Continuing Education Activity
Three distinct types of longitudinal melanonychia exist, including 1. lentigo, 2. nail matrix nevus, and 3. subungual melanoma. The first two conditions are benign lesions, while subungual melanoma is malignant. Subungual melanoma is a distinct subtype of cutaneous malignant melanoma arising from structures within the nail apparatus. Unlike cutaneous malignant melanoma, subungual melanoma does not appear to be related to sun exposure. It is ordinarily a variant of acral lentiginous melanoma, a malignant melanoma originating on palms and soles. This activity seeks to provide an up-to-date and accurate review of subungual melanoma and its interprofessional team management.
Objectives:
- Identify the etiology of subungual melanoma.
- Review the presentation of subungual melanoma.
- Outline the management options available for subungual melanoma.
- Summarize the importance of improving care coordination among interprofessional team members to improve outcomes for patients affected by subungual melanoma.
Introduction
Three distinct types of longitudinal melanonychia exist, including 1. lentigo, 2. nail matrix nevus, and 3. subungual melanoma. The first two conditions are benign lesions, while subungual melanoma is malignant.[1] Subungual melanoma is a distinct subtype of cutaneous malignant melanoma arising from structures within the nail apparatus. It is ordinarily a variant of acral lentiginous melanoma, a malignant melanoma originating on palms and soles. Boyer originally recognized it in 1834. Hutchinson described the features in greater detail in 1886, offering a more accurate view of the condition. He described a specific sign strongly associated with subungual melanoma where the pigment extends beyond the nail and into the adjacent skin ("Hutchinson sign"). This article provides an up-to-date and accurate review of subungual melanoma and its management.[2][3][4]
Nail unit melanoma, also called subungual melanoma, accounts for up to 3 percent of all melanomas in populations with lightly pigmented skin. However, it accounts for up to 30 percent of melanomas in populations with darkly pigmented skin.[14] In approximately sixty-five percent of cases, nail melanoma presents as a dark black, vertical band involving a single nail.[15] The band is usually wider than 3 mm, with proximal widening and irregular side borders. Nail plate dystrophy is a common finding.
Etiology
Malignant melanoma of the nail matrix originates from melanocytes, as with cutaneous melanoma. Unlike cutaneous malignant melanoma, subungual melanoma does not appear to be related to sun exposure.[5]
Epidemiology
Subungual melanomas are rare and account for 0.7% to 3.5% of all malignant melanomas worldwide. Melanoma of the nail apparatus occurs equally in all racial groups. However, it is the most common variant of malignant melanoma among African-Americans, Asians, and Hispanics. It accounts for 75% of melanomas in African populations, 25% in Chinese populations, and 10% in Japanese populations. These groups usually have a very low incidence of cutaneous malignant melanoma due to the melanin pigment protecting their skin from ultraviolet (UV) radiation from the sun. It is most common in the seventh decade of life for men and the sixth for women. The great toe and thumb are the most common digits affected. These digits account for 75% to 90% of cases.[6][7]
Pathophysiology
Subungual melanoma occurs because there is increased melanin production by the melanocytes. When activated, the melanocytes differentiate into matrix cells and migrate distally.
Melanocytes in the nail unit are lower than in normal skin. Moreover, melanonychia usually involves the distal nail matrix. Melanocyte dormancy in the proximal matrix results in a lower potential for involvement with melanonychia. However, almost half of the melanocytes in the distal matrix have the potential to become activated. Accordingly, longitudinal melanonychia results from one of the following events; 1. activation of previously dormant proximal melanocytes or 2. proliferation of melanocytes in the distal nail matrix.[8][9]
Melanocytic activation might occur during the following circumstances; 1. physiologically in darkly pigmented skin individuals; 2. hormonally stimulated during pregnancy; or 3. in response to inflammatory or infectious stimuli of the nail unit (including but not limited to nail psoriasis, and nail lichen planus), 4. drugs adverse effects, 5. repetitive frictional trauma, or 6. systemic disorders (Laugier-Hunziker syndrome, Peutz-Jeghers syndrome). Melanocytic activation ("functional melanonychia," "melanocytic stimulation," or "hyper melanosis") causes an increase in melanic pigmentation of the nail matrix epithelium without a concurrent increase in the number of melanocytes.
