[1]
Runge C, Jensen JM, Clemmesen L, Knudsen HB, Holm C, Børglum J, Bendtsen TF. Analgesia of Combined Femoral Triangle and Obturator Nerve Blockade Is Superior to Local Infiltration Analgesia After Total Knee Arthroplasty With High-Dose Intravenous Dexamethasone. Regional anesthesia and pain medicine. 2018 May:43(4):352-356. doi: 10.1097/AAP.0000000000000731. Epub
[PubMed PMID: 29346228]
[2]
Ishiguro S, Yokochi A, Yoshioka K, Asano N, Deguchi A, Iwasaki Y, Sudo A, Maruyama K. Technical communication: anatomy and clinical implications of ultrasound-guided selective femoral nerve block. Anesthesia and analgesia. 2012 Dec:115(6):1467-70. doi: 10.1213/ANE.0b013e31826af956. Epub 2012 Aug 10
[PubMed PMID: 22886842]
[3]
Watanabe T, Ogihara H, Soeta T, Fujiwara T, Yoshida H. Comparison of range of motion during movement from supine to sitting position in healthy young and elderly participants. Journal of physical therapy science. 2019 Jan:31(1):102-107. doi: 10.1589/jpts.31.102. Epub 2019 Jan 29
[PubMed PMID: 30774215]
[4]
Gold M, Munjal A, Varacallo M. Anatomy, Bony Pelvis and Lower Limb, Hip Joint. StatPearls. 2024 Jan:():
[PubMed PMID: 29262200]
[6]
Gupton M, Imonugo O, Black AC, Launico MV, Terreberry RR. Anatomy, Bony Pelvis and Lower Limb, Knee. StatPearls. 2024 Jan:():
[PubMed PMID: 29763193]
[7]
Sheeba CJ, Andrade RP, Palmeirim I. Getting a handle on embryo limb development: Molecular interactions driving limb outgrowth and patterning. Seminars in cell & developmental biology. 2016 Jan:49():92-101. doi: 10.1016/j.semcdb.2015.01.007. Epub 2015 Jan 21
[PubMed PMID: 25617599]
[8]
Stainton H, Towers M. Polarizing Region Tissue Grafting in the Chick Embryo Limb Bud. Methods in molecular biology (Clifton, N.J.). 2018:1863():143-153. doi: 10.1007/978-1-4939-8772-6_8. Epub
[PubMed PMID: 30324596]
[9]
Mróz I, Kielczewski S, Pawlicki D, Kurzydło W, Bachul P, Konarska M, Bereza T, Walocha K, Kaythampillai LN, Depukat P, Pasternak A, Bonczar T, Chmielewski P, Mizia E, Skrzat J, Mazur M, Warchoł Ł, Tomaszewski K. Blood vessels of the shin - anterior tibial artery - anatomy and embryology - own studies and review of the literature. Folia medica Cracoviensia. 2016:56(1):33-47
[PubMed PMID: 27513837]
[10]
Rivera RE, Hootnick DR, Gingold AR, Levinsohn EM, Kruger LM, Packard DS Jr. Anatomy of a duplicated human foot from a limb with fibular dimelia. Teratology. 1999 Nov:60(5):272-82
[PubMed PMID: 10525205]
[11]
