Continuing Education Activity
Placenta previa is the complete or partial covering of the internal os of the cervix with the placenta. It is a major risk factor for postpartum hemorrhage and can lead to morbidity and mortality of the mother and neonate. This situation prevents a safe vaginal delivery and requires the delivery of the neonate to be via cesarean delivery. Most cases are diagnosed early on in pregnancy via sonography and others may present to the emergency room with painless vaginal bleeding in the second or third trimester of pregnancy. The presence of placenta previa can also increase a woman's risk for placenta accreta spectrum (PAS). This spectrum of conditions includes placenta accreta, increta, and percreta. This activity reviews the evaluation and management of patients with placenta previa. It also highlights the role of an interprofessional team in managing patients with this condition in order to improve outcomes for mother and fetus.
Objectives:
- Describe the risk factors for placenta previa.
- Describe the pathophysiology of placenta previa.
- Describe the management of patients with placenta previa and how this varies with gestational age, presentation, and stability of the patient.
- Explain the importance of improving care coordination, collaboration, and communication amongst an interprofessional team to enhance the delivery of care and improve outcomes for patients with placenta previa.
Introduction
Placenta previa is the complete or partial covering of the internal os of the cervix with the placenta.[1][2][3] It is a major risk factor for postpartum hemorrhage and can lead to morbidity and mortality of the mother and neonate.[4] This situation prevents a safe vaginal delivery and requires the delivery of the neonate to be via cesarean delivery. Most cases are diagnosed early on in pregnancy via sonography and others may present to the emergency room with painless vaginal bleeding in the second or third trimester of pregnancy. The presence of placenta previa can also increase a woman's risk for placenta accreta spectrum (PAS).[5] This spectrum of conditions includes placenta accreta, increta, and percreta. Uncontrolled postpartum hemorrhage from placenta previa or PAS may necessitate a blood transfusion, hysterectomy thus leaving the patient infertile, admission to the ICU, or even death.
Etiology
The underlying cause of placenta previa is unknown. There is, however, an association between endometrial damage and uterine scarring.[6] The risk factors that correlate with placenta previa are advanced maternal age, multiparity, smoking, cocaine use, prior suction, and curettage, assisted reproductive technology, history of cesarean section(s), and prior placenta previa.[3][6][7] The implantation of a zygote (fertilized egg) requires an environment rich in oxygen and collagen. The outer layer of the dividing zygote, blastocyst, is made up of trophoblast cells which develops into the placenta and fetal membranes. The trophoblast adheres to the decidua basalis of the endometrium, forming a normal pregnancy. Prior uterine scars provide an environment that is rich in oxygen and collagen. The trophoblast can adhere to the uterine scar leading to the placenta covering the cervical os or the placenta invading the walls of the myometrium.[7][8]
Epidemiology
Placenta previa affects 0.3% to 2% of pregnancies in the third trimester and has become more evident secondary to the increasing rates of cesarean sections.[3][4][6]
Pathophysiology
Placenta previa is the complete or partial covering of the cervix. A low-lying placenta is where the edge is within 2 to 3.5 cm from the internal os.[8] Marginal placenta previa is where the placental edge is within 2cm of the internal os.[8] Nearly 90% of placentas identified as "low lying" will ultimately resolve by the third trimester due to placental migration.[1][9][10] The placenta itself does not move but grows toward the increased blood supply at the fundus, leaving the distal portion of the placenta at the lower uterine segment with relatively poor blood supply to regress and atrophy.[9][10] Migration can also take place by the growing lower uterine segment thus increasing the distance from the lower margin of the placenta to the cervix.[9][10]
History and Physical
The risks factors for placenta previa include a history of advanced maternal age (age greater than 35 years old), multiparity, smoking, history of curettage, use of cocaine, and history of cesarean section(s).[7] The relationship between advanced maternal age and placenta previa may be confounded by higher parity and a higher probability of previous uterine procedures or fertility treatment. However, it may also represent an altered hormonal or implantation environment.[11] The nicotine and carbon monoxide, found in cigarettes, act as potent vasoconstrictors of placental vessels; this compromises the placental blood flow thus leading to abnormal placentation.[12]
Painless vaginal bleeding during the second or third trimester of pregnancy is the usual presentation. The bleeding may be provoked from intercourse, vaginal examinations, labor, and at times there may be no identifiable cause.[13] On speculum examination, there may be minimal bleeding to active bleeding. Sometimes the placenta can be visualized on speculum examination if the cervix is dilated. A digital examination should be avoided to prevent massive hemorrhage.
