Continuing Education Activity
Allergic contact dermatitis (ACD) is a type 4 or delayed-type hypersensitivity response (DTH) by an individual’s immune system to a small molecule (less than 500 daltons), or hapten, that contacts a sensitized individual’s skin. ACD accounts for 20% of contact dermatoses, and allergens differ greatly based upon geography, personal habits, and hobbies, and often, the types of preservatives that are legally permissible. This activity illustrates the etiology, pathophysiology, and highlights the role of the interprofessional team in the management of allergic contact dermatitis.
Objectives:
- Outline the etiology of allergic contact dermatitis.
- Describe the clinical presentation, workup, and management of allergic contact dermatitis.
- Review that allergic contact dermatitis involves a complex interplay between biological, psychological, behavioral, and dietary factors.
- Explain the role of the interprofessional team in ensuring comprehensive patient and caregiver education to achieve better clinical outcomes.
Introduction
Allergic contact dermatitis (ACD) is a type 4 or delayed-type hypersensitivity response (DTH) by an individual’s immune system to a small molecule (less than 500 daltons), or hapten, that contacts a sensitized individual’s skin.[1] The initial or induction phase of ACD occurs when the hapten combines with a protein to form a complex that leads to the expansion of an allergen-specific T cell population; the name for this process is sensitization. During the elicitation phase, re-exposure to the antigen leads to the development of dermatitis. ACD accounts for 20% of contact dermatoses, and allergens differ greatly based upon geography, personal habits, and hobbies, and often, the types of preservatives that are legally permissible, such as quaternium-15 in the United States but not Europe.[2]
Etiology
Allergic contact dermatitis is an inflammatory disease of the skin that is caused by a type 4 hypersensitivity reaction. It results from the contact of an offending chemical or antigen with the skin, and the subsequent T-cell mediated response.[3] Morphology and location of the dermatitis are often the best indicators of the offending agent. For instance, when found around the wrist, it may indicate an allergic response to a bracelet or watchband.
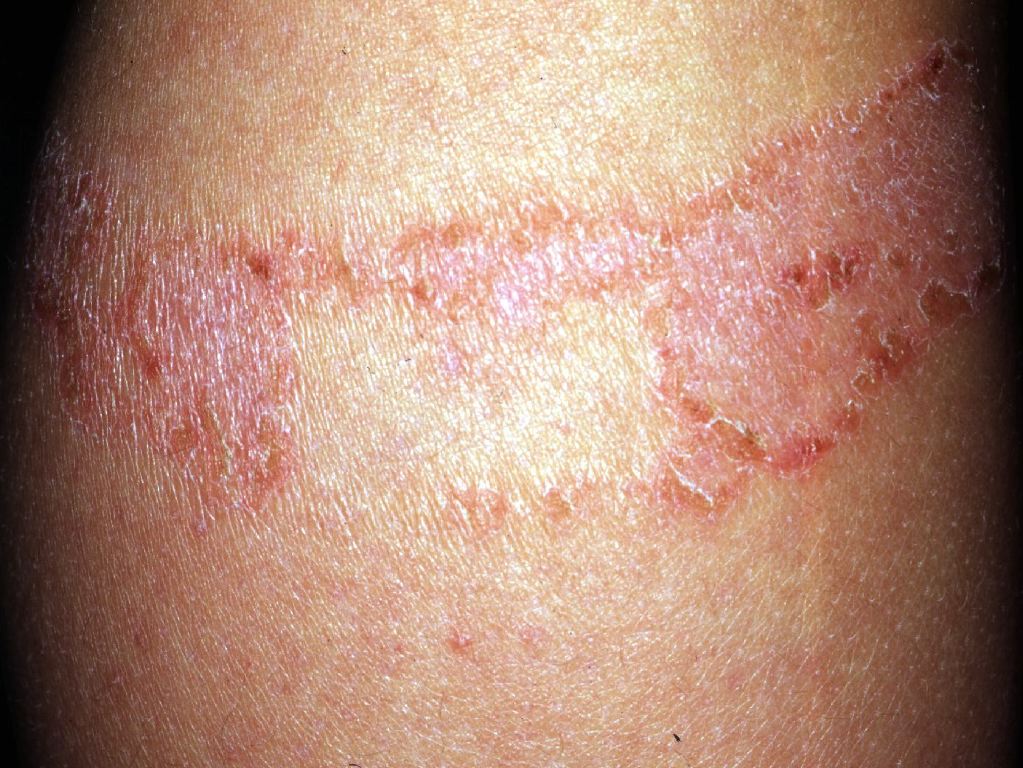
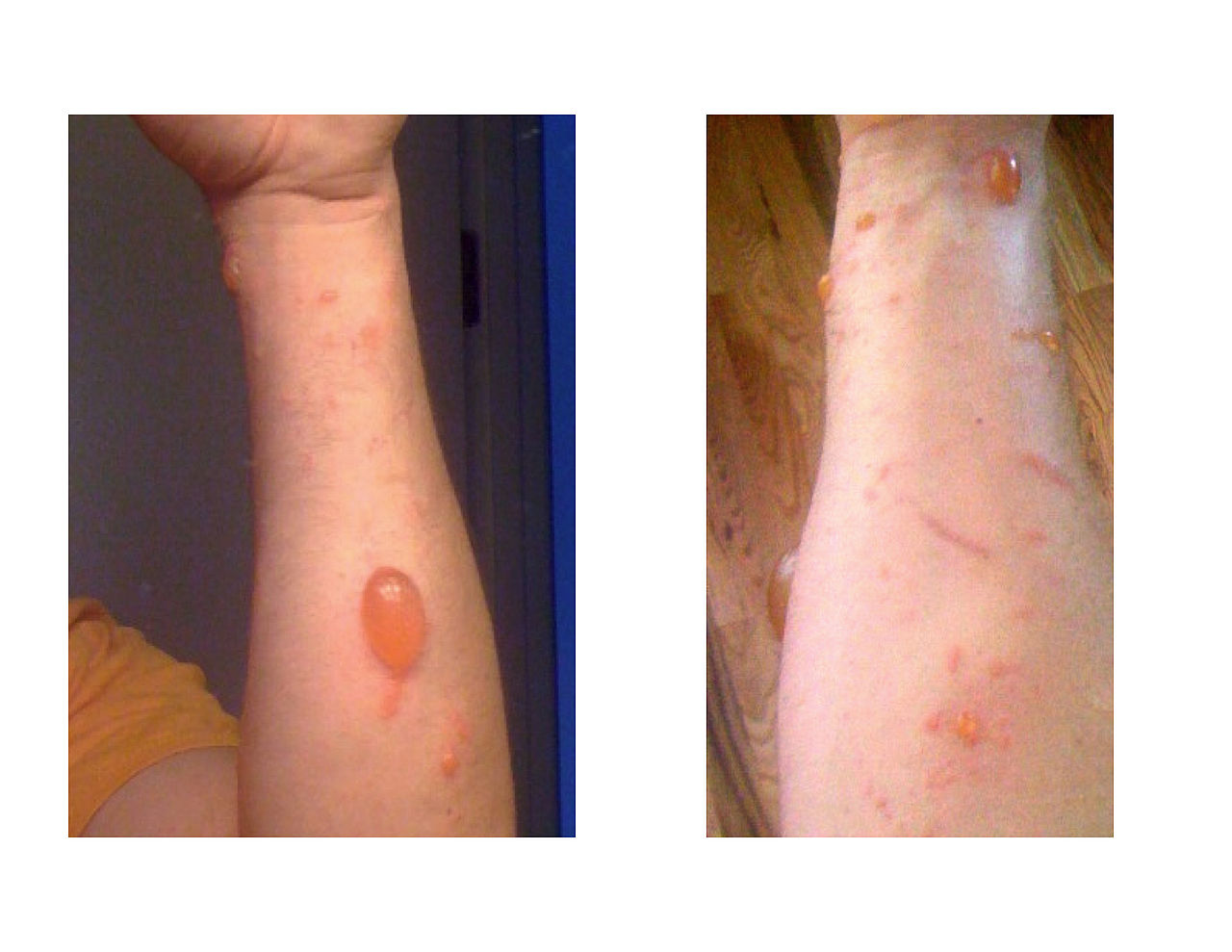
Poison ivy is a common cause of ACD and presents as linear streaks where the plant comes into contact with the skin.