Dennis SC, Berkland CJ, Bonewald LF, Detamore MS. Endochondral ossification for enhancing bone regeneration: converging native extracellular matrix biomaterials and developmental engineering in vivo. Tissue engineering. Part B, Reviews. 2015 Jun:21(3):247-66. doi: 10.1089/ten.TEB.2014.0419. Epub 2014 Dec 4
[PubMed PMID: 25336144]
[12]
Sun Q, Fan G, Li X, Gong J, Ge W, Cai M. Relationship Between Femur and Femoral Arteries for Identifying Risk Factors for Vascular Injury. Medical science monitor : international medical journal of experimental and clinical research. 2017 Apr 10:23():1733-1740
[PubMed PMID: 28392552]
[13]
Mednick RE, Alvi HM, Morgan CE, Stover MD, Manning DW. Femoral vein blood flow during a total hip arthroplasty using a modified Heuter approach. The Journal of arthroplasty. 2015 May:30(5):786-9. doi: 10.1016/j.arth.2014.12.015. Epub 2014 Dec 17
[PubMed PMID: 25660612]
[14]
Portugal IB, Ribeiro Ide L, Sousa-Rodrigues CF, Monte-Bispo RF, Rocha AC. Distribution of saphenous vein valves and its practical importance. Revista brasileira de cirurgia cardiovascular : orgao oficial da Sociedade Brasileira de Cirurgia Cardiovascular. 2014 Oct-Dec:29(4):564-8. doi: 10.5935/1678-9741.20140038. Epub
[PubMed PMID: 25714210]
[15]
Rao AS, Rajmanickam K, Narayanan GS. Study of distribution of inguinal nodes around the femoral vessels and contouring of inguinal nodes. Journal of cancer research and therapeutics. 2015 Jul-Sep:11(3):575-9. doi: 10.4103/0973-1482.163735. Epub
[PubMed PMID: 26458584]
[16]
Fracol ME, Janes LE, Ko JH, Dumanian GA. Targeted Muscle Reinnervation in the Lower Leg: An Anatomical Study. Plastic and reconstructive surgery. 2018 Oct:142(4):541e-550e. doi: 10.1097/PRS.0000000000004773. Epub
[PubMed PMID: 30020229]
[17]
Swezey E, Bordoni B. Anatomy, Bony Pelvis and Lower Limb: Lateral Femoral Cutaneous Nerve. StatPearls. 2024 Jan:():
[PubMed PMID: 30335334]
[18]
Kendir S, Torun Bİ, Akkaya T, Comert A, Tuccar E, Tekdemir I. Re-defining the anatomical structures for blocking the nerves in adductor canal and sciatic nerve through the same injection site: an anatomical study. Surgical and radiologic anatomy : SRA. 2018 Nov:40(11):1267-1274. doi: 10.1007/s00276-018-2094-1. Epub 2018 Aug 23
[PubMed PMID: 30167824]
[19]
Üçeyler N, Vollert J, Broll B, Riediger N, Langjahr M, Saffer N, Schubert AL, Siedler G, Sommer C. Sensory profiles and skin innervation of patients with painful and painless neuropathies. Pain. 2018 Sep:159(9):1867-1876. doi: 10.1097/j.pain.0000000000001287. Epub