Evaluation
Routine sonography in the first and second trimester of pregnancy provides early identification of placenta previa. It is important to realize that the earlier the diagnosis of placenta previa is, the more likely it is to resolve at delivery secondary to placental migration. Nearly 90% of placentas identified as "low lying" will ultimately resolve by the third trimester.[1][9] Follow up sonogram is recommended at 28 to 32 weeks of gestation to look for persistent placenta previa.[6]
A patient presenting with vaginal bleeding in the second or third trimester should receive a transabdominal sonogram before a digital examination. If there is a concern for placenta previa, then a transvaginal sonogram should be performed to confirm the location of the placenta. Transvaginal sonogram has been shown to be superior to a transabdominal sonogram and is safe.[6][10][9] Low lying and marginal placentas are identified with sonography and are determined by measuring the distance of the edge of the placenta to the internal os.
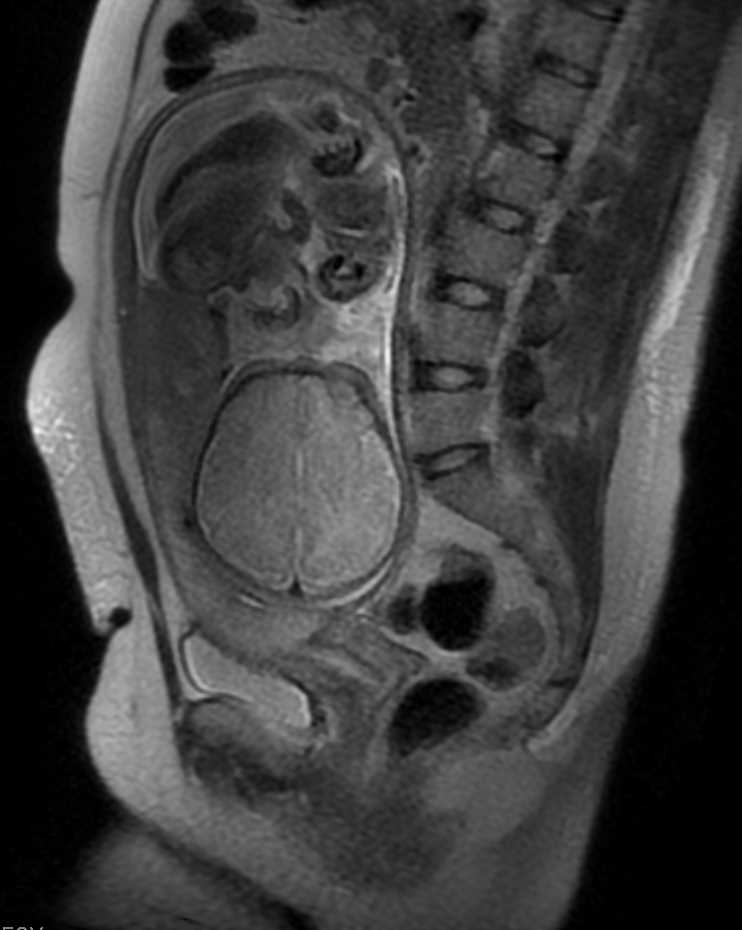
At the time of sonography, evaluation for PAS is also necessary. High suspicion for placenta accreta should be a consideration early on in diagnosis. Placenta accreta is the attachment of the placenta beyond the normal boundary of the myometrium that is established by the Nitabuch fibrinoid layer.[14] Placenta increta is the invasion of the placenta into the myometrium, and placenta percreta is the invasion into the uterine serosa and or surrounding organs.[14] Placenta accreta spectrum can lead to massive hemorrhage, and an integrated team approach is necessary before delivery. Placenta accreta spectrum diagnosis is via ultrasonography with very high sensitivities and specificities.[5] MRI is useful for cases of posterior placenta previa or to assess potential invasion to the bladder. However, they are costly and have not been shown to improve diagnosis or outcomes compared to ultrasonography alone.[5] If there is a high suspicion for a PAS, then a plan for cesarean hysterectomy should be discussed with the patient. The plan should be to leave the placenta in situ to avoid massive hemorrhage.
Treatment / Management
With the diagnosis of placenta previa, the patient is scheduled for elective delivery at 36 to 37 weeks via cesarean section.[15] However, some patients with placenta previa present with complications and require urgent cesarean sections at an earlier gestational age.
