Continuing Education Activity
Pilar cysts, also trichilemmal cysts, are common dermal cysts. They occur in less than 10 percent of the population but are the most common type of skin cyst. They mostly affect the skin of the scalp. This activity illustrates the evaluation and treatment of pilar cysts and reviews the role of the interprofessional team in managing those with this condition.
Objectives:
- Describe the pathophysiology of pilar cysts.
- Identify potential complications of pilar cysts.
- Summarize the management of pilar cysts.
- Explain the role of interprofessional team members in optimizing collaboration and communication to ensure patients with pilar cysts receive high-quality care, which will lead to enhanced outcomes.
Introduction
Pilar or Trichilemmal cysts are common dermal cysts. They occur in less than 10% of the population. Of all skin cysts, Pilar cysts are the most common cysts, mostly affect the skin of the scalp. Trichilemmal cysts never give rise to malignant lesions. They are usually sporadic. The cysts contain keratin and are outlined by stratified squamous epithelium similar to what we see in the outer(external) root sheath of the hair follicle. Proliferating trichilemmal cysts are the tumor form of pilar cysts, and it would appear in less than 3% of all cases of pilar cysts, and it might ulcerate and may be locally aggressive.
Etiology
Trichilemmal cysts may be inherited as an autosomal dominant trait. Patients with familial pilar cysts are often younger and often present with multiple lesions at the same time. They arise from the epithelium located between the sebaceous gland and the arrector pili muscle. They are most common on the head especially the scalp. The pilar cyst rate of growth is very slow; it takes several years to grow to a big size.
Epidemiology
Young individuals are more prone to developing trichilemmal cysts. Pilar cysts have no known racial predilection, and they occur more commonly in women than in men. Family history may be present since the disease follows autosomal dominant inheritance in some cases.
Pathophysiology
Pilar cysts are intradermal cysts that arise from the epithelium located between the sebaceous gland and the arrector pili muscle. They are lined by stratified squamous epithelium without a granular cell layer similar to what is seen in the outer root sheath of the hair follicle and filled with keratin and its breakdown products.
Histopathology
Pilar cysts are lined by thick capsules containing small layers of cuboidal, dark-staining basal epithelial cells in a palisade arrangement without an obvious intercellular gap. Those cells coalesce with multiple layers of keratinocytes forming squamous epithelium; these cells showed more maturation with dense eosinophilic-staining keratin in the absence of a granular cell layer. Sometimes we might see some areas of calcifications. Keratin in the pilar cysts stains with antikeratin antibodies similar to that seen in keratin derived from human hair. Trichilemmal cysts might rupture and of their components will leak into the dermis leading to the formation of foreign-body reaction. Rare malignant transformation in the form of increase mitotic figure along with cell atypia and necrosis might be seen in cases of proliferating trichilemmal cysts.
History and Physical
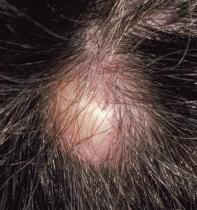
Pilar cysts are primarily diagnosed on clinical presentation. Most commonly, they are multiple lesions, but sometimes, single lesions might be seen. Pilar cysts usually occur in areas with dense hair follicle so that they are most commonly seen on the head especially the scalp, but they can also be found on the face, head, and neck. Trichilemmal cysts are usually asymptomatic unless they calcify or rupture their contents leading to inflammatory process and pain in the affected site. Sometimes, the presence of pilar cyst overpressure or bony prominence might lead to pain. Trichilemmal cysts usually present as flesh-colored, smooth, mobile, firm, and well-circumscribed nodules. Family history is very important since this condition can have an autosomal dominant pattern of inheritance. Usually, they are slow-growing nodules but sometimes they increase in size rapidly and it would indicates infection or malignant transformation. Young females are affected more than males.
Evaluation
Diagnosis of pilar cysts is mainly clinical, based on signs and symptoms and additional investigations rarely need to be done. Radiological studies sometimes are needed to exclude other differentials, especially with midline head and neck lesions and to check for the extent of the lesion and the involvement of the underlying central nervous system (CNS). CT scan is the best way to determine the extent of bone invasion. MRI can be used for more deeper soft tissue involvement and to visualize very tiny invasion.
Treatment / Management
The mainstay of treatment is radical surgical excision of the lesion including the wall of the cysts to avoid the recurrence. Then the content should be sent to the pathology department to confirm the diagnosis. Treatment is complete excision of the cyst. If the cysts return or become inflamed, then it is not recommended to remove surgically, and it is better to wait until the inflammation subsides to proceed to the option of surgical removal. Wound swab and culture sensitivity for the inflamed lesion is mandatory to exclude infection and to guide treatment options. Proliferating trichilemmal cysts might need need multiple surgical removal sessions along with radiation therapy and/ or chemotherapy.
Differential Diagnosis
- Acne keloidalis nuchae
- Cutaneous lipomas
- Dermoid cyst
- Epidermal inclusion cyst
- Favre-Racouchot syndrome (nodular elastosis with cysts and comedones)
- Pilomatrixoma
- Steatocystoma multiplex
Treatment Planning
- Conservative treatment
- Surgical intervention in the form of complete surgical excision of the cyst with its sac to avoid recurrence
- Radiotherapy for select cases with malignant transformation
- Chemotherapy for rare malignant cases[1]
Prognosis
Generally, pilar cysts have good prognosis regardless of the presence of complications. Sequelae of trichilemmal cysts include inflammation, infection and malignant transformation (which is rare). Counseling is needed to assure the patient and his or her family since the disease is transmitted through the autosomal dominant way.[2]
Complications
A pilar cyst might cause pain especially over pressure areas; other complications include inflammation, cosmetic disfigurements, infection, and calcification. A complication from surgical removal may include bleeding, pain, infection, and scarring.[3]
Postoperative and Rehabilitation Care
After surgical removal of Pilar cyst, it is very important to taking care of the surgical site. Daily dressing is advisable along with normal saline and disinfectant solution, covering the sutures with gauze is recommended for the first very days. Typically, sutures should be removed in 7 to 10 days depending on the site of the cyst and status of the wound.[4]
Consultations
Pilar cyst is purely cutaneous condition and does not require consultations to any other specialties unless there is a comorbid disease or any additional complications.[5]
Pearls and Other Issues
Trichilemmal cysts are benign lesions, and they might transform into malignancy on rare occasions. Head and neck are the commonest sites to be affected. Recurrences and metastases have been observed. If the surgeon does not remove the sac completely, then the recurrence rate will be high. Merkel cell carcinoma sometimes might arise from pilar cysts.[6]
Enhancing Healthcare Team Outcomes
Assessment of any patients with Pilar cyst begins with members of an interprofessional team of nurses and physicians taking a thorough history and careful physical examination which is usually enough to reach the diagnosis in most of the cases. Rarely, biopsy of the lesion is needed for the diagnosis. Reassurance of the patient is very important. Patients who are interested in surgical treatment should be aware of the consequences of surgery since scar formation can be more disfiguring to the patient's image rather than the lesion itself.[7]