 Mohs Micrographic Surgery: Design and Execution of Tunneled Flaps
Mohs Micrographic Surgery: Design and Execution of Tunneled Flaps
Introduction
Mohs micrographic surgery is a procedure used to treat skin cancers. The procedure removes cancer cells, achieving a clear surgical margin, while preserving as much healthy tissue as possible. Mohs micrographic surgery is recommended for aggressive infiltrating tumors or those located in cosmetically or functionally sensitive areas, such as the head, neck, hands, feet, pretibial area, and genitalia, where tissue-sparing treatment is preferred. This type of surgery is most frequently used for basal cell carcinoma, squamous cell carcinoma, and, increasingly, melanoma in situ.[1][2][3] After tumor removal, Mohs surgeons face the challenge of repairing the surgical defect left by skin cancer excision. Depending on the size, shape, and location of the surgical defect; skin texture characteristics; and patient comorbidities, the surgeon chooses the most functionally and cosmetically sensitive wound repair.[4][5]
Broadly, options for repairing surgical defects include secondary healing, linear closure, skin grafts, and skin flaps. Secondary healing allows the wound to heal naturally without surgical intervention to close the defect. Secondary healing may offer excellent cosmetic results in areas where the skin is depressed compared to surrounding structures and in areas of concavity, such as the temples, nasolabial folds, or conchal bowl. Linear repairs involve closing a wound primarily side-to-side, resulting in a straight line–shaped scar. Skin grafting is a surgical procedure in which a piece of skin is transplanted from one area of the body to cover a surgical defect. For facial defects, skin graft donor sites typically include preauricular, postauricular, or, for larger defects, the clavicle or abdomen. Skin grafts are often used for large defects to avoid distortion of adjacent structures or if there is concern that an aggressive tumor may recur. This approach helps avoid further tissue manipulation and distortion that could occur with skin rearrangement during flap procedures. Artificial skin graft substitutes from porcine, placenta, cadaver, or fish also facilitate wound healing.[6][7][8]
Repairing a defect primarily or allowing the wound to heal secondarily can lead to contraction and distortion of key anatomical features, such as the eyes, nose, lips, and ears. In such cases, flaps are commonly used, especially for large defects or those located on the head and neck. Flaps are classified based on their principal tissue movement into rotation, advancement, transposition, and interpolation categories. On the face, where most key fixed structures are located centrally, many flaps are laterally based, where an existing tissue reservoir may be moved forward and medially. Rotation flaps use an adjacent tissue reservoir and rotate tissue around a pivot into the defect. Advancement flaps use adjacent tissue that is lifted and advanced into the defect. Transposition flaps use a nearby tissue reservoir and lift a pedicle of skin over an island of normal skin to inset into the defect.
Interpolation flaps are typically a two-stage procedure that uses a known tissue reservoir with a robust blood supply and rotates the tissue across normal skin to inset in the defect. These flaps are left in place, with the pedicle base connected to its blood supply for 3 weeks. After approximately 3 weeks, when the flap has adhered well and a new blood supply has been established, the pedicle is separated in a take-down procedure. Although this offers an excellent cosmetic result, it requires a multiweek and multiprocedure commitment from the patient, making it a challenging process.[9] A tunneled flap is a type of interpolation flap that involves moving the tissue to the donor site in a subcutaneous tunnel made under the skin. This technique often has the advantage of typically being a single-stage procedure, as the flap is not pulled across normal tissue requiring separation at a later date.[10]
Indications
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Indications
Skin flaps are indicated to repair large surgical defects or to minimize distortion of anatomically or cosmetically sensitive areas of the head and neck, such as eyelids, nose, lips, or mouth. Surgical defect repairs on the face can be particularly challenging due to this area's dynamic nature, function, mobility, and cosmetic importance. Surgeons often find it useful to conceptualize the face in terms of cosmetic units, dividing it into distinct regions based on location, fixed anatomical features, and functional considerations. This approach helps guide surgical planning to ensure repairs blend seamlessly with the face's natural contours and aesthetic characteristics. A surgical defect involving more than half of a cosmetic unit or important structures, such as cartilage, muscle, mucosa, and fat, may be classified as a more challenging or complex defect requiring a more complicated repair.[11]
