Continuing Education Activity
Metacarpal fractures are a prevalent concern, comprising 40% of all hand fractures. Particularly affecting an active and youthful demographic are 5th metacarpal fractures, also known as boxer's fractures. These injuries can impair grip strength and dexterity, which are essential for various daily activities and sports. Without proper treatment, boxer's fractures in the young are at risk for malunion or nonunion due to their active lifestyles. Chronic pain, weakness, and hand function limitations may result if the condition is not properly addressed. Nonoperative and operative treatments may be considered, depending on the fracture type and severity.
This activity for healthcare professionals is designed to enhance learners' competence in evaluating and managing 5th metacarpal fractures. Participants in this activity gain in-depth insights into the etiology, presentation, evaluation, and management of these injuries. Treatment strategies are meticulously explored, differentiating between open and closed fractures and considering factors such as angulation, shortening, and rotation. This activity also underscores the interprofessional healthcare team's pivotal role in improving patient outcomes and mitigating the potential economic impact of missed workdays.
Objectives:
Identify the signs and symptoms indicative of a 5th metacarpal fracture.
Determine critical diagnostic imaging studies when evaluating patients with a suspected 5th metacarpal fracture.
Compare the treatment options available for 5th metacarpal fractures, including both conservative and surgical care.
Improve interprofessional coordination and communication practices when formulating short- and long-term care plans for individuals with 5th metacarpal fractures.
Introduction
Overview of Fifth Metacarpal Fractures
Metacarpal fractures account for 40% of all hand fractures.[1] Fifth metacarpal injuries account for 20% of all hand fractures and usually affect the young and active. Certain 5th metacarpal fracture patterns produce functional impairment, evident in declining 5th finger grip strength and 5th metacarpophalangeal (MCP) joint mobility.[2] Manual dexterity consequently diminishes, causing missed workdays and their economic implications.[3][4]
A boxer’s fracture is a fracture of the 5th metacarpal neck, named for the classic injury mechanism involving direct trauma to a clenched fist. This injury represents 10% of all hand fractures. The treatment varies based on whether the fracture is open or closed and its characteristics, including the degree of angulation, shortening, rotation, and presence of concomitant injuries. Immobilization with an ulnar gutter splint is the definitive treatment for closed, nondisplaced fractures without angulation or rotation. In contrast, open and significantly angulated or malrotated fractures or injuries with neurovascular involvement may require operative fixation.[5]
Metacarpal Anatomy
The metacarpus comprises the palm's skeleton, connecting the wrist bones (carpus) and phalanges. Each digit has a metacarpal bone, with the 1st metacarpal supporting the thumb and the 5th metacarpal assisting the little finger. Each metacarpal has a head, shaft, neck, and base. The heads articulate with the proximal phalanges distally, while the bases articulate with the carpus proximally. The neck is the narrowed portion of the metacarpal bone just distal to the base. This area is commonly involved in boxer's fractures.
The metacarpal bones form the palm's framework and provide attachment points for muscles responsible for hand movements and grip strength. Metacarpals 2 to 5 are closely attached. Consequently, isolated fractures are often stable. The palm's bones are also highly vascularized. Thus, metacarpal fractures heal rapidly except if crushed or severely displaced. Metacarpal injuries can significantly impair hand function, affecting daily living, work, and sports activities if not properly treated.
Etiology
The most common mechanism of injury for a boxer’s fracture is punching, ie, a strong axial pressure is applied to the metacarpal bone when the fist is clenched. A direct blow, projectile injury, or trauma to the hand dorsum may also fracture the 5th metacarpal neck. Unlike many other hand and wrist fractures, a boxer’s fracture typically does not occur with a fall onto an outstretched hand.[6] Metacarpal fractures may be attributed to several factors, including falls, sports-related injuries, direct trauma, and road traffic accidents.[7]
Epidemiology
The incidence of metacarpal neck fractures presenting for hospital care in the United States is 13.6 per 100,000 person-years. Metacarpal fractures account for 40% of all hand fractures, while fractures of the 5th metacarpal neck account for 10%. The incidence in males is 5 times higher than in females.[8] Males aged 10 to 19 have the highest incidence, followed by males aged 20 to 29. Fifth metacarpal injuries commonly occur at home and athletic events.[9]
Pathophysiology
Axial load via direct trauma to a clenched fist transfers energy to the metacarpal bone, causing fractures most commonly at the 5th metacarpal's neck. The injury typically results in apical-dorsal angulation due partly to the forces exerted by the interosseous muscles' pull.[10]
The interosseous muscles, responsible for finger adduction and abduction, originate from the metacarpal shafts and insert into the proximal phalanges. The collateral ligaments join the metacarpal bones to the proximal phalanges and must be considered during splinting to minimize ligament shortening and consequent mobility loss. The ligaments are taut in flexion and slack in extension. Therefore, the MCP joints should be splinted in flexion to prevent shortening (intrinsic plus positioning).[11]
The arteries and nerves supplying the fingers are adjacent to the metacarpal bones. Severely displaced boxer's fractures may injure the fingers' neurovascular supply, requiring surgical intervention.