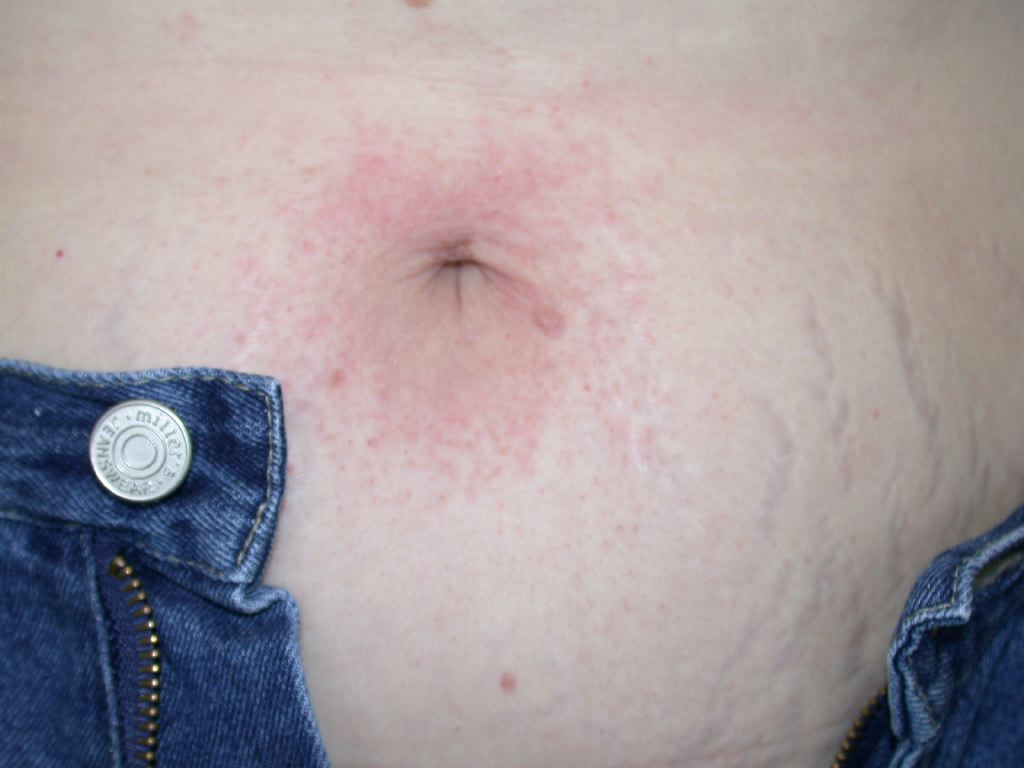
Nickel is another common cause of ACD and presents as dermatitis where necklaces and earrings containing nickel are worn.
Rubber gloves are also a common cause of chronic dermatitis.
Other agents include hair dyes, textile chemicals, preservatives, fragrances, sunscreens, and photo allergens.
Epidemiology
Allergic contact dermatitis is an inflammatory disease of the skin that is common in the general population. It is the most common type of occupational skin disease.[4]
The disorder is more common in women than in men. In the elderly, the condition often correlates with topical medications.
Pathophysiology
The pathophysiology of allergic contact dermatitis starts with the contact of the allergen to the skin. This allergen penetrates that stratum corneum of the skin and is taken up by Langerhans cells.[5] [6] The antigens subsequently undergo processing by these cells and get displayed on their surface. Langerhans cells then migrate towards regional lymph nodes. The antigens taken up by these cells come in contact with the adjacent T-lymphocytes. Due to the process of clonal expansion as well as cytokine-induced proliferation, antigen-specific T lymphocytes get created. These lymphocytes may then travel through the blood and into the epidermis. This process collectively is known as the sensitization phase of allergic contact dermatitis. The elicitation phase is what occurs after reexposure to the antigen takes place. The Langerhans cells containing the antigen interacts with the antigen-specific T-lymphocytes for that antigen, which triggers a cytokine-induced proliferation process. This proliferation, in turn, creates a localized inflammatory response.
Histopathology
The diagnosis of allergic contact dermatitis is usually established by a combination of history and physical examination, clinical presentation, and a positive patch test. If further evaluation is required, a skin biopsy of an affected area of skin will typically demonstrate spongiosis. However, this finding is unlikely to facilitate differentiation of ACD from other eczematous dermatologic disorders. [7]
Toxicokinetics
The intensity of the inflammatory response in allergic contact dermatitis is dependent on both the sensitizing ability of the allergen and the concentration of the allergen present. Poison ivy is an example of a strong sensitizer that can create an intense inflammatory response, even in small concentrations.[8]
History and Physical
Obtain a thorough history of occupation, hobbies, medications, lifestyle, use of fragrances, and perfumes.
