Continuing Education Activity
Lisfranc injuries describe a broad spectrum of foot injuries involving the Lisfranc (tarsometatarsal) joint complex. Injuries to this area include sprain, subluxation, joint widening with or without a fracture, dislocation, and crush injury. The condition varies in severity and typically results from trauma, such as from sports activities, falls, and motor vehicular crashes. Lisfranc joint injuries are uncommon and often misdiagnosed and mismanaged. Up to 20% of the cases are missed initially.
Early recognition and intervention are essential as Lisfranc injuries may produce midfoot arthritis, chronic pain, and functional foot instability as complications. This activity describes the pathophysiology, evaluation, and management of Lisfranc joint injuries and highlights the interprofessional team's role in caring for affected patients.
Objectives:
Identify signs and symptoms indicative of Lisfranc dislocations in foot injuries, distinguishing them from other midfoot pathologies.s.
Differentiate between various grades and types of Lisfranc injuries, categorizing them based on severity and associated complications.
Implement timely and tailored treatment plans for Lisfranc injuries, considering conservative and surgical approaches.
Collaborate with orthopedic surgeons, radiologists, and physical therapists in the multidisciplinary management of Lisfranc dislocations.
Introduction
The Lisfranc joint is formed by the articulation between the metatarsal bones (M1 to M5) and tarsal bones (cuneiforms C1 to C3 and cuboid). The Lisfranc ligament is a 3-component structure connecting the medial cuneiform (C1) to the 2nd metatarsal (M2).[1]
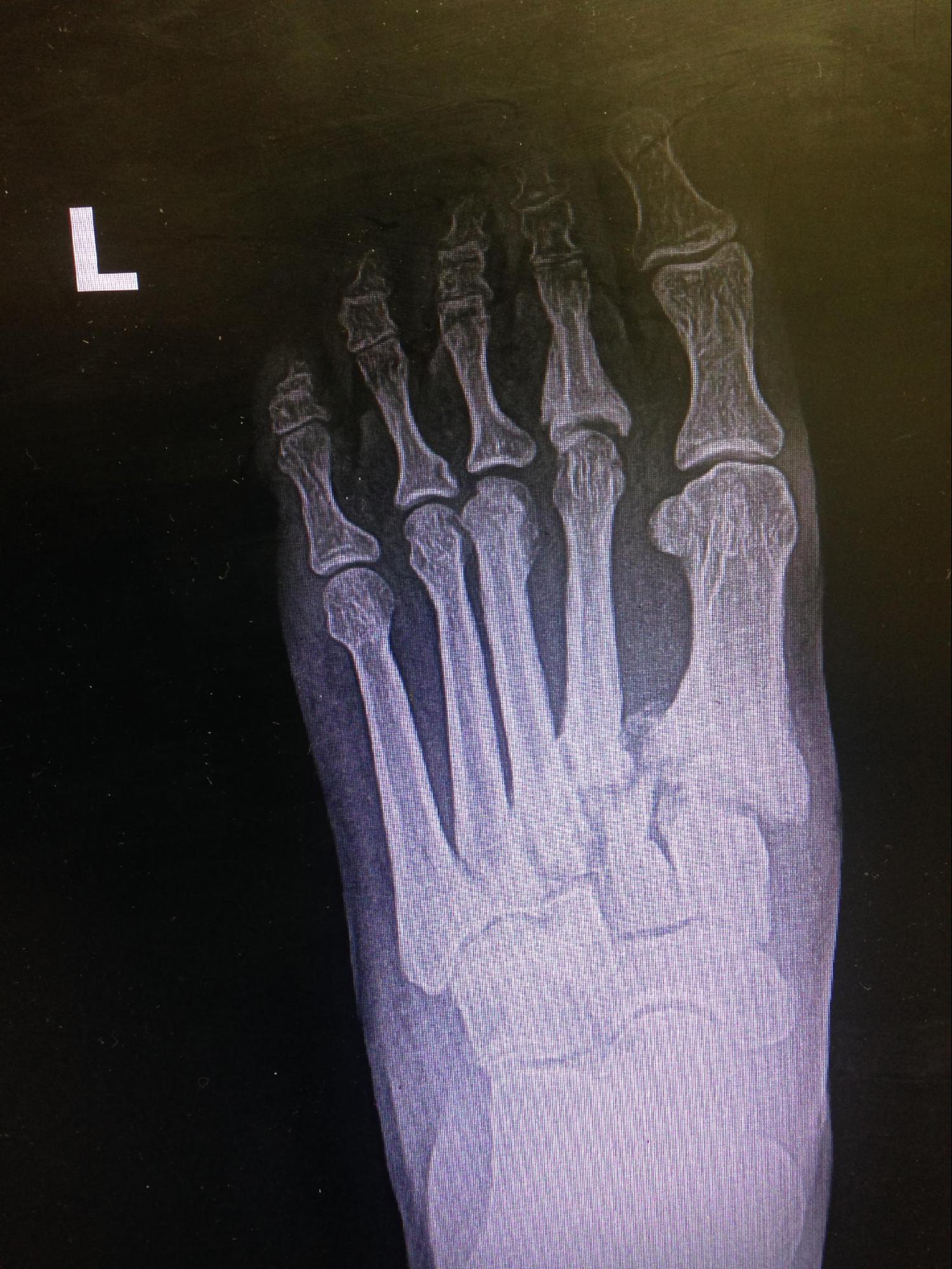
The Lisfranc joint can be disrupted by a sprain, subluxation, joint widening with or without fracture, dislocation, or crush injury (see Image. Lisfranc Dislocation).[2][3] Lisfranc injuries are uncommon, affecting 1 in every 55,000 people in the United States. However, these conditions are often misdiagnosed and mismanaged, and up to 20% are initially missed.[4] Lisfranc injuries produce disabling complications such as midfoot arthritis, chronic pain, and functional foot instability, especially when not managed properly.[5]
Etiology
Lisfranc injuries arise from high-energy and low-energy mechanisms and may be classified according to these mechanisms.[6]
Injuries arising from a high-energy mechanism arise from high-collision events like motor vehicular crashes and falls from heights. The immense impact produces a crush injury at high risk for acute complications such as an open fracture, compartment syndrome, wound dehiscence, and vascular disruptions. These Lisfranc joint injuries have no classic signs that can aid in diagnosis.[7]
Meanwhile, injuries arising from a low-energy mechanism are often associated with sports activities where the plantarflexed foot is subjected to an axial or rotational force. Plantarflexion weakens the dorsal foot ligaments, making the metatarsal bases and plantar capsule vulnerable to rotational injuries. This damage mechanism may occur in basketball, football, and rugby. A similar mechanism happens to equestrians, which may lead to transverse metatarsal dislocation.[8]