[PubMed PMID: 29863528]
[20]
Migirov A, Arbor TC, Vilella RC. Anatomy, Abdomen and Pelvis: Adductor Canal (Subsartorial Canal, Hunter Canal). StatPearls. 2024 Jan:():
[PubMed PMID: 32310506]
[21]
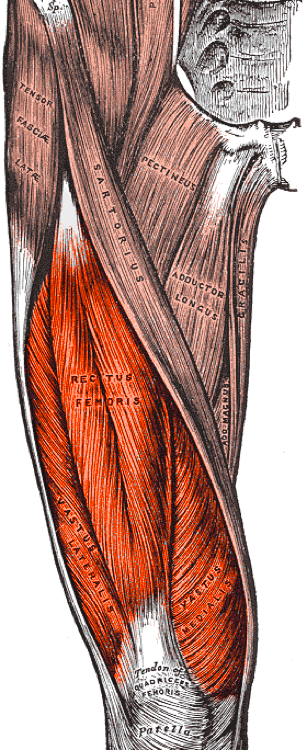
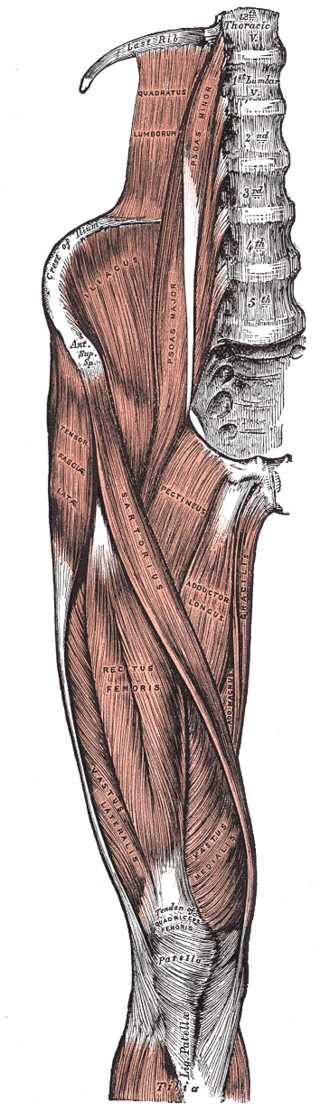
Launico MV, Sinkler MA, Nallamothu SV. Anatomy, Bony Pelvis and Lower Limb: Femoral Muscles. StatPearls. 2024 Jan:():
[PubMed PMID: 29763184]
[22]
Yamauchi K, Kato C, Kato T. Characteristics of individual thigh muscles including cross-sectional area and adipose tissue content measured by magnetic resonance imaging in knee osteoarthritis: a cross-sectional study. Rheumatology international. 2019 Apr:39(4):679-687. doi: 10.1007/s00296-019-04247-2. Epub 2019 Jan 28
[PubMed PMID: 30689015]
Level 2 (mid-level) evidence
[23]
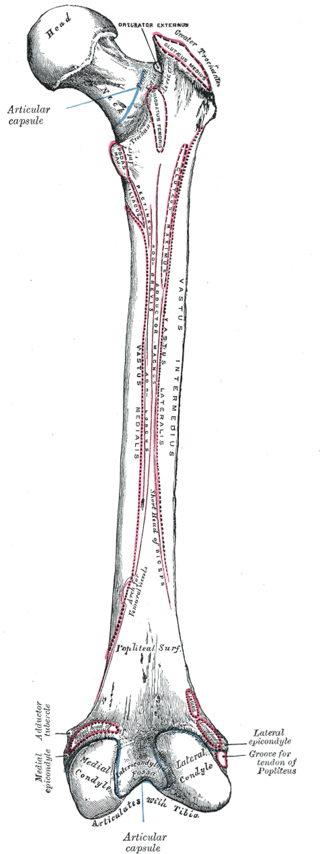
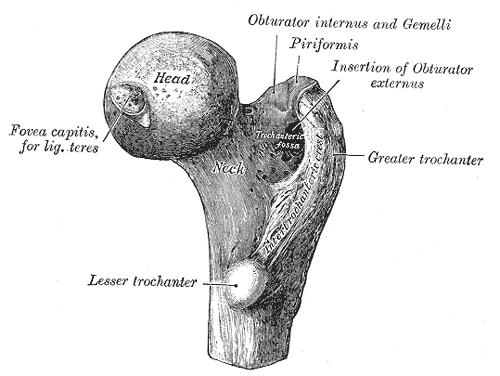
Chang A, Breeland G, Black AC, Hubbard JB. Anatomy, Bony Pelvis and Lower Limb: Femur. StatPearls. 2024 Jan:():
[PubMed PMID: 30422577]
[24]
Hartel MJ, Petersik A, Schmidt A, Kendoff D, Nüchtern J, Rueger JM, Lehmann W, Grossterlinden LG. Determination of Femoral Neck Angle and Torsion Angle Utilizing a Novel Three-Dimensional Modeling and Analytical Technology Based on CT Datasets. PloS one. 2016:11(3):e0149480. doi: 10.1371/journal.pone.0149480. Epub 2016 Mar 2
[PubMed PMID: 26933877]
[25]
Seto AH, Tyler J, Suh WM, Harrison AT, Vera JA, Zacharias SJ, Daly TS, Sparling JM, Patel PM, Kern MJ, Abu-Fadel M. Defining the common femoral artery: Insights from the femoral arterial access with ultrasound trial. Catheterization and cardiovascular interventions : official journal of the Society for Cardiac Angiography & Interventions. 2017 Jun 1:89(7):1185-1192. doi: 10.1002/ccd.26727. Epub 2016 Aug 27
[PubMed PMID: 27566991]
[26]
Nasr AY, Badawoud MH, Al-Hayani AA, Hussein AM. Origin of profunda femoris artery and its circumflex femoral branches: anatomical variations and clinical significance. Folia morphologica. 2014 Feb:73(1):58-67. doi: 10.5603/FM.2014.0008. Epub
[PubMed PMID: 24590524]
[27]
Yu SK, Chung TT, Yeh CC, Cherng CH, Lin SL. A patient with femoral triangle anatomy transposition challenges NAVY rule. Journal of clinical anesthesia. 2018 Feb:44():80-81. doi: 10.1016/j.jclinane.2017.11.014. Epub
[PubMed PMID: 29161543]
[28]
Radowsky JS, Rodriguez CJ, Wind GG, Elster EA. A Surgeon's Guide to Obtaining Hemorrhage Control in Combat-Related Dismounted Lower Extremity Blast Injuries. Military medicine. 2016 Oct:181(10):1300-1304