History and Physical
Patients with metacarpal fractures present with complaints of dorsal hand pain, swelling, and deformity in the setting of one of the mechanisms that may give rise to this injury. Patients may also report bruising and difficulty moving the ulnar-side digits.
During physical examination, the affected hand must be entirely assessed and compared to the contralateral hand, with particular attention to the following:
- Skin: The skin must be closely inspected for any breaks, especially near the metacarpal head, typically the point of impact. Open fractures warrant immediate surgery. When a boxer's fracture occurs during a punch to the face, the recipient's tooth may cause a laceration or abrasion known as a "fight bite." Fight bites often require operative irrigation and debridement.
- Neurovascular exam: As with all suspected fractures, a neurovascular exam should test for sensation, motor function, and blood flow distal to the injury. Compartment syndrome rarely develops in the hand. However, the condition can lead to functional loss if unrecognized and treatment is delayed.[12]
- Angulation: Boxer's fractures are typically associated with apical dorsal angulation, resulting in MCP joint depression and loss of the normal knuckle contour. With significantly angulated fractures, "pseudoclawing" may be observed due to extensor apparatus damage. Pseudoclawing occurs when the MCP joints are hyperextended, and the proximal interphalangeal (PIP) joints are flexed. Plain films can help determine the degree of angulation.[13][14]
- Rotational alignment: Any degree of malrotation warrants referral to a hand surgeon. Rotational alignment evaluation is a crucial physical exam component. Alignment may be assessed by examining the hand with the MCP and PIP joints flexed and distal interphalangeal (DIP) joints extended. If lines are drawn along the digits and extended distally, normally aligned digits will show the convergence of these lines. Suspect malrotation if the line extending from the 5th finger does not converge toward the others.
- Malrotation: This condition can also be detected by examining the hand with the MCPs flexed and PIPs and DIPs extended. The fingernails should be in line along a single plane.[15]
Evaluation
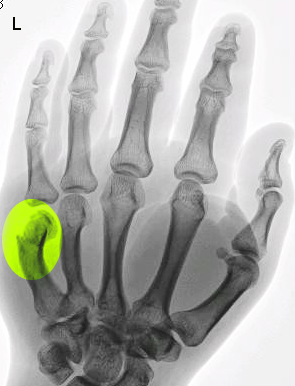
Plain radiographs are the preferred imaging modality when evaluating suspected metacarpal fractures (see Image. Boxer's Fracture). Anteroposterior, lateral, and oblique views should be obtained. The lateral view should be used to measure the degree of angulation between the metacarpal shaft and the fracture fragment's midpoint.[16] The metacarpal head and neck normally form an angle of 15°. Fracture angulation usually exceeds this value. The tangential radiographic projection helps identify occult radial head fractures. Brewerton's x-ray imaging technique is performed by placing the fingers flat on the x-ray plate, flexing the MCP joints at a 65° angle, and angulating the beam 15° toward the hand's ulnar side.[17]
Recent literature suggests that bedside ultrasound may also be used to diagnose a metacarpal fracture initially.[18] Computed tomography is generally not used for diagnosing metacarpal fractures. However, metacarpal head injuries and occult fractures in other bones may be detected by this modality in patients with negative plain radiographs but with clinical signs suspicious of a fracture.[19]
Treatment / Management
Fight bites pose an infection risk. Tiny wounds must be thoroughly irrigated and sterilized. Bigger wounds often warrant antibiotic treatment and surgical debridement.
Meanwhile, boxer's fracture treatment varies based on whether the fracture is open, angulated, rotated, and accompanied by other injuries. The options are discussed below.
Immobilization Alone
A closed boxer's fracture without angulation, malrotation, or displacement may be initially immobilized with splinting, often using an ulnar gutter splint. Alternatively, a premade Galveston splint or a custom orthosis may be used.[20]
The hand should be in the intrinsic plus position for splinting—with mild wrist extension, 70° to 90° of flexion at the MCP joint, and slight flexion at the DIP and PIP joints. Flexion of these joints helps prevent collateral ligament shortening and subsequent loss of mobility and function.[21]
Closed Reduction
Closed reduction is required for a boxer's fracture with angulation greater than 30°. Analgesia options during the procedure include a hematoma and ulnar nerve block. Young children or patients with anxiety may require sedation. However, this procedure typically is tolerated well, even without sedation.