Patients who present with a known history of placenta previa and vaginal bleeding should have vitals performed, and should have electronic fetal monitoring initiated. The patient should receive two large-bore intravenous lines with a complete blood count, type and screen, and have coags drawn. If she presents with substantial bleeding, then 2-4 units of blood should be crossed and matched.
Patients with excessive or continuous vaginal bleeding should be delivered via cesarean section regardless of gestational age. If bleeding subsides then expectant management is permissible if the gestational age is less than 36 weeks. If at or greater than 36 weeks of gestation then cesarean delivery is recommended.[15] The patient should be admitted and, if qualified, receive magnesium sulfate for fetal neuroprotection and steroids for fetal lung maturity. Bedrest, reduced activity, and avoidance of intercourse are commonly mandated, though there is no clear benefit.[6][16] If the vaginal bleeding subsides for more than 48 hours and the fetus is judged to be healthy, then inpatient monitoring is continued, or the patient may be discharged for outpatient management. Inpatient vs. outpatient management depends on the stability of the patient, the number of episodes of bleeding, proximity to the hospital, as well as compliance.
Delivery
A cesarean section should optimally occur under controlled conditions. A discussion with the patient should take place during prenatal care of the diagnosis, possible complications, and the plan for cesarean section and possible hysterectomy if there is uncontrolled postpartum hemorrhage or PAS. The surgeon, anesthesiologist, nursing staff, pediatricians, and blood bank should receive notification of these patients. If there is a concern for PAS then urology, general surgery, as well as interventional radiology should have involvement as well. Communication should take place among the teams regarding the expected date of surgery, planned procedures such as uterine artery embolization, and updated imaging studies, which allows the various units to be aware of the patient if the patient presents earlier in an emergency setting.
The patient should have two large bore IV lines in place and blood crossed and matched. Uterine artery catheters can be placed before the procedure by interventional radiology for precautions as well. Regional anesthesia, spinal-epidural combination, is recommended at the time of delivery for nonurgent cases.[17] In the event a hysterectomy is necessary, the patient can convert to general anesthesia.[17][18] Regional anesthesia is considered superior to general anesthesia because of the decreased operative blood loss and the need for blood transfusion.[6] Inhaled anesthetics can lead to uterine relaxation worsening postpartum hemorrhage. During the procedure, if there is a postpartum hemorrhage, then the catheters can be inflated to decrease the blood supply to the uterus.
A vertical skin incision is the recommended incision for optimal exposure. A high vertical uterine incision may be required if the placenta is covering the lower uterine segment, or if the lower uterine segment is underdeveloped. After delivery of the fetus, the placenta spontaneously detaches, and the uterine incision can be closed. There may be hemorrhage after detachment of the placenta secondary to the decreased contractability of the lower uterine segment, which can be managed with bimanual uterine massage, uterotonics, intrauterine tamponade using balloon or gauze, B-Lynch sutures, Hackethal suture, Cho sutures, uterine artery or internal iliac artery ligation, and uterine artery or internal iliac artery embolization.[19][4] At times the massive hemorrhage may not be controlled with conservative measures, and a hysterectomy is necessary.[4] If the placenta does not detach or partially detaches then the patient has PAS, and the placenta should remain in situ, the uterine incision closed, and a cesarean hysterectomy should follow. If there is high suspicion for PAS, then a cesarean section should be performed without manipulation of the placenta.
There is an option for conservative management in patients with PAS if the patient desires fertility. The placenta can be left in situ until there is devascularisation of the placental bed so that the remaining placental tissue may either be more safely removed or resorbs itself. Several studies have reported excellent fertility rates following conservative treatment.[20] However, there is a high recurrence rate of placenta accreta, ranging from 17 to 29%.[20] The discussion of an emergent cesarean hysterectomy and a possible second operation for hysterectomy must be discussed with the patient. A third of women that undergo conservative management will experience ongoing vaginal bleeding where they may require a delayed hysterectomy, blood transfusion, or develop an infection.[20] There is no clear evidence of the benefits of using methotrexate because there is limited or absent trophoblastic proliferation at term to take effect.[20]
Patients with a low-lying placenta, placenta lies greater than 2cm from the cervical os, may qualify for a trial of labor but are at an increased risk for postpartum hemorrhage and emergent cesarean section compared to women with normal placentation.[6][21] There is no consensus for the recommended mode of delivery for marginal placenta previa.[6] One study by Jansen et al. showed that if the distance of the edge of the placenta to the internal os is greater than 10mm a trial of labor should be the recommended procedure.[21]
Differential Diagnosis
Vaginal bleeding during pregnancy can be due to numerous factors. Based on the trimester of pregnancy the differential diagnosis can vary greatly. In the first and second trimester, vaginal bleeding can be secondary to subchorionic hematoma, cervicitis, cervical cancer, threatened abortion, ectopic pregnancy, or molar pregnancy. In the third trimester, vaginal bleeding can be due to labor, placental abruption, vasa previa, or placenta previa.
