbosacral muscle strains and sprains: Usually from a traumatic incident or repetitive overuse; pain worsens with movement and gets better with rest; range of motion is restricted; muscles are tender to palpation
- Lumbar spondylosis: The patient is typically older than 40 years; hip pain may be present; pain occurs with lower limb extension or rotation; neurologic exam is usually normal
- Disk herniation: Usually involves the L4 to S1 segments; may have associated paresthesia, sensory change, loss of strength or reflexes, depending on the severity and nerve root involved
- Spondylolysis and spondylolisthesis: Caused by repetitive spinal stress; may present with back pain radiating to the gluteal area and posterior thighs; neurologic deficits follow the L5 distribution.[50]
- Vertebral compression fracture: Localized back pain worsening with flexion; point tenderness on palpation; may be acute or chronic; steroid use, vitamin D deficiency, and osteoporosis are risk factors
- Spinal stenosis: Accompanied by leg sensory and motor weakness relieved with rest (neurologic claudication); neurologic exam may be normal initially but progress with increasing stenosis
- Tumor: May be accompanied by unexplained weight loss, focal tenderness to palpation, or malignancy risk factors on history (97% of spinal tumors are metastatic).[51]
- Infection: The patient may have a history of spinal surgery in the last 12 months, intravenous drug use, or immunosuppression; accompanying symptoms include fever, wound in the spinal region, localized pain, and tenderness, most commonly from vertebral osteomyelitis, diskitis, septic sacroiliitis, epidural abscess, and paraspinal muscle abscess; consider tuberculosis if the patient comes from a developing country.[52]
- Fracture: May arise from trauma, prolonged corticosteroid use, and osteoporosis; common among patients older than 70 years; associated findings include contusions, abrasions, tenderness to palpation over spinous processes
Differential Diagnosis of Back Pain in Children and Adolescents
- Tumor: May present with fever, malaise, weight loss, nighttime pain, and recent onset scoliosis; osteoid osteoma is the most common tumor presenting with back pain easily relieved by NSAIDs.[53][54][55]
- Infection: Associated symptoms include fever, malaise, weight loss, nighttime pain, and recent-onset scoliosis; patients may refuse to walk; most common conditions are vertebral osteomyelitis, diskitis, septic sacroiliitis, epidural abscess, and paraspinal muscle abscess; consider epidural abscess if neurologic deficits and radicular pain also appear.[56][57]
- Disk herniation and slipped apophysis: May present with acute back pain, radicular pain, and recent-onset scoliosis; physical findings include positive SLR test and pain on spinal forward flexion.
- Spondylolysis, spondylolisthesis, and posterior arch lesion: Acute-onset back pain presents with radicular pain; hamstring tightness may be present; physical findings include positive SLR test and pain on spinal extension.
- Vertebral fracture: Trauma is the most common cause; acute back pain may be associated with other injuries; neurologic deficits may be present on physical examination; stress fractures may present insidiously and produce progressive postural changes.
- Muscle strain: Acute back pain is typically associated with muscle tenderness without radiation.Scheuermann’s kyphosis: Back pain is chronic and associated with rigid kyphosis.
- Inflammatory spondyloarthropathies: Pertinent findings on history include chronic pain, morning stiffness lasting greater than 30 minutes, and sacroiliac joint tenderness.
- Psychological disorder, eg, conversion and somatization disorder: Persistent subjective pain with normal physical findingsIdiopathic scoliosis: Most commonly asymptomatic, with a positive Adam test; back pain may be due to another cause.[58]
Prognosis
In adults, the prognosis of back pain depends on the etiology. Most nonspecific cases resolve without serious sequelae. The success of conservative therapy and patient education in treating adult back pain shows that pain is subjective and often stress-related. For some patients with unidentifiable causes of back pain, prior back pain episodes, greater symptom intensity, depression, fear-avoidance behavior, and the presence of leg or widespread symptoms are associated with chronic, disabling back pain.[59]
Underlying social factors have significant prognostic accuracy.[60] Conditions such as low educational attainment, having a highly laborious job, poor compensation, and poor job satisfaction worsen outcomes, including disability rates.[61][62] Lifestyle activities also play a role. A body mass index (BMI) greater than 25 and smoking are associated with persistent back pain.[63].
Fewer studies have been made about back pain prognosis in pediatric patients than in adult individuals, though it appears the etiology also impacts outcomes.[64] For example, back pain caused by cancer is more likely to cause disability than muscle strain.[65] Some studies show that nonspecific back pain in younger people worsens with behavioral comorbidities.[66] Conduct problems, attention deficit hyperactivity disorder (ADHD), passive coping, and fear-avoidance behavior have been implicated in the literature as having a negative impact on back pain.[67][68]
Complications
The underlying back pain etiology determines the potential for complications. The condition can have both physical and social consequences. Physically, back pain can become chronic and associated with deformity, neurologic deficits, or both. Socially, the complications of this condition include disability, decreased gross domestic product, and increased absenteeism. A 2015 study found that back pain has caused 60.1 million years of disability worldwide, making this symptom the most common cause of disability globally.[69] In the US, low-back pain is the most common reason for disability.[70]
Addressing the problem before it becomes chronic helps prevent complications. Early ambulation helps improve outcomes, while sedentariness leading to obesity tends to worsen the prognosis.
