Continuing Education Activity
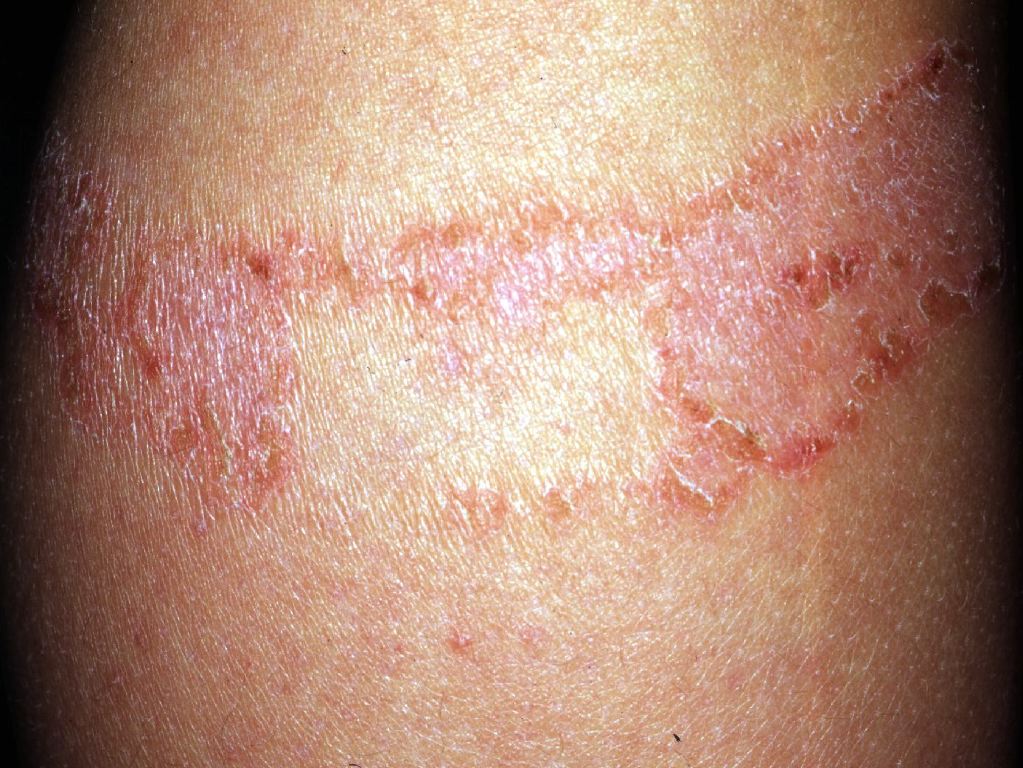
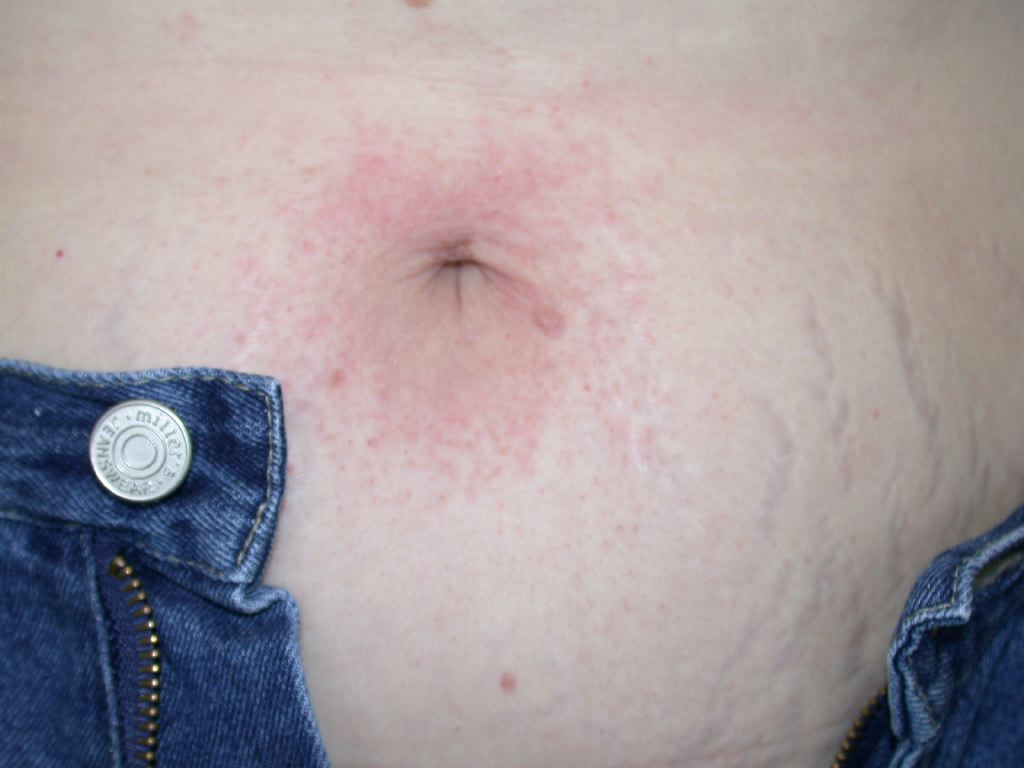
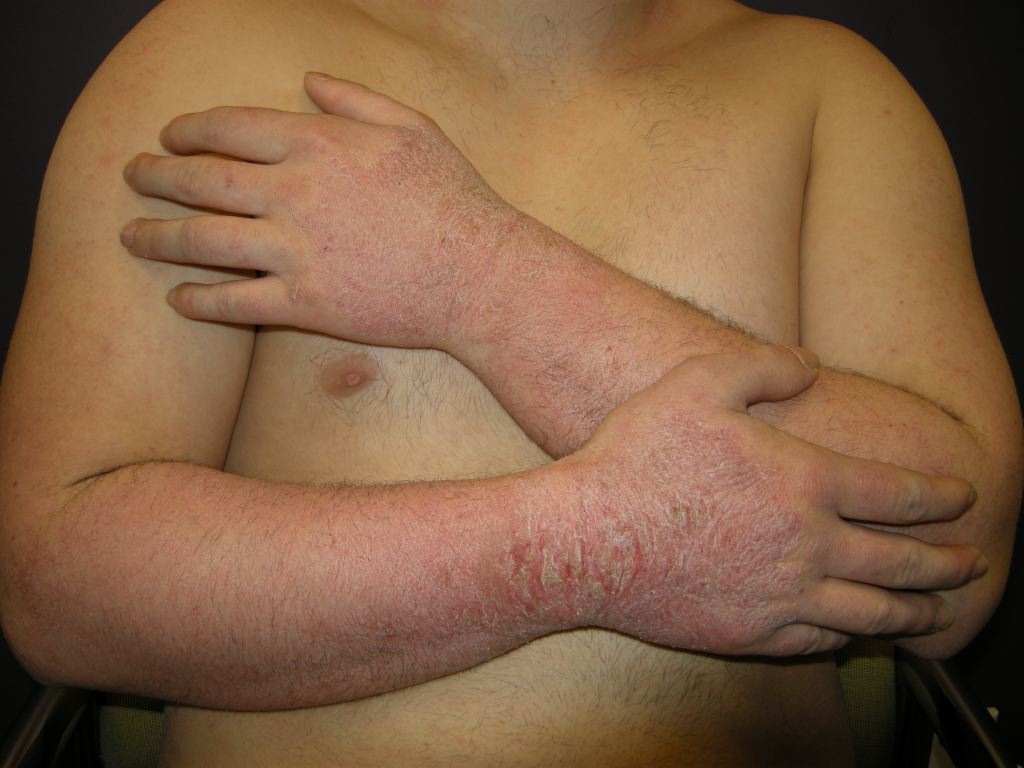
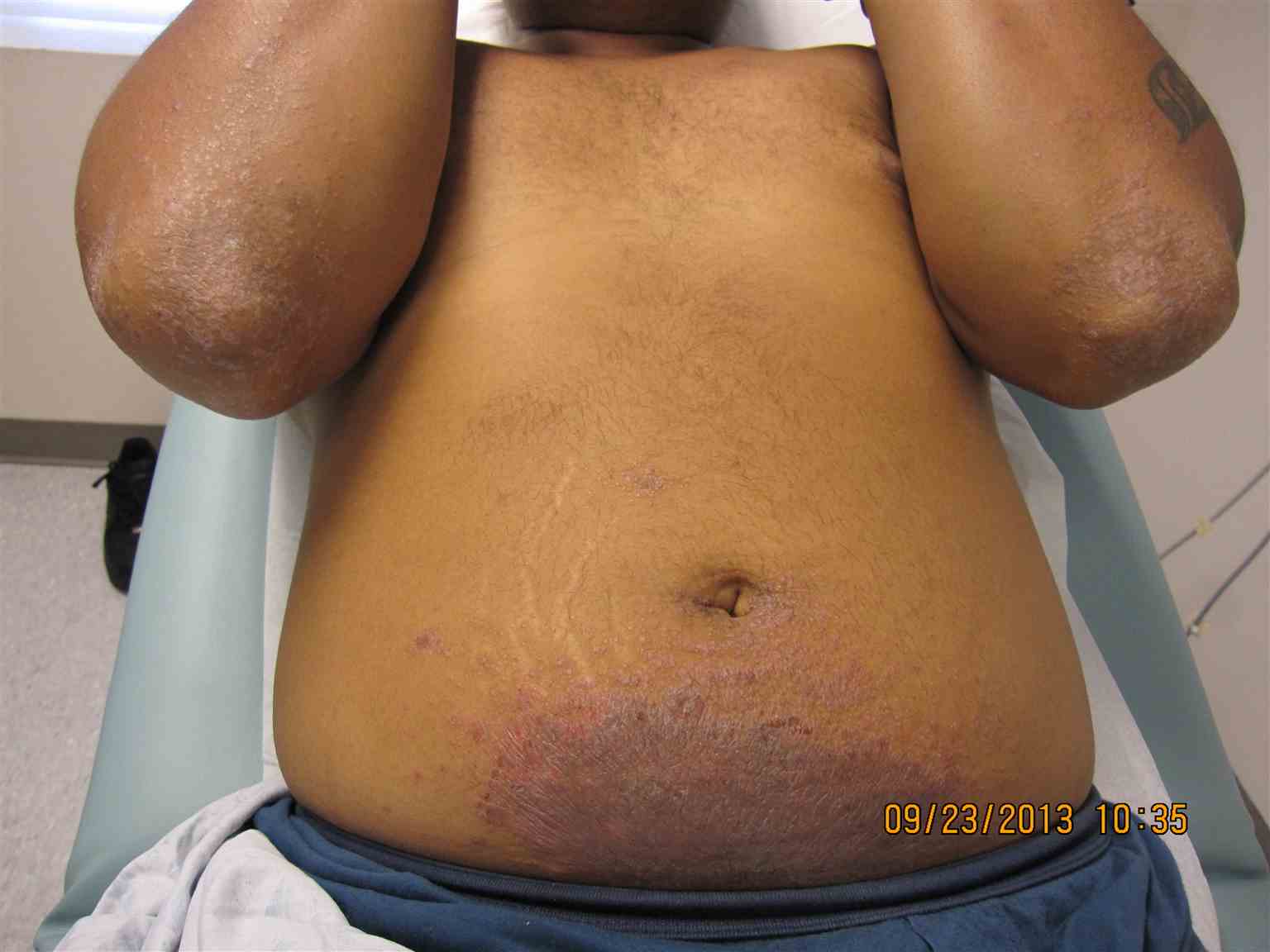
Contact dermatitis is an inflammatory eczematous skin disease. It is caused by chemicals or metal ions that exert toxic effects without inducing a T-cell response (contact irritants) or by small reactive chemicals that modify proteins and induce innate and adaptive immune responses (contact allergens). Contact dermatitis is divided into irritant contact dermatitis and allergic contact dermatitis. Irritant contact dermatitis is a nonspecific response of the skin to direct chemical damage that releases mediators of inflammation predominantly from epidermal cells while allergic contact dermatitis is a delayed (type 4) hypersensitivity reaction to exogenous contact antigens. Immunological responses are due to the interaction of cytokines and T cells. In photo contact, allergic dermatitis lesions are confined to sun-exposed areas even though the allergen is in contact with covered areas. This activity reviews the causes, pathophysiology, and diagnosis of contact dermatitis and highlights the role of the interprofessional team in its management.
