Continuing Education Activity
Acute ankle sprains are commonly seen in both primary care practices and emergency departments and can result in significant short-term morbidity, recurrent injuries, and functional instability. Appropriate initial evaluation and treatment can decrease the likelihood of these complications. This activity reviews the evaluation and treatment of ankle sprains and highlights the role of the interprofessional team in improving patient outcomes.
Objectives:
- Identify the most commonly injured ankle ligament and the associated mechanism of injury.
- Describe the evaluation of a patient presenting with an ankle injury.
- Explain how to use the Ottawa ankle rules to evaluate and manage a patient with an ankle injury.
- Explain the value of a well-integrated, team approach to provide optimal care for patients with ankle sprains.
Introduction
Acute ankle sprains are commonly seen in both primary care and sports medicine practices as well as emergency departments and can result in significant short-term morbidity, recurrent injuries, and functional instability. Although nonoperative treatment is often successful in achieving satisfactory outcomes, correct diagnosis and treatment is important at the time of initial evaluation to mitigate the risks of recurrent instability. Appropriate treatment can limit the impact of long-term detrimental effect such as chronic recurrent ankle instability, arthritic progression, and long-term disability.[1][2][3]
Etiology
Ankle sprains most commonly involve injury to the anterior talofibular ligament (ATFL) and/or the calcaneofibular ligament (CFL). Ankle sprains vary depending on the mechanism of injury (high- versus low-energy injuries), position of the foot, and rotational force on the joint and stabilizing ligamentous structures. Low grade injuries (grade I and II) result in stretching or microscopic tears of the stabilizing ligaments, while a high grade (grade III) ankle sprain compromises the syndesmotic structures[4]. The mechanism may also lead to complete tendon disruptions and fractures of the ankle and foot in the highest energy scenarios.
Epidemiology
Over two million ankle sprains are treated in the emergency departments alone in the United States and United Kingdom [5][6]. Ankle sprains are the most frequent injury sustained in sports [7]. Depending on the specific sport participation in consideration, there is a variable distribution when comparing the incidence rate of ankle sprains in male and female athletes. Many studies comparing sex-comparable sports note a similar incidence rate for ankle sprains when comparing male and female athletes. For example, a 2017 epidemiology study of high ankle sprain injury rates noted that male athletes had a higher overall injury rate compared to female athletes in sex-comparable sports [8]. Another 2017 study reporting the incidence rate of ankle sprains in male and female elite soccer players noted comparable incidence rates. Furthermore, multiple studies report the high rate of recurrent injuries and recurrent instability in patients sustaining a single primary ankle sprain[9], and up to 40% of patients sustaining a lateral ankle sprain note persistent symptoms, recurrent sprains, and chronic lateral ankle instability [7].
Pathophysiology
The ankle joint is composed of the articulation of the tibia, fibula, and talus [4][10]. The joint is stabilized by three ligamentous systems: the lateral ligament complex, the medial deltoid ligament, and the syndesmotic ligaments. The most common ankle injury occurs with inversion of the ankle which stresses the lateral ligament complex. The three ligaments that compose the lateral complex are the anterior talofibular (ATFL), the calcaneofibular (CFL), and posterior talofibular (PTFL) and they tend to be injured in this order with the anterior talofibular ligament being injured most commonly. The ATFL is the weakest ligament of the lateral ligament complex, and approximately 70% of lateral ankle sprains involve only this ligament and a mechanicsm of plantar flexion and inversion. The CFL is injuries more commonly in dorsiflexion and inversion mechanisms. The posterior talofibular ligament is the least commonly injured of the lateral ligament complex.
The medial deltoid ligament is the strongest of the ankle ligaments and tends to be injured with eversion injuries. Isolated deltoid ligament injuries are extremely rare. The superficial deltoid complex limits talar abduction moments, while the deep deltoid complex limits external rotation of the talus on the distal tibia.
The distal tibiofibular syndesmotic ligaments stabilize the distal tibia and fibula together in a physiologic manner. Syndesmotic injuries are often referred to as “high ankle sprains” and are much less common than low grade ankle sprains. Given the amount of force required to injure this ligamentous complex, these injuries are distinctly uncommon in the general population and tend to occur primarily in competitive athletes. The most common mechanism of high ankle injuries is external rotation and/or ankle dorsiflexion [4].