When selecting a repair method, surgeons must carefully evaluate the defect's width, depth, and location; the presence of fixed anatomic structures; patient comorbidities; skin texture characteristics; and the availability of tissue reservoirs for movement. These factors ensure optimal functional and aesthetic outcomes. A tunneled island flap may be a good option for repairing large defects, minimizing distortion of fixed structures, or for patients wanting to limit the number of procedures. Tunneled flaps may be particularly useful for one-stage repairs in the central face where anatomical structures converge and on the ears with minimal distortion of facial architecture. In particular, they have been used to repair defects in the medial canthus, paranasal, and auricular areas.[10][12][13][14]
Tunneled flaps can minimize wound healing time compared to large defects left for secondary healing, thereby limiting the number of surgical repair procedures required. Compared to a standard island pedicle flap, the tunneled flap has a longer pedicle. The longer pedicle offers greater mobility and larger movement, allowing coverage of larger defects. In addition, preserving the integrity of the tunnel of normal skin helps enhance and maintain facial symmetry.[5]
Technique or Treatment
In a tunneled flap procedure, a subcutaneous tunnel is created adjacent to the defect, allowing a nearby stalk of skin to be moved through the tunnel to cover the defect left by tumor excision.
The procedure begins with tumor excision and confirmation of complete tumor clearance, either through Mohs micrographic surgery or permanent histological evaluation. A donor skin area of size and shape similar to the defect is selected nearby, and the pedicle is marked using a skin marker. To ensure flap survival, the pedicle must be designed with a width sufficient to maintain adequate blood supply (approximately 10-20 mm) and a length long enough to reach the defect without tension.
A full-thickness vertical incision is made, preserving underlying subcutaneous tissue and, in some cases, a portion of the muscle in the central pedicle. A tunnel is then created by lifting the subcutaneous plane with forceps and dissecting it with scissors to form a passage for the flap. The portion of the pedicle beneath the tunnel is typically de-epithelialized. The donor flap is passed through the tunnel and positioned into the recipient site with forceps. The flap is sutured into place, and the donor site is closed (see Image. Supraclavicular Artery Island Flap for Facial Reconstruction). Care is taken to avoid compressing, twisting, or overstretching the flap, as these factors can impede vascular perfusion and lead to necrosis or flap failure.[5]
Tunneled transposition flaps for auricular conchal bowl defects have demonstrated favorable aesthetic outcomes.[13] Common reconstruction options for conchal bowl defects include secondary healing, skin grafts, and flaps. Two-stage procedures, such as the flip-flop flap or cartilage-sacrificing flaps, are also frequently used for repair in this region. Tunneled flaps are particularly advantageous when tumor removal results in perichondrium loss. In such cases, secondary healing may be prolonged, and full-thickness skin grafts carry a high risk of failure unless the area is allowed to granulate or cartilage is removed to ensure adequate vascular perfusion. The tunnel often passes through the cartilage rather than subcutaneous tissue for auricular repair. The flap pedicle is typically harvested from the preauricular or postauricular region, depending on the defect's location, size, surrounding skin quality, and degree of sun damage.
A tunneled flap technique for conchal bowl reconstruction involves creating a subcutaneous tunnel between the tragus and antitragus and using a preauricular transposition flap with a caudal base. The segment of skin passed through the tunnel is de-epithelialized, allowing it to integrate with the recipient site. The preauricular donor site is closed linearly, and the distal end of the flap is sutured into the conchal bowl defect. This single-stage approach demonstrated excellent cosmetic outcomes, with a remarkable result observed 3 months postoperatively.[13]
Another option for conchal bowl reconstruction is a posterior-inferior-based postauricular donor pedicle tunneled through a subcutaneous channel at the defect's inferior edge. This technique offers the advantage of sun-protected donor skin, providing a good cosmetic texture and matching the conchal bowl. Another postauricular transcartilage tunneled flap, called the flip-flop flap, involves raising an island of skin from the mastoid and posterior ear surface.[15][5] These approaches provide effective aesthetic and functional repair options for conchal bowl defects.