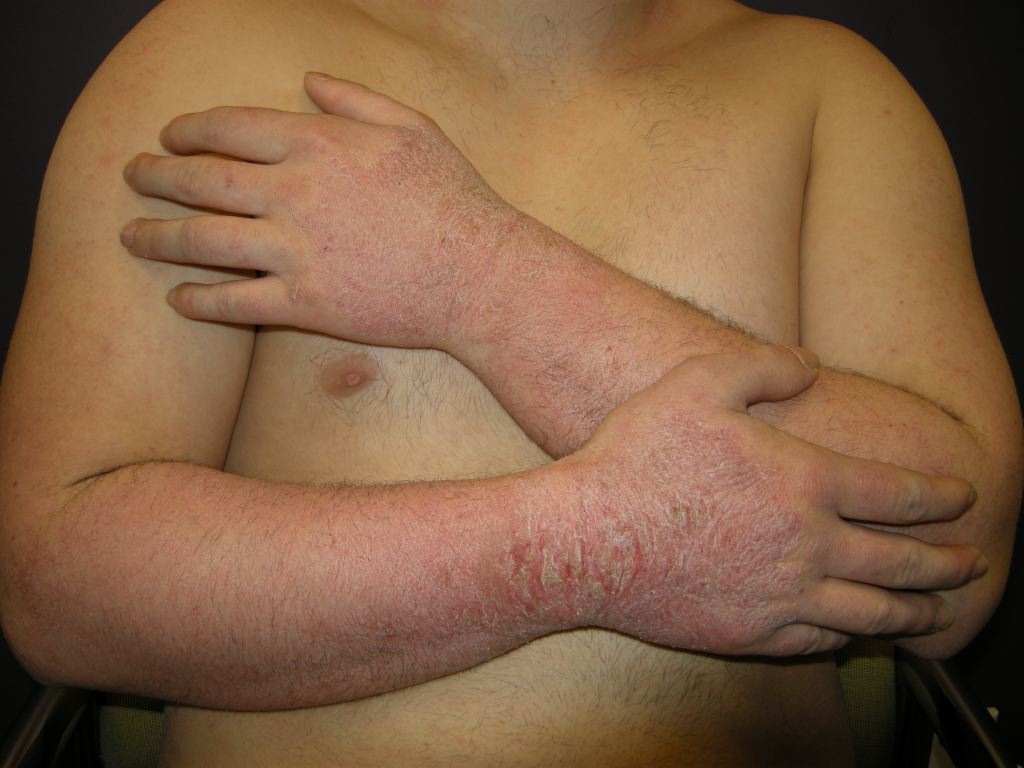
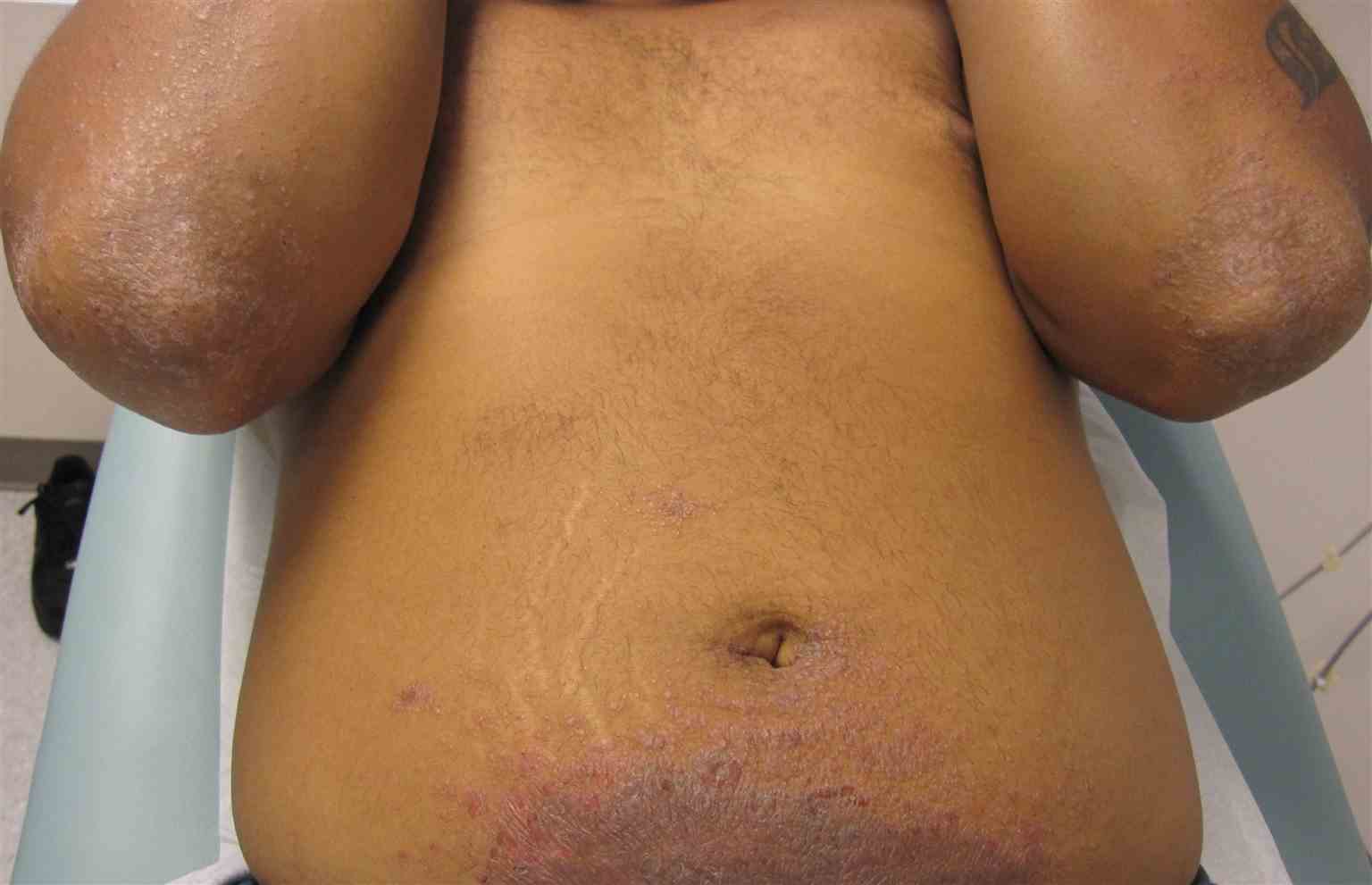
Allergic contact dermatitis can present on physical exam as acute or chronic. Acute ACD characteristically presents as an erythematous, eczematous, or vesicular dermatitis. Although ACD may present with a localized, well-demarcated skin eruption most commonly on the hands or face, it can also be more widespread. For example, rinse-off products such as shampoo or body wash may come into contact with many parts of the body, leading to a more diffuse presentation.[9] Additionally, in cases where the patient systemically consumes an allergen, a more diffuse cutaneous reaction may occur. Chronic ACD more commonly presents with lichenification, fissuring, and scale.[10]
Evaluation
A good clinical evaluation of allergic contact dermatitis involves a detailed history and physical. The morphology and location of the dermatitis is often the best indicator of the offending agent. Patch testing is the gold standard to confirm the diagnosis and should be performed when ACD is suspected in patients with persistent symptoms. Patch testing can help determine the allergen to avoid future exposure. While patch testing is easy to perform, the test may be over-utilized, leading to higher costs for the patient. If the diagnosis is still not certain, a skin biopsy usually demonstrates spongiosis.[11]
One should always rule out tinea as a cause of dermatitis.
Treatment / Management
The only definitive treatment of ACD is the identification and removal of the offending agent, and all patients with suspected or confirmed ACD should be advised of this. First-line medical therapy includes topical steroids when ACD is confined to less than 20% of the body, and oral corticosteroids when greater than 20% of the body is involved. If ACD involves a delicate area such as skin folds or eyelids, topical calcineurin inhibitors or PDE4 inhibitors may also be effective. Upon identification of the allergen, strict avoidance is necessary to prevent a recurrence.[12] Symptomatic management includes oral antihistamines, topical hydrocortisone, and cool water soaks. Vesicles should not be ruptured as there is a risk of infection. The use of moisturizers is a recommended adjunct.
For severe cases, topical immunomodulators like tacrolimus may be beneficial. Some patients may benefit from phototherapy using UV A plus psoralen. Rarely in severe cases, one may require immunosuppressive agents like mycophenolate.