History and Physical
In the evaluation of an ankle injury, a practitioner should elicit a history of the mechanism of injury. The practitioner should also investigate whether the injury involved inversion, eversion, rotational stressing, or direct contact, and take into account a history of previous ankle injuries and the patient's ability to bear weight after the injury.
Physical examination should include inspection, palpation, and functional testing. Each of the three lateral ligaments should be palpated at the anterior (ATFL), inferior (CFL), and posterior (PTFL) aspects of the lateral malleoli. The medial ankle should also be palpated along with the entire fibula. Palpation of the proximal fibula is critical to elicit for pain and/or crepitus, which may suggest a maisonneuve fracture pattern. The latter consists of a high grade ankle injury, typically involving an exerternal rotational force with associated fibular fracture component depending on inversion or eversion position of the hindfoot. The maisonneuve fracture pattern disrupts the deltoid ligament, the syndesmotic ligaments, and the fracture force propagating proximally and exiting as a fracture of the proximal fibula.
The foot should also be palpated for associated injuries, particularly over the base of the fifth metatarsal, the navicular, and the midfoot to rule out a potential lisfranc injury. In the latter, plantar-based ecchymosis is often observed on the inspection part of the physical examination.
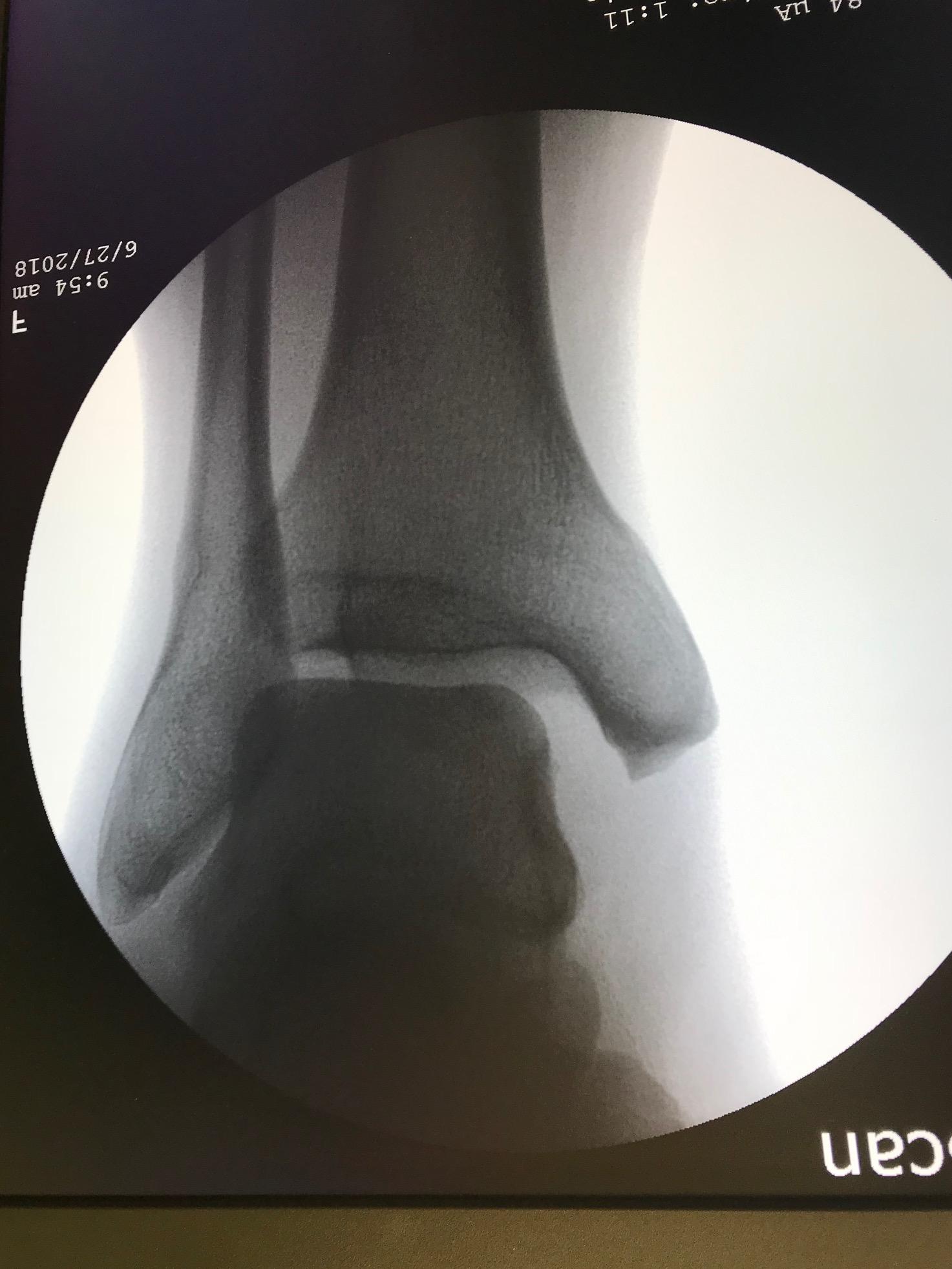
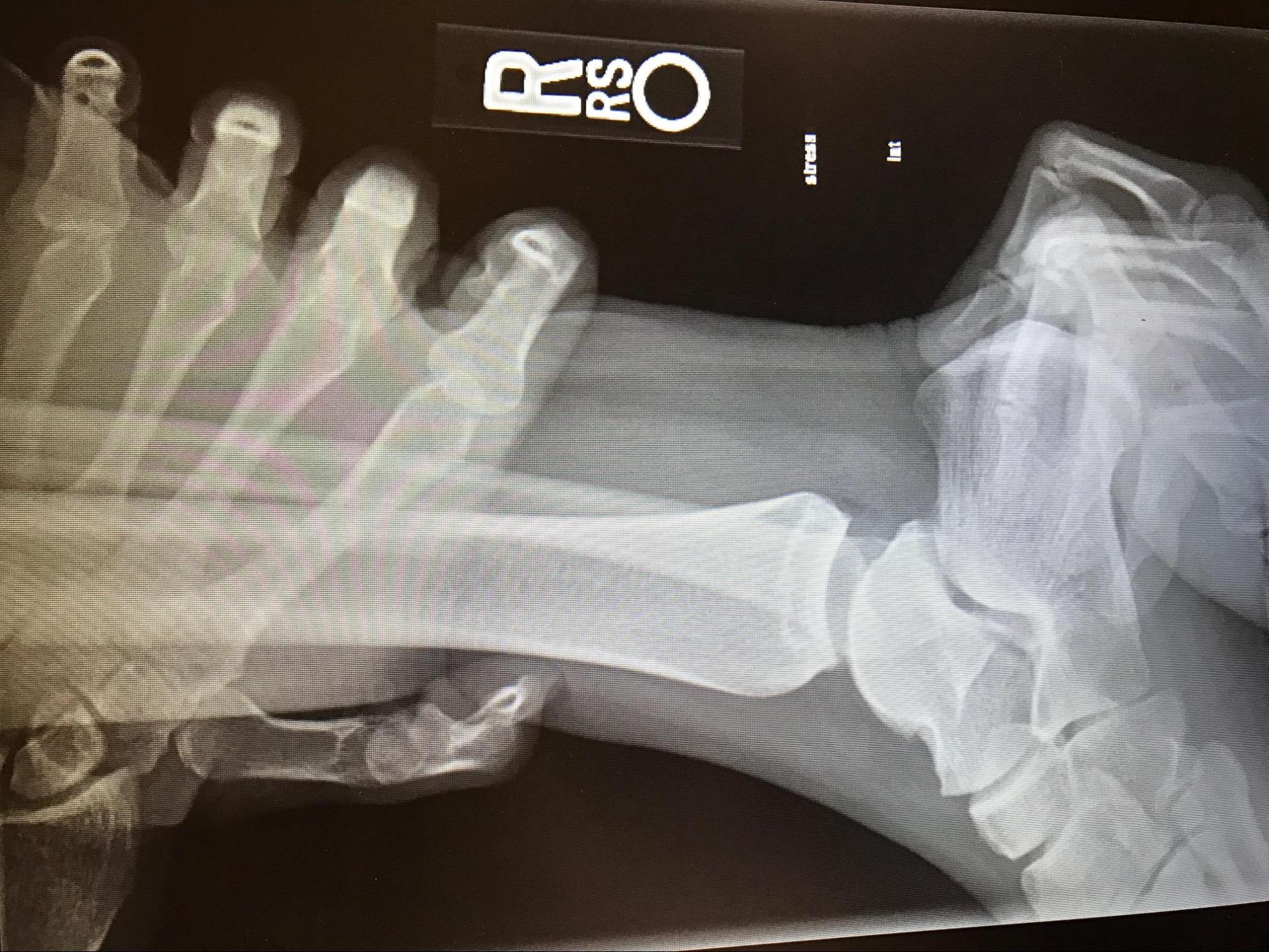
