Continuing Education Activity
Epidermoid cysts, also known as a sebaceous cysts, are encapsulated subepidermal nodules filled with keratin. Although most commonly located on the face, neck, and trunk, epidermoid cysts can form anywhere on the body. Sebaceous cysts are generally considered to be benign, however new evidence indicates that they can develop de novo malignancy. This activity reviews the presentation, evaluation, and management of sebaceous cysts and highlights the role of the interprofessional team caring for patients affected by this condition.
Objectives:
- Identify the etiology of sebaceous cysts.
- Describe the typical presentation of a patient with a sebaceous cyst.
- Review the management options available for sebaceous cysts.
- Describe interprofessional team strategies to improve care coordination and management for patients with sebaceous cysts.
Introduction
Epidermoid cyst, also known as a sebaceous cyst, is a benign encapsulated, subepidermal nodule filled with keratin material. Although most commonly located on the face, neck, and trunk, epidermoid cysts can be found anywhere including the scrotum, genitalia, fingers, and cases within the buccal mucosa. Cysts may progress slowly and remain present for years. The term sebaceous cyst is commonly used; however, the term is a misnomer in that it does not involve the sebaceous gland. Epidermoid cysts develop within the infundibulum. Other common synonyms include infundibular cyst, epidermal cyst, and epidermal inclusion cyst. Although these cysts are recognized as benign lesions, rare malignancy can arise.[1][2][3]
Etiology
The majority of cases are of epidermoid cysts are sporadic. Although epidermoid cysts can be found in autosomal dominant (AD) Gardner syndrome (familial adenomatous polyposis) and Gorlin syndrome (basal cell nevus syndrome). Epidermoid cysts occurring before puberty in unusual locations and numbers raise the suspicion of a syndrome. In Favre-Racouchot syndrome (nodular elastosis with cysts and comedones) in elderly patients, epidermoid cysts may result from chronic sun damage. Patients on BRAF inhibitors can develop epidermoid cysts of the face. Lately, imiquimod and cyclosporine have been noted to cause epidermal inclusion cysts.[4][5][6]
Epidemiology
Epidermoid cysts are the most common cutaneous cysts and typically occur in the third and fourth decades of life. It is rare to find these cysts before puberty. They are predominantly found in males versus females (ratio 2:1). In the neonatal period, small epidermal cysts, referred to as milia, are common. Approximately 1% of epidermoid cysts have been noted to have a malignant transformation to squamous cell carcinoma (SCC) and basal cell carcinoma (BCC).
Pathophysiology
Epidermoid cysts are derived from the follicular infundibulum. Generally, these cysts are the result of plugging of the follicular orifice. The cyst communicates with the surface of the skin through a keratin-filled orifice. Disruption of the follicle is important in the pathogenesis as those with acne vulgaris may have multiple epidermoid cysts originating from comedones. Additionally, they can also occur from traumatic and penetrate injuring leading to the implantation of the epithelium. Epidermoid cysts are lined with stratified squamous epithelium that leads to an accumulation of keratin within the subepidermal layer or dermis. Generally, the cysts are asymptomatic until they rupture. When the cysts rupture, an inflammatory reaction occurs from the displacement of soft and yellow keratin into the dermis and surrounding tissue. Recently ultraviolet (UV) light and infection with the human papillomavirus (HPV) have been implicated as causing epidermoid cysts.
Histopathology
Stratified squamous epithelium lines the cyst. Histological examination reveals an epithelial-lined cyst filled with laminated keratin located within the dermis. The lining of the cyst is similar to the surface epithelium but differs in that it lacks rete ridges. A granular layer is present that is filled with keratohyalin granules.
