Continuing Education Activity
Skin grafts consist of fully detached pieces of skin taken from one anatomic site and placed in a wound elsewhere. Full-thickness skin grafts include the full thickness of both the epidermis and dermis. This activity describes and explains the role of the surgeon and nursing assistants in performing this procedure and identifying situations in which this represents an appropriate option in re-establishing function and appearance in patients who have undergone excisional surgery.
Objectives:
- Identify the anatomical structures, skin and wound characteristics, indications, and contraindications of full-thickness skin graft technique.
- Describe the equipment, personnel, preparation, and technique in regards to performing full-thickness skin grafting.
- Outline the evaluation of the potential complications and clinical significance of full-thickness skin grafts.
- Explain interprofessional team strategies for enhancing coordination and communication to advance surgical outcomes.
Introduction
A skin graft is a cutaneous free tissue transfer that is separated from a donor site and transplanted to a recipient site.[1][2] Skin grafts are chosen when healing by second intention, primary closure, or flap repair are deemed unsuitable. Full-thickness skin grafts (FTSGs) consist of complete epidermis and dermis, whereas partial-thickness skin grafts (PTSG) include the entire epidermis and only partial dermis. FTSGs are relatively simple to harvest and to secure within the recipient site, and they are particularly well suited to defects on the nasal tip, dorsum, ala, and sidewall as well as on the eyelids and the ears.[3] Optimal donor skin should closely match color, thickness, the degree of actinic damage, and texture of the skin surrounding the defect. Advantages of FTSGs are that they do not alter the architecture of the recipient site and are relatively easy for both the patient and the surgeon. The main complication of this procedure is that partial or full-thickness graft failure may occur. FTSGs have advantages over PTSGs, and these include less contraction on healing, generally better aesthetic result, and thicker skin that is more resistant trauma. However, FTSGs also have a greater risk of graft failure, are more limited in the size of defects and choice of the donor site, and the donor defect must be closed or proceed through a lengthier period of second intention healing.
Anatomy and Physiology
Skin grafts can technically be harvested from virtually any area of skin on the body, although certain areas are preferable. Full-thickness skin grafts (FTSGs) consist of complete epidermis and dermis, whereas partial-thickness skin grafts (PTSG) include the entire epidermis and only partial dermis. One should try to match, as closely as possible, the skin at the recipient site. Among the variables to consider are skin thickness, number, and prominence of sebaceous glands, presence or absence of hair, skin color, and amount of actinic damage. Some areas that are particularly useful for skin harvest are the pre- and postauricular areas, clavicular skin, and inner arm among others. Sites in which grafts are most commonly useful include the nasal tip, dorsum, ala, and sidewall as well as the eyelids and the ears.
Graft survival depends on the ingrowth of capillaries from the recipient site for survival, so a viable base of tissue with some vascularity is needed. Provision of vascularity from peripheral to the wound, or "bridging," may supply up to about 5 mm of the periphery of the graft. A defect without adequate vascularity may be allowed to heal secondarily for a time to allow growth of granulation tissue, and then a delayed graft may be performed. Alternately, a muscle or soft tissue flap may be moved into the wound base, providing a vascular bed for the graft.[4] In the first 24 hours after placement, the graft absorbs transudate from the recipient bed and becomes edematous, a stage known as "plasmatic imbibition." Fibrin acts as a physiologic adhesive that holds the graft in place during this time. The fibrin is eventually replaced by granulation tissue. Vascular anastomoses between the recipient bed and donor graft begin to develop at about 48 to 72 hours after grafting. This process is known as "inosculation." Full circulation is restored within 4 to 7 days, and a lymphatic circulation occurs within 7 days. Although re-innervation of the graft begins 2 to 4 weeks after grafting, full sensation may require several months or even years to return to normal.
Indications
Skin grafts are chosen when healing by second intention, primary closure, or flap repair are deemed unsuitable. They are particularly well-suited to defects on the nasal tip, dorsum, ala, and sidewall as well as the eyelids and the ears.