Melanocytic hyperplasia (matrix melanocyte proliferation) is a less frequent cause of longitudinal melanonychia and occurs in only three situations: nevus, lentigo, and melanoma—benign melanocytic hyperplasia results in lentigines and nevi of the nail matrix. Malignant melanocytic hyperplasia includes in situ and invasive melanoma of the nail apparatus.[10]
Histopathology
The histopathological process of subungual melanoma is unique due to the involvement of the nail unit. The pathology demonstrates an increased number of melanocytes in the basal layer of the specimen. This layer contains pleomorphic melanocytes with irregularly shaped nuclei. Invasive nail melanoma will show a high melanocyte count, two to three times that of benign melanonychia. The other features include multinucleation, atypia, and extensive pagetoid spread of melanocytes. Inflammation is also present in advanced melanoma but not demonstrated in benign melanonychia.
The histology is most likely consistent with acral lentiginous melanoma (67% of cases), a subtype of melanoma involving palms and soles. Fifty percent of cases are consistent with superficial spreading, and some cases have features of both. Acral lentiginous melanoma is characterized by acanthosis, elongation of rete ridges, and proliferation of atypical melanocytes in the epidermis. Basal keratinocytes become replaced by malignant melanocytes.
Histopathologic evaluation is the gold standard for obtaining the diagnosis of longitudinal melanonychia. Still, differentiating early-stage melanoma with the nail matrix involvement from benign melanocytic lesions is not straightforward. Accordingly, specific histopathological characteristics, including 1. cellular atypia, 2. pagetoid spread, and 3. nest formation, are common in not only melanoma in situ but also lentigines and nevi.[11] To obtain the melanoma diagnosis compared to the other potential differentials, the following main indexes should be reviewed;
Melanocytic activation – Nonspecific melanic pigmentation of the matrix epithelium with identical melanocyte numbers represents the activation of melanocytes. Early-stage melanocytic activation might be diagnosed with Fontana-Masson staining. The main advantage of Fontana-Masson staining is in cases with limited visible pigmentation. That said, pigmented dendrites and keratinocytes; and sparse melanophages without any evidence of atypia in the superficial dermis are expected.[12]
Lentigo – is identified by a mild to moderate number-wise increase in the matrix melanocytes ( 30 per mm). The increased melanocytes are individually located and aligned sparsely in the basal layer.[13] Cytologic atypia could be mildly present. The pagetoid spread is not diffuse. The pigmentation is observed only in the lower third of the nail epithelium. However, full-thickness pigmentation has been reported in some circumstances. Fontana-Masson staining indicates fine granularity of the melanin.[12]
Nevus – A melanocytic nevus of the nail matrix is identified by melanocytic hyperplasia and nest formation.[13] Further histopathologic indexes of a melanocytic nevus include; 1. a lentiginous pattern at the center of the nevus, 2. suprabasal pagetoid spread tendency,3. mild nuclear pleomorphism, and 4. periungual pigmentation.[14]