For defects on the nasal root or medial canthus, a tunneled flap pedicle can be used to repair medially based surgical wounds. A lateral tissue reservoir supported by the superficial temporal artery may be tunneled medially for reconstruction. The glabellar region, supplied by the supratrochlear artery, serves as a viable tissue reservoir for nasal root defects.[16] A tunneled paramedian forehead flap using the supratrochlear artery minimizes the need for multiple procedures compared to the classic paramedian flap.[5][17] However, care must be taken to preserve the supraorbital nerve that runs superiorly from above the eyebrows to the scalp. Damage to this nerve during forehead surgery can lead to paresthesias, a risk that should be discussed with patients.
Tunneled flap pedicles have also been successfully taken laterally from the nasolabial fold to repair defects on the nasal tip, dorsum, or ala. This approach allows for a sebaceous tissue match to enhance cosmesis and discreetly places the donor site scar within the nasolabial groove. Unlike classic nasolabial cheek-to-nose flaps, tunneled paranasal flaps avoid complications such as blunting or fold elevation.[4] Tunneled flaps may rely on random vascularization, provided their length is less than 3 times their width. In cases like paramedian flaps, a named vessel, such as the supratrochlear artery, can be used for perfusion.[5][18]
Complications
Tunneled pedicle flaps are limited by the distance they can cover and the elevation they may cause above the pedicle. As with many skin flaps, tunnel flaps can also result in a trap door effect.[5] In some cases, this can be prominent and cosmetically unappealing. Oversizing the flap can result in bulkiness, tightness, or protrusion of the tissue tunnel. The trapdoor effect, or protrusion of the flap above the surrounding skin, can be minimized by designing a flap with a small base, undercutting the edges of the surrounding skin, undersize the flap by 20% to 25%, massaging the flap, and use of intralesional steroids. Primarily due to the flap causing elevation along the tunnel affecting the final cosmetic result, this flap is rarely used by plastic and dermatologic surgeons in favor of other more cosmetically pleasing closure techniques.[5][10][19]
Periorbital flaps carry the risk of ectropion, and perioral flaps have the risk of eclabium. Perinasal or auricular flaps with cartilage removal carry the risk of inadequate functional support, contracture, or collapse. Other possible complications of tunneled flap procedures include flap failure or necrosis, most commonly at the distal edge of the flap. General surgical risks such as bleeding, hematoma, infection, bruising, contracture, and scarring also apply. The risk of flap failure or poor blood supply increases with a longer pedicle length, an overly narrow pedicle base limiting blood flow, or patient-specific risk factors, such as smoking or diabetes mellitus. Smoking, in particular, poses the highest risk to flap viability by impairing blood perfusion. Patients should be strongly encouraged to cease smoking before surgery to minimize this risk and optimize outcomes.
Clinical Significance
Tunneled flaps hold significant clinical value because they can achieve functional and cosmetic reconstruction of surgical defects while preserving nearby tissue integrity. These flaps are particularly beneficial in areas where tissue conservation is crucial, such as the face, ears, or other anatomically complex regions. By creating a subcutaneous or transcartilage tunnel to transfer a vascularized flap to the defect, this technique ensures a reliable blood supply and promotes optimal healing with minimal risk of wound dehiscence or necrosis.
Clinically, tunneled flaps are used to repair defects in cosmetically sensitive areas such as the nasal root, medial canthus, conchal bowl, and nasal tip. These flaps allow surgeons to use tissue reservoirs with similar texture, color, and sebaceous quality, enhancing overall aesthetic outcomes. In addition, tunneled flaps reduce donor site morbidity and often hide scar lines in natural anatomic concavities, such as the nasolabial fold or postauricular region.