Postoperative and Rehabilitation Care
The underlying cause, patient comorbidities, and health goals determine back pain rehabilitation efforts. The McKenzie method is often cited as beneficial for nonspecific low-back pain treatment, especially if it is chronic.[71] The Clinical Practice Guidelines for Physical Therapy recommend manual therapy, trunk strengthening, centralization, directional preference, and progressive endurance exercises for rehabilitation. Occupational therapy can also help patients manage activities of daily living and use adaptive equipment as needed. Using assistive devices during patient transfers reduces low-back pain incidence in female healthcare workers.[72][73]
Deterrence and Patient Education
Patient education about preventing back pain recurrence or aggravation must be tailored to personal factors. For example, individuals with jobs that do not require hard physical labor must be reminded to stay active to maintain a healthy body weight. A BMI greater than 25 correlates with worse outcomes. The same reminder must be given to people with labor-intensive occupations. However, these individuals should also avoid factors precipitating back pain, such as heavy-load lifting and excessive or repeated back-twisting. These patients should lighten their loads or use lifting equipment when moving weighty objects.
All patients must be reminded to avoid smoking, which increases the risk of back pain in people of any age.[74][75] Intensive patient education lasting for 2.5 hours discussing activity modification, staying active, and early return to normal activity has been proven effective in encouraging adult patients to return to work.[76]
In pediatric patients, evidence is mixed about whether bookbag weight plays a role in pediatric back pain. Still, the American Academy of Pediatrics recommends that bookbags do not exceed 10% to 20% of a child’s body weight.[77]
The vast majority of back pain cases are self-limited. However, all discharged patients advised to follow up should be instructed to seek medical attention immediately for concerning signs like sudden sensory and motor weakness.
Pearls and Other Issues
The following are the practice pearls worth remembering in back pain management:
For Adults
- History and physical examination usually suffice for evaluating atraumatic, acute back pain without clinical red flags. Wait 6 weeks for symptom resolution before ordering imaging tests.[78][79]
- Patient education focusing on remaining active is the first-line treatment for nonspecific back pain. Studies show that pharmacologic and physical therapy do not consistently benefit patients with back pain. However, clinicians may consider NSAIDs, opioids, and SNRIs like duloxetine as second-line therapy for nonspecific chronic low-back pain. These medications are more effective than placebo for this condition.[80][81]
- Acetaminophen, antidepressants (except SNRIs), lidocaine patches, and TENS are not consistently more effective than placebo in treating chronic low-back pain.[82][83]
- Consider a physical therapy referral for the McKenzie technique to reduce recurrence risk.[84][85]
For Children
- Children with transient back pain and a history of minor injury but without significant physical findings can be treated conservatively without further evaluation.
- Abnormal physical findings, constant pain, nighttime pain, or radicular pain are indications for further evaluation.[86]
- Plain APL films are recommended as the first-line radiographic studies.
- Consider laboratory tests in the presence of clinical red flags. Thoracic malignancy and infection are more likely in children than adults, especially those younger than 4 years.[87]
Enhancing Healthcare Team Outcomes
Integrating the expertise of various healthcare professionals ensures comprehensive care, better outcomes, and improved quality of life for individuals experiencing back pain. The multidisciplinary team for managing back pain comprises the primary care provider, nurse, pharmacist, nutritionist, physical therapist, occupational therapist, radiologist, and medical specialists appropriate to each case.
The primary care provider is the first medical specialist who examines the patient. Evaluation of back pain starts with a complete medical history and physical examination. From there, the primary care provider determines the appropriate initial treatment and evaluates the need for further diagnostic testing and specialist referral. The primary care provider also takes charge of patient education and communicating follow-up recommendations to the patient. When educating patients, smoking cessation and maintaining a healthy body weight should be emphasized.[88]
The nurse should reiterate the important parts of patient education and follow-up instructions. Evidence-based answers must be given to patients asking about the role of nonpharmacologic therapy and continued physical activity in back pain management. The nurse must ensure the patient is clinically stable before discharge and care plans are coordinated before the next appointment.
If the primary care physician prescribes medications, the pharmacist can help educate patients about the prescribed drugs' back pain-specific benefits and risks. Intake instructions and the potential risks of overdose must be emphasized. The pharmacist should not hesitate to contact the primary care provider to clarify a patient's prescription.
Obesity in a patient with back pain is associated with adverse outcomes. Patients can work with nutritionists to make healthier dietary choices and maintain a healthy weight. If a patient is obese, an obesity medicine specialist can prescribe antiobesity medications as adjunct to lifestyle modifications to help them lose significant weight.
The physical therapist can prescribe the appropriate strength and endurance exercises for managing back pain and preventing recurrences. Physical therapy is effective in weaning patients with back pain from opioid use.[89] An occupational therapist can provide ergonomic guidance and recommend assistive devices to manage back pain in work and home settings.
The radiologist helps the primary care physician interpret imaging findings. These specialists can also make recommendations for additional imaging tests if necessary.
The primary care physician can make referrals to other specialists as needed. A pain specialist can help patients with chronic back pain by modifying their current pharmacologic treatment regimen or performing a pain-management procedure. A rheumatologist may be consulted for back pain associated with signs of chronic inflammatory disease. Severe radiculopathy or rapid neurological changes are indications for prompt neurosurgery referral. A mental health therapist can teach stress-coping techniques, administer cognitive behavioral therapy, and prescribe other treatments appropriate for back pain with a prominent psychological component.[90] Alternative medicine providers may also be instrumental in improving patient function.
The interprofessional team should communicate with each other to prevent duplicating diagnostic tests and contradicting treatments, both of which can hinder a patient's progress.
