Continuing Education Activity
Dermatosis papulosa nigra (DPN) is a benign epidermal growth that presents as hyperpigmented or skin-colored papules that develop on the face and neck beginning in adolescence. It typically occurs in individuals with Fitzpatrick skin types III to VI, most commonly affecting people of African and Asian descent. It is considered to be a common variant of seborrheic keratoses (SKs). It was first described in 1925 by Dr. Aldo Castellani based on his observations while visiting Jamaica and Central America. This activity reviews the evaluation and management of dermatosis papulosa nigra and the role of interprofessional team members in collaborating to provide well-coordinated care and enhance patient outcomes.
Objectives:
- Review the presentation of dermatosis papulosa nigra.
- Describe the epidemiology of dermatosis papulosa nigra.
- Summarize the treatment of dermatosis papulosa nigra.
- Review the evaluation and management of dermatosis papulosa nigra and the role of interprofessional team members in collaborating to provide well-coordinated care and enhance patient outcomes.
Introduction
Dermatosis papulosa nigra (DPN) is a benign epidermal growth that presents as hyperpigmented or skin-colored papules that develop on the face and neck beginning in adolescence. It typically occurs in individuals with Fitzpatrick skin types III to VI, most commonly affecting people of African and Asian descent. It is considered to be a common variant of seborrheic keratoses (SKs). It was first described in 1925 by Dr. Aldo Castellani based on his observations while visiting Jamaica and Central America.
Etiology
The cause of DPN is unknown. Similar to SKs, a somatic activating mutation in FGFR3 has been found in lesions of DPN, supporting the concept that these two lesions share common genetic pathogenesis and may explain the genetic predisposition observed in DPN.[1] Because the lesions occur mainly in a photodistribution on the head, neck, and upper trunk, a potential association with cumulative ultraviolet (UV) exposure has been proposed. FGFR3 mutations have been found to occur more in sun-exposed regions and with increasing age. One study showed that darker-skinned patients who used topical treatments for artificial depigmentation had an exacerbation of DPNs, possibly due to decreased UV protection from loss of skin pigment.[2] These features suggest that UV exposure may have a role in the pathogenesis of DPN.
Epidemiology
DPN is common in those of African descent and relatively common in Asians, with reported incidences ranging from 10% to 75% in selected study populations of individuals with darker pigmentation.[3] The condition has been reported in populations of African heritage, Filipinos, Vietnamese, Europeans, and Mexicans.[4] Up to one-third of African American adults in the United States have DPN. Studies have reported that more lightly pigmented African-Americans had a lower frequency of involvement when compared to those with Fitzpatrick skin type VI.[2] DPN occurs with a strong familial predisposition. Various studies of patients with DPN reported positive family histories in 77% to 93% of cases.[5] Women are twice as likely to be affected as men. The onset of DPN is typical during adolescence, in contrast to SKs. Rarely, it occurs in children and has been reported in patients as young as age 3. The number and size of lesions increase with age, peaking in the sixth decade. DPN is not related to any systemic disease or syndrome; however, an eruptive form has been reported in association with adenocarcinoma of the colon.[6]
Histopathology
DPN is characterized by irregular acanthosis, papillomatosis, and hyperkeratosis of the epidermis. There are elongated and interconnected rete ridges, with deposits of unusually large amounts of pigment throughout the rete, particularly in the basal layer.[5] Keratin-filled invaginations of the epidermis are often present. A prominent fibrous stroma is typically seen within papillomatous acanthotic structures. The pattern is similar to the acanthotic and reticulate types of SKs, although horn pseudocysts are not commonly seen, and the epithelial proliferation is not usually composed of basaloid cells in DPN lesions.[3]
History and Physical
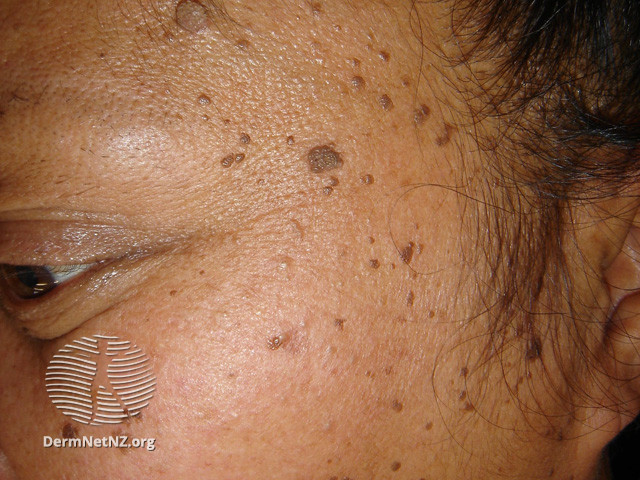
The lesions of DPN initially present in adolescent patients as minute, round, skin-colored to dark brown macules, resembling freckles, gradually becoming papular and increasing in size and number with age. There may be a family history of similar lesions. The lesions often become hyperpigmented, filiform to sessile, smooth-surfaced papules, ranging from 1- to 5-mm in diameter and 1- to 3-mm in elevation. They most commonly appear in a symmetric distribution on the malar cheeks, temples, and forehead. They may also occur on the neck, upper chest, and back with less frequency. Approximately one-fourth of patients with facial lesions will also have lesions on the body. The papules are asymptomatic, without scaling, crusting, or ulceration. Lesions do not spontaneously resolve.
