Continuing Education Activity
Bazex syndrome, also known as acrokeratosis paraneoplastica or acrokeratosis neoplastica syndrome is a rare, acral psoriasiform dermatosis associated with malignancies, most frequently squamous cell carcinoma. Typically the carcinoma involves the upper aerodigestive tract, but it is important to know that it can be associated with almost any squamous cell malignancy. It is crucial for providers to be aware of this syndrome so that patients can get a thorough workup to determine the location of the malignancy. This activity reviews the evaluation and management of patients with acrokeratosis paraneoplastica and highlights the important role of the interprofessional team in caring for patients with this condition.
Objectives:
- Describe the history and physical exam findings of acrokeratosis paraneoplastica.
- Outline the evaluation of acrokeratosis paraneoplastica.
- Identify the best treatment strategy for patients with acrokeratosis paraneoplastica.
- Summarize the importance of an interprofessional team approach in evaluating and caring for patients with acrokeratosis paraneoplastica.
Introduction
Bazex syndrome, also known as acrokeratosis paraneoplastica or acrokeratosis neoplastica (AN) syndrome is a rare, acral psoriasiform dermatosis associated with internal malignancies, most frequently squamous cell carcinoma of the upper aerodigestive tract. However, it is important to know that almost any malignancy of squamous cells can be associated with the syndrome. Thus, these patients need an exhaustive workup to determine the location of the malignancy. The skin lesions are usually noticed before the diagnosis of the underlying malignancy and frequently subside spontaneously after complete treatment of the malignancy.[1] If the primary malignancy is not treated, not only is the prognosis poor, but the skin lesions will also fail to respond.[1][2][3]
Etiology
The pathogenesis of Bazex syndrome is unknown. Bolognia reported that in 67% of the cases with Bazex syndrome, the cutaneous lesions predicted the diagnosis of an underlying malignancy, whereas, in 15% of the patients, the skin lesions developed after diagnosis of the neoplasm.[1] Risk factors for Bazex syndrome include tobacco and alcohol use.[4][1]
Epidemiology
The population most often affected is White middle-aged males in their 40s -70s.[4] Females are rarely affected.[5]
Pathophysiology
The pathogenesis of Bazex syndrome is unknown. Some authors have implicated an immunological mechanism based on the findings of immunoglobulins (IgG, IgA, IgM) and complement (C3) along the basal membrane of the involved and healthy skin. An immune reaction to a common antigen (skin and tumor) has been suggested.[5] It has been suggested that the underlying malignancies might be associated with a shift to a Th2 immune pathway which in turn might lead to increase expression of epidermal growth factor receptors in the affected keratinocytes.[6]
Histopathology
Features in the epidermis can include spongiosis, interface change including vacuolar degeneration and dyskeratotic keratinocytes, and in the dermis, a lichenoid infiltrate, melanophages, and papillary dermal fibrosis.
Recent studies indicate that immunohistochemistry of the skin lesions will reveal localized deposits of complement factor 3, immunoglobulins, and fibrin within the basement membrane.
History and Physical
The typical clinical features include tender, largely nonpruritic, and erythematous psoriasiform eruptions that favor acral sites such as the fingers (61%), toes (39%), ears (79%), and nose (63%). Nail involvement is almost always present, is indistinguishable from nail changes associated with psoriasis, and is often the first sign of the condition. Unlike in psoriasis, the helical rim of the ear and nasal tip are affected. Intensive violaceous erythema, erosions, and yellowish crusts may be present. Rarely, bullous lesions may be present as well.[7] If the underlying tumor is not treated, the eruption has been seen to extend proximally. As the tumor progresses, the lesions of AN may spread and may involve the cheeks, elbows, knees, and trunk. The most common localization of malignancies is the neck and head area. Approximately 39% of the underlying malignancies were squamous cell carcinomas of the pharynx, esophagus, and larynx. The other malignancies that are found to be associated are squamous cell carcinoma of the lung (11%), adenocarcinoma of the lung (4%), gastrointestinal adenocarcinoma (8%), genitourinary tumors (5%), and lymphomas.
In 63% of cases, skin lesions precede the diagnosis of the tumor by approximately one year.
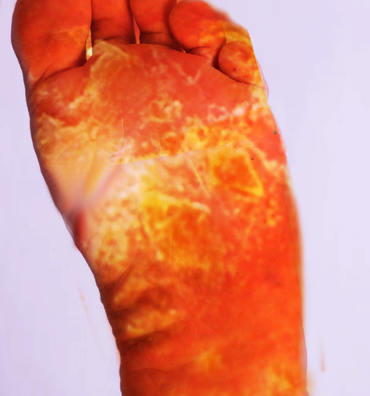
According to Bazex et al., the disease develops in three stages. The first stage is typically asymptomatic and typically affects the earlobes, the ear helix, the tip of the nose, distal fingertips, or nails. Vesicles, subungual hyperkeratosis, or nail dystrophy can be noted. Nail involvement is almost always present, is often the first sign of the condition, and nail changes are indistinguishable from those due to psoriasis. Nail changes can include horizontal and vertical ridging, yellow discoloration, onycholysis, subungual hyperkeratosis, and in more severe cases, nail plate atrophy. Later, in stage two, the palms and soles may become involved. The skin lesions spread to involve the cheeks, forehead, elbows, and knees. In stage three, if the underlying tumor is progressing, erythema can spread to the trunk.