Media
(Click Image to Enlarge)
References
Freburger JK, Holmes GM, Agans RP, Jackman AM, Darter JD, Wallace AS, Castel LD, Kalsbeek WD, Carey TS. The rising prevalence of chronic low back pain. Archives of internal medicine. 2009 Feb 9:169(3):251-8. doi: 10.1001/archinternmed.2008.543. Epub [PubMed PMID: 19204216]
Level 2 (mid-level) evidenceBarros G, McGrath L, Gelfenbeyn M. Sacroiliac Joint Dysfunction in Patients With Low Back Pain. Federal practitioner : for the health care professionals of the VA, DoD, and PHS. 2019 Aug:36(8):370-375 [PubMed PMID: 31456628]
Cohen SP, Chen Y, Neufeld NJ. Sacroiliac joint pain: a comprehensive review of epidemiology, diagnosis and treatment. Expert review of neurotherapeutics. 2013 Jan:13(1):99-116. doi: 10.1586/ern.12.148. Epub [PubMed PMID: 23253394]
Buell KG, Sivasubramaniyam S, Sykes M, Zafar K, Bingham L, Mitra A. Expediting the management of cauda equina syndrome in the emergency department through clinical pathway design. BMJ open quality. 2019:8(4):e000597. doi: 10.1136/bmjoq-2018-000597. Epub 2019 Nov 2 [PubMed PMID: 31799444]
Level 2 (mid-level) evidenceMusich S, Wang SS, Slindee LB, Keown K, Hawkins K, Yeh CS. Using Pain Medication Intensity to Stratify Back Pain Among Older Adults. Pain medicine (Malden, Mass.). 2019 Feb 1:20(2):252-266. doi: 10.1093/pm/pny007. Epub [PubMed PMID: 29394401]
Owen PJ, Miller CT, Mundell NL, Verswijveren SJJM, Tagliaferri SD, Brisby H, Bowe SJ, Belavy DL. Which specific modes of exercise training are most effective for treating low back pain? Network meta-analysis. British journal of sports medicine. 2020 Nov:54(21):1279-1287. doi: 10.1136/bjsports-2019-100886. Epub 2019 Oct 30 [PubMed PMID: 31666220]
Level 1 (high-level) evidenceWei X, Liu B, He L, Yang X, Zhou J, Zhao H, Liu J. Acupuncture therapy for chronic low back pain: protocol of a prospective, multi-center, registry study. BMC musculoskeletal disorders. 2019 Oct 27:20(1):488. doi: 10.1186/s12891-019-2894-4. Epub 2019 Oct 27 [PubMed PMID: 31656194]
Qin J, Zhang Y, Wu L, He Z, Huang J, Tao J, Chen L. Effect of Tai Chi alone or as additional therapy on low back pain: Systematic review and meta-analysis of randomized controlled trials. Medicine. 2019 Sep:98(37):e17099. doi: 10.1097/MD.0000000000017099. Epub [PubMed PMID: 31517838]
Level 2 (mid-level) evidencePatrick N, Emanski E, Knaub MA. Acute and chronic low back pain. The Medical clinics of North America. 2014 Jul:98(4):777-89, xii. doi: 10.1016/j.mcna.2014.03.005. Epub [PubMed PMID: 24994051]
Balagué F, Mannion AF, Pellisé F, Cedraschi C. Non-specific low back pain. Lancet (London, England). 2012 Feb 4:379(9814):482-91. doi: 10.1016/S0140-6736(11)60610-7. Epub 2011 Oct 6 [PubMed PMID: 21982256]
Hoy D, Brooks P, Blyth F, Buchbinder R. The Epidemiology of low back pain. Best practice & research. Clinical rheumatology. 2010 Dec:24(6):769-81. doi: 10.1016/j.berh.2010.10.002. Epub [PubMed PMID: 21665125]
Walker BF. The prevalence of low back pain: a systematic review of the literature from 1966 to 1998. Journal of spinal disorders. 2000 Jun:13(3):205-17 [PubMed PMID: 10872758]
Level 1 (high-level) evidenceLeboeuf-Yde C, Kyvik KO. At what age does low back pain become a common problem? A study of 29,424 individuals aged 12-41 years. Spine. 1998 Jan 15:23(2):228-34 [PubMed PMID: 9474731]
Level 2 (mid-level) evidenceJeffries LJ, Milanese SF, Grimmer-Somers KA. Epidemiology of adolescent spinal pain: a systematic overview of the research literature. Spine. 2007 Nov 1:32(23):2630-7 [PubMed PMID: 17978666]
Level 2 (mid-level) evidenceDeyo RA, Rainville J, Kent DL. What can the history and physical examination tell us about low back pain? JAMA. 1992 Aug 12:268(6):760-5 [PubMed PMID: 1386391]
M Das J, Nadi M. Lasegue Sign. StatPearls. 2023 Jan:(): [PubMed PMID: 31424883]
Patel DR, Kinsella E. Evaluation and management of lower back pain in young athletes. Translational pediatrics. 2017 Jul:6(3):225-235. doi: 10.21037/tp.2017.06.01. Epub [PubMed PMID: 28795014]
Downie A, Williams CM, Henschke N, Hancock MJ, Ostelo RW, de Vet HC, Macaskill P, Irwig L, van Tulder MW, Koes BW, Maher CG. Red flags to screen for malignancy and fracture in patients with low back pain: systematic review. BMJ (Clinical research ed.). 2013 Dec 11:347():f7095. doi: 10.1136/bmj.f7095. Epub 2013 Dec 11 [PubMed PMID: 24335669]
