Continuing Education Activity
Herpes simplex virus (HSV) is common and is most often transmitted in childhood through direct physical contact. The most common infectious sites are oral mucosa (HSV-1) or genital mucosa (HSV-2). Rarely, the infection may be spread to the distal phalanx via direct inoculation and cause pain, swelling, erythema, and vesicles in an entity known as herpetic whitlow. This diagnosis is of particular importance given its close similarity on presentation to paronychia and its drastically differing treatment. This activity reviews the evaluation and management of herpetic whitlow and highlights the role of the interprofessional team in the care of patients with this condition.
Objectives:
- Describe the pathophysiology of herpetic whitlow.
- Review the presentation of herpetic whitlow.
- Outline the treatment of herpetic whitlow.
- Summarize the importance of improving care coordination among interprofessional team members in order to improve outcomes for patients affected by herpetic whitlow.
Introduction
Herpes simplex virus (HSV) is common and is most often transmitted in childhood through direct physical contact.[1] The most common infectious sites are oral mucosa (HSV-1) or genital mucosa (HSV-2). Rarely, the infection may be spread to the distal phalanx via direct inoculation and cause pain, swelling, erythema, and vesicles in an entity known as herpetic whitlow. This diagnosis is of particular importance given its close similarity on presentation to paronychia and its drastically differing treatment.[1][2][3]
Etiology
Herpetic whitlow is caused by the herpes simplex virus, type 1 or type 2.[4][5][6] Primary infection is through direct exogenous or autogenous inoculation through broken skin. Recurrent infection may occur when a patient gets herpetic whitlow by reactivation of latent virus months to years following primary infection.[7]
Epidemiology
This infection can be found in any age group. However, it is most common in children who suck their thumbs and in healthcare providers (medical or dental) who are exposed to patients’ oral mucosa while not wearing gloves.[8] The infection is most common in dental hygienists and respiratory therapists. Herpetic whitlow has also been documented in athletes who wrestle and adolescents and young adults following genital herpes exposure.[5] Its incidence has been reported at 2.4 cases per 100,000 people per year.[9]
Pathophysiology
Exposure to the herpes virus type 1 or type 2 results in viral invasion and replication in epidermal and dermal cells. This may progress to involve the sensory dorsal root ganglion, where latency is established. Infection usually occurs 2 to 20 days following exposure.[5] One or more vesicles appear around the nail, and they usually coalesce into large, honeycomb-like bullae in 5 to 6 days. They may spread proximally and may also involve the nail bed. The infection is usually self-limited and resolves in 2-4 weeks.[5][10]
Histopathology
The diagnosis of a herpetic infection can be made by performing a microscopic examination of the margin of the vesicles in a Tzanck test. After unroofing and swabbing vesicles to obtain a sample, it is stained (commonly with Giemsa) and shows characteristic multinucleated “balloon" giant cells. The nuclei of herpes simplex virus (HSV)-infected cells appear blue and homogenous. Negative staining of vesicle fluid may show herpes virus by electron microscopy. Monoclonal antibodies or polymerase chain reaction (PCR) confirm the diagnosis by immunofluorescence and also differentiate type 1 from type 2 herpes simplex virus.[11]
History and Physical
Herpetic whitlow is typically a clinical diagnosis. Patients may report local trauma preceding infection, especially to the nail cuticle, although they often deny a history of injury. There is often exposure to the herpes virus via autogenous or exogenous contact with cold sores (herpes labialis) or genital herpes infection. Coexisting primary oral herpetic lesions suggest autoinoculation.[5]
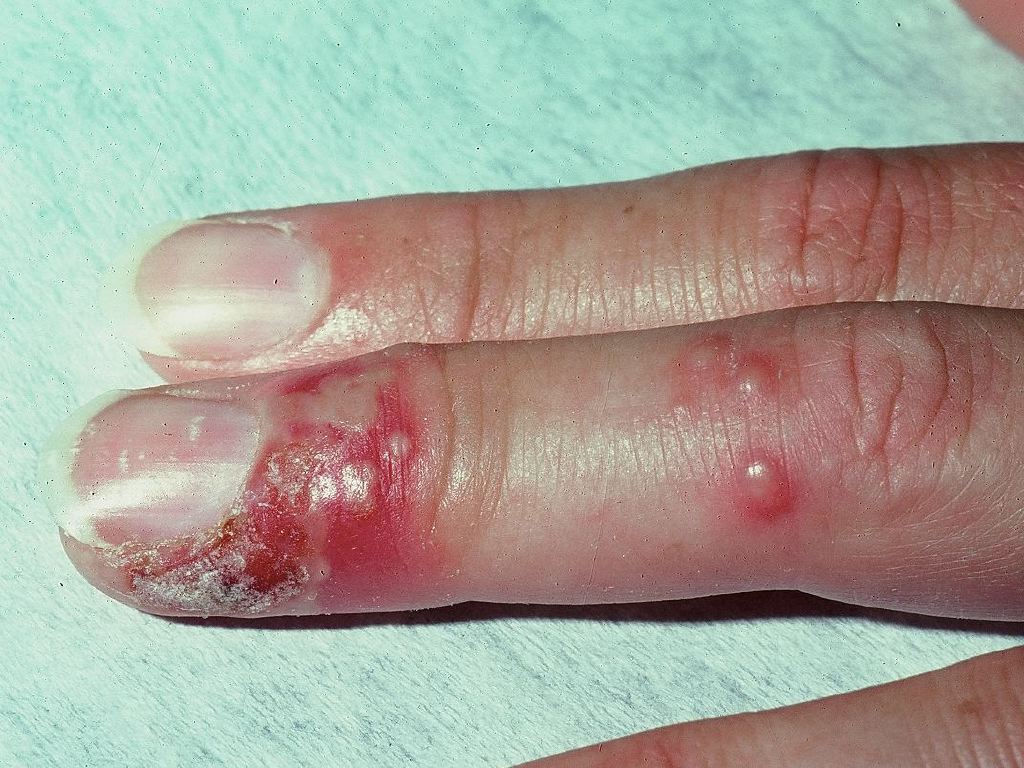
Patients will often experience pain and tingling in the finger before any skin changes (prodromal phase).[12] This will be followed by local tenderness, erythema, and edema with an initial crop of vesicles which are most common along the pulp and lateral aspect of the finger. The infection usually involves just one finger but has rarely been noted to involve several fingers. Vesicles usually coalesce into large, honeycomb-like bullae. They may spread proximally and may involve the nail bed where hemorrhagic or purpuric lesions may be noted. Patients will often report a disproportionate intensity of pain, particularly if there is nailbed involvement.[2] Fever, lymphadenitis, epitrochlear and axillary lymphadenopathy may be present.[13] Rarely, lymphedema of the hand and forearm may be present, although reports favor bacterial superinfection in most of these cases.