In cases of chronic or recalcitrant ACD, use patch testing to identifying the causative agent.[13] Successful patch testing requires several components: choice of appropriate chemicals for testing, a positive patch test to relevant allergens, and patient counseling of patch test results. Additionally, the American Contact Dermatitis Society’s Contact Allergen Management Program (CAMP) can be utilized to generate a “safe list” of products that do not contain the patient’s allergens. In the case where allergens are unavoidable, systemic therapy may be necessary.[14]
Differential Diagnosis
Morphologically the clinical presentation of allergic contact dermatitis is very similar to irritant contact dermatitis and atopic dermatitis.[15] Other skin conditions that should be ruled out include drug eruptions, scabies, urticarial bullous pemphigoid, urticaria, psoriasis, seborrheic dermatitis, periorificial dermatitis, and rosacea.
Treatment Planning
The goal of the treatment of allergic contact dermatitis is to decrease the inflammatory response that is triggered by the type 4 hypersensitivity reaction. Reactions caused by strong sensitizers may require quicker and more aggressive treatment as the intensity of dermatitis will increase. Identifying and removing the allergen is the most effective definitive treatment. Ointment-based moisturizers and steroids are preferred vehicles of treatment as creams contain a variety of chemicals and preservatives.[16]
Toxicity and Adverse Effect Management
The most important step in the management of allergic contact dermatitis is the removal of the offending agent. Toxicities and adverse effects to monitor are related to the treatment options. It is crucial to control the strength of the topical steroids to appropriate dosages as the most common adverse effect of these medications is thinning of the skin.[16]
Prognosis
This disease stays with the affected populations throughout their lives. Strict avoidance of the allergen needs to be the implemented strategy. Management of the inflammatory response is the essential goal in treatment.[12]
The longer a person has ACD, the more time it will take to resolve.
Complications
Complications associated with allergic contact dermatitis (ACD) involve the inflammatory response.[4] The inflammation subsides with the removal of the allergen. If the allergen is consumed systemically, diffuse dermatitis might occur, but this condition is not considered a dermatologic emergency.
Consultations
Unknown causes of allergic contact dermatitis (ACD) may require patch testing, which is best performed by a dermatologist, immunologist, allergist, or physician with clinical experience in analyzing and testing allergic contact dermatitis.
Deterrence and Patient Education
Educating patients on allergic contact dermatitis (ACD) involves assisting the patient in identifying their allergic triggers. Patients must then be provided with practical behavioral modifications to help decrease the inflammatory response of this disease. For instance, in professions that require regular use of rubber gloves, it is essential that patients can identify the natural rubber allergy and choose a glove type that uses a rubber accelerator (i.e., thiurams, carbamates, mercapto compounds) towards which they do not form a reaction.[4]
A diet low in nickel and other minerals has been said to improve symptoms in some patients.
Pearls and Other Issues
Cross-sensitization may occur in the population affected by allergic contact dermatitis (ACD). This process occurs when an antigen that is chemically similar to an antigen that had previously been sensitized by the host triggers a contact dermatitis. Additionally, systemically-induced allergic dermatitis may take place when an individual who already has undergone sensitization to a contact allergen consumes the allergen by another route (inhalation, ingestion, injection).[17]
Enhancing Healthcare Team Outcomes
The pharmacist is in the prime position to educate the patient on prevention. Patients should be told to avoid wearing nickel-containing jewelry, use latex-free gloves, avoid hair dyes and fragrances which trigger dermatitis. Patients should receive education about reading labels on products to ensure that they do not contain the trigger chemicals. Nurses are also in a strong position to provide counsel on these avoidance strategies.
For those who have ACD of the hands, the use of latex-free gloves may help. Also, patients should use mild cleansing agents on the skin and use protective agents like emollients to help minimize symptoms.
Enhancing patient outcomes is the interprofessional healthcare team's number one priority. Physicians will prescribe treatment when necessary and would do well to verify agent selection and strength with the pharmacist. Nurses should monitor for compliance and also spot adverse events from treatments like topical steroids. Patients with allergic contact dermatitis must have strict return precautions and information on the natural progression of the disease. Patients should not simply receive treatment and sent out the door with a prescription. It is crucial to tailor the treatment to the patient, and the body part affected. Patients also need to have a follow-up with a specialist and continued education. It is vital to utilize nurses and ancillary staff to help communicate in a way that the patient understands. Patients should also have continuous monitoring and follow up with their primary care physician who can help coordinate care. In this collaborative environment, the entire interprofessional healthcare team can direct therapy to its optimal result. [Level V]