Level 1 (high-level) evidenceCasazza BA. Diagnosis and treatment of acute low back pain. American family physician. 2012 Feb 15:85(4):343-50 [PubMed PMID: 22335313]
Feldman DS, Hedden DM, Wright JG. The use of bone scan to investigate back pain in children and adolescents. Journal of pediatric orthopedics. 2000 Nov-Dec:20(6):790-5 [PubMed PMID: 11097256]
Level 2 (mid-level) evidenceHollingworth P. Back pain in children. British journal of rheumatology. 1996 Oct:35(10):1022-8 [PubMed PMID: 8883446]
Patel ND, Broderick DF, Burns J, Deshmukh TK, Fries IB, Harvey HB, Holly L, Hunt CH, Jagadeesan BD, Kennedy TA, O'Toole JE, Perlmutter JS, Policeni B, Rosenow JM, Schroeder JW, Whitehead MT, Cornelius RS, Corey AS. ACR Appropriateness Criteria Low Back Pain. Journal of the American College of Radiology : JACR. 2016 Sep:13(9):1069-78. doi: 10.1016/j.jacr.2016.06.008. Epub 2016 Aug 3 [PubMed PMID: 27496288]
Jarvik JG, Hollingworth W, Martin B, Emerson SS, Gray DT, Overman S, Robinson D, Staiger T, Wessbecher F, Sullivan SD, Kreuter W, Deyo RA. Rapid magnetic resonance imaging vs radiographs for patients with low back pain: a randomized controlled trial. JAMA. 2003 Jun 4:289(21):2810-8 [PubMed PMID: 12783911]
Level 1 (high-level) evidenceMiller R, Beck NA, Sampson NR, Zhu X, Flynn JM, Drummond D. Imaging modalities for low back pain in children: a review of spondyloysis and undiagnosed mechanical back pain. Journal of pediatric orthopedics. 2013 Apr-May:33(3):282-8. doi: 10.1097/BPO.0b013e318287fffb. Epub [PubMed PMID: 23482264]
Level 2 (mid-level) evidenceBorchers AT, Gershwin ME. Transverse myelitis. Autoimmunity reviews. 2012 Jan:11(3):231-48. doi: 10.1016/j.autrev.2011.05.018. Epub 2011 May 18 [PubMed PMID: 21621005]
Kujala UM, Kinnunen J, Helenius P, Orava S, Taavitsainen M, Karaharju E. Prolonged low-back pain in young athletes: a prospective case series study of findings and prognosis. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society. 1999:8(6):480-4 [PubMed PMID: 10664307]
Level 2 (mid-level) evidenceWang H, Cheng J, Xiao H, Li C, Zhou Y. Adolescent lumbar disc herniation: experience from a large minimally invasive treatment centre for lumbar degenerative disease in Chongqing, China. Clinical neurology and neurosurgery. 2013 Aug:115(8):1415-9. doi: 10.1016/j.clineuro.2013.01.019. Epub 2013 Feb 16 [PubMed PMID: 23419406]
Level 2 (mid-level) evidenceGran JT, Husby G. HLA-B27 and spondyloarthropathy: value for early diagnosis? Journal of medical genetics. 1995 Jul:32(7):497-501 [PubMed PMID: 7562959]
Reveille JD. HLA-B27 and the seronegative spondyloarthropathies. The American journal of the medical sciences. 1998 Oct:316(4):239-49 [PubMed PMID: 9766485]
McGhee JL, Burks FN, Sheckels JL, Jarvis JN. Identifying children with chronic arthritis based on chief complaints: absence of predictive value for musculoskeletal pain as an indicator of rheumatic disease in children. Pediatrics. 2002 Aug:110(2 Pt 1):354-9 [PubMed PMID: 12165590]
Level 2 (mid-level) evidenceEjaz AA, Pourafshar N, Mohandas R, Smallwood BA, Johnson RJ, Hsu JW. Uric acid and the prediction models of tumor lysis syndrome in AML. PloS one. 2015:10(3):e0119497. doi: 10.1371/journal.pone.0119497. Epub 2015 Mar 16 [PubMed PMID: 25775138]
Level 2 (mid-level) evidenceRosedale R, Rastogi R, May S, Chesworth BM, Filice F, Willis S, Howard J, Naudie D, Robbins SM. Efficacy of exercise intervention as determined by the McKenzie System of Mechanical Diagnosis and Therapy for knee osteoarthritis: a randomized controlled trial. The Journal of orthopaedic and sports physical therapy. 2014 Mar:44(3):173-81, A1-6. doi: 10.2519/jospt.2014.4791. Epub 2014 Jan 22 [PubMed PMID: 24450370]
Level 1 (high-level) evidenceDunsford A, Kumar S, Clarke S. Integrating evidence into practice: use of McKenzie-based treatment for mechanical low back pain. Journal of multidisciplinary healthcare. 2011:4():393-402. doi: 10.2147/JMDH.S24733. Epub 2011 Nov 1 [PubMed PMID: 22135496]
Kamper SJ, Apeldoorn AT, Chiarotto A, Smeets RJ, Ostelo RW, Guzman J, van Tulder MW. Multidisciplinary biopsychosocial rehabilitation for chronic low back pain: Cochrane systematic review and meta-analysis. BMJ (Clinical research ed.). 2015 Feb 18:350():h444. doi: 10.1136/bmj.h444. Epub 2015 Feb 18 [PubMed PMID: 25694111]