[PubMed PMID: 27753567]
[29]
Waewsawangwong W, Ruchiwit P, Huddleston JI, Goodman SB. Hip arthroplasty for treatment of advanced osteonecrosis: comprehensive review of implant options, outcomes and complications. Orthopedic research and reviews. 2016:8():13-29. doi: 10.2147/ORR.S35547. Epub 2016 Jun 28
[PubMed PMID: 30774467]
[30]
Liu C, Von Keudell A, McTague M, Rodriguez EK, Weaver MJ. Ideal length of thread forms for screws used in screw fixation of nondisplaced femoral neck fractures. Injury. 2019 Mar:50(3):727-732. doi: 10.1016/j.injury.2019.01.036. Epub 2019 Jan 31
[PubMed PMID: 30772052]
[31]
Gao YS, Guo YJ, Yu XG, Chen Y, Chen C, Lu NJ. A novel cerclage wiring technique in intertrochanteric femoral fractures treated by intramedullary nails in young adults. BMC musculoskeletal disorders. 2018 Oct 6:19(1):359. doi: 10.1186/s12891-018-2284-3. Epub 2018 Oct 6
[PubMed PMID: 30292231]
[32]
Streubel PN, Gardner MJ, Ricci WM. Management of femur shaft fractures in obese patients. The Orthopedic clinics of North America. 2011 Jan:42(1):21-35, v. doi: 10.1016/j.ocl.2010.07.004. Epub 2010 Oct 8
[PubMed PMID: 21095432]
[33]
Christ AB, Chawla H, Gausden EB, Villa JC, Wellman DS, Lorich DG, Helfet DL. Radiographic and Clinical Outcomes of Periprosthetic Distal Femur Fractures Treated With Open Reduction Internal Fixation. Journal of orthopaedic trauma. 2018 Oct:32(10):515-520. doi: 10.1097/BOT.0000000000001265. Epub
[PubMed PMID: 30247279]
Level 2 (mid-level) evidence
[35]
Wong WY, Bjørn S, Strid JM, Børglum J, Bendtsen TF. Defining the Location of the Adductor Canal Using Ultrasound. Regional anesthesia and pain medicine. 2017 Mar/Apr:42(2):241-245. doi: 10.1097/AAP.0000000000000539. Epub
[PubMed PMID: 28002228]
[36]
Aso K, Izumi M, Sugimura N, Okanoue Y, Kamimoto Y, Yokoyama M, Ikeuchi M. Additional benefit of local infiltration of analgesia to femoral nerve block in total knee arthroplasty: double-blind randomized control study. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA. 2019 Jul:27(7):2368-2374. doi: 10.1007/s00167-018-5322-7. Epub 2018 Dec 8
[PubMed PMID: 30536047]
Level 1 (high-level) evidence
[37]
Saugel B, Scheeren TWL, Teboul JL. Ultrasound-guided central venous catheter placement: a structured review and recommendations for clinical practice. Critical care (London, England). 2017 Aug 28:21(1):225. doi: 10.1186/s13054-017-1814-y. Epub 2017 Aug 28
[PubMed PMID: 28844205]