This technique is particularly advantageous for managing complex defects caused by tumor excision, trauma, or congenital anomalies. The versatility of tunneled flaps allows for tailored repair in cases where secondary healing, skin grafts, or other flaps may not provide satisfactory results. Furthermore, using vascularized pedicles minimizes the risk of infection and enhances wound healing, making tunneled pedicle flaps a cornerstone in reconstructive surgery for challenging defects.
Enhancing Healthcare Team Outcomes
Effective execution of Mohs micrographic surgery with tunneled flap reconstruction requires a multidisciplinary approach to optimize patient-centered care, outcomes, and safety. Clinicians and surgeons must possess advanced skills in defect mapping, flap design, and tunneling techniques to ensure vascular integrity and achieve functional and cosmetic success. Nurses are critical in preoperative education, assisting during surgery, and monitoring for postoperative complications such as infection or flap necrosis. Pharmacists contribute by managing perioperative medications, including antibiotics and analgesics, and advising on anticoagulation management for patients at risk of bleeding. Advanced practitioners assist with patient evaluations, counseling, and setting realistic expectations. Collaborative interprofessional communication ensures thorough surgical planning, tailored patient care, and adherence to postoperative regimens, ultimately enhancing safety, outcomes, and team performance.
Although many Mohs micrographic surgical repairs can be completed in an outpatient setting under local anesthesia, some cases require referral to specialists for operating room-based procedures under general anesthesia. For example, extensive eyelid involvement affecting the tarsal plate, lacrimal apparatus, or levator muscle warrants referral to an oculoplastic surgeon. Large or complex nasal defects, particularly those involving the upper nose, may require an otolaryngologist, whereas oral involvement often necessitates oral maxillofacial or otolaryngology expertise. Total ear defects may need plastic surgery for rib grafting.[20][16] Recognizing when to involve specialists ensures optimal outcomes, especially for tumors in anatomically or functionally critical areas, underscoring the importance of a coordinated, multidisciplinary approach to care.
Media
(Click Image to Enlarge)
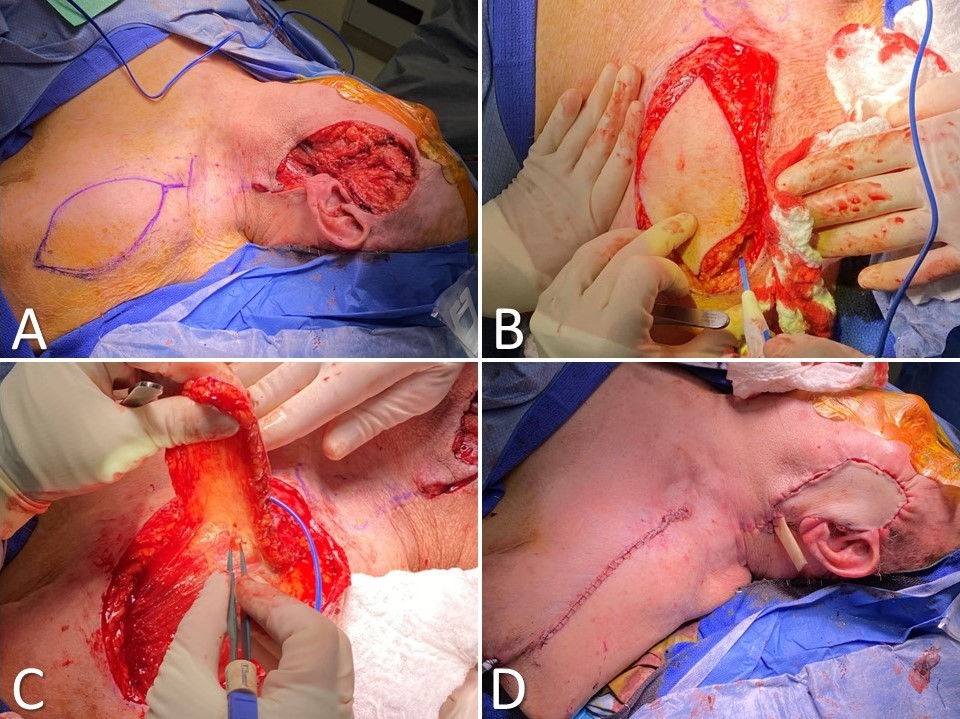
Supraclavicular Artery Island Flap for Facial Reconstruction. (A) Parotidectomy and skin defect due to dermatosarcoma with supraclavicular artery island flap (SCAIF) drawn out incorporating the supraclavicular artery; (B) the skin paddle is circumcised down to the level of the deltoid muscle; (C) the flap is elevated, ensuring the vascular pedicle remains intact medially; (D) the flap is tunneled into the defect and inset over a Penrose drain, whereas the donor site is closed primarily.