Certain anatomical variations have been shown to predispose individuals to Lisfranc injuries and their complications. One study reveals that the ratio between M2 and foot length is significantly smaller in more than 50% of patients who sustained Lisfranc injuries. Another study showed that a shorter 2nd tarsometatarsal joint height significantly increased the risk of developing an unstable Lisfranc injury.[9]
Epidemiology
Lisfranc injuries are relatively uncommon. These injuries account for 0.2% of all fractures, though the prevalence is likely higher because 20% of the cases are undiagnosed. The reported incidence of this injury is approximately 1 per 55,000 persons per year. Additionally, about 1 Lisfranc injury case is seen at a hospital for every 60,000 to 88,0000 of the population in a region.
This injury can occur in all ages but is more common in the 3rd decade of life and is 2 to 4 times more common in males. However, females are more likely to develop an unstable injury. Lisfranc injuries occur more frequently in athletes and have become increasingly diagnosed in this group due to widespread high-performance athletic training.[10]
High-energy injuries account for most cases, with 43% arising from motor vehicular crashes, 24% from falls from heights, 13% from crush injuries, and 10% from sports injuries.
Pathophysiology
Lisfranc injuries arise from damage to the structures comprising the Lisfranc joint complex. High- or low-impact trauma can produce lesions in the ligaments, bones, and soft tissues in the area. The injury results in abnormal weight distribution and biomechanical changes in the foot arch.
Risk factors for the development of Lisfranc injuries include a shallow mortise between the medial and lateral cuneiforms and a small M2-to-foot-length ratio, diabetes, and neuropathy.[11] Altered foot sensation, as in cases of diabetes and neuropathy, may lead to microtrauma in the Lisfranc joint area that can evolve into bigger injuries. Lisfranc injuries in these patients may also be associated with ulceration, infection, and Charcot neuroarthropathy, possibly requiring amputation.[12]
History and Physical
On history, patients typically present with midfoot pain after an acute injury, worsening with weight-bearing and the push-off phases of walking and running. A high- or low-energy mechanism may be identified as the cause of damage. Injury severity is often underestimated at the time of impact. Patients may delay consultation for the condition until complications emerge. A Lisfranc injury should be highly suspected if midfoot pain persists beyond 5 days and is associated with swelling and altered foot mechanics.[13]
The physical exam may reveal midfoot swelling and tenderness and plantar ecchymosis. Swelling and tenderness are most prominent over the tarsometatarsal joints. Foot widening and flattening are occasionally present. A "positive gap" or increased distance between the 1st and 2nd toes may be appreciated due to intercuneiform instability.