Vesicular fluid is clear early on but may become turbid, seropurulent, or hemorrhagic as it progresses. There should not be frank pus unless a bacterial superinfection is present. In immunocompromised patients (particularly acquired immunodeficiency syndrome with a CD4 count of less than 50), ulceration and necrosis may be seen.
Evaluation
The diagnosis of herpetic whitlow is typically made by the appearance of lesions and the patient’s history. If the diagnosis is unclear, there are multiple tests available for HSV. A viral culture can be sent by unroofing vesicles and swabbing fluid at the base. This method is about 50% sensitive overall. Vesicles contain the highest concentration of virus within the first 24 to 48 hours after they appear (89% positive). PCR testing is much more sensitive. Serology and direct fluorescent antibody testing are other tests that may be sent but are less common. A Tzank test consists of scraping the floor of a herpetic vesicle, staining the specimen, and looking for multinucleated "balloon" giant cells, with as high as approximately 70% sensitivity and high specificity for the disease.[14][15]
HIV testing should be considered in patients with atypical presentations and recurrent infections.[6]
Treatment / Management
Symptomatic relief and avoidance of secondary infection are the mainstays of therapy for herpetic whitlow. The natural course of the infection in an immunocompetent patient is a spontaneous resolution of symptoms in 2 to 4 weeks.[2] Incision and drainage should not be performed as it provides no symptomatic relief and may cause viremia and bacterial superinfection. There have been reports of significant pain relief following nail segment excision for decompression of vesicles along the nail bed.[1][5][8]
While there are few studies specific to herpetic whitlow, antivirals have been shown to shorten the duration of symptoms by up to 4 days in one study and decreased days of positive viral culture. Data is especially favorable if the antiviral is started within 48 hours of the onset of symptoms.[2] For recurrent herpetic whitlow, suppressive therapy with an antiviral agent may be helpful. Treatment with acyclovir, famciclovir, or valacyclovir has not been specifically compared. Antibiotics must be considered in a secondarily infected digit.
Differential Diagnosis
Herpetic whitlow is most commonly mistaken for paronychia (a localized bacterial abscess in the nail fold) or bacterial felon (digital pulp abscess).[1][14] The pale-yellow color of the vesicles may suggest pyogenic infection, but incision or needle aspiration will not demonstrate frank pus.
Other diagnoses on the differential include herpes zoster infections, which will involve the whole dermatome of the hand, and rarely, primary cutaneous Neisseria gonorrhoeae infection and Mycobacterium marinum infection.
Prognosis
Herpetic whitlow is classically self-limited and usually resolves in 2 to 4 weeks for primary infection.[2] After the acute stage, the pain abates, and the vesicles begin to dry and crust. Usually, the pain resolves in about 14 days, and the remaining skin changes continue to heal after that. Fingers and nails typically completely heal with no further issues, although there are reports of residual scarring, numbness, and hypersensitivity.[5]
A recurrent outbreak due to latent sensory ganglion infection has been noted in up to 30% to 50% of cases.[2]
Complications
Herpetic whitlow is frequently misdiagnosed as a bacterial paronychia or felon. This may result in procedures that increase the risk of bacterial superinfection, systemic infection, and even the possible development of herpes encephalitis. Other complications include:
- Scarring
- Numbness
- Hypersensitivity
- Occular spread
- Recurrent infection
Consultations
If unsure of the diagnosis, consider a dermatology or infectious disease consultation.
Deterrence and Patient Education
Patients should be educated that the virus can spread to other parts of their body or to other people via direct contact. Viral shedding is present until the epidermal lesion is healed, so patients should be counseled on the importance of wearing gloves or another protective barrier. The patient should also be counseled that the chance of recurrence is about 30% to 50%.[2] Patients should be encouraged to adhere to their medication regimen and to follow up if they develop signs of bacterial superinfection.
Enhancing Healthcare Team Outcomes
The diagnosis and management of herpetic whitlow are best accomplished with an interprofessional team that consists of a nurse practitioner, primary care provider, pediatrician, dermatologist, and an infectious disease expert. The disorder is diagnosed clinically and the management is supportive. The role of antiviral agents is still being debated but should be considered in immunocompromised patients.[10] For most immunocompetent patients, the infection spontaneously resolves in 2 to 4 weeks. Incision and drainage should not be performed as it provides no symptomatic relief and may cause viremia and bacterial superinfection. There have been reports of significant pain relief following nail segment excision for decompression of vesicles along the nail bed. Viral shedding is present until the epidermal lesion is healed, so patients should be counseled on the importance of wearing gloves or another protective barrier. The patient should also be counseled that the chance of recurrence is about 30% to 50%. [Level 5][2][10][2]