Level 1 (high-level) evidenceStraube S, Harden M, Schröder H, Arendacka B, Fan X, Moore RA, Friede T. Back schools for the treatment of chronic low back pain: possibility of benefit but no convincing evidence after 47 years of research-systematic review and meta-analysis. Pain. 2016 Oct:157(10):2160-2172. doi: 10.1097/j.pain.0000000000000640. Epub [PubMed PMID: 27257858]
Level 1 (high-level) evidenceFranke H, Franke JD, Fryer G. Osteopathic manipulative treatment for nonspecific low back pain: a systematic review and meta-analysis. BMC musculoskeletal disorders. 2014 Aug 30:15():286. doi: 10.1186/1471-2474-15-286. Epub 2014 Aug 30 [PubMed PMID: 25175885]
Level 1 (high-level) evidenceShanthanna H, Gilron I, Rajarathinam M, AlAmri R, Kamath S, Thabane L, Devereaux PJ, Bhandari M. Benefits and safety of gabapentinoids in chronic low back pain: A systematic review and meta-analysis of randomized controlled trials. PLoS medicine. 2017 Aug:14(8):e1002369. doi: 10.1371/journal.pmed.1002369. Epub 2017 Aug 15 [PubMed PMID: 28809936]
Level 1 (high-level) evidenceMuehlbacher M, Nickel MK, Kettler C, Tritt K, Lahmann C, Leiberich PK, Nickel C, Krawczyk J, Mitterlehner FO, Rother WK, Loew TH, Kaplan P. Topiramate in treatment of patients with chronic low back pain: a randomized, double-blind, placebo-controlled study. The Clinical journal of pain. 2006 Jul-Aug:22(6):526-31 [PubMed PMID: 16788338]
Level 1 (high-level) evidenceBuchmuller A, Navez M, Milletre-Bernardin M, Pouplin S, Presles E, Lantéri-Minet M, Tardy B, Laurent B, Camdessanché JP, Lombotens Trial Group. Value of TENS for relief of chronic low back pain with or without radicular pain. European journal of pain (London, England). 2012 May:16(5):656-65. doi: 10.1002/j.1532-2149.2011.00061.x. Epub 2011 Dec 20 [PubMed PMID: 22337531]
Level 1 (high-level) evidenceChou R, Loeser JD, Owens DK, Rosenquist RW, Atlas SJ, Baisden J, Carragee EJ, Grabois M, Murphy DR, Resnick DK, Stanos SP, Shaffer WO, Wall EM, American Pain Society Low Back Pain Guideline Panel. Interventional therapies, surgery, and interdisciplinary rehabilitation for low back pain: an evidence-based clinical practice guideline from the American Pain Society. Spine. 2009 May 1:34(10):1066-77. doi: 10.1097/BRS.0b013e3181a1390d. Epub [PubMed PMID: 19363457]
Level 1 (high-level) evidenceStaal JB, de Bie R, de Vet HC, Hildebrandt J, Nelemans P. Injection therapy for subacute and chronic low-back pain. The Cochrane database of systematic reviews. 2008 Jul 16:2008(3):CD001824. doi: 10.1002/14651858.CD001824.pub3. Epub 2008 Jul 16 [PubMed PMID: 18646078]
Level 1 (high-level) evidenceMachado GC, Ferreira PH, Yoo RI, Harris IA, Pinheiro MB, Koes BW, van Tulder MW, Rzewuska M, Maher CG, Ferreira ML. Surgical options for lumbar spinal stenosis. The Cochrane database of systematic reviews. 2016 Nov 1:11(11):CD012421 [PubMed PMID: 27801521]
Level 1 (high-level) evidenceKaratas AF, Dede O, Atanda AA, Holmes L Jr, Rogers K, Gabos P, Shah SA. Comparison of Direct Pars Repair Techniques of Spondylolysis in Pediatric and Adolescent Patients: Pars Compression Screw Versus Pedicle Screw-Rod-Hook. Clinical spine surgery. 2016 Aug:29(7):272-80. doi: 10.1097/BSD.0b013e318277cb7d. Epub [PubMed PMID: 23075858]
Menga EN, Kebaish KM, Jain A, Carrino JA, Sponseller PD. Clinical results and functional outcomes after direct intralaminar screw repair of spondylolysis. Spine. 2014 Jan 1:39(1):104-10. doi: 10.1097/BRS.0000000000000043. Epub [PubMed PMID: 24108299]
Helenius I, Lamberg T, Osterman K, Schlenzka D, Yrjönen T, Tervahartiala P, Seitsalo S, Poussa M, Remes V. Scoliosis research society outcome instrument in evaluation of long-term surgical results in spondylolysis and low-grade isthmic spondylolisthesis in young patients. Spine. 2005 Feb 1:30(3):336-41 [PubMed PMID: 15682016]
Level 2 (mid-level) evidenceLundine KM, Lewis SJ, Al-Aubaidi Z, Alman B, Howard AW. Patient outcomes in the operative and nonoperative management of high-grade spondylolisthesis in children. Journal of pediatric orthopedics. 2014 Jul-Aug:34(5):483-9. doi: 10.1097/BPO.0000000000000133. Epub [PubMed PMID: 24590330]
Level 2 (mid-level) evidenceTsirikos AI, Jain AK. Scheuermann's kyphosis; current controversies. The Journal of bone and joint surgery. British volume. 2011 Jul:93(7):857-64. doi: 10.1302/0301-620X.93B7.26129. Epub [PubMed PMID: 21705553]
