Continuing Education Activity
Acromioclavicular joint injuries account for more than forty percent of all shoulder injuries. Mild injuries are not associated with any significant morbidity, but severe injuries can lead to significant loss of strength and function of the shoulder. Acromioclavicular injuries may be associated with a fractured clavicle, impingement syndromes, and, more rarely, neurovascular insults. This activity reviews the evaluation and management of this condition and highlights the role of the interprofessional team in caring for patients effected by this acromioclavicular joint injuries.
Objectives:
Identify the most common mechanism of injury associated with acromioclavicular joint injury.
Evaluate a patient with a suspected acromioclavicular injury.
Identify the difference between managing patients with Rockwood Classification type I to II injuries and patients with Rockwood Classification type III to VI.
Strategize with the interprofessional care team to provide optimal management and counseling to improve outcomes for patients with acromioclavicular joint injuries.
Introduction
Injury to the acromioclavicular joint is common among athletes and young individuals. Acromioclavicular joint injuries account for more than 40% of all shoulder injuries. Mild injuries are not associated with any significant morbidity, but severe injuries can lead to significant loss of strength and function of the shoulder. Acromioclavicular injuries may be associated with a fractured clavicle, impingement syndromes, and, more rarely, neurovascular insults.
Etiology
The acromioclavicular joint is a diarthrodial joint defined by the lateral process of the clavicle articulating with the acromion process as it projects anteriorly off the scapula. The joint is primarily stabilized by the acromioclavicular ligament, composed of an anterior, posterior, inferior, and superior component. Of note, the superior portion of the acromioclavicular ligament is the most important component for the stability of the acromioclavicular joint. Supporting structures include two coracoclavicular ligaments (trapezoid and conoid), which provide vertical stability, and the coracoacromial ligament. Mild injuries are not associated with any significant morbidity, but severe injuries can lead to considerable loss of strength and function of the shoulder. Acromioclavicular injuries may be associated with a fractured clavicle, impingement syndromes, and, more rarely, neurovascular insults.[1][2]
Epidemiology
Acromioclavicular injuries are frequently seen after sporting events, car accidents, falls from a bicycle, and other sports-related activities (eg, skiing). Acromioclavicular joint injuries may account for as much as 40% of all shoulder injuries and nearly 10% of all injuries in collision sports such as football, lacrosse, and ice hockey.[3][4]
Pathophysiology
The most common mechanism of injury is direct trauma to the lateral aspect of the shoulder or acromion process with the arm in adduction. Falling on an outstretched hand or elbow may also lead to acromioclavicular joint separation.
History and Physical
Patients with an acromioclavicular joint injury typically present with anterosuperior shoulder pain and will describe a mechanism of injury of blunt trauma to the abducted shoulder or landing on an outstretched arm, suggestive of this type of injury. They may describe pain radiating to the neck or shoulder, often worse with movement or when they try to sleep on the affected shoulder. On examination, the clinician may observe swelling, bruising, or a deformity of the acromioclavicular joint, depending on the injury. The patient will be tender at that location. They may have a restriction in the active and passive range of motion secondary to pain. "Piano key sign" may be seen, with an elevation of the clavicle that rebounds after inferior compression. Finally, It is essential to evaluate the entire clavicle for possible fracture or sternoclavicular injury and perform a full neurovascular exam on the affected extremity.