Pain may be elicited by weight-bearing and abducting the inverted forefoot. Stress-testing of the individual tarsometatarsal joints through the piano key test can reveal instability and reproduce pain. A single-limb toe rise test can uncover Lisfranc joint instability in weight-bearing patients. One should also ensure the injury is closed, as open fractures and dislocations are surgical emergencies.[14]
Evaluation
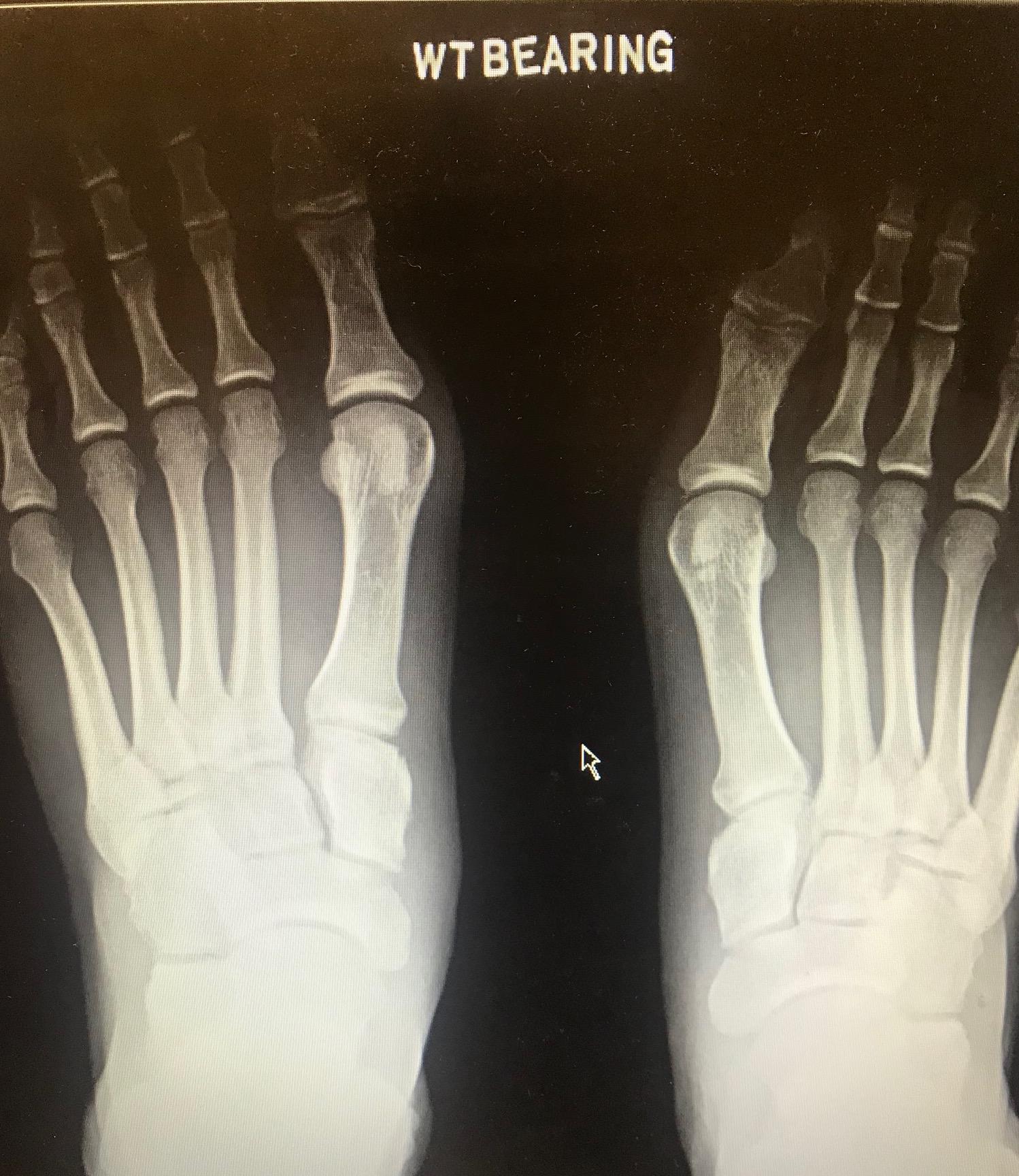
When a Lisfranc injury is suspected, anteroposterior (AP), 30° medial oblique (MO), and lateral weight-bearing radiographs of both feet should be obtained. Compliance with weight-bearing films is as difficult as they are essential due to their increased sensitivity in uncovering subtle Lisfranc injuries. Additionally, subtle diastasis is missed up to 50% of the time in non-weight-bearing radiographs. A contralateral radiograph is essential for comparison (see Image. Lisfranc Dislocation on Bilateral Weight-Bearing X-ray).[15]
Radiographic findings of a Lisfranc injury include the following:
- Misalignment between the medial edges of C2 and M2 on AP view
- Misalignment between the medial edges of the cuboid and M4 on MO view
- The presence of a bone chip in the 1st metatarsal space, also known as the fleck sign, indicating a Lisfranc ligament avulsion
- Diastasis of more than 2 mm between the M1 and M2 bases or a difference greater than 1 mm compared to the contralateral radiograph on AP view
- Dorsal or plantar displacement of the metatarsal bases in the lateral view
Plain radiographs are usually the initial imaging tests obtained for Lisfranc injuries. However, this modality's sensitivity in detecting the condition is only 84%. Thus, close to 20% of these injuries go undiagnosed. CT scans are often helpful adjuncts and are considered the second imaging modality of choice for Lisfranc injuries. CT scans can identify more subtle fractures, nondisplaced fractures, or minimal sub-dislocations not apparent on plain radiographs. This imaging test may also be helpful for surgical planning.
MRI helps evaluate the extent of soft tissue and ligamentous injury. The sagittal, long axial, and oblique coronal planes should be ordered in T1-weighted and fluid-sensitive sequences.[16]
Treatment / Management
Lisfranc injuries can be managed operatively or nonoperatively, depending on the clinical presentation. Regardless of the approach, treatment goals include restoring stability, minimizing long-term complications, and recovering normal foot function and mobility.
Conservative Management Of Lisfranc Injuries