Contraindications
Graft survival depends on the ingrowth of capillaries from the recipient site for survival, so a viable base of tissue with some vascularity is needed. Therefore, full-thickness skin grafts should not be placed in defects of any size without an underlying blood supply. For example, large (> 1 cm) areas of exposed bone or cartilage are not optimal for graft placement. Smoking significantly compromises oxygenation of tissue and should be stopped before graft placement if possible.
Equipment
Essential equipment is minimal and includes the following:
Preoperatively
- Local anesthetic (typically lidocaine 0.5% with epinephrine 1:200,000 and buffered with sodium bicarbonate)
- 3 cc syringe(s)
- 30 gauze needle(s)
- Antiseptic scrub
- Surgical marker
- Foil or other material for a template of defect
Intraoperatively
- Sterile drape
- Scalpel with #15 blade
- Toothed forceps
- Serrated scissors (for trimming away fat from graft)
- Suture scissors
- Needle holders
- Normal saline
- Sterile gauze
- Absorbable suture (for subcutaneous/deep stitches)
- Cutaneous suture (non-absorbable or absorbable)
- Ideally, an electrosurgical device should be available for hemostasis
Postoperatively
- Nonstick dressing
- Petrolatum-infused gauze strip or other material to form a bolster over the graft site. This may be sutured or taped securely in place to provide some pressure and to keep graft immobilized.
- Sterile ointment (author prefers sterile petrolatum to antibiotic ointment as significant numbers of patients develop allergies to bacitracin and neomycin, while their ability to decrease infection is minimal)
- Adhesive dressing, preferably hypoallergenic and stretchy.
- Additional adhesive liquid may be used to further secure dressing
Personnel
Full-thickness skin grafts can be performed by one surgeon and one surgical assistant.
Preparation
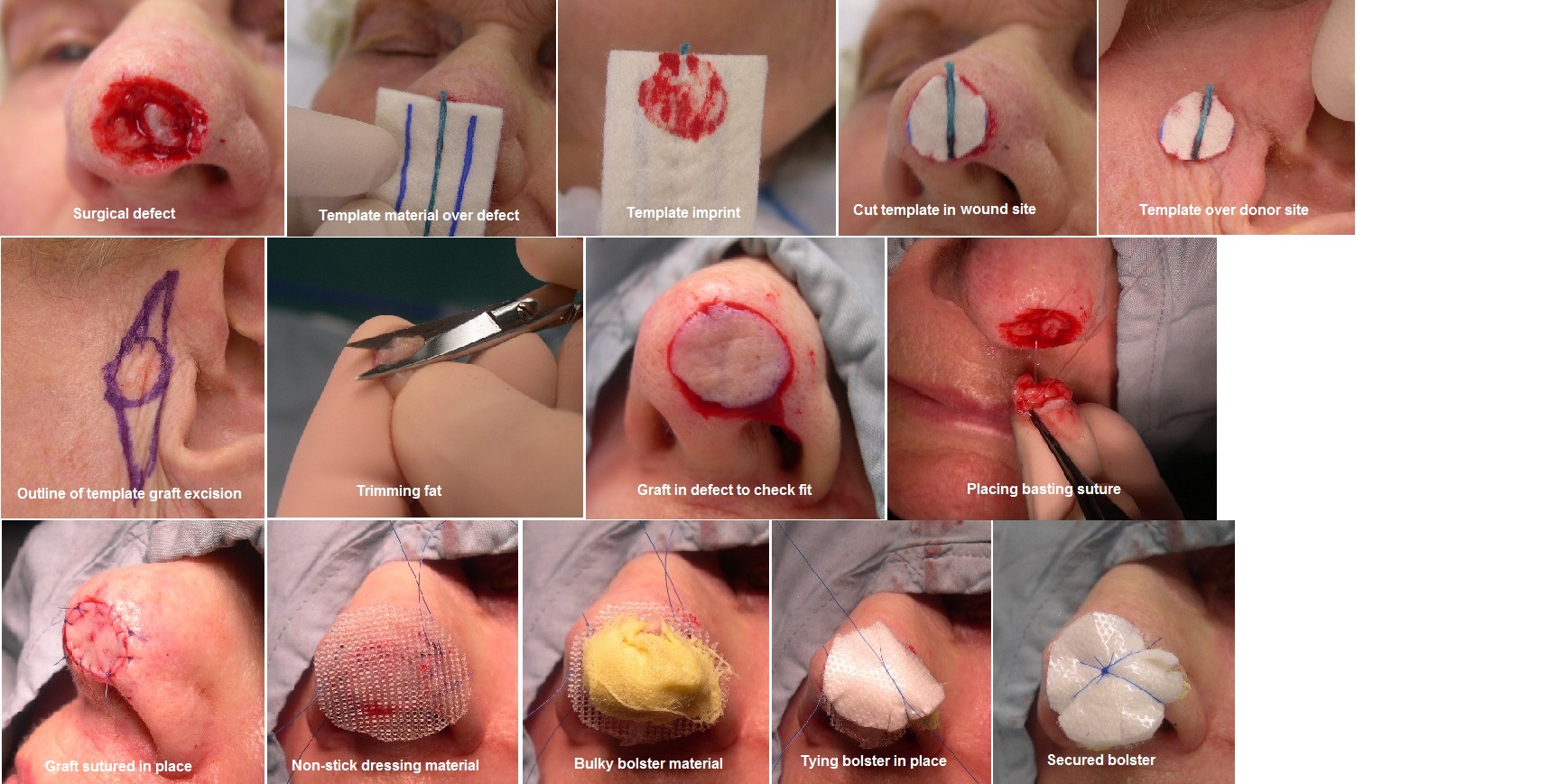
The donor site should be chosen from an area with optimal tissue match and preferably in an area of least significant scarring. When taking a graft, it is often best to make a template of the wound to guide the graft design. A template is made of the surgical defect with foil from a suture packet or other malleable material and then placed over the donor site. This template is then outlined in the donor site with a surgical marker, and then both the donor and recipient sites are locally anesthetized and prepped in the usual sterile fashion.
Technique or Treatment