Objectives:
- Describe the causes of contact dermatitis.
- Review the workup of a patient with contact dermatitis.
- Summarize the treatment options for contact dermatitis.
- Outline the importance of improving care coordination among interprofessional team members to improve outcomes for patients affected by contact dermatitis.
Introduction
Contact dermatitis is an inflammatory eczematous skin disease. It is caused by chemicals or metal ions that exert toxic effects without inducing a T-cell response (contact irritants) or by small reactive chemicals that modify proteins and induce innate and adaptive immune responses (contact allergens).[1][2][3][4]
Contact dermatitis is divided into irritant contact dermatitis and allergic contact dermatitis. Irritant contact dermatitis is a nonspecific response of the skin to direct chemical damage that releases mediators of inflammation predominantly from epidermal cells while allergic contact dermatitis is a delayed (type 4) hypersensitivity reaction to exogenous contact antigens. Immunological responses are due to the interaction of cytokines and T cells. In photo contact, allergic dermatitis lesions are confined to sun-exposed areas even though the allergen is in contact with covered areas.
Until recently it was believed that allergic contact dermatitis was rare, unfortunately, data indicate that it is very common and affects close to 20% of children.
The good news is that the majority of cases of contact dermatitis are self-limited and managed with simple supportive measures. However, in some patients, the disorder is chronic and can significantly affect the quality of life.
Etiology
Irritant contact dermatitis
The likelihood of developing irritant contact dermatitis (irritant contact dermatitis ) increases with the duration, intensity, and concentration of the substance. Chemical or physical agents and microtrauma may produce skin irritation thus causing Irritant contact dermatitis. Physical irritants like friction, abrasions, occlusion, and detergents like sodium lauryl sulfate produce more irritant contact dermatitis in combination than alone.[5][6]
The factors which determine the severity of irritant contact dermatitis include the quantity and concentration of the irritant, duration, and frequency of exposure. It also depends on the type of skin if it is thick, thin, oily, dry, very fair, previously damaged skin, or having a pre-existing atopic tendency. Environmental factors like high or low temperature and humidity also determine the severity.
Allergic contact dermatitis
Common etiological allergens for allergic contact dermatitis are nickel, balsam of Peru, chromium, neomycin, formaldehyde, thiomersal, fragrance mix, cobalt, and parthenium.[7] Poison Ivy (Toxicodendron, formerly known as Rhus), in the United States, is considered to be the most common cause of allergic contact dermatitis.[8] As much as 50-70% of the adult population is sensitive to poison ivy or poison oak.[8] Once exposed to the skin, urushiol (the allergin responsible for the skin reaction), should be diligently removed by washing the affected area as soon as possible. Studies have shown that washing with regular soap, e.g. Dial, is sufficient and should be done within a 2-hour window.[8] If the patient has not removed the urushiol oil from their skin within the appropriate time frame, high-potency topical steroids may be used to reduce inflammation in early stages, i.e. within 12 hours of exposure.[9] It should be noted that low-potency topical steroids are of little use and even high-potency steroids do not significantly relieve symptoms once vesicles have formed.[9]
Epidemiology
Females, infants, elderly, and individuals with atopic tendencies are more susceptible to irritant contact dermatitis. It is reported that up to 80% of cases of occupational dermatitis are irritant contact dermatitis.[10]
All individuals are at risk of developing allergic contact dermatitis. Risk factors for allergic contact dermatitis include age, occupation, and history of atopic dermatitis.
Overall contact dermatitis is most common in people with red hair and fair skin. Women are more likely to develop contact dermatitis because of the use of jewelry and fragrances.