Evidence of a syndesmotic sprain can be elicited with the squeeze test and the external rotation stress test. A positive squeeze test results in pain in the area of the tibiofibular syndesmosis when the mid-calf is compressed and released. To perform the external rotation stress test, externally rotate the slightly dorsiflexed foot. Pain with this maneuver is a positive result and suggests a syndesmotic sprain. This examination can be done under live fluoroscopy in the operating room or in a static radiograph with the foot/ankle positioned in the same position as obtaining a mortise ankle radiographic film. The other stress examination is the gravity stress view. To obtain a gravity stress view, the patient is positioned in the contralateral lateral decubitus position with the injuried extremity/fibula pointed upward and the leg elevated with a leg holder. The cassette is positioned posterior to the heel of the affected ankle, and the beam again directed at an angle of 15-20 degrees of internal rotation to view the ankle in the "mortise trajectory"[11].
Stability of the ATFL can be assessed with the anterior drawer test. This is performed by stabilizing the distal leg with one hand while the other hands grasp the calcaneus. With the foot in 20 degrees of plantar flexion, the examiner pulls forward on the calcaneus. Greater than 1 cm of translation of the foot compared with the uninjured leg suggests ligamentous laxity.
The talar tilt test also assesses the lateral ankle ligaments for laxity, specifically calcaneofibular ligamentous laxity. The test is performed by stabilizing the distal leg in a neutral position while the examiner inverts the ankle. The degree of inversion is compared with the uninjured ankle. Both the talar tilt test and anterior drawer test can be falsely negative soon after the injury due to pain and muscle spasm.
Evaluation
The Ottawa ankle rules have been demonstrated to be accurate in predicting which patients with ankle injuries require x-rays to exclude fractures in both adult and children older than five years.[12]
The Ottawa ankle rules suggest ankle radiographs should be obtained in the setting of pain in the malleolar region and any of the following:
- Tenderness over the posterior edge of the distal 6 cm or tip of the lateral malleolus
- Tenderness over the posterior edge of the distal 6 cm or tip of the medial malleolus
- Inability to bear weight immediately after the injury and for four steps at the time of evaluation.
A foot series is indicated in patients with midfoot pain and any of the following:
- Tenderness of the base of the fifth metatarsal
- Tenderness over the navicular bone
- Inability to bear weight immediately after the injury and for four steps at the time of evaluation
These rules should not be used in the presence of a distracting injury, intoxication, conditions causing diminished lower extremity sensation, and those with head injury or other conditions that would make cooperation difficult. The Ottawa ankle rules have been found to have only moderate specificity but a high sensitivity for ankle fractures. Less than 2% of those in whom no imaging was recommended by these rules have been found to have a fracture.