Nonoperative treatment is recommended for the following cases:
- Anatomically stable and non-displaced injuries on weight-bearing radiographs
- Midfoot sprains without evidence of bony injury
- Patients who cannot tolerate surgery
Conservative treatment includes reduction, splinting, and aggressive elevation. The injured foot is placed in a short-leg cast or boot. Repeat evaluation and radiography should be performed after 2 weeks to rule out any diastasis that might require surgical management. The patient is advised to avoid bearing weight on the affected extremity for 6 weeks.
Symptom resolution and radiographic evidence of improvement after 6 weeks indicate that the patient may be ready to begin weight-bearing on the injured limb and rehabilitation. The patient may gradually resume physical activity using a full-length orthosis to distribute forces along the medial longitudinal arch.
Tenderness without radiologic evidence of displacement warrants an extension of booting or casting of the injured for at least 4 more weeks before considering rehabilitation. A ligamentous disruption requires a period of immobilization lasting up to 4 months.
Most candidates for nonoperative Lisfranc injury treatment recover in 2 to 4 months, though some patients can take up to 6 months.[17]
Surgical Management Of Lisfranc Injuries
Surgical intervention is indicated in the presence of Lisfranc joint instability, compartment syndrome, or an open fracture. Compartment syndrome is considered a medical emergency. This condition must be ruled out immediately as it requires prompt surgical fasciotomy. Open fractures also warrant immediate surgical intervention as they can lead to severe infection. Once these conditions are ruled out, the injured foot may be initially treated with closed reduction and immobilization to minimize soft-tissue swelling until definitive repair can be performed.
The definitive treatment of a Lisfranc injury may proceed in a staged approach, first with a closed or minimally invasive midfoot reduction and second with a permanent fixation. In the first stage, immobilization of the structures requires K-wire pinning or external fixation. In the second, open reduction internal fixation (ORIF), primary arthrodesis (PA), or tendon grafting is performed. In cases where staged treatment is unnecessary, surgery is delayed for 10 to 14 days until the foot swelling subsides.[18]
Operative procedures for Lisfranc injury have been debated for many years. Details about each technique and its relevance in the literature are described below.