Pathophysiology
Irritant contact dermatitis
It is due to sufficient inflammation arising from the release of proinflammatory cytokines from keratinocytes, usually in response to chemical stimuli. It mainly causes skin barrier disruption, epidermal cellular changes, and cytokine release.
Irritants can be classified as cumulatively toxic (e.g., hand soap causing irritant dermatitis in a hospital employee), subtoxic, degenerative, or toxic (e.g., hydrofluoric acid exposure at a chemical plant).
Allergic contact dermatitis
It is T-cell mediated inflammation of the skin caused by repeated skin exposure to haptens in a sensitized individual.
Allergic contact dermatitis has two phases. The sensitization phase in which antigen-specific effector T cells are induced in the draining lymph nodes by antigen captured cutaneous dendritic cells that migrate from the skin. The elicitation phase includes effector T cells that are activated in the skin by antigen captured cutaneous dendritic cells and produce various chemical mediators, which create antigen-specific inflammation.
Photo contact dermatitis occurs when an allergen becomes an irritant in the presence of light.
Contact urticaria usually presents with a 'wheal and flare' reaction after exposure to the offending topical agent. While most cases are mild, anaphylactic reactions can occur. Some common types of contact urticaria include exposure to cold, dermatographism, pressure, exercise, solar, heat and cholinergic.
Contact dermatitis can also occur after exposure to plants of the Urticaceae family.
Histopathology
Contact irritant dermatitis presents with mild spongiosis, epidermal cell necrosis, and neutrophilic infiltration of the epidermis, while in allergic contact dermatitis dermal inflammatory infiltrates predominately contains lymphocytes and other mononuclear cells.
History and Physical
Symptoms of irritant contact dermatitis may include burning, itching, stinging, soreness, and pain, particularly at the beginning of the clinical course, while pruritus is more common in allergic contact dermatitis. Patients with a history are at increased risk for developing nonspecific hand dermatitis and irritant contact dermatitis.
Both irritant contact dermatitis and allergic contact dermatitis can present with three morphological patterns.
- Acute phase: erythema, edema, oozing, crusting, tenderness, vesicles or pustules
- Subacute phase: crusts, scales, and hyperpigmentation
- Chronic phase: Lichenification.
Hands are the common site of contact allergic dermatitis.
No pathognomonic clinical signs and symptoms can differentiate between allergic contact dermatitis and irritant contact dermatitis.
The acute irritant reaction usually reaches its peak quickly, within minutes to few hours after exposure, and then starts to heal, while in allergic contact dermatitis, the elicitation time depends on the characteristics of the sensitizer, the intensity of exposure, and degree of sensitivity. Lesions usually appear 24 to 72 hours after the exposure to the causative agent and reach their peak at approximately 72 to 96 hours. Allergic contact dermatitis improves more slowly than irritant contact dermatitis and then recurs faster (in a few days) when exposure is re-established.
Common allergens causing allergic contact dermatitis include the following -
- Paraphenylenediamine (PPD) present in hair dye; a common cause of allergic contact dermatitis on the scalp, face, ears
- Neomycin and bacitracin applied to the areas of stasis dermatitis and leg ulcers may be the cause of allergic contact dermatitis on the legs and feet
- Topical neomycin and corticosteroids can lead to allergic contact dermatitis in patients with otitis externa
- In women with lichen sclerosus et atrophicus, benzocaine applied in pruritus ani and pruritus vulvae may develop allergic contact dermatitis
- Nickel is the most common metal present in artificial jewelry which is the cause of allergic contact dermatitis.
Different clinical patterns of allergic contact dermatitis include erythema multiforme, urticarial papular plaques, lichen-planus, lichenoid eruptions, purpuric petechial reactions, dermal reactions, lymphomatoid contact dermatitis, granulomatous and pustular reactions, pigmentation disturbances, or pemphigoid.
