Introduction
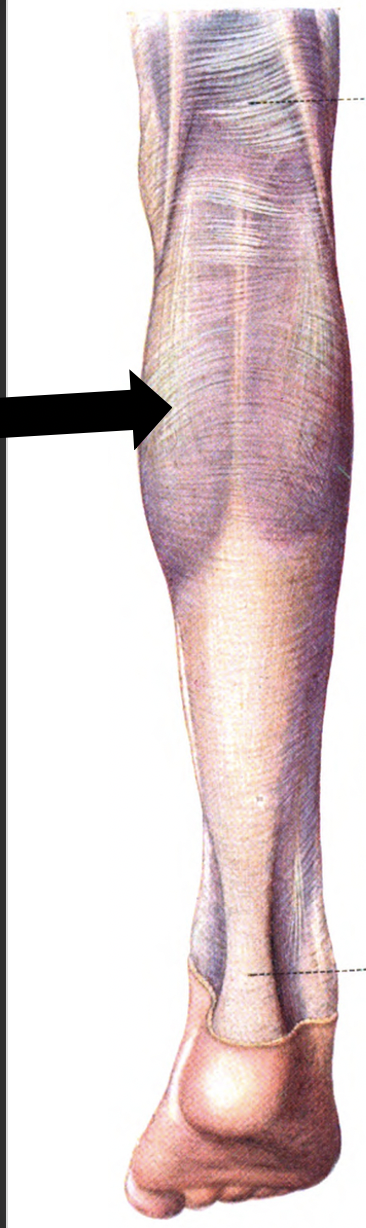
The calf (Latin: sura) refers to the posterior portion of the lower leg. The two largest muscles in this region include the gastrocnemius and the soleus. The gastrocnemius is the most superficial of the muscles and has two heads, medial and lateral. The two heads of the gastrocnemius converge and form a confluent muscle belly. The lateral head originates from the lateral surface of the lateral femoral condyle and the medial head from the posterior, non-articular aspect of the medial femoral condyle. The muscle belly of the gastrocnemius joins the soleus muscle distally to form the calcaneal tendon (i.e. the achilles tendon), which inserts onto the posterior calcaneus.[1][2][3][4][5]
The calf muscle plantarflexes the ankle joint and is innervated by the tibial nerve. The soleus is a large, flat muscle located deep to the gastrocnemius. The plantaris is a relatively small muscle with an appreciably long tendonous portion. The tendinous portion can easily be mistaken for a nerve. The plantaris muscle arises from the lateral supracondylar line of the femur and is completely absent in up to 10% of the population. The muscle descends medially, eventually forming into a tendon that runs down the leg, between the gastrocnemius and soleus. This tendon blends with the calcaneal tendon.
Structure and Function
The calf muscles are responsible for plantarflexion the foot and ankle. The calf muscles are engaged in activities such as running and jumping.
Embryology
In most cases, the upper limbs develop before the lower limbs. The development of the lower limbs starts at week 4 of gestation, and the limb is well differentiated by weeks 8 to 10. The limb buds start to develop after activation of the mesenchymal cells in the lateral plate mesoderm.
Blood Supply and Lymphatics
The blood supply of the calf muscles is derived from the popliteal artery, which divides into the anterior and posterior tibial arteries. The fibular (or peroneal) artery originates from the posterior tibial artery. The posterior tibial artery accompanies the tibial nerve and enters the plantar aspect of the foot through the tarsal tunnel. The anterior tibial artery runs anteriorly between the tibia and fibula through a gap in the interosseous membrane. It extends down the entire length of the leg and into the foot becoming the dorsalis pedis artery.
The venous supply of the calf can be divided into the superficial and deep veins. The superficial veins consist of the greater saphenous vein and the small saphenous vein. The deep veins include the popliteal vein, the anterior tibial vein, the posterior tibial vein, and the fibular vein. The greater saphenous vein is the longest vein in the body and runs the entire length of the lower extremity. Cardiothoracic surgeons commonly use this vein during coronary artery bypass grafting. The small saphenous vein is actually a relatively large vein that runs along the posterior aspect of the calf and passes between the heads of the gastrocnemius muscle and usually drains into the popliteal vein. The popliteal vein is formed when the anterior and posterior tibial veins merge. The popliteal vein becomes the femoral vein as it extends into the femoral region. The anterior tibial veins drain the knee joint, ankle joint, tibiofibular joint, and part of the anterior leg. The posterior tibial vein gets blood from the lateral and medial plantar veins and drains the posterior muscles of the lower leg and the plantar surface of the foot. The fibular veins, also known as the peroneal veins, transport blood from the lateral compartment of the leg and drain into the posterior tibial vein.
Nerves
The tibial nerve (S1, S2) innervates the majority of the muscles of the calf. The tibial nerve passes through the popliteal fossa and gives off branches to the gastrocnemius, popliteus, soleus, and plantaris muscles. There is also a cutaneous branch that will become the sural nerve.
Muscles
The lower leg consists of four compartments: anterior, lateral, superficial posterior, and deep posterior.
- The anterior compartment includes the tibialis anterior, extensor hallucis longus, extensor digitorum longus, peroneus tertius, tibialis anterior and the deep peroneal nerve
- The lateral compartment contains the peroneus longus and brevis and also the superficial peroneal nerve
- The deep posterior compartment consists of the tibialis posterior, flexor hallucis longus, flexor digitorum longus, popliteus, and the tibialis nerve
- The popliteus muscle solely acts at the knee by internally rotating the tibia relative to the femur, thus its function is to "unlock" the knee joint during the initiation of flexion
- The popliteus is located behind the knee joint and forms the base of the popliteal fossa
- The tibialis posterior is the deepest of the four muscles and originates from the interosseous membrane between the tibia and fibula. It inverts and plantar flexes the foot and maintains the medial arch of the foot. The flexor digitorium longus (FDL) is located medially in the posterior leg and is responsible for flexing the lateral four toes. The flexor hallucis longus is located on the lateral side of the leg and flexes the great toe
- The superficial posterior compartment has the gastrocnemius, soleus, plantaris, and the sural nerve
- The tibial nerve innervates all of the superficial and deep muscles of the calf.
Surgical Considerations
Peripheral arterial disease of the lower extremity is a result of atherosclerotic plaques. As the atherosclerotic plaques increase in size, it results in claudication or pain with ambulation. Treatment options include angioplasty, stenting, or lower extremity bypass grafting.
Clinical Significance
When the leg veins clot, thrombosis can result with a potential for pulmonary embolus. If the lower leg arteries are stenosed or occluded, a cold ischemic leg can occur which requires immediate intervention to salvage the leg. If nerve injuries occur, the patient may be left with various types of neurological deficits. Compartment syndrome is a surgical emergency and requires prompt fasciotomy. Compartment syndrome results when the increased pressure within the compartment causes the tissues to be hypoperfused. Since the fascia that surrounds the compartment does not stretch, any swelling of the muscles or bleeding within the compartment can cause an increase in the pressure within the compartment.[6][7][8][1]