Lim M, Green DW, Billinghurst JE, Huang RC, Rawlins BA, Widmann RF, Burke SW, Boachie-Adjei O. Scheuermann kyphosis: safe and effective surgical treatment using multisegmental instrumentation. Spine. 2004 Aug 15:29(16):1789-94 [PubMed PMID: 15303023]
Level 2 (mid-level) evidenceParent S, Newton PO, Wenger DR. Adolescent idiopathic scoliosis: etiology, anatomy, natural history, and bracing. Instructional course lectures. 2005:54():529-36 [PubMed PMID: 15948477]
Will JS, Bury DC, Miller JA. Mechanical Low Back Pain. American family physician. 2018 Oct 1:98(7):421-428 [PubMed PMID: 30252425]
Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, Hoy D, Karppinen J, Pransky G, Sieper J, Smeets RJ, Underwood M, Lancet Low Back Pain Series Working Group. What low back pain is and why we need to pay attention. Lancet (London, England). 2018 Jun 9:391(10137):2356-2367. doi: 10.1016/S0140-6736(18)30480-X. Epub 2018 Mar 21 [PubMed PMID: 29573870]
Trecarichi EM, Di Meco E, Mazzotta V, Fantoni M. Tuberculous spondylodiscitis: epidemiology, clinical features, treatment, and outcome. European review for medical and pharmacological sciences. 2012 Apr:16 Suppl 2():58-72 [PubMed PMID: 22655484]
Slipman CW, Patel RK, Botwin K, Huston C, Zhang L, Lenrow D, Garvan C. Epidemiology of spine tumors presenting to musculoskeletal physiatrists. Archives of physical medicine and rehabilitation. 2003 Apr:84(4):492-5 [PubMed PMID: 12690585]
Level 2 (mid-level) evidenceCohen MD, Harrington TM, Ginsburg WW. Osteoid osteoma: 95 cases and a review of the literature. Seminars in arthritis and rheumatism. 1983 Feb:12(3):265-81 [PubMed PMID: 6603021]
Level 2 (mid-level) evidenceAzouz EM, Kozlowski K, Marton D, Sprague P, Zerhouni A, Asselah F. Osteoid osteoma and osteoblastoma of the spine in children. Report of 22 cases with brief literature review. Pediatric radiology. 1986:16(1):25-31 [PubMed PMID: 2935775]
Level 3 (low-level) evidenceKang HM, Choi EH, Lee HJ, Yun KW, Lee CK, Cho TJ, Cheon JE, Lee H. The Etiology, Clinical Presentation and Long-term Outcome of Spondylodiscitis in Children. The Pediatric infectious disease journal. 2016 Apr:35(4):e102-6. doi: 10.1097/INF.0000000000001043. Epub [PubMed PMID: 26974751]
Spencer SJ, Wilson NI. Childhood discitis in a regional children's hospital. Journal of pediatric orthopedics. Part B. 2012 May:21(3):264-8. doi: 10.1097/BPB.0b013e32834d3e94. Epub [PubMed PMID: 22015583]
Ramirez N, Johnston CE, Browne RH. The prevalence of back pain in children who have idiopathic scoliosis. The Journal of bone and joint surgery. American volume. 1997 Mar:79(3):364-8 [PubMed PMID: 9070524]
Level 2 (mid-level) evidenceHendrick P, Milosavljevic S, Hale L, Hurley DA, McDonough S, Ryan B, Baxter GD. The relationship between physical activity and low back pain outcomes: a systematic review of observational studies. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society. 2011 Mar:20(3):464-74. doi: 10.1007/s00586-010-1616-2. Epub 2010 Nov 4 [PubMed PMID: 21053026]
Level 1 (high-level) evidencePinheiro MB, Ferreira ML, Refshauge K, Maher CG, Ordoñana JR, Andrade TB, Tsathas A, Ferreira PH. Symptoms of depression as a prognostic factor for low back pain: a systematic review. The spine journal : official journal of the North American Spine Society. 2016 Jan 1:16(1):105-16. doi: 10.1016/j.spinee.2015.10.037. Epub 2015 Oct 30 [PubMed PMID: 26523965]
Level 1 (high-level) evidenceWertli MM, Eugster R, Held U, Steurer J, Kofmehl R, Weiser S. Catastrophizing-a prognostic factor for outcome in patients with low back pain: a systematic review. The spine journal : official journal of the North American Spine Society. 2014 Nov 1:14(11):2639-57. doi: 10.1016/j.spinee.2014.03.003. Epub 2014 Mar 7 [PubMed PMID: 24607845]
Level 1 (high-level) evidenceWertli MM, Rasmussen-Barr E, Weiser S, Bachmann LM, Brunner F. The role of fear avoidance beliefs as a prognostic factor for outcome in patients with nonspecific low back pain: a systematic review. The spine journal : official journal of the North American Spine Society. 2014 May 1:14(5):816-36.e4. doi: 10.1016/j.spinee.2013.09.036. Epub 2013 Oct 18 [PubMed PMID: 24412032]
Level 1 (high-level) evidenceChou R, Shekelle P. Will this patient develop persistent disabling low back pain? JAMA. 2010 Apr 7:303(13):1295-302. doi: 10.1001/jama.2010.344. Epub [PubMed PMID: 20371789]