Closed reduction of a boxer's fracture is accomplished using the "90-90 method." The MCP, DIP, and PIP joints should all be flexed to 90°. The clinician should then apply volar pressure over the dorsal aspect of the fracture site while applying pressure axially to the flexed PIP joint.[20] This axial pressure to the PIP applies dorsal force to the distal fracture fragment. The clinician should be able to feel the reduction when it has been achieved. The injury should be immobilized with an ulnar gutter splint. Postreduction films should be taken to assess reduction adequacy.[22] The 5th metacarpal neck can tolerate angulation up to 70°. Nonoperative management can continue if the fracture remains within acceptable tolerances. The 5th metacarpal shaft's acceptable angulation is 30°.[23]
Surgical Referral
Surgical referral is indicated for fractures that are open, severely comminuted, malrotated, or associated with neurovascular injury.[24] Surgical referral is also appropriate for cases of malunion, nonunion, and persistent angulation after conservative treatment. Surgical options include open reduction with internal fixation and closed reduction with percutaneous pinning.
Follow-Up
Repeat radiographs must be obtained within a week to assess alignment. Radiographs should be obtained every 2 weeks afterward until clinical and radiographic healing are present, typically between 4 to 6 weeks. Even with adequate reduction, cosmetic deformity may arise due to loss of the normal knuckle contour. After a short immobilization period, passive and active range-of-motion exercises should alleviate MCP and PIP joint stiffness. Literature supports early mobilization rather than prolonged immobilization of these injuries.[25][26] Persistent functional loss after several weeks of physical therapy warrants occupational therapy.
Differential Diagnosis
The differential diagnosis for 5th metacarpal fractures includes 5th metacarpal chondromas, soft tissue laceration, and sarcomas. A boxer's knuckle is an MCP joint sagittal band tear causing subluxation of the associated extensor tendon.[27] Clinical history and imaging findings can distinguish metacarpal fractures from these conditions.
Treatment Planning
Surgical Incision During Metacarpal Fixation
A direct longitudinal incision along the 5th metacarpal bone's dorsal-ulnar aspect is made during operative fixation. The incision can be extended obliquely in both proximal and distal directions. The incision's proximal third risks damaging the ulnar nerve's dorsal sensory branches and nearby longitudinal veins.
The extensor tendons are then retracted. The opponens and abductor digiti minimi muscles may be partly subperiosteally detached if required. The periosteum should be applied over the implant to reduce contact between the extensor tendons and the implant.
Surgical Indications in Metacarpal Fracture Treatment
Finger fractures have a low tolerance for rotational deformity. A single degree of metacarpal rotation causes a 5° rotation at the fingertip, resulting in a 1.5 cm overlap between the digits.[28]
All fingers typically align toward the scaphoid tubercle. Deviations signify the presence of a rotated fracture fragment.
Intraarticular fractures warrant specific attention. Operative fixation can realign the joint and reduce the risk of further arthrosis when a step-off greater than 1 mm or more than 25% articular surface involvement is present.
Operative fixation is indicated for all segmental, displaced, and irreducible fractures. Greater than 6 mm shortening and residual angulation of more than 40° in the 5th metacarpal shaft requires definitive fixation.
Surgical Fixation Devices
Metacarpal shaft fractures can be fixated using devices such as K-wires, intraosseous wires, lag screws, and plates. These devices are selected based on the specific fracture characteristics. The current consensus does not support using the metacarpal head as an insertion site for these fixation instruments due to possible complications arising from extensor tendon issues and MCP joint stiffness. Antegrade wires are often used in practice.[29]
A protected range of motion is advised when utilizing K-wires for surgical treatment due to their inherent lack of rigidity. Lag screws offer effective fixation in long oblique fractures and enable early motion. However, lag screws should only be used on oblique fractures and at least twice the width of the metacarpal.
Facca et al demonstrated no statistically significant grip strength, discomfort, and DASH rating differences between locking plates and K-wires when fixating 5th metacarpal fractures. However, avascular necrosis was a rare complication (0.05%) observed with plate fixation, primarily attributed to periosteal stripping.[30]
Regarding implant type, outcomes from miniplate (1.3 mm thick) and microplate (0.6 mm plates) fixation were reported to have no discernible distinction.[31] Another study comparing bioabsorbable and titanium plates for metacarpal fractures discovered no significant difference in clinical and radiological outcomes.[32]
Metacarpal Neck Fractures
Certain 5th metacarpal neck fracture patterns may result in functional impairment, manifesting as diminished 5th finger grip strength, pseudoclawing, and decreased 5th MCP joint mobility. Two randomized control trials demonstrated no statistically significant disparities in clinical or radiological outcomes between the surgical and nonsurgical subgroups of individuals with metacarpal neck fractures after 12 months.