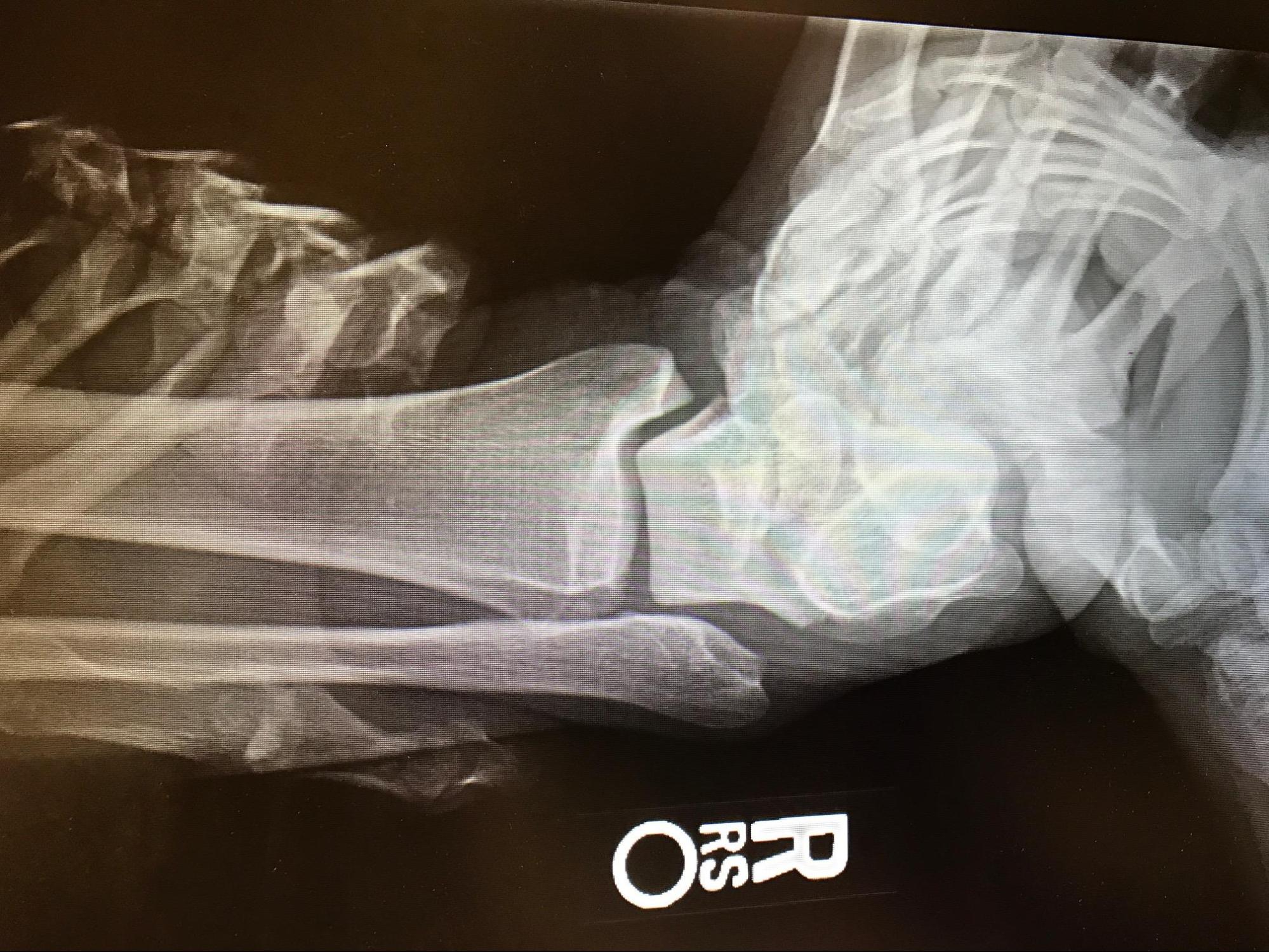
A typical ankle x-ray series would include anteroposterior, lateral, and mortise views. Standard views with a foot series include anteroposterior, lateral, and oblique views.