Jones GT, Watson KD, Silman AJ, Symmons DP, Macfarlane GJ. Predictors of low back pain in British schoolchildren: a population-based prospective cohort study. Pediatrics. 2003 Apr:111(4 Pt 1):822-8 [PubMed PMID: 12671119]
Level 2 (mid-level) evidenceLynch AM, Kashikar-Zuck S, Goldschneider KR, Jones BA. Psychosocial risks for disability in children with chronic back pain. The journal of pain. 2006 Apr:7(4):244-51 [PubMed PMID: 16618468]
Korovessis P, Repantis T, Baikousis A. Factors affecting low back pain in adolescents. Journal of spinal disorders & techniques. 2010 Dec:23(8):513-20. doi: 10.1097/BSD.0b013e3181bf99c6. Epub [PubMed PMID: 20075753]
Ramond A, Bouton C, Richard I, Roquelaure Y, Baufreton C, Legrand E, Huez JF. Psychosocial risk factors for chronic low back pain in primary care--a systematic review. Family practice. 2011 Feb:28(1):12-21. doi: 10.1093/fampra/cmq072. Epub 2010 Sep 10 [PubMed PMID: 20833704]
Level 1 (high-level) evidenceMustard CA, Kalcevich C, Frank JW, Boyle M. Childhood and early adult predictors of risk of incident back pain: Ontario Child Health Study 2001 follow-up. American journal of epidemiology. 2005 Oct 15:162(8):779-86 [PubMed PMID: 16150891]
Level 2 (mid-level) evidenceGBD 2015 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet (London, England). 2016 Oct 8:388(10053):1545-1602. doi: 10.1016/S0140-6736(16)31678-6. Epub [PubMed PMID: 27733282]
Level 1 (high-level) evidenceUS Burden of Disease Collaborators, Mokdad AH, Ballestros K, Echko M, Glenn S, Olsen HE, Mullany E, Lee A, Khan AR, Ahmadi A, Ferrari AJ, Kasaeian A, Werdecker A, Carter A, Zipkin B, Sartorius B, Serdar B, Sykes BL, Troeger C, Fitzmaurice C, Rehm CD, Santomauro D, Kim D, Colombara D, Schwebel DC, Tsoi D, Kolte D, Nsoesie E, Nichols E, Oren E, Charlson FJ, Patton GC, Roth GA, Hosgood HD, Whiteford HA, Kyu H, Erskine HE, Huang H, Martopullo I, Singh JA, Nachega JB, Sanabria JR, Abbas K, Ong K, Tabb K, Krohn KJ, Cornaby L, Degenhardt L, Moses M, Farvid M, Griswold M, Criqui M, Bell M, Nguyen M, Wallin M, Mirarefin M, Qorbani M, Younis M, Fullman N, Liu P, Briant P, Gona P, Havmoller R, Leung R, Kimokoti R, Bazargan-Hejazi S, Hay SI, Yadgir S, Biryukov S, Vollset SE, Alam T, Frank T, Farid T, Miller T, Vos T, Bärnighausen T, Gebrehiwot TT, Yano Y, Al-Aly Z, Mehari A, Handal A, Kandel A, Anderson B, Biroscak B, Mozaffarian D, Dorsey ER, Ding EL, Park EK, Wagner G, Hu G, Chen H, Sunshine JE, Khubchandani J, Leasher J, Leung J, Salomon J, Unutzer J, Cahill L, Cooper L, Horino M, Brauer M, Breitborde N, Hotez P, Topor-Madry R, Soneji S, Stranges S, James S, Amrock S, Jayaraman S, Patel T, Akinyemiju T, Skirbekk V, Kinfu Y, Bhutta Z, Jonas JB, Murray CJL. The State of US Health, 1990-2016: Burden of Diseases, Injuries, and Risk Factors Among US States. JAMA. 2018 Apr 10:319(14):1444-1472. doi: 10.1001/jama.2018.0158. Epub [PubMed PMID: 29634829]
Lam OT, Strenger DM, Chan-Fee M, Pham PT, Preuss RA, Robbins SM. Effectiveness of the McKenzie Method of Mechanical Diagnosis and Therapy for Treating Low Back Pain: Literature Review With Meta-analysis. The Journal of orthopaedic and sports physical therapy. 2018 Jun:48(6):476-490. doi: 10.2519/jospt.2018.7562. Epub 2018 Mar 30 [PubMed PMID: 29602304]
Level 1 (high-level) evidenceDelitto A, George SZ, Van Dillen L, Whitman JM, Sowa G, Shekelle P, Denninger TR, Godges JJ, Orthopaedic Section of the American Physical Therapy Association. Low back pain. The Journal of orthopaedic and sports physical therapy. 2012 Apr:42(4):A1-57. doi: 10.2519/jospt.2012.42.4.A1. Epub 2012 Mar 30 [PubMed PMID: 22466247]
Holtermann A, Clausen T, Jørgensen MB, Aust B, Mortensen OS, Burdorf A, Fallentin N, Andersen LL. Does rare use of assistive devices during patient handling increase the risk of low back pain? A prospective cohort study among female healthcare workers. International archives of occupational and environmental health. 2015 Apr:88(3):335-42. doi: 10.1007/s00420-014-0963-4. Epub 2014 Jul 23 [PubMed PMID: 25053444]
Hestbaek L, Leboeuf-Yde C, Kyvik KO. Are lifestyle-factors in adolescence predictors for adult low back pain? A cross-sectional and prospective study of young twins. BMC musculoskeletal disorders. 2006 Mar 15:7():27 [PubMed PMID: 16539729]
