[1]
Seeras K, Qasawa RN, Ju R, Prakash S. Anatomy, Abdomen and Pelvis: Anterolateral Abdominal Wall. StatPearls. 2024 Jan:():
[PubMed PMID: 30247850]
[2]
Klaassen Z, Marshall E, Tubbs RS, Louis RG Jr, Wartmann CT, Loukas M. Anatomy of the ilioinguinal and iliohypogastric nerves with observations of their spinal nerve contributions. Clinical anatomy (New York, N.Y.). 2011 May:24(4):454-61. doi: 10.1002/ca.21098. Epub 2011 Jan 3
[PubMed PMID: 21509811]
[3]
Willard FH, Vleeming A, Schuenke MD, Danneels L, Schleip R. The thoracolumbar fascia: anatomy, function and clinical considerations. Journal of anatomy. 2012 Dec:221(6):507-36. doi: 10.1111/j.1469-7580.2012.01511.x. Epub 2012 May 27
[PubMed PMID: 22630613]
[4]
Cho HM, Park DS, Kim DH, Nam HS. Diagnosis of Ilioinguinal Nerve Injury Based on Electromyography and Ultrasonography: A Case Report. Annals of rehabilitation medicine. 2017 Aug:41(4):705-708. doi: 10.5535/arm.2017.41.4.705. Epub 2017 Aug 31
[PubMed PMID: 28971057]
Level 3 (low-level) evidence
[5]
Whiteside JL, Barber MD, Walters MD, Falcone T. Anatomy of ilioinguinal and iliohypogastric nerves in relation to trocar placement and low transverse incisions. American journal of obstetrics and gynecology. 2003 Dec:189(6):1574-8; discussion 1578
[PubMed PMID: 14710069]
[6]
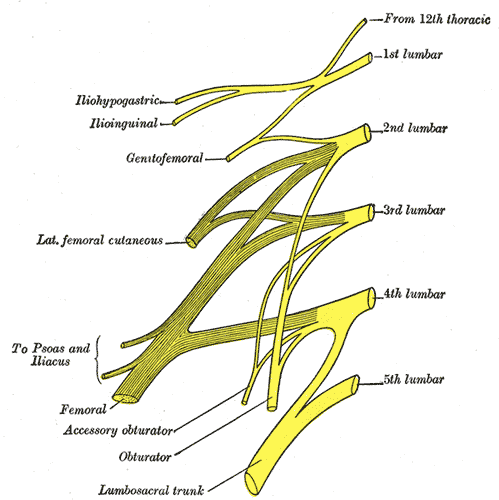
Iwanaga J, Simonds E, Schumacher M, Kikuta S, Watanabe K, Tubbs RS. Revisiting the genital and femoral branches of the genitofemoral nerve: Suggestion for a more accurate terminology. Clinical anatomy (New York, N.Y.). 2019 Apr:32(3):458-463. doi: 10.1002/ca.23327. Epub
[PubMed PMID: 30592097]
[7]
Ellis J, Schneider JR, Cloney M, Winfree CJ. Lateral Femoral Cutaneous Nerve Decompression Guided by Preoperative Ultrasound Mapping. Cureus. 2018 Nov 28:10(11):e3652. doi: 10.7759/cureus.3652. Epub 2018 Nov 28
[PubMed PMID: 30723651]
[8]
Yoshida T, Nakamoto T, Kamibayashi T. Ultrasound-Guided Obturator Nerve Block: A Focused Review on Anatomy and Updated Techniques. BioMed research international. 2017:2017():7023750. doi: 10.1155/2017/7023750. Epub 2017 Feb 9
[PubMed PMID: 28280738]
[9]
Clifton W,Nicolas Cruz CF,Dove C,Damon A,Pichelmann M,Nottmeier E, Abdominal wall paresis after posterior spine surgery: An anatomic explanation. Clinical neurology and neurosurgery. 2019 Nov;
[PubMed PMID: 31605897]
[10]
Jelinek LA, Scharbach S, Kashyap S, Ferguson T. Anatomy, Abdomen and Pelvis: Anterolateral Abdominal Wall Fascia. StatPearls. 2024 Jan:():
[PubMed PMID: 29083814]
[11]
Dibra FF, Prieto HA, Gray CF, Parvataneni HK. Don't forget the hip! Hip arthritis masquerading as knee pain. Arthroplasty today. 2018 Mar:4(1):118-124. doi: 10.1016/j.artd.2017.06.008. Epub 2017 Aug 12
[PubMed PMID: 29560406]
[14]
Dragieva P, Zaharieva M, Kozhuharov Y, Markov K, Stoyanov GS. Psoas Minor Muscle: A Cadaveric Morphometric Study. Cureus. 2018 Apr 8:10(4):e2447. doi: 10.7759/cureus.2447. Epub 2018 Apr 8
[PubMed PMID: 29888151]
[15]