Evaluation
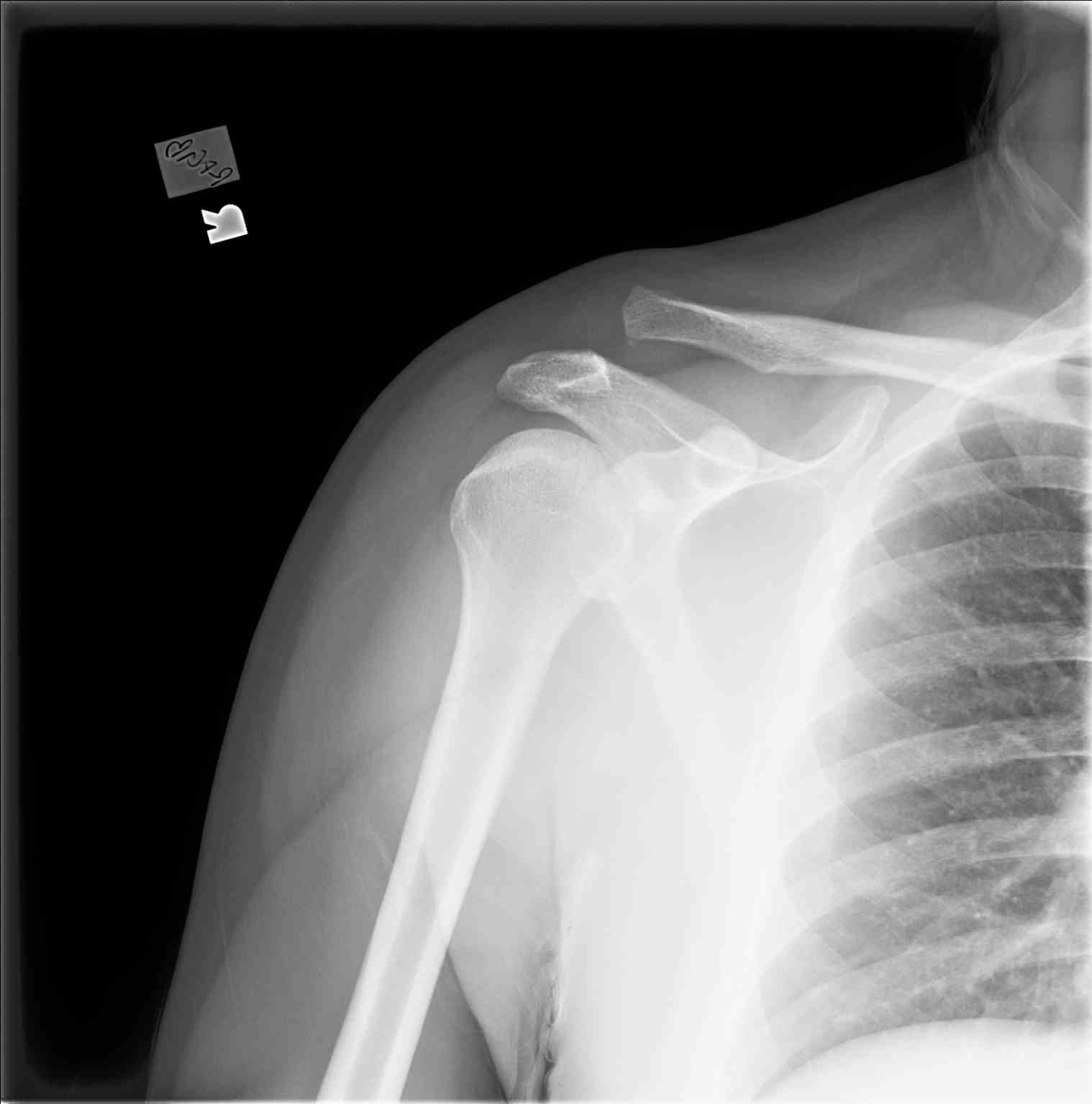
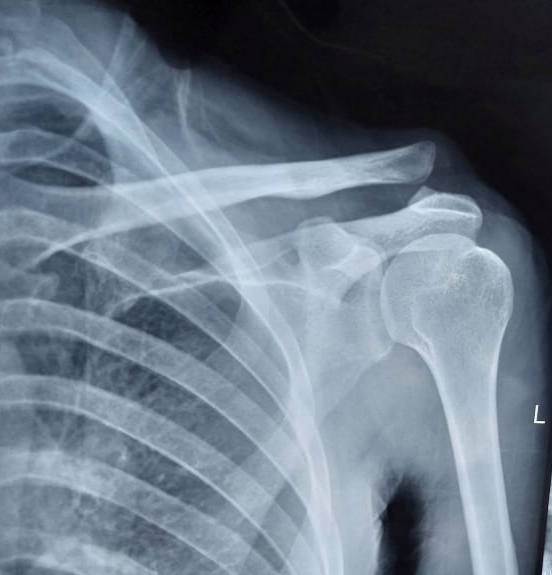
Standard X-rays are adequate to make a diagnosis of acromioclavicular joint injury and should be used to evaluate for other causes of traumatic shoulder pain. Acromioclavicular joint injuries may not always be evident on regular radiographic views (anteroposterior, lateral). Additional views include the Zanca view, an anteroposterior view performed by tilting the beam 10 to 15 degrees cranial, and bilateral anteroposterior views to compare displacement to the contralateral shoulder. Weighted stress views may be useful in evaluating the displacement of the joint when the diagnosis is uncertain based on standard anteroposterior views. If there is continued uncertainty in diagnosis, the provider may also consider ultrasound or MRI for further diagnostic evaluation.[5]
Consider the Rockwood Staging System outlined below when evaluating radiographs, especially when compared to the contralateral shoulder, which will be important for guiding treatment. In most cases, identifying the coracoclavicular interspace distance compared to the contralateral view will help guide treatment options. An example of the appropriate method for measuring coracoclavicular interspace distance appears below.
Treatment / Management
Rockwood classification
Acromioclavicular joint injuries follow the Rockwood classification system of type I to type VI.
Type I
Type I is a sprain of the acromioclavicular ligaments only and demonstrates no radiographic displacement.
Type II
Type II involves tearing of the acromioclavicular ligament and sprain of the coracoclavicular ligament with less than 25% increase in the coracoclavicular interspace or with the clavicle elevated but not superior to the border of the acromion. Type I and II sprains are managed nonoperatively with a sling, analgesia, ice, and physical therapy.
Type III
Type III acromioclavicular joint separation involves tearing of both the acromioclavicular ligament and coracoclavicular ligaments, resulting in clavicle elevation above the border of the acromion with a 25 to 100% increased coracoclavicular distance on X-ray compared to the contralateral side. Type III injuries are frequently managed nonoperatively, similar to type I and II; however, if the displacement is greater than 75%, the patient is a laborer, elite athlete, or concerned about cosmesis, or is not improving with conservative management, then surgical intervention may be considered.
Type IV
Posterior displacement of the distal clavicle into the trapezius defines type IV injuries (see Image. Shoulder Rediograph, Acromioclavicular Joint Separation With Injury Type III/IV).
Type V
Superior displacement of the distal clavicle by more than 100% compared with contralateral defines type V injuries.