Contributed by MW Herr, MD; KG Anderson MD, FACS; and MH Hohman, MD, FACS
References
Prusinski Fernung LE, Micklus NE, Potter KA. Low Rate of Upstaging of Melanoma in Situ When Central Debulk Sent for Permanent Sections During Mohs Micrographic Surgery. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2024 Dec 1:50(12):1212-1213. doi: 10.1097/DSS.0000000000004321. Epub 2024 Jul 9 [PubMed PMID: 38984533]
Contestable JJ, Lim GFS, Willenbrink T, Zitelli JA, Brodland DG. Mohs for Melanoma: A Review of MART-1 Frozen Section Interpretation. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2024 Dec 1:50(12):1102-1108. doi: 10.1097/DSS.0000000000004312. Epub 2024 Jul 8 [PubMed PMID: 38975654]
Taylor MA, Thomas SI, Fernandez JM, Wackel M, Sharma D, Voss VB, Wysong A. Enhanced disease-specific survival in lentigo maligna melanoma patients treated with Mohs surgery over wide local excision: A retrospective cohort analysis of the Surveillance, Epidemiology, and End Results database. Journal of the American Academy of Dermatology. 2024 Nov:91(5):939-941. doi: 10.1016/j.jaad.2024.06.059. Epub 2024 Jul 3 [PubMed PMID: 38969012]
Level 2 (mid-level) evidenceMoro-Bolado F, Carmona-Rodríguez M, Alwattar-Ceballos O, Martínez-Montalvo L, Rogel-Vence M, Sánchez-Caminero P, Romero-Aguilera G. Tunneled Island Flaps for the Reconstruction of Nasal Defects: A 21-Case Series. Journal of clinical medicine. 2023 Dec 2:12(23):. doi: 10.3390/jcm12237473. Epub 2023 Dec 2 [PubMed PMID: 38068525]
Level 2 (mid-level) evidenceRogel-Vence M, Carmona-Rodríguez M, Moro-Bolado F, González-Ruiz L, Sánchez-Caminero MP, Romero-Aguilera G. Versatility of Tunneled Island Flaps for the Reconstruction of Facial Defects. Actas dermo-sifiliograficas. 2022 Feb:113(2):123-133. doi: 10.1016/j.ad.2021.06.001. Epub 2021 Jun 25 [PubMed PMID: 35249690]
Garcia N, Jiminez V, Graham L, Huang C. Unique Usages of Dehydrated Human Amnion Chorion Membrane Allografts in Dermatology. Journal of drugs in dermatology : JDD. 2023 Dec 1:22(12):1228-1231. doi: 10.36849/JDD.7115. Epub [PubMed PMID: 38051836]
Wilmas KM, Patel J, Silapunt S, Doan HQ, Migden MR. The Use of a Dehydrated Complete Human Placental Membrane Allograft for Mohs Surgical Defects of the Nose. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2023 Apr 1:49(4):343-347. doi: 10.1097/DSS.0000000000003711. Epub 2023 Feb 13 [PubMed PMID: 36799879]
Suski M. Use of intact fish skin xenograft in the closure of a large scalp Mohs defect with exposed cranium in an irradiated area. Journal of wound care. 2024 Mar 1:33(Sup3):S15. doi: 10.12968/jowc.2024.33.Sup3.S15. Epub [PubMed PMID: 38457295]
Goyal K, Swick M, Mattox A, Pelster MW, Maher IA. Cheek Interpolation Flaps: A Review of the Uses and Execution of Melolabial and Paranasal Interpolation Flaps. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2021 Feb 1:47(2):200-205. doi: 10.1097/DSS.0000000000002621. Epub [PubMed PMID: 33565774]