Once harvested, the graft should be trimmed of all underlying adipose and hair structures, if present. The graft is then secured with simple interrupted sutures, and the donor site is repaired with a layered closure. Particularly on the nose, the surgical defect may be partially closed, taking a Burow's triangle of adjacent skin to facilitate tissue movement. The Burow's triangle of skin can then be used as a FTSG to repair the remainder of the defect.[5],[6] The graft is generally left in place for one week. The graft must maintain direct contact with the underlying wound bed, and it should remain immobile during this time. Basting sutures may be placed within the graft to secure it to the bed, and it is important to apply a secure pressure dressing, with or without a sutured bolster, over the surgical site. The patient should avoid trauma to the site and strenuous activity for at least 2 weeks after surgery.
Complications
Complete or partial graft failure is the main complication with FTSGs, and it may be caused by hematoma, disruption of base-graft contact, infection, smoking, or excessive intra-operative electrocoagulation. If necrosis does occur, it is generally best to not remove the graft; rather, it is left in place to serve as "scaffolding" for new skin growth. Full-thickness skin grafts should not be harvested from or placed into infected tissue. Smoking is a relative contraindication, and heavy smokers (more than 1 pack per day) have been found to be 3 times more likely to experience necrosis of their flaps. Smoking should be discontinued at least 2 days before surgery and not resumed for at least 1 week after graft placement. Obtaining a preoperative consultation with the hematologist is prudent.
Clinical Significance
Full-thickness skin grafts can provide skin coverage in wounds in which healing by second intention, primary closure, or flap repair would not be optimal.
Enhancing Healthcare Team Outcomes
The surgeon should be competent in basic surgical skills, including the following:
- Sterile procedure
- Skin excision and wound closure
- Handling of tissue, including trimming of underlying fat from the skin
- Fine suturing
- Precise electrocoagulation to obtain adequate hemostasis without excessive tissue char
The surgical assistant must be:
- Familiar with the instruments used in this procedure
- Trained in maintaining sterility of the surgical field and tray
- Highly competent in the design and placement of secure dressings that apply optimal pressure and stability