Type VI
Type VI is a rare injury, defined as an inferolateral displacement in a subacromial or subcoracoid displacement behind the coracobrachialis or biceps tendon. Type IV through VI injuries are typically managed surgically and warrant referral to an orthopedic surgeon.[1][3][6]
Management of Acute Acromioclavicular Joint Disruption
If the acromioclavicular joint injury presents within 6 weeks, it is considered acute. The main goal of treatment is acromioclavicular joint stabilization. The following techniques are used to stabilize and reduce the acromioclavicular joint (see Image. Acromioclavicular Joint Disruption).[7]
Hook plate
In the setting of Rockwood type Types III and V injuries, a distal clavicle hook plate may be employed to restore the alignment of the acromioclavicular joint. The "hook" portion of the hook plate is placed inferior to the acromion, with superior plating on the clavicle. While this does provide excellent reduction of the joint, the plate must be removed in a subsequent surgery to prevent subacromial irritation, subacromial impingement, acromion osteolysis, and iatrogenic damage to the rotator cuff.[8] Kienast et al reported 84% good and excellent results (Taft score) in type III through V acromioclavicular disruption with a hook plate.[9] A superior approach is used for plate fixation. The hook is placed posteriorly under the acromion, and screws are placed after the reduction of the acromioclavicular joint.[7]
Bosworth screw
All types of acromioclavicular joint injuries can be treated with the Bosworth screw (coracoclavicular screw fixation), which has outstanding results and is very cost-effective. Bosworth screws, along with acromioclavicular and coracoclavicular ligament reconstruction, provide excellent long-term outcomes. A 6.5-mm screw is placed from the clavicle to the coracoid through a mini-open incision or percutaneously. Early screw removal (usually 8 weeks) is necessary to prevent fatigue failure and crew breakage.[10][11]
Tension band wiring
Tucek et al compared tension band wiring versus hook plate in 80 patients with type 5 AC joint disruption. Tension band wiring provides comparable clinico-radiological results; however, hook plate allows an earlier range of motion and has a reduced rate of complications. Tension band wiring should be removed after 8 weeks to prevent wire malposition, migration, and breakage.[12]
Endobutton
A suitable treatment option for acromioclavicular dislocation is coracoclavicular ligament reconstruction utilizing an endobutton, which has the benefits of solid fixation and an early functional range of motion. [13] Double or triple Ethibond no.5 loops are used with titanium endobuttons from clavicle to coracoid. Compared with a single suspension system, continuous and double loops minimize the risk of loop-knot slippage.[14]
Management of chronic acromioclavicular joint disruption
There are 3 main goals of treatment
- Acromioclavicular joint debridement
- Ligament reconstruction (acromioclavicular/coracoclavicular)
- Stable fixation
The following procedures are used for chronic acromioclavicular joint disruptions.
Modified Weaver-Dunn procedure
An incision is made from the acromioclavicular joint, the tip of the coracoid. After raising skin flaps, the acromioclavicular joint is debrided, and a distal 1 cm of the clavicle is excised. The coracoacromial ligament and a small piece of the acromion are transferred to the distal end of the clavicle. The modification in the original procedure is done in the form of added fixation with a screw or plate.[15][16]
Mazzocca technique
The incision extends from the tip of the coracoid to 2 cm posterior to the acromioclavicular joint. The distal 1 cm of the clavicle is excised after acromioclavicular joint debridement. A semitendinosus autograft is prepared and looped around the coracoid. The anatomical reconstruction is done by making bony tunnels in the clavicle shaft at the footprint of the conoid and trapezoid ligament.[17]
Neviaser technique
The coracoacromial ligament and a small bony piece from its attachment site are mobilized from the coracoid. K-wires are used to anchor the ligament to the distal end of the clavicle.[18]
Rockwood procedure
The original procedure includes the transfer of coracoacromial ligament from the acromion to the distal end of the clavicle. The bony tunnels are made through the lateral end of the clavicle to anchor this coracoacromial ligament. A Bosworth screw provides stable reduction to secure this ligament reconstruction.
Docking technique
The coracoacromial ligament is transferred from the acromion into the distal end of the clavicle. The docking procedure involves tensioning the coracoacromial ligament into the distal clavicle's medullary canal using 2 nonabsorbable sutures.[19]
Mumford procedure
This procedure is required for chronic type I and II acromioclavicular joint disruptions with intact ligaments. The distal 2.5 cm of the clavicle is excised to reduce joint pain. The soft tissue and periosteum are pilcated over the lateral end of the clavicle.[20]
Differential Diagnosis
The differential diagnoses for acromioclavicular joint injury include the following:
- Acromioclavicular distal clavicle osteolysis
- Acromioclavicular joint arthritis
- Acromion fracture
- Adhesive capsulitis
- Anterior humerus subluxation
- Complex pain syndrome
- Erb-Duchenne injury
- Glenoid labrum tear
- Os acromiale
- Rotator-cuff injury
- Superior labral tear
- Septic arthritis
- Shoulder dislocation
Staging
Rockwood Classification of acromioclavicular joint injuries coracoclavicular [CC]).