Cook JL. Tunneled and transposed island flaps in facial reconstructive surgery. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2014 Sep:40 Suppl 9():S16-29. doi: 10.1097/DSS.0000000000000119. Epub [PubMed PMID: 25158873]
Wong N, Kossintseva I. Gaining Large Coverage With Small Island Pedicle Flaps in Tight Cosmetic Subunits: Taking Advantage of Rotation and Pincer Principles on the Nasal Ala. Journal of cutaneous medicine and surgery. 2020 Mar/Apr:24(2):154-160. doi: 10.1177/1203475420902044. Epub 2020 Feb 27 [PubMed PMID: 32103678]
Gouveia MP, Gouveia AI, Brinca A, Vieira R. Tunneled island flaps in facial defects reconstruction. Anais brasileiros de dermatologia. 2017:92(5 Suppl 1):151-153. doi: 10.1590/abd1806-4841.20175565. Epub [PubMed PMID: 29267477]
Marsidi N, Genders RE. Tunneled transposition flap for conchal defect. Journal of the American Academy of Dermatology. 2020 Jun:82(6):e197-e198. doi: 10.1016/j.jaad.2019.03.035. Epub 2019 Mar 21 [PubMed PMID: 30905799]
Caretto AA, Colavincenzo C, Gentileschi S. Tunnelised superiorly based preauricular flap and conchal cartilage graft for antihelix reconstruction. BMJ case reports. 2024 Feb 13:17(2):. doi: 10.1136/bcr-2023-259025. Epub 2024 Feb 13 [PubMed PMID: 38350704]
Level 3 (low-level) evidenceFader DJ, Johnson TM. Ear reconstruction utilizing the subcutaneous island pedicle graft (flip-flop) flap. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 1999 Feb:25(2):94-6 [PubMed PMID: 10037510]
Gladstone HB, Stewart D. An algorithm for the reconstruction of complex facial defects. Skin therapy letter. 2007 Mar:12(2):6-9 [PubMed PMID: 17393051]
Level 3 (low-level) evidenceBrundridge WL, Sismanis DN, Altman AH, DeBacker CM, Holck DEE. Single-staged Tunneled Forehead Flap for Medial Canthal and Eyelid Reconstruction. Plastic and reconstructive surgery. Global open. 2022 Apr:10(4):e4223. doi: 10.1097/GOX.0000000000004223. Epub 2022 Apr 22 [PubMed PMID: 35475283]
Mukovozov IM, Laroche A, Wong A, Zloty D. Viability and Cosmesis of Right Angle and Vertical Paramedian Forehead Flaps Are Equivalent: A Retrospective Quantitative Study. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2022 Jul 1:48(7):716-719. doi: 10.1097/DSS.0000000000003476. Epub 2022 May 16 [PubMed PMID: 35576435]
Level 2 (mid-level) evidenceKrishnan RS, Clark DP, Donnelly HB. Tunneled transposition flap for reconstruction of defects of the nasal ala. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2007 Dec:33(12):1496-501 [PubMed PMID: 18076618]
Blumenthal SR, Swick M, Bayan CA, Ramanathan D, Maher I. Complex Eyelid Reconstruction: A Practical Guide for the Mohs Surgeon. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2022 Sep 1:48(9):916-923. doi: 10.1097/DSS.0000000000003526. Epub 2022 Jul 5 [PubMed PMID: 36054043]