Melanoma in situ – is characterized by an increased number of melanocytes in the basal cell layer (on average 90 per mm), with a single melanocyte, a few nests, nuclear atypia, and pagetoid spreading. Atypical melanocytes, melanoma markers in situ, have large, hyperchromatic, pleomorphic nuclei and branching dendrites.[6]
History and Physical
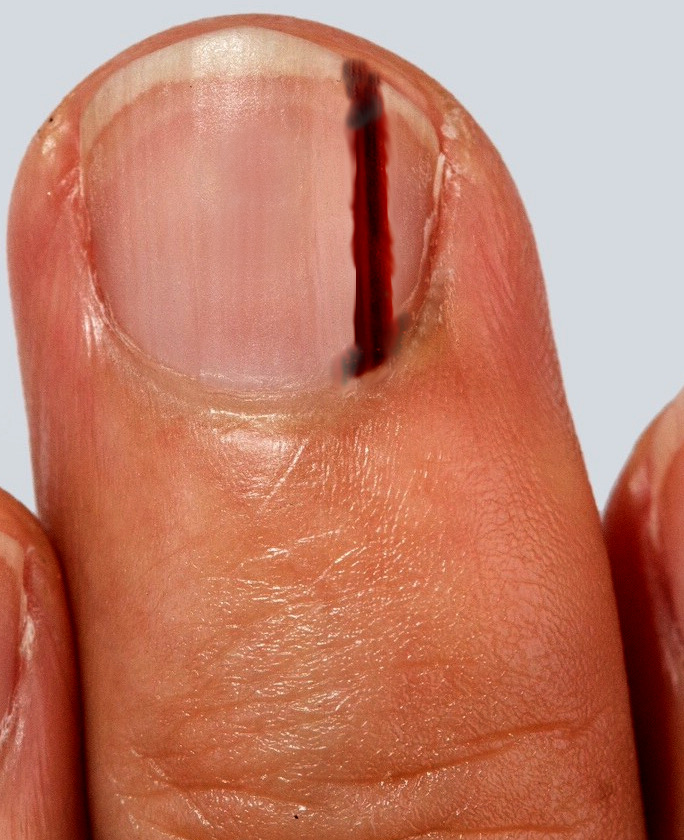
Subungual melanoma presents as brown-black discolorations of the nail bed. It can present as either a streak of pigment or irregular pigmentation. The discoloration can progress to thickening, splitting, or destruction of the nail with pain and inflammation. A periungual pigmentation (Hutchinson sign) may be present and supports the clinical diagnosis of melanoma.
Hutchinson sign and pseudo-Hutchinson sign — The Hutchinson sign is defined as the periungual discoloration of the proximal or lateral nail folds.[9][15] It was considered a pathognomonic sign of subungual melanoma. However, a periungual pigmentation may be seen in other differential diagnoses, including approximately thirty percent of patients with nail lentigines or nevi and melanonychia in patients with darkly pigmented skin, Laugier-Hunziker syndrome or Peutz-Jeghers syndrome.[16][17] It should be noted that this pigmental discoloration, in these circumstances, is called the "pseudo-Hutchinson sign."[18][19]
The history should include episodes of trauma to consider a subungual hematoma and infection to consider pigmented fungal nail conditions.
Levit et al. described the ABCDEF guidelines that can be utilized to assess for risk of a pigmented nail lesion being a melanoma. These guidelines are:
- Age: 50 to 70 years of age and African, Japanese, Chinese, and Native American heritage
- Brown-black band greater than 3 mm with an irregular border
- Change in size and growth rate
- Digit: thumb, big toe, or index finger
- Extension of discoloration into the skin surrounding the nail (Hutchinson sign)
- Family histology of melanoma
Evaluation
The primary way to make a diagnosis is with a full-thickness biopsy of the nail bed. A recent study by Reilly et al., published in December 2017, demonstrated that there could be a large disparity between the tumor thickness on initial biopsy versus the final tumor thickness. This point highlights the importance of having a good quality biopsy to make the initial histological assessment followed up with a management plan.
A nail bed biopsy should be performed using a digital nerve block. A tourniquet is useful for hemostasis, but the digit should not be exsanguinated in malignancy. The nail plate should be carefully removed using a periosteal elevator. To visualize the germinal matrix, two radial incisions can be made at 45 degrees on either side of the eponychial fold. A full-thickness biopsy should then be taken of the pigmented area. Ideally, this should be an excisional biopsy if possible. The defect is then repaired using an absorbable suture, and the nail is replaced in the eponychial fold.