The most life-threatening cause of vaginal bleeding in pregnancy that should be ruled out is placental abruption, which is placental separation before delivery, a complication in about 1% of births.[3] Placental abruption presents with severe abdominal pain, vaginal bleeding, and electronic fetal monitoring may show tachysystole and a nonreassuring fetal heart tracing; this too can lead to high morbidity in mortality to the fetus and mother secondary to hemorrhage.
Vasa previa is the overlying of the internal cervical os with the fetal vessels that run through the membranes.[22] It is uncommon and occurs in 1 in 2500 to 1 to 5000 pregnancies.[6] It can lead to fetal-neonatal hemorrhage and exsanguination if the fetal vessels tear by spontaneous or artificial rupture of membranes.[6][22]
Prognosis
Neonatal Prognosis
There is a threefold to fourfold increased neonatal mortality and morbidity rate with placenta previa primarily from preterm delivery.[6] The neonate is at increased risk of preterm birth, lower birth weight, lower APGAR scores, and increased risk for respiratory distress syndrome.[1][10][23]
Maternal Prognosis
About 90% of placenta previa cases resolve through delivery.[1] Jing et al. found that women with anterior placentas have poorer prognostic factors and are more likely to have massive blood loss and higher hysterectomy rates compared to any other location.[7] This outcome is secondary to the placenta attaching to a prior uterine incision causing PAS and an incision going through the placenta. Patient's with confirmed placenta previa are at risk for blood transfusion, injury to nearby organs, cesarean hysterectomy (0.2%), intensive care admission, and death.[6] There is also an increased risk in subsequent pregnancies.
Complications
Vaginal bleeding secondary to placenta previa can lead to postpartum hemorrhage requiring a blood transfusion, hysterectomy, maternal intensive care admission, septicemia, and maternal death.[6] Postpartum hemorrhage is blood loss greater than or equal to 1000 ml accompanied by signs or symptoms of hypovolemia occurring within 24 hours after delivery, regardless of the route of delivery.[24] This condition may necessitate blood transfusion, uterotonics, uterine artery embolization, iliac artery ligation, balloon tamponade, and hysterectomy. Placenta previa that is not diagnosed early enough or managed improperly can lead to morbidity and mortality for both the mother and fetus. Placenta previa is also associated with preterm birth, low birth weight, lower APGAR scores, longer duration of hospitalization, and higher blood transfusion rates.[1] Women with placenta previa and prior history of cesarean sections are at an increased risk of PAS. Risk of placenta accreta is 3%, 11%, 40%, 61%, and 67%, for the first, second, third, fourth, and fifth or more cesarean, respectively.[25]
Deterrence and Patient Education
- Placenta previa is the covering of the internal cervical os preventing a safe vaginal delivery.
- Delivery should be performed from 36 to 37 full weeks, via cesarean section, in uncomplicated cases.[15]
- Bed rest, avoiding intercourse, and avoiding digital examinations are recommended. Any manipulation of the placenta can lead to hemorrhage.
- Patients with placenta previa should go to the emergency room if they have any episodes of vaginal bleeding.
- Prior history of placenta previa and a history of cesarean sections may increase a patient's risk for placenta accreta.
- If there is a concern for placenta accreta, increta, or percreta, then a cesarean hysterectomy may need to be performed.
Enhancing Healthcare Team Outcomes
Placenta previa can lead to serious consequences and requires immediate attention to the presentation of vaginal bleeding. an interprofessional team approach must be taken to provide the utmost care for the patient. Patients diagnosed with placenta previa prior to vaginal bleeding should have multiple discussions with the OB/GYN regarding management and expectations. Patients should consent for possible blood transfusions, uterine artery embolization, and possible cesarean hysterectomy. Various disciplinaries, participating in an interprofessional team approach should be aware of the patient including, labor and delivery physicians, anesthesiologist, interventional radiologist, vascular surgeon, urology surgeon, and both surgical and neonatal nurses.