During the physical exam, one must be aware of signs of malignancy and paraneoplastic syndromes. Features that may be indicative of malignancy include the following:
- Pruritus
- Ichthyosis
- Sister Mary Joseph nodule
- Clubbing
- Sign of Leser-Trelat
- Blummer shelf
- Virchow's nodes[1][8]
Evaluation
Upon suspicion of Bazex syndrome, a detailed patient history, and a physical examination are mandatory. A diagnostic workup, including otolaryngologic examination, chest x-ray, a complete blood cell count, serum and urine protein electrophoresis, an erythrocyte sedimentation rate, a biochemistry profile, tumor markers (e.g., prostate-specific antigen, carcinoembryonic antigen), and a test for occult blood in the stool should be performed.
Imaging and Endoscopic Studies
- Gastrointestinal imaging using barium
- Chest x-ray must be done in all patients suspected of having acrokeratosis paraneoplastica
- Ultrasound of the abdomen and pelvis
- Computed tomography (CT) scan of the chest, head/neck, and abdomen
- Magnetic resonance imaging (MRI) of the chest, head/neck, and pelvis
- Mammography
- Positron emission tomography (PET) scan
Other Tests Based on Clinical Presentation
- Upper and lower endoscopy
- Cystoscopy
- Bronchoscopy
- Bone marrow biopsy
- Lymph node biopsy
Treatment / Management
The favored therapy to eliminate the described skin lesions is the effective treatment of the underlying tumor. Paraneoplastic skin lesions as seen in Bazex syndrome do not respond to the classical dermatological therapy of inflammatory skin diseases. Improvement after the treatment with Vitamin D3, salicylic acid, and topic or systemic steroids have been reported. Reported topical treatments include topical corticosteroids, as clobetasol 0.05% or betamethasone 0.01%, salicylic acid 10% in vaseline, itraconazole, isosorbide dinitrate, fluconazole, cephalexin, keratolytic, neomycin, nystatin, zinc ointment, antibiotic, and emollients. Some authors suggest a treatment with oral dexamethasone 10 mg/day leading to a good response of the cutaneous lesions.
In the last decade, anecdotal reports indicate that the use of both systemic and topical retinoids may help ease the skin lesions. Early initiation of acitretin has been reported to be effective in the amelioration of acrokeratosis paraneoplastica in a patient with an incurable primary malignancy.[9] These vitamin A derivatives may be combined with oral corticosteroids. Some reports indicate that the use of psoralen plus ultraviolet light therapy may be helpful in selected patients with localized skin lesions.
There are even reports indicating that supplementation of zinc may help ease the skin lesions.
Differential Diagnosis
The differential diagnosis mainly includes psoriasis and other psoriasiform dermatitis. Pityriasis rubra pilaris, Reiter's syndrome and tinea manuum need to be considered in the differential of the acral lesions.[1] There have been case reports of acrokeratosis paraneoplastica-like findings in patients with systemic lupus erythematosus.[10][1]
Prognosis
The success of the treatment of acrokeratosis paraneoplastica depends on the primary malignancy. if the malignancy fails to respond or is advanced, then the skin lesions typically will not respond.
In any patient with cervical lymph node metastases at the time of diagnosis, the prognosis is poor. In all cases, the morbidity of the disorder is directly related to the underlying primary malignancy and not the skin lesions.
However, overall the response to treatment is extremely variable, unpredictable, and not satisfactory.
Complications
Other than the skin lesions, acrokeratosis paraneoplastica does not lead to any complications by itself.[1]
Deterrence and Patient Education
Patients need to be counseled regarding the paraneoplastic nature of the disease and that usually, the skin lesions subside after complete and effective treatment of the primary malignancy.[1]
Enhancing Healthcare Team Outcomes
In the early stage of the disease, skin lesions often serve as an indicator for a symptomless internal malignancy. Whereas the skin lesions improve significantly after adequate tumor therapy, the nail changes often remain. The original nail growth is often reduced, and a complete remission is absent. If the tumor reoccurs or if there are metastases present, the skin lesions usually worsen again. The management of these patients should involve an interprofessional team of healthcare professionals due to the varied types of cancers that can be involved. Once the diagnosis is made, there should be no delay in ruling out a malignancy. [Level 5]