Following the excisional biopsy of the pigmented lesion in the nail bed, a further management plan can be made based on the histological report. The report will detail the subtype of malignant melanoma, the Breslow thickness, and other histological characteristics.[15][16]
Treatment / Management
The multidisciplinary melanoma team will use this information to determine what further investigations are necessary and which treatment is appropriate. The mainstay of management of melanoma of any kind is excision. The initial excision is a biopsy, which offers a histological report, and guidelines determine the wide local excision margin according to the depth of a tumor. This is the same for subungual melanoma.[4][17][20]
The lymph node basins should be clinically assessed, and those with clinically palpable nodes should be further evaluated with imaging and with or without a biopsy and go on to have a lymph node dissection if the disease is detected. According to guidelines, those lesions with a thickness of 1 to 4 mm with no lymphadenopathy should be offered sentinel lymph node biopsies.
Those with tumor thicknesses greater than 4 mm should be considered for pre-operative staging with CT-PET and brain MRI scans.
Management of melanoma patients is a complex and evolving subject. Plastic surgeons should be aware of the recent changes in the field. Excisional biopsy remains the gold standard for diagnosis, although there is no evidence using other biopsy types alters survival or recurrence. Wide local excisions should be carried out with margins as recommended by National Comprehensive Cancer Network guidelines according to lesion Breslow depth, with sentinel lymph node biopsy being offered to all medically suitable candidates with intermediate thickness melanomas (1.0 to 4.0 mm) and with sentinel lymph node biopsy being considered for high-risk lesions (ulceration and/or high mitotic figures) with melanomas of 0.75 to 1.0 mm.
Differential Diagnosis
The two most common misdiagnoses of subungual melanoma are striate melanonychia and onychomycosis. Striate melanonychia is the deposition of melanin in the nail plate and is typically not a solitary pigmented streak. Onychomycosis is a fungal nail infection producing a painless, dystrophic pigment change in the nail. Other differential diagnoses include a subungual hematoma, which is usually a painful lesion that presents following trauma and migrates distally as the nail grows, and a junctional naevus, a single benign lesion not in a streaked pattern. Subungual hematoma and nail bed infections should not be ignored while evaluating a patient with suspicious subungual melanoma.
Surgical Oncology
The surgical management of subungual melanoma has been controversial for the last decade. For many years, the only acceptable option for management was digital amputation. In 1965 Das Gupta et al. conducted a study looking at the management of subungual melanoma. The study included 34 patients looking at amputation at the interphalangeal joint versus more proximal amputation. This study reported that all patients who underwent amputation at the interphalangeal joint did not survive for five years. Following this, surgeons believed that these rare cancer cases should undergo aggressive treatment in the form of proximal amputations at the level of the carpometacarpal or tarsometatarsal joint. This level of amputation can impede the function of the hand or foot affected, especially because the most common digits affected are the thumb and the hallux. The findings of this study are significant; however, the authors did not report the depth of the lesions, and half of the patients had metastatic or recurrent disease at presentation. Therefore, the treatment recommendations are perhaps a little skewed.[21][22][23]
More recently, this aggressive treatment has become less acceptable, leading to the investigation of less radical surgical options to preserve length and obtain surgical clearance. Cochran et al. published a literature review in 2014, looking specifically at the management options of subungual melanoma. This review concluded that in situ excision surgery for lower-grade melanomas and melanoma is a reasonable option. This translates as excision down to periosteum or paratenon. Other deeper, higher-grade melanomas could undergo amputation at a more distal level (interphalangeal joint) than advised by Das Gupta. However, despite the encouraging evidence that surgeons are considering less aggressive options, the data quality is weak, with no randomized controlled trials and mostly retrospective data collection. The surgical excision method remains controversial and should be assessed on a case-by-case basis.
- In situ: 0.5 cm to 1 cm
- Invasive melanoma less than 1 mm Breslow thickness: 1 cm
- One to 2 mm: 1 mm to 2 cm
- Greater than 2 mm: 2 cm
These guidelines should help to determine the excision of subungual melanoma but may need to be adjusted to allow the most functional outcome for the patient.
Those with clinically palpable nodes should be offered a lymph node dissection. The United Kingdom's national guidance is that sentinel lymph node biopsy should be offered to all patients with melanoma of a depth of 1 to 4 mm. Those with a node-positive for micrometastasis should be offered a completion lymph node dissection.