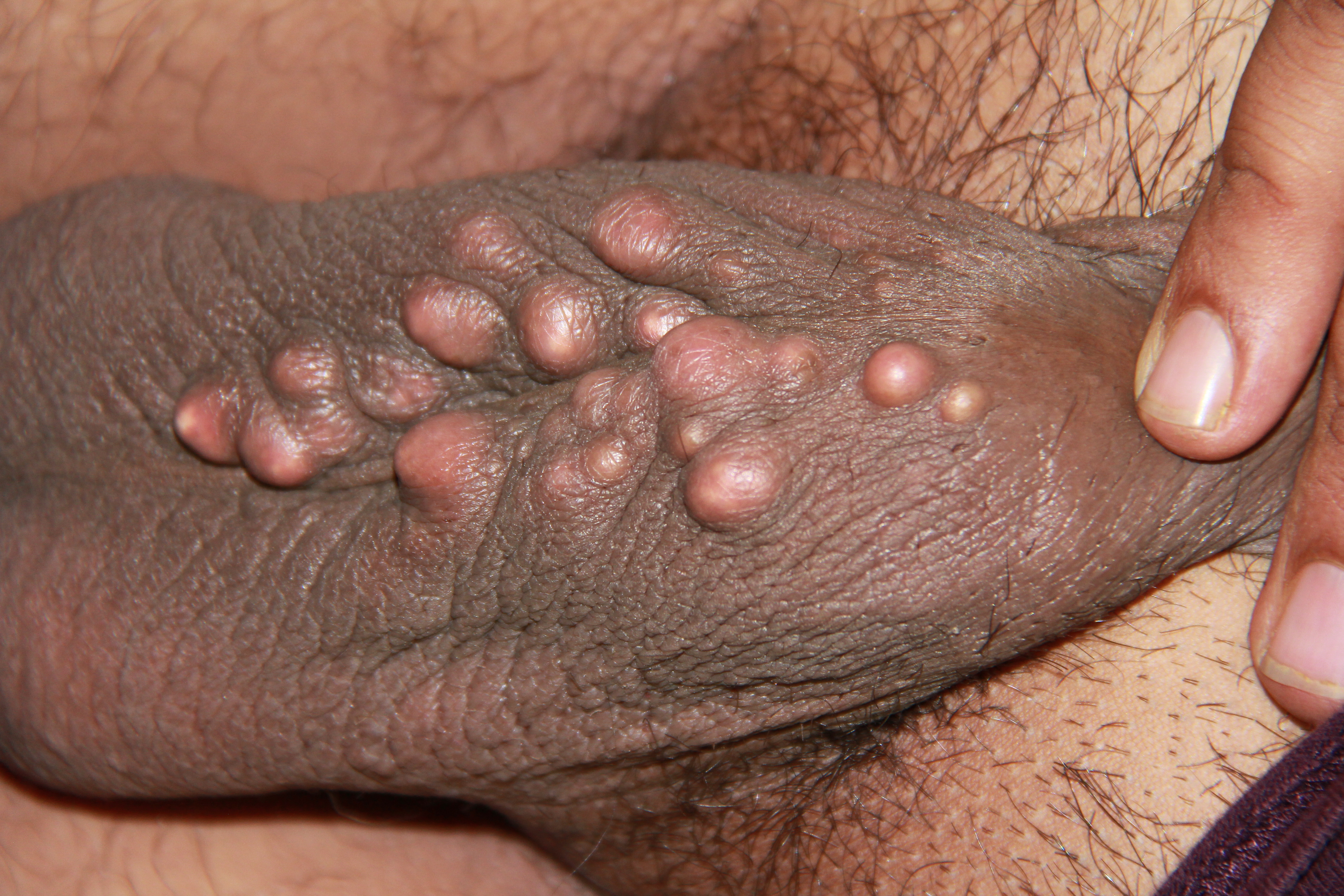
History and Physical
Physical examination generally reveals a 0.5 cm to several centimeters of non-fluctuant, compressible mass. A central, dark comedone opening (punctum) is often described. Epidermoid cysts are usually asymptomatic; however, if ruptured it may closely resemble a furuncle with tenderness to palpation, erythema, and swelling. A foul-smelling yellowish cheese-like material discharged from the skin may be described. Some patients may describe an event of a fall on their back or someone slapping their back causing painful swelling and the resulting cystic rupture. Epidermoid cysts can be found anywhere but are commonly found on the face, neck, chest, upper back, scrotum, and genitals. They can also be found on the buttocks, palms, and plantar side of feet if due to penetrating trauma. If occurring on the distal portion of the fingers, changes to the nail plate may occur. Taking a good history can aid in determining if the cyst is an isolated case, caused by medications, or if it is part of a genetic syndrome.
