Continuing Education Activity
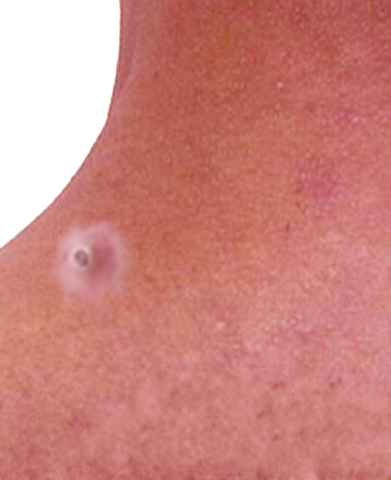
A dilated pore of Winer, first described by Louis H. Winer in 1954, is a commonly occurring benign adnexal tumor of follicular differentiation. Although most commonly located on the head and neck, a dilated pore of Winer can also be found on the trunk of middle-aged and elderly individuals (see Image. Dilated Pore of Winer). This activity reviews the cause of dilated pore of Winer, its presentation, and its treatment.
Objectives:
Identify the causes of dilated pore of Winer.
Apply the presentation of dilated pore of Winer.
Implement the treatment and management options available for dilated pore of Winer.
Apply some interprofessional team strategies for improving care and outcomes in patients with dilated pore of Winer.
Introduction
A dilated pore of Winer, first described by Louis H. Winer in 1954, is a commonly occurring benign adnexal tumor of follicular differentiation. Although most commonly located on the head and neck, a dilated pore of Winer can also be found on the trunk of middle-aged and elderly individuals. These clinically present as an asymptomatic, solitary, enlarged pore with a keratin plug and normal surrounding skin. Prognosis is excellent for these lesions as they are benign and typically do not require any further testing or work-up. Histopathologic evaluation can confirm the diagnosis in uncertain cases. Removal can be performed via excision for cosmetic purposes.
Etiology
Some have considered the dilated pore of Winer to simply be an epidermal inclusion cyst with reactive hyperplasia of its epithelial lining, and others have proposed it to be a variant of nevus comedonicus.[1][2] However, this lesion has been shown to be a distinct entity as an adnexal neoplasm of the follicular infundibulum.[3][4] The exact cause and pathophysiology of a dilated pore of Winer are unknown. Winer, in his original study, noted an association with a history of inflammatory cystic acne and other cystic processes.[5] Actinic damage has also been attributed to the development of these lesions.
Epidemiology
Although it occurs in both sexes, a dilated pore of Winer occurs more frequently in males than females and is also more frequent in whites. Most cases occur at the age of 40 and older; however, there are reports of dilated pores occurring as early as 20 years of age.
Histopathology
A dilated pore of Winer is characterized histopathologically by a markedly dilated follicular infundibulum extending deeply into the dermis. The cavity is filled with lamellar keratin material. It is lined by epithelium that is atrophic near the ostium and acanthotic at the deeper portion of the invagination. Radiating off the epithelium are regularly spaced, small, finger-like epithelial projections pushing into the surrounding dermis. These finger-like projections do not contain keratin cysts, ducts, or hair shafts.[1]
History and Physical
A dilated pore of Winer presents as a single, enlarged pore. The pore may be occluded by a keratin plug with softer, white, keratin material beneath. They are asymptomatic, and the surrounding skin appears normal; however, a background of actinic damage may be noted. Inflammation or infection, along with pain and swelling, can occur with manipulation. Although they have a predilection for the head and neck, particularly the face, they can also present on the trunk, most commonly the back. Patients are usually middle-aged or older and may report a previous history of severe acne.
Evaluation
A dilated pore of Winer is usually a clinical diagnosis. Histopathologic examination is not required but can be performed if the diagnosis is uncertain or in cases where the lesion is excised for cosmetic purposes. No other testing or work-up is needed.
Treatment / Management
No treatment is required for a dilated pore of Winer. Removal can be performed for cosmetic concerns. Excision in an elliptical fashion or by punch biopsy is usually curative.[6] Merely removing the keratin material can be done using a comedone extractor. However, keratin gradually re-accumulates within the lesion. Destructive techniques such as electrodesiccation, electrocautery, laser surgery, dermabrasion, and cryotherapy are less effective due to the deeply situated base of the invagination.[5] There are no effective medical treatments for these lesions.
Differential Diagnosis
A dilated pore of Winer and a typical nevus comedonicus can be easily differentiated clinically as the latter is a group of multiple keratin-filled openings. A solitary lesion of a nevus comedonicus and a dilated pore of Winer may only be differentiated histologically. The age of onset differs between the 2 lesions in that a dilated pore of Winer presents in the middle-aged to elderly while an NC presents at birth or during childhood.[2] A Pilar sheath acanthoma closely resembles a dilated pore of Winer clinically as both have a central dilated opening filled with keratin and both commonly occur on the face of older adults. Pilar sheath acanthomas occur most commonly on the upper cutaneous lip and have a more papular component compared to the dilated pore of Winer. Histologically the pilar sheath acanthoma has a more proliferative wall with thicker acanthotic projections radiating from the central cavity, which may contain keratin cysts, squamous eddies, or sebaceous ducts.[1] An epidermal inclusion cyst with a punctum may also clinically resemble a dilated pore of Winer and can also commonly occur on the face and trunk. Epidermal inclusion cysts have a more nodular component which is usually freely mobile and does not contain a keratin plug. They contain thick, cheesy keratin material, which has a foul odor when expressed. Histologically, epidermal inclusion cysts differ because they present as true cysts in the dermis with a lining of stratified squamous epithelium with a granular layer and filled with loose lamellar keratin. Although rare, some basal cell carcinomas (BCCs) can have an associated dilated pore. These large-pore BCCs tend to occur on the face of men and may be confused for a dilated pore of Winer. A large-pore BCC has a history of slowly enlarging over the years and may or may not have keratin debris. Patients tend to have thick sebaceous skin and have a history of tobacco use.[7]
Prognosis
Complete excision of the lesion is curative. Incomplete excision can result in the recurrence of the remaining infundibular lining. To date, there have been no reports of death associated with a dilated pore of Winer. Also, there have been no reports of syndromes associated with this entity. There have been rare case reports of other malignant cutaneous neoplasms, such as basal cell carcinoma and squamous cell carcinomas, arising in dilated pores of Winer. However, these are most likely coincidental.[8][9] There has been one case report of a trichoblastoma arising in a dilated pore of Winer.[10] Inflammation or infection of the surrounding skin can result from manipulation of the lesion by the patient in an attempt to remove the keratin plug.
Complications
Complications of surgical removal include scarring, infection, and bleeding. Infection risk after surgery can be minimized by using proper aseptic or clean technique. Infection before or following surgery can be treated using topical or oral antibiotics depending on severity.
Enhancing Healthcare Team Outcomes
A dilated pore of Winer is best managed by an interprofessional team that includes a dermatologist and a primary care provider. Although these lesions are benign, a biopsy may be required to rule out malignancy in individuals with an atypical presentation. The majority of patients seek medical help for cosmesis. The prognosis for most patients is excellent.