Radiation Oncology
Radiotherapy has limited use in melanoma and should only be used in specific circumstances. It is reserved for use on the lymph node basin in post-lymphadenectomy cases where there is bulky lymphadenopathy or extracapsular disease. It is also recommended for the treatment of cerebral metastases.
Medical Oncology
Immunotherapy is an option that can be discussed with patients with metastatic disease and should be offered by oncologists.
Staging
Subungual melanoma is staged using the AJCC staging and classification system. The Tumour Node Metastasis (TNM) staging is used as per other malignant melanomas.
Prognosis
Some papers have reported a worse prognosis for subungual melanoma compared to cutaneous melanomas. This is likely to be related to the late presentation of the condition. Therefore, the prognosis is likely the same as for cutaneous malignant melanoma.
The American Cancer Society has recently published up-to-date prognostic statistics:
- Stage IA: The 5-year survival rate is around 97%. The 10-year survival is approximately 95%.
- Stage IB: The 5-year survival rate is around 92%. The 10-year survival is approximately 86%.
- Stage IIA: The 5-year survival rate is around 81%. The 10-year survival is approximately 67%.
- Stage IIB: The 5-year survival rate is around 70%. The 10-year survival is approximately 57%.
- Stage IIC: The 5-year survival rate is around 53%. The 10-year survival is approximately 40%.
- Stage IIIA: The 5-year survival rate is around 78%. The 10-year survival is approximately 68%.
- Stage IIIB: The 5-year survival rate is around 59%. The 10-year survival is approximately 43%.
- Stage IIIC: The 5-year survival rate is around 40%. The 10-year survival is approximately 24%.
- Stage IV: The 5-year survival rate is about 15% to 20%. The 10-year survival is about 10% to 15%. The outlook is better if the spread is only to distant parts of the skin or distant lymph nodes rather than to other organs and if the blood level of lactate dehydrogenase (LDH) is normal.
Complications
Nail dystrophy can occur after surgery. A cosmetic deformity is universally seen in all patients.
Postoperative and Rehabilitation Care
Those patients who refuse a biopsy should be closely monitored.
Deterrence and Patient Education
Patients need to understand that subungual melanoma is not correlated with sun exposure. In the future, they should exercise good hand and foot hygiene, which may be of some benefit. They should also inspect their nails and nail beds for signs of recurrence or other new lesion development.
Pearls and Other Issues
The key points to remember for subungual melanoma are:
- It has the same histopathological process as cutaneous malignant melanoma.
- Some studies suggest it is more aggressive than cutaneous malignant melanoma, but this is likely due to late presentation.
- It should be diagnosed using an excision or an incision biopsy.
- The excision margin is determined by the depth of the tumor and may lead to the amputation of part or all of the digit.
Enhancing Healthcare Team Outcomes
Subungual melanoma is most common in non-White race persons, with both men and women having equal risk, and requires the efforts of an interprofessional healthcare team. This team includes clinicians (MDs, DOs, NPs, and PAs), dermatological specialists, nursing staff, and pharmacists. Like other forms of melanoma, subungual melanoma can also spread to other parts of the body and is lethal. The key to diagnosis and early treatment is awareness. All healthcare team members, including nurses, should routinely examine the nails and maintain a high index of suspicion for any pigmented lesion on the nails. The only way to reduce the high mortality is an early referral to a dermatologist for a biopsy. Further, the nurse should educate patients on examining their skin and nails for unusual changes. Finally, both the nurse and the pharmacist should educate the public about using sunscreen when going outdoors and wearing protective clothing when going outdoors. Sunglasses are also recommended as the sun's UV rays can damage the retinal cells.[24][25] [Level 5]
Outcomes
For early lesions, the outcomes are good, but for advanced lesions, the outcomes are poor. Disease-free survival is not affected by the type of surgery on the nail. The earlier the diagnosis, the better the survival.[26][27] [Level 5]