Evaluation
Evaluation of epidermoid cysts is based largely upon history and physical. The need for histological examination of the excised mass is often debated. Laboratory examination is not necessary. Radiographic tests are not commonly utilized in the evaluation of epidermoid cysts.
Treatment / Management
The most effective treatment involves complete surgical excision of the cyst with the cyst wall intact. The complete excision should be delayed if an active infection is present as the planes of dissection will be difficult. In these cases an initial incision and drainage may be indicated with a potential for reoccurrence in the future A local anesthetic with epinephrine is preferred to minimize bleeding. The anesthetic should be injected around the cyst, with avoidance of direct injection into the cyst. A small diameter elliptical incision with the inclusion of the central core, or punctum can be utilized. For optimal cosmetic results, maintaining the incision in the minimal skin tension lines is important. A multiple-layered subcuticular and epidermal closure will yield an optimal outcome. An alternative surgical approach can also be done with a punch biopsy and expulsion of the intact cyst through the small defect or standard excision. If there is surrounding inflammation, intralesional triamcinolone may be used to help decrease inflammation in addition to a delay in surgical removal. If the cyst has ruptured and the lining destroyed, the cyst will not reoccur. However, removing of the entire cystic lining is important in decreasing recurrence.[7][8][9]
Differential Diagnosis
Depending on location, the differential diagnoses of epidermoid cysts include the following: lipoma, dermoid cyst, pilar cyst (isthmus-catagen cyst, trichilemmal, wen), furuncle, branchial cleft cyst, milia, pilonidal cyst, calcinosis cutis, Pachyonychia Congenita, steatocystoma, and cutaneous findings of Gardner syndrome.
Prognosis
Epidermal inclusion cysts are recognized as benign cysts. However, rare malignancy can occur. Squamous cell carcinoma (SCC) is the most common malignancy followed by basal cell carcinoma (BCC). In developing malignancy, squamous cell carcinoma occurs approximately 70% of the time.
Complications
Complications of rupture include erythema, swelling, and pain. Complications of surgical removal include bleeding, infection, and scaring. Erythema and pain can be managed with intralesional triamcinolone. Infection following surgery can be prevented using proper aseptic techniques. While recognized as a benign cyst, rare malignancy may occur.
Postoperative and Rehabilitation Care
Following surgical excision, it appropriate to avoid contact sports and strenuous activity. Sutures may be removed within 7-10 days. Patients should be instructed on the fact that the surgical scar will generally take 8 weeks to reach a maximum of 80% tensile strength of the original skin strength. Scar revision, if necessary, should take place between 6 months to 1 year following excision as the remodeling phase of wound healing occurs between 3 weeks to 1 year.
Consultations
Consultations are not necessary unless the cyst is large and in an unusual location such as the mouth or face. In those circumstances, specialist consultation may be warranted. Adults with epidermoid cysts in rare locations such as the fingers and toes, history of multiple lipomas, and a family history of colon cancer should raise the suspicion of Gardner syndrome with an appropriate specialist referral.
Pearls and Other Issues
Epidermoid cysts (sebaceous cysts) are common benign encapsulated cysts. Due to the inflammatory reaction from the release of keratin contents, many practitioners will mistake the cyst for an abscess and prescribe antibiotics.
Enhancing Healthcare Team Outcomes
Epidermal cysts are commonly encountered by the primary care provider, dermatologist, nurse practitioner, surgeon and the internist. While the majority of these cysts are benign, it is important to send the excised sample for evaluation to ensure that there is no malignancy.
When completely excised, the outcomes are excellent. However, recurrences are common in patients with genetic syndromes.[10]