Level 2 (mid-level) evidenceLeboeuf-Yde C. Smoking and low back pain. A systematic literature review of 41 journal articles reporting 47 epidemiologic studies. Spine. 1999 Jul 15:24(14):1463-70 [PubMed PMID: 10423792]
Level 1 (high-level) evidenceEngers A, Jellema P, Wensing M, van der Windt DA, Grol R, van Tulder MW. Individual patient education for low back pain. The Cochrane database of systematic reviews. 2008 Jan 23:2008(1):CD004057. doi: 10.1002/14651858.CD004057.pub3. Epub 2008 Jan 23 [PubMed PMID: 18254037]
Level 1 (high-level) evidenceSkaggs DL, Early SD, D'Ambra P, Tolo VT, Kay RM. Back pain and backpacks in school children. Journal of pediatric orthopedics. 2006 May-Jun:26(3):358-63 [PubMed PMID: 16670549]
Chou R, Qaseem A, Owens DK, Shekelle P, Clinical Guidelines Committee of the American College of Physicians. Diagnostic imaging for low back pain: advice for high-value health care from the American College of Physicians. Annals of internal medicine. 2011 Feb 1:154(3):181-9. doi: 10.7326/0003-4819-154-3-201102010-00008. Epub [PubMed PMID: 21282698]
Saragiotto BT, Machado GC, Ferreira ML, Pinheiro MB, Abdel Shaheed C, Maher CG. Paracetamol for low back pain. The Cochrane database of systematic reviews. 2016 Jun 7:2016(6):CD012230. doi: 10.1002/14651858.CD012230. Epub 2016 Jun 7 [PubMed PMID: 27271789]
Level 1 (high-level) evidenceRoelofs PD, Deyo RA, Koes BW, Scholten RJ, van Tulder MW. Nonsteroidal anti-inflammatory drugs for low back pain: an updated Cochrane review. Spine. 2008 Jul 15:33(16):1766-74. doi: 10.1097/BRS.0b013e31817e69d3. Epub [PubMed PMID: 18580547]
Level 1 (high-level) evidencevan Tulder MW, Touray T, Furlan AD, Solway S, Bouter LM. Muscle relaxants for non-specific low back pain. The Cochrane database of systematic reviews. 2003:2003(2):CD004252 [PubMed PMID: 12804507]
Level 1 (high-level) evidenceUrquhart DM, Hoving JL, Assendelft WW, Roland M, van Tulder MW. Antidepressants for non-specific low back pain. The Cochrane database of systematic reviews. 2008 Jan 23:2008(1):CD001703. doi: 10.1002/14651858.CD001703.pub3. Epub 2008 Jan 23 [PubMed PMID: 18253994]
Level 1 (high-level) evidenceLong A, May S, Fung T. The comparative prognostic value of directional preference and centralization: a useful tool for front-line clinicians? The Journal of manual & manipulative therapy. 2008:16(4):248-54 [PubMed PMID: 19771197]
Level 2 (mid-level) evidenceAina A, May S, Clare H. The centralization phenomenon of spinal symptoms--a systematic review. Manual therapy. 2004 Aug:9(3):134-43 [PubMed PMID: 15245707]
Level 1 (high-level) evidenceClare HA, Adams R, Maher CG. Reliability of McKenzie classification of patients with cervical or lumbar pain. Journal of manipulative and physiological therapeutics. 2005 Feb:28(2):122-7 [PubMed PMID: 15800512]
Szpalski M, Gunzburg R, Balagué F, Nordin M, Mélot C. A 2-year prospective longitudinal study on low back pain in primary school children. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society. 2002 Oct:11(5):459-64 [PubMed PMID: 12384754]
Feldman DS, Straight JJ, Badra MI, Mohaideen A, Madan SS. Evaluation of an algorithmic approach to pediatric back pain. Journal of pediatric orthopedics. 2006 May-Jun:26(3):353-7 [PubMed PMID: 16670548]
Roffey DM, Ashdown LC, Dornan HD, Creech MJ, Dagenais S, Dent RM, Wai EK. Pilot evaluation of a multidisciplinary, medically supervised, nonsurgical weight loss program on the severity of low back pain in obese adults. The spine journal : official journal of the North American Spine Society. 2011 Mar:11(3):197-204. doi: 10.1016/j.spinee.2011.01.031. Epub [PubMed PMID: 21377601]
Level 3 (low-level) evidenceArnold E, La Barrie J, DaSilva L, Patti M, Goode A, Clewley D. The Effect of Timing of Physical Therapy for Acute Low Back Pain on Health Services Utilization: A Systematic Review. Archives of physical medicine and rehabilitation. 2019 Jul:100(7):1324-1338. doi: 10.1016/j.apmr.2018.11.025. Epub 2019 Jan 24 [PubMed PMID: 30684490]
Level 1 (high-level) evidenceHajihasani A, Rouhani M, Salavati M, Hedayati R, Kahlaee AH. The Influence of Cognitive Behavioral Therapy on Pain, Quality of Life, and Depression in Patients Receiving Physical Therapy for Chronic Low Back Pain: A Systematic Review. PM & R : the journal of injury, function, and rehabilitation. 2019 Feb:11(2):167-176. doi: 10.1016/j.pmrj.2018.09.029. Epub 2019 Feb 11 [PubMed PMID: 30266349]
Level 2 (mid-level) evidence