The Rockwood classification of acromioclavicular joint injuries remains the gold standard for driving treatment decisions and is an excellent tool for managing acromioclavicular joint injuries.
- I: Acromioclavicular ligament sprain; coracoclavicular ligament intact; no radiographic abnormalities
- II: Acromioclavicular ligament is torn; coracoclavicular ligament sprain; the clavicle has elevated but is not superior to the border of the acromion, or exhibits a less than 25% increase in the coracoclavicular interspace compared to the contralateral
- III: Acromioclavicular and coracoclavicular ligaments are torn; the clavicle has elevated above the border of the acromion, or there is an increase of 25% to 100% in the coracoclavicular interspace compared to the contralateral
- IV: Acromioclavicular and coracoclavicular ligaments are torn; posterior displacement of the distal clavicle into the trapezius
- V: Acromioclavicular and coracoclavicular ligaments are torn; superior displacement of the distal clavicle by more than 100% in the coracoclavicular interspace compared to the contralateral
- VI: Acromioclavicular and coracoclavicular ligaments are torn; inferolateral displacement in a subacromial or subcoracoid displacement behind the coracobrachialis or biceps tendon [21]
Prognosis
The prognosis for acromioclavicular joint injuries is generally favorable. Most injuries receive nonoperative management, and individuals typically regain functional motion by 6 weeks and return to normal activity by 12 weeks. Surgically managed injuries have a more extended recovery timeframe, including immobilization for 6 weeks and a gradual return to full activity around 6 months.[22][23][24]
Complications
The most frequently encountered complication of acromioclavicular joint separation is residual joint pain, affecting anywhere from 30% to 50% of individuals. Acromioclavicular joint arthritis is also a known complication and is more common with surgical management. Hardware irritation, infection, adhesive capsulitis, coracoid, and clavicular fractures are common complications following fixation. Hook plate leads to acromion irritation, subacromial impingement, and osteolysis.[25]
Postoperative and Rehabilitation Care
Weeks 1 to 6
- An arm sling is applied
- Ice packs are applied to the shoulder
- Elbow and wrist mobilization is started
- Auxiliary hygiene is maintained
- Adequate analgesia is provided [26]
Weeks 6 to 12
- Limit abduction above 90 degrees
- Wean off polysling and start pendulum exercises
- Passive and then active range of motion exercises are started
- Start isometric and then strengthening exercises of the rotator cuff
- Elbow and wrist mobilization is continued
Weeks 12+
- Start full range of motion of the shoulder above 90 degrees
- Proprioceptive and strengthening exercises are allowed
The patient is allowed to return to sports after 6 months.[27]
Consultations
Type I and II AC joint separations do not necessarily require an evaluation by a specialist; however, type III through VI should have an evaluation by an orthopedic surgeon or sports medicine physician.
Deterrence and Patient Education
Injuries of the acromioclavicular joint are common causes of shoulder pain and frequently occur in athletes and the setting of traumatic injuries. Patients should seek an evaluation from a trained orthopedic or sports management physician. Early management with sling immobilization, ice, rest, and antiinflammatory medications is generally an appropriate treatment for these injuries. Patients can generally return to normal activities after they have been evaluated and cleared by their treating physician.
Enhancing Healthcare Team Outcomes
Acromioclavicular joint injuries are commonly present in the emergency department. The mild injuries are usually managed conservatively, but the severe injuries may require surgery; hence, it is crucial to consult an orthopedic surgeon when arriving at the diagnosis to grade the injury. For mild injuries, the nurse practitioner, emergency department physician, and primary caregiver should recommend physical therapy once the acute pain has resolved. Pharmacists and nurses should work with the team to educate the patient and family and assist in pain control. Those wishing to return to sports should first consult with the orthopedic surgeon.[28]