Wong TL, Kikuta S, Iwanaga J, Tubbs RS. A multiply split femoral nerve and psoas quartus muscle. Anatomy & cell biology. 2019 Jun:52(2):208-210. doi: 10.5115/acb.2019.52.2.208. Epub 2019 Jun 30
[PubMed PMID: 31338239]
[16]
Khalid S, Iwanaga J, Loukas M, Tubbs RS. Split Femoral Nerve Due to Psoas Tertius Muscle: A Review with Other Cases of Variant Muscles Traversing the Femoral Nerve. Cureus. 2017 Aug 9:9(8):e1555. doi: 10.7759/cureus.1555. Epub 2017 Aug 9
[PubMed PMID: 29021927]
Level 3 (low-level) evidence
[17]
Ndiaye A, Diop M, Ndoye JM, Ndiaye A, Mané L, Nazarian S, Dia A. Emergence and distribution of the ilioinguinal nerve in the inguinal region: applications to the ilioinguinal anaesthetic block (about 100 dissections). Surgical and radiologic anatomy : SRA. 2010 Jan:32(1):55-62. doi: 10.1007/s00276-009-0549-0. Epub 2009 Aug 26
[PubMed PMID: 19707710]
[18]
Tubbs RI, Gabel B, Jeyamohan S, Moisi M, Chapman JR, Hanscom RD, Loukas M, Oskouian RJ, Tubbs RS. Relationship of the lumbar plexus branches to the lumbar spine: anatomical study with application to lateral approaches. The spine journal : official journal of the North American Spine Society. 2017 Jul:17(7):1012-1016. doi: 10.1016/j.spinee.2017.03.011. Epub 2017 Mar 30
[PubMed PMID: 28365495]
[19]
Tubbs RS, Salter EG, Wellons JC 3rd, Blount JP, Oakes WJ. Anatomical landmarks for the lumbar plexus on the posterior abdominal wall. Journal of neurosurgery. Spine. 2005 Mar:2(3):335-8
[PubMed PMID: 15796359]
[20]
van Schoor AN, Boon JM, Bosenberg AT, Abrahams PH, Meiring JH. Anatomical considerations of the pediatric ilioinguinal/iliohypogastric nerve block. Paediatric anaesthesia. 2005 May:15(5):371-7
[PubMed PMID: 15828987]
[21]
Cheatham SW, Kolber MJ, Salamh PA. Meralgia paresthetica: a review of the literature. International journal of sports physical therapy. 2013 Dec:8(6):883-93
[PubMed PMID: 24377074]
[22]
Nobel W,Marks SC Jr,Kubik S, The anatomical basis for femoral nerve palsy following iliacus hematoma. Journal of neurosurgery. 1980 Apr
[PubMed PMID: 6445414]
[23]
Gilbert JD, Byard RW. Obturator hernia and the elderly. Forensic science, medicine, and pathology. 2019 Sep:15(3):491-493. doi: 10.1007/s12024-018-0046-z. Epub 2018 Nov 5
[PubMed PMID: 30397870]
[24]
Abdalmageed OS, Bedaiwy MA, Falcone T. Nerve Injuries in Gynecologic Laparoscopy. Journal of minimally invasive gynecology. 2017 Jan 1:24(1):16-27. doi: 10.1016/j.jmig.2016.09.004. Epub 2016 Sep 14
[PubMed PMID: 27639546]
[25]
Knockaert DC, D'Heygere FG, Bobbaers HJ. Ilioinguinal nerve entrapment: a little-known cause of iliac fossa pain. Postgraduate medical journal. 1989 Sep:65(767):632-5
[PubMed PMID: 2608591]
[26]
Toreih AA,Sallam AA,Ibrahim CM,Maaty AI,Hassan MM, Intercostal, ilioinguinal, and iliohypogastric nerve transfers for lower limb reinnervation after spinal cord injury: an anatomical feasibility and experimental study. Journal of neurosurgery. Spine. 2018 Nov 23
[PubMed PMID: 30497147]
Level 2 (mid-level) evidence