Evaluation
DPN can usually be diagnosed clinically. Dermoscopy may be a useful, noninvasive, cost-effective diagnostic tool in distinguishing DPN from other pigmented lesions. One study in 2017 reported the most common dermoscopy finding was fissures and ridges in a cerebriform pattern, seen in 59% of cases. Another common finding is comedo-like openings, seen in 27% of cases in the study. Milia-like cysts and a combination of the above findings may also be seen.[5]
If there is any concern for malignancy, the lesion should be biopsied and sent for histopathology.
Treatment / Management
Treatment of DPN is not necessary and is generally performed for cosmetic purposes. Due to the tendency of darker skin types to heal with dyspigmentation, caution should be used when choosing treatment modalities, and all patients should be counseled that removal of DPN lesions may result in dyspigmentation. Initial treatment should be limited to a small number of lesions to allow for the evaluation of post-inflammatory dyspigmentation. Aggressive treatment should be avoided to minimize scarring and pigmentation problems.
The most common treatment modalities include snip excision with scissors, light curettage with or without anesthesia, and light electrodesiccation, which are generally effective for smaller lesions.[7] Electrodesiccation should be done at a low setting after applying a topical anesthetic, and the patient should be instructed to apply ointment to the desiccated crust daily until healed.[8] Cryotherapy is problematic due to the risk of hypopigmentation secondary to melanocyte damage and should be used with extreme caution. Studies and case reports have described successful treatment of DPN lesions with KTP, PDL, Nd:YAG, and CO2 lasers, with minimal adverse events and efficacy comparable to electrodesiccation.[9][10][11] Repeated laser treatments may be necessary. A 2016 study of 45 patients treated with CO2 laser reported high patient satisfaction with cosmetic outcomes after an average of 3 treatment sessions, although 28% reported a recurrence of a few lesions after CO2 ablation.[12] Patients should be counseled that lesions may recur after treatment with any modality.
Differential Diagnosis
The differential diagnosis of DPN includes seborrheic keratoses, acrochordons, verrucae, melanocytic nevi, angiofibromas, and various adnexal tumors, including trichoepitheliomas, fibrofolliculomas, tricholemmomas, basaloid follicular hamartomas, syringomas.
Prognosis
DPN is a benign and asymptomatic cutaneous condition without the risk of malignancy. DPN lesions may increase in number and size with age and do not spontaneously resolve.
Complications
Similarly to seborrheic keratoses, DPN lesions can become inflamed and irritated. Removal of lesions can lead to cosmetic complications, including infection, scarring, and dyspigmentation.
Consultations
For primary care providers, consultation with a dermatologist may be indicated if there is uncertainty regarding the diagnosis or any concern for cutaneous malignancy.
Pearls and Other Issues
DPN is presumed to be a variant of seborrheic keratoses (SKs); however, some clinicians believe it to be a clinically and histopathologically distinct entity. There are key differences between DPN and SKs that lead to this debate. The two lesions affect different demographics, with DPN affecting darker skin types with a female predominance. SKs are found in all skin types with a predominance in lighter-pigmented individuals with Fitzpatrick skin type I to II.[13] Clinically, DPN lesions are largely limited to sun-exposed areas, whereas SKs have a more widespread distribution. Morphologically, DPN lesions are relatively small and uniform, while SKs vary widely in size and shape, with diameters that can reach several centimeters. Genetically, DPN and SKs share a common somatic activating mutation in FGFR3; however, DPN lacks the mutation in PIK3CA that is found in SKs, suggesting different genetic causes.[14] Subtle but consistent differences between the histology of DPN and SKs have been reported, including the prominence of fibrous stroma within papillomatous acanthotic structures, seen in DPN but not SKs. Further studies on the pathogenesis of DPN may yield insight into whether it is truly a variant of SKs or its own distinct entity.
Enhancing Healthcare Team Outcomes
Dermatosis papulosa nigra (DPN) is a benign epidermal growth that presents as hyperpigmented or skin-colored papules that develop on the face and neck beginning in adolescence. Most healthcare workers including nurse practitioners are probably unfamiliar with this skin disorder, hence referral to a dermatologist is recommended. The key reason patients seek care is for cosmesis.