Evaluation
History regarding occupation, hobbies and any topical or oral medications is important in diagnosing contact dermatitis. Patch testing is considered to be the gold standard in diagnosing contact allergic dermatitis and is used to determine the exact cause. A patch test mainly relies on the principle of a. The chemicals included in the patch test kit are chemicals present in metals (e.g., nickel), rubber, leather, formaldehyde, lanolin, fragrance, toiletries, hair dyes, medicine, pharmaceutical items, food, drink, preservative, and other additives. Patch testing helps identify which substances may be causing a delayed-type allergic reaction. It produces a local allergic reaction on a small area of the patient's back, where the diluted chemicals are applied.[11][12]
Allergens are placed on Finn chambers and applied on the back. Patches are removed at 48 hours, and final results are read 48-72 hours later. Grading of the reactions is completed based on the International Contact Dermatitis Research Group guidelines.
- Negative (-)
- Irritant reaction (IR)
- Equivocal / uncertain (+/-)
- Weak positive (+)
- Strong positive (++)
- Extreme reaction (+++)
In patients with nickel allergy, a few drops of dimethylgloxime and hydroxide solutions are on a cotton tip applicator and rubbed on the metallic surface of the jewelry. If the color pink appears on the applicator, this is a positive test for nickel. Women with nickel allergy can perform the test at home on jewelry for the presence of nickel.
Treatment / Management
Compliance with avoidance is important. The key to avoidance is proper evaluation and detection of causative allergen. Wear appropriate clothing to protect against irritants at home and in a work environment.[13][14]
High-potency topical corticosteroids, e.g. clobetasol propionate 0.05% cream, may be used to reduce the inflammation.[9] As a general rule, high-potency corticosteroids should not be used on thin skin, e.g. face, genitals, intertriginous areas, to avoid the risk of skin atrophy. Antihistamines such as hydroxyzine and cetirizine are recommended to control pruritus. Systemic steroids are advised in severe cases but should be tapered gradually to prevent recurrences. Friction should be avoided as well as the use of soaps, perfumes, and dyes. Emollients are used for hydrating the skin. Tacrolimus ointment and pimecrolimus cream are immunomodulating drugs that inhibit calcineurin and are helpful in allergic contact dermatitis.
Differential Diagnosis
- Contact Urticaria syndrome
- Drug-induced bullous disorders
- Drug-induced photosensitivity
- Irritant contact dermatitis
- Transient acantholytic dermatosis
Prognosis
The prognosis of patients with contact dermatitis depends on the cause and lifestyle. Isolated cases usually resolve if the offending agent exposure is discontinued. Those who do not remain compliant and continue to wear jewelry with metal or are exposed to plants because of lifestyle generally tend to have a chronic course. Relapses are very common. In healthcare, latex allergy is a very common form of contact dermatitis and can have an impact on clinical practice. Cases of anaphylaxis are reported all the time.
Enhancing Healthcare Team Outcomes
Contact dermatitis is a relatively common disorder encountered in clinical practice. However, the condition is best managed by an intradisciplinary team that includes a dermatologist, allergist, primary care provider, nurse practitioner, and a pharmacist. The key is compliance with avoidance is important. The key to avoidance is proper evaluation and detection of causative allergen. Wear appropriate clothing to protect against irritants at home and in a work environment.
The pharmacist should educate the patient on over the counter products that can be used to ease symptoms. Topical corticosteroids may be used to reduce the inflammation. Antihistamines such as hydroxyzine and cetirizine are recommended to control pruritus. Systemic steroids are advised in severe cases but should be tapered gradually to prevent recurrences. Friction should be avoided as well as the use of soaps, perfumes, and dyes. Emollients are used for hydrating the skin. Tacrolimus ointment and pimecrolimus cream are immunomodulating drugs that inhibit calcineurin and are helpful in allergic contact dermatitis.
The nurse and primary care physician should educate the patient on avoidance of the offending agents and maintain some type of barrier protection. Patients should be educated that contact dermatitis can recur if repeated exposure occurs. When going hiking, long-sleeved garments are recommended for individuals with an allergy to plants.
Unfortunately, recurrence is common and people with no identifiable cause have a poor quality of life.[15] A nurse educator specializing in dermatology and dermatology should work together to assist in patient education, particularly for challenging cases. [Level V]