- ORIF may involve either of the following techniques:
- Transarticular-screw placement: This traditional cheap option avoids extensive soft-tissue stripping. However, a single 3.5-mm transarticular screw has been shown to damage articular surfaces by 2 to 3.6% on average.[19][20]
- Dorsal-bridge plating: This technique provides superior functional outcomes compared to transarticular-screw placement. Dorsal bridge plating is useful in repairing highly comminuted injuries.
- Suture button: This newer technique has promising results but needs more evidence.
- PA: About 40% to 94% of patients who have undergone ORIF develop posttraumatic osteoarthritis, which is treated with PA. Compared to ORIF with transarticular-screw placement, PA provides increased function scores, postoperative activity level, and lower complication rate.[21] However, a recent systematic review comparing PA and the different ORIF techniques showed no statistically significant difference in return-to-work-or-activity rates, complications, and satisfaction rates.[22] Besides the contradiction in the literature, PA is preferred for Lisfranc injuries older than 6 weeks, which are prone to developing post-traumatic osteoarthritis.
- Tendon graft reconstructive surgery: This option is for purely ligamentous injuries. Evidence supporting this technique is limited to cadaveric or small case studies.[23][24]
Differential Diagnosis
The condition most commonly confused with a Lisfranc injury is a stable midfoot sprain, which providers may manage inadequately.[25] Due to their long-term complications and clinical presentation, Lisfranc injuries may also be misdiagnosed as a primary pes planus, posterior tibial tendon dysfunction, or osteoarthritis, which are all managed differently.[26]
Staging
Quenu and Kuss were the first to classify Lisfranc injuries in 1909 into 3 types: homolateral, isolated, and divergent. In 1982, Hardcastle modified this classification scheme, designating the complete displacement of all metatarsal bones as type A, the displacement of 1 or more metatarsal bones as type B, and divergent patterns as type C.
The most recent and widely accepted classification of these injuries is Myerson's classification, which is derived from the previous two. According to this Myerson, Lisfranc injuries must be categorized as follows:
- Type A: total lateral or dorsoplantar incongruity, with all 5 metatarsal bases displaced in the same direction
- Type B: isolated incongruity
- B1: medial M1 displacement
- B2: lateral or at least 1 of the lateral 4 metatarsals is displaced
- Type C
- C1: partial divergent
- C2: total divergent
- Type D
- D1: distance between C1 and M2 is 2 mm or less (does not require operative fixation)
- D2: distance between C1 and M2 is greater than 2 mm (requires surgery)
- D2L: purely ligamentous
- D2B: with bone avulsion
However, the above classification systems are normally useful only for high-impact Lisfranc injuries. In 2002, Nunley and Vertullo introduced a system for classifying athletic Lisfranc sprains based on clinical features, weight-bearing foot X-rays, and bone scintigraphy. Still, this classification is not widely adopted, possibly due to widespread MRI use for subtle injuries. Nunley and Vertullo's classification is as follows:
- Stage I: Lisfranc ligament sprain (no radiographic diastasis, no loss of arch length, positive bone scintigram)
- Stage II: overt injury of the Lisfranc ligament (1-5 mm diastasis, no loss of arch length)
- Stage III: stage II injury with damaged plantar ligaments and a possible fracture (greater than 5 mm diastasis, loss of midfoot arch length)
None of the classifications reliably provide a prognosis or guide treatment.
Prognosis
High-energy injuries have a poor prognosis and worse outcomes. Surgical delays greater than 6 months are also linked to worse functional outcomes. Type B injuries have a poorer prognosis than Types A and C as they are often diagnosed late.
Among surgical techniques for Lisfranc joint repair, PA has the best prognosis as it does not require a follow-up procedure or implant removal. Patients also return to activity faster after having this procedure, as compared to an ORIF.[27]
Complications
Acute complications following a Lisfranc injury include compartment syndrome, infection, thrombosis, and wounds. Chronic complications include failure of hardware, pes planus, and, most commonly, posttraumatic osteoarthritis. Up to 60% of patients experience posttraumatic osteoarthritis.
Postoperative and Rehabilitation Care
Weight-bearing exercises must be delayed for 6 to 8 weeks after surgery. After that, the patient may be reevaluated if they can be cleared to walk in a boot or short-leg cast, which must stay in place for another 6 weeks. By the 3rd month, most patients who have had a Lisfranc joint surgery recover well in supportive shoes and start physical therapy.