Treatment / Management
Initial management of ankle sprains includes the PRICE protocol (protection, rest, ice, compression, and elevation). Resting the injured ankle for the first 72 hours followed by gradual resumption of activity as tolerated is a reasonable approach. Initially, crutches can be used, if needed for comfort. When compared with immobilization, early weight-bearing with support (elastic compression wrap or a walking boot, aircast, or walking cast) has been found to improve return to sports, return to work, persistent swelling, the range of motion, and patient satisfaction.[13][14][15][3]
Compression can be achieved with an elastic bandage, any lace-up ankle support, or a semi-rigid or inflatable brace. Elevation of the injured ankle above the level of the heart as frequently as possible for the first 24 to 48 hours may lessen the swelling associated with the injury. The range of motion exercises can be initiated when pain and edema resolve. Nonsteroidal anti-inflammatory drugs or acetaminophen can be used for analgesia.
Early functional rehabiilitation programs should begin with a focus on restoring range of motion, following by proprioception and neuromuscular training, and strength training (especially the peroneal muscles) to help combat recurrent injuries. The strengthening phase should begin once swelling and pain has decreased and the patient demonstrates full range of motion (active and passive). The functional braces should be utilized early on in the strengthening phases and when the patient initially returns to activity.
Mild to moderate ankle sprains typically have a full recovery in 7 to 15 days. Symptoms persisting beyond this period should prompt reevaluation. All symptoms should be resolved before return to sports. For highly competitive athletes, reevaluation by a sports medicine physician for all but mild sprains is reasonable before returning to play to ensure full recovery to avoid recurrent injury and ankle instability.
Recurrent Instability Patients
Patients with evidence of ligamentous laxity should be immobilized, given crutches to allow ambulation without weight-bearing of the injured ankle, and referred to a sports medicine specialist or orthopedic surgeon. The referral is critical given that higher energy injuries are often associated with osteochondral defects of the talus, peroneal tendon injuries, intra-articular loose bodies, and fractures.
Patients suspected of having syndesmotic complex injuries should also be referred given that these injuries are often associated with a prolonged recovery and may require surgical intervention. Acute syndesmotic injuries demonstrating diastasis and ankle instability on exam and stress radiographs will require screw versus tightrope fixation methods [4]. Chronic, recurrent ankle instability should also be referred for ligamentous reconstruction by a variety of accepted surgical techniques.
Differential Diagnosis
- Ankle sprain
- High ankle sprain and syndemotic injury
- Ankle fractures
- Subtalar dislocation
- Lisfranc injuries
Prognosis
While most ankle sprains are successfully managed with nonoperative modalities, recurrent instability and associated defects can be seen in up to 25-40% of patients. Recognition of these possible concomitant injuries and the appropriate referral to an orthopedic/sports medicine specialist is mandatory to mitigate the risks of long-term detrimental outcomes
Complications
- Chronic pain/disability
- Recurrent Ankle instability
- Osteochondral defects of the talus
- Peroneal tendon injuries
- Neurovascular injury
- Tibiotalar arthritis
- Pantalar arthritis
Pearls and Other Issues
An important injury that can be mistaken for an ankle sprain is the Maisonneuve fracture. This injury typically occurs with an eversion injury that results in a tear of the deltoid ligament or medial malleolar fracture. The forced eversion causes a complete disruption of the tibiofibular syndesmosis and fracture of the proximal fibula. This injury, therefore, involves the complete disruption of the ligamentous stability of the ankle thus necessitating surgical fixation. In the absence of a medial malleolar fracture, the associated disruption of the ankle mortise may not be evident on the x-ray and ankle films may be completely normal. Weight-bearing views of the injured foot should demonstrate a widened ankle mortise but often are not obtained unless a high index of suspicion is maintained. Tenderness of the proximal calf should also raise suspicion of this injury. When suspected, x-rays of the tibia and fibula should be obtained.
Enhancing Healthcare Team Outcomes
Ankle sprains remain one of the most common musculoskeletal injuries that present to the emergency department. Ankle sprain is frequently seen in certain sports and is best managed by an interprofessional team approach. The key to ankle sprain is to prevent them in the first place and this requires patient education. Healthcare workers including nurses should emphasize the importance of stretching and conditioning to minimize the severity of ankle sprain. A brief period of warm is essential. In addition, the athlete should be encouraged to wear proper shoes and use braces or even taps to further protect the ankle. Finally, patients with ankle sprain should enter physical therapy before returning to their sporting activity.[16][17]