Metacarpal Head Fractures
Most metacarpal head fractures exhibit articular involvement and often display comminution, making surgery treatment the preferred strategy for these injuries. If the fracture has tiny fragment sizes, small screws (2 mm) may be used in conjunction with the screw head countersinking method. Other options, such as replacement arthroplasty or arthrodesis, may be explored when the articular surface cannot be effectively repaired.
Prognosis
Literature has shown that closed management of 5th metacarpal neck fractures angulated by less than 70° but without rotational deformity confers high functional capabilities, as indicated by quickDASH scores at 4 months.[33] Most of these fractures typically heal uneventfully within 8 weeks. However, a complete resolution may take many months. Common symptoms of a 5th metacarpal fracture often include pain or discomfort, stiffness, reduced muscular strength, and a localized bump. Nevertheless, this injury is not expected to impact hand functionality adversely. Diabetes and cigarette smoking are factors that can delay bone healing.
Complications
Complications of 5th metacarpal neck fractures include digit malrotation, nonunion, joint stiffness, grip weakness, neurovascular injury, and loss of the 5th knuckle's aesthetic appearance.[33] Open fractures and fight bites predispose to infection. Incompletely healed fractures may cause chronic pain and refracture. These potential complications should be communicated with the patient when discussing operative and nonoperative treatments.
Postoperative and Rehabilitation Care
Physiotherapy to restore optimal hand functionality plays a crucial role in rehabilitation. The primary rehabilitation objectives include restoring complete muscular strength and attaining optimal range of motion. Appropriate splinting is crucial since inadequate splinting may lead to stiffness, pressure sores, or even compartment syndrome.[34] The recommended splinting technique for this kind of fracture entails positioning the wrist in 20° extension, flexing the MCP joint to 60° to 70°, and extending the interphalangeal joint.[35]
Postoperatively, starting active range-of-motion exercises without resistance around 2 to 3 weeks postinjury is generally recommended. Tendon gliding prevents scarring, enhances fracture site circulation, and reduces edema. Passive motion may be commenced upon adequate clinical and radiological healing. Most metacarpal fractures managed with immobilization are generally started on gentle resistance exercises about 4 weeks postinjury. Active motion should be limited when healing has not started.[36][37]
Deterrence and Patient Education
Boxer's fractures usually result from trauma to the 5th metacarpal. Primary preventive measures for these injuries include hand protection, proper hand motion techniques in sports, avoiding risky behaviors, and enhancing home safety. Secondary preventive measures are taken to avoid complications postinjury. Conservative treatment may be sufficient if patients have minimal pain and no rotational malalignment, even for angulated fractures. However, severe angulation, comminution, neurovascular injury, functional impairment, and severe pain warrant a referral to a hand surgeon. No rotational malalignment is acceptable because it causes significant functional impairment and finger overlapping while making a fist. Patients must be counseled about the importance of follow-up consults and adherence to rehabilitative measures posttreatment.
Pearls and Other Issues
Boxer's fractures are common injuries of the 5th metacarpal neck, typically caused by direct trauma such as punching a hard object with a closed fist. Patients often present with pain, swelling, bruising, difficulty making a fist or moving the little finger, and hand deformity. The diagnosis of this condition is typically made based on clinical examination and confirmed with x-rays, which help determine fracture location, angulation, and severity, guiding treatment decisions.
Nondisplaced or minimally displaced fractures may be managed conservatively with immobilization using splints or casts, followed by hand therapy. Severe fractures warrant surgery. Complications arising from boxer's fractures include malunion, nonunion, joint stiffness, grip weakness, chronic pain, and infection. Following treatment, rehabilitation helps restore hand function and prevent stiffness. Physical therapy exercises may be prescribed to improve the affected hand and fingers' range of motion, strength, and coordination.
Preventive strategies include proper hand protection techniques, avoiding risky behaviors that increase the likelihood of hand injuries, and using appropriate protective gear during sports or activities with a high risk of hand trauma. Overall, prompt diagnosis, appropriate treatment, and diligent rehabilitation are essential for optimizing outcomes and minimizing complications in patients with 5th metacarpal fractures.
Enhancing Healthcare Team Outcomes
Fifth metacarpal fractures are best managed with an interprofessional approach. Primary care and emergency medicine practitioners are often the first to encounter patients with this condition and, thus, the first to evaluate and treat the injury. Radiologists can lend their expertise in interpreting imaging results to help guide further management. Referrals must be made to orthopedic or hand surgeons for definitive treatment. Anesthesia specialists can ensure patient comfort during surgical procedures if warranted.
The nursing staff coordinates care, administers treatments, reinforces patient education, and monitors patients. Pharmacists help manage medications and educate patients about proper medication intake and toxicity prevention. Physical and occupational therapists help patients recover hand function after definitive treatment. Fifth metacarpal fractures typically heal without any functional detriment.