Consultations
Patients consulting at the Emergency Department for severe midfoot pain after a high-energy injury must be evaluated for emergent conditions like compartment syndrome. A surgeon specializing in foot and ankle injuries, such as an orthopedic or podiatric surgeon, can be consulted once emergencies have been ruled out. Patients with Lisfranc injuries eventually require rehabilitation and physical therapy.
Deterrence and Patient Education
Individuals engaged in activities that predispose them to Lisfranc joint disruption must be counseled in the following areas:
- Wearing proper footwear: Lisfranc injuries related to sports activities and certain occupations may be prevented by wearing specially designed footwear. Athletes can wear shoes that provide adequate midfoot support and protection during a sports activity.
- Increasing training intensity gradually: Gradual training regimens allow for proper conditioning, strengthening, and flexibility of the feet and ankles, reducing the risk of injuries.
- Using the proper movement techniques: Individuals must train in the proper movement techniques to minimize falls and awkward foot positions.
- Warming up and stretching adequately before a physical activity: These measures prepare the muscles, tendons, and ligaments for movement and reduce injury risk.
- Ensuring environmental safety: This step allows for environmental hazard identification that may predispose individuals to Lisfranc injuries. Following work guidelines carefully also helps prevent accidents.
- Maintaining strength and flexibility: Exercises that maintain foot and ankle strength, stability, and flexibility improve foot dynamics and help prevent injuries.
Coaches, trainers, and providers must help promote these preventive practices and remind athletes and workers to seek help immediately in the event of an injury.
Pearls and Other Issues
The key points in managing Lisfranc injuries are the following.[28][29]
-
Lisfranc injuries often result from high-energy or low-energy trauma.
- Lisfranc joint disruption has diverse presentations, making diagnosis difficult.
-
The imaging modality typically used initially is radiography. However, nearly 20% of Lisfranc injuries are missed using X-rays alone. CT and MRI can help improve diagnostic accuracy.
-
Treatment may be nonoperative or operative, depending on presentation and patient's status. Surgical indications include Lisfranc joint instability and association with emergent conditions like compartment syndrome. Among surgical techniques, PA is associated with better outcomes.
-
As with any other injuries, the timeliness of treatment helps minimize complications and disability.
-
Rehabilitation plays a significant role in recovery, focusing on restoring strength, mobility, and function. Close monitoring and follow-up are essential for assessing healing and addressing residual problems.
- Inadequately managed Lisfranc injuries can lead to chronic pain, instability, arthritis, or long-term foot dysfunction.
-
Each Lisfranc injury case is unique, requiring an individualized treatment plan based on injury severity, patient characteristics, and functional goals.
Understanding these pearls can help healthcare professionals optimize patient outcomes.
Enhancing Healthcare Team Outcomes
An interprofessional healthcare team ensures comprehensive care and optimal outcomes for patients with Lisfranc injuries. The interprofessional team for Lisfranc injuries may include the following:
-
Emergency department physicians: These providers assess and stabilize patients with acute foot injuries, including suspected Lisfranc injuries. They provide initial care and pain management and arrange for further evaluation by specialists.
-
Radiologists: Radiologists interpret imaging studies to help diagnose Lisfranc injuries accurately and guide treatment decisions.
- Nurses: These professionals work at various patient care levels to provide essential care, monitor patients, administer medications, and educate patients about postoperative care and rehabilitation.
-
Orthopedic surgeon or podiatrist: These specialists play a central role in managing Lisfranc injuries, as they determine the appropriate treatment strategy and perform procedures if necessary.
-
Anesthesiologists or anesthetists: These professionals administer anesthesia during surgery and can help manage pain during rehabilitation.
-
Physical therapists: These providers design personalized rehabilitation programs that restore foot function and allow patients to return to normal activities.
-
Occupational therapists: These professionals help patients attain functional independence activities and perform activities of daily living.
-
Primary care physicians: These providers coordinate care, assess patients on follow-up, and manage other medical conditions that may affect the recovery of patients with Lisfranc injuries.
-
Dietitians and nutritionists: These professionals help optimize the patient's nutritional status, especially if surgery and rehabilitation require specific dietary considerations.
Collaboration among these healthcare professionals ensures a comprehensive approach to managing Lisfranc injuries.