Continuing Education Activity
A corn, also known as a "calvus," heloma," or "focal intractable plantar hyperkeratosis," is a type of callosity. Corns are uncomfortable, thickened skin lesions that result from repeated mechanical trauma due to friction or pressure forces. In the literature, confusing terminology is often used to call different types of hyperkeratotic skin lesions. Nevertheless, a corn should be distinguished from a callus, which is a more diffuse type of callosity. Thus, a corn is a well-delimited focal area of hyperkeratosis. This condition is often seen in athletes and patients exposed to unequal friction force from footwear or gait problems, including the elderly, patients with diabetes, and amputees. It should be regarded as a symptom rather than an effective disease. This activity reviews the etiology, presentation, evaluation, and management of corns and examines the role of the interprofessional team in evaluating, diagnosing, and managing the condition.
Objectives:
Review the etiology and pathophysiology of corn formation.
Describe appropriate physical exam techniques to diagnose a corn, and differentiate between the two types.
Review management techniques for helping patients who present with corns.
Describe the importance of improving coordination among the interprofessional team to enhance care for patients affected by corns.
Introduction
A corn, also known as a "clavus," "heloma," or "focal intractable plantar hyperkeratosis," is a type of callosity. Corns are uncomfortable, thickened skin lesions that result from repeated mechanical trauma due to friction or pressure forces. In the literature, confusing terminology is often used to call different types of hyperkeratotic skin lesions. Nevertheless, clinicians need to distinguish a corn from a callus, which is a more diffuse type of callosity. Thus, a corn is a well-delimited focal area of hyperkeratosis. This condition is often seen in athletes and in patients exposed to unequal friction force from footwear or gait problems, including older adults, patients with diabetes, and amputees. It should be regarded as a symptom rather than an effective disease.[1][2][3]
Etiology
Corns typically result from repeated accumulated mechanical trauma as well as other contributing factors like ill-fitting footwear, the presence of bony prominences (foot deformity), and certain physical activities.[4] They are most common on the feet: on the dorsum of the toes, in the last interdigital web space, as well as on the soles of the feet.
Epidemiology
The incidence of corns on the feet has been reported to be ranging anywhere from 14% to 48%.[5] Individuals with darkly pigmented skin are more prone to developing corns. They have been reported to affect older age groups with a slight female predominance due to wearing narrow shoes. The elderly are also subject to loss of the protective fat pad cushioning, called fat pad atrophy, which can increase the incidence of painful corn.[6]
Pathophysiology
The repeated friction and pressure of the skin overlying the bony prominences leads to a hyperkeratotic thickness resulting in corn formation. This corn is a protective body reaction that produces an excess of the horny epithelial layer to prevent skin ulceration. This explains the preferential location of corns next to the condyles of the metatarsals and phalanges and the occurrence of corns in patients with a foot deformity.
Histopathology
Histopathologic examination of a corn is usually not necessary, but on a few occasions, it might be helpful to differentiate corns and calluses from other diseases like a plantar wart. A biopsy specimen from corn will show proliferation of all epidermal layers (acanthosis), including the stratum corneum; the cells at the stratum corneum layers will return their nuclei (parakeratosis), indicating premature differentiation. The granular cell layer may be diminished or absent. The dermis may often show dense fibrous tissue with hypertrophied nerves, and scar tissue may extend to the subcutaneous fat.[7]
History and Physical
Corns are primarily diagnosed on clinical presentation. It is helpful to look at other lesions on an individual's skin to see their body's response to physical trauma. It is also easier to diagnose corns by inspection and palpation because of their rough hyperkeratotic texture. History should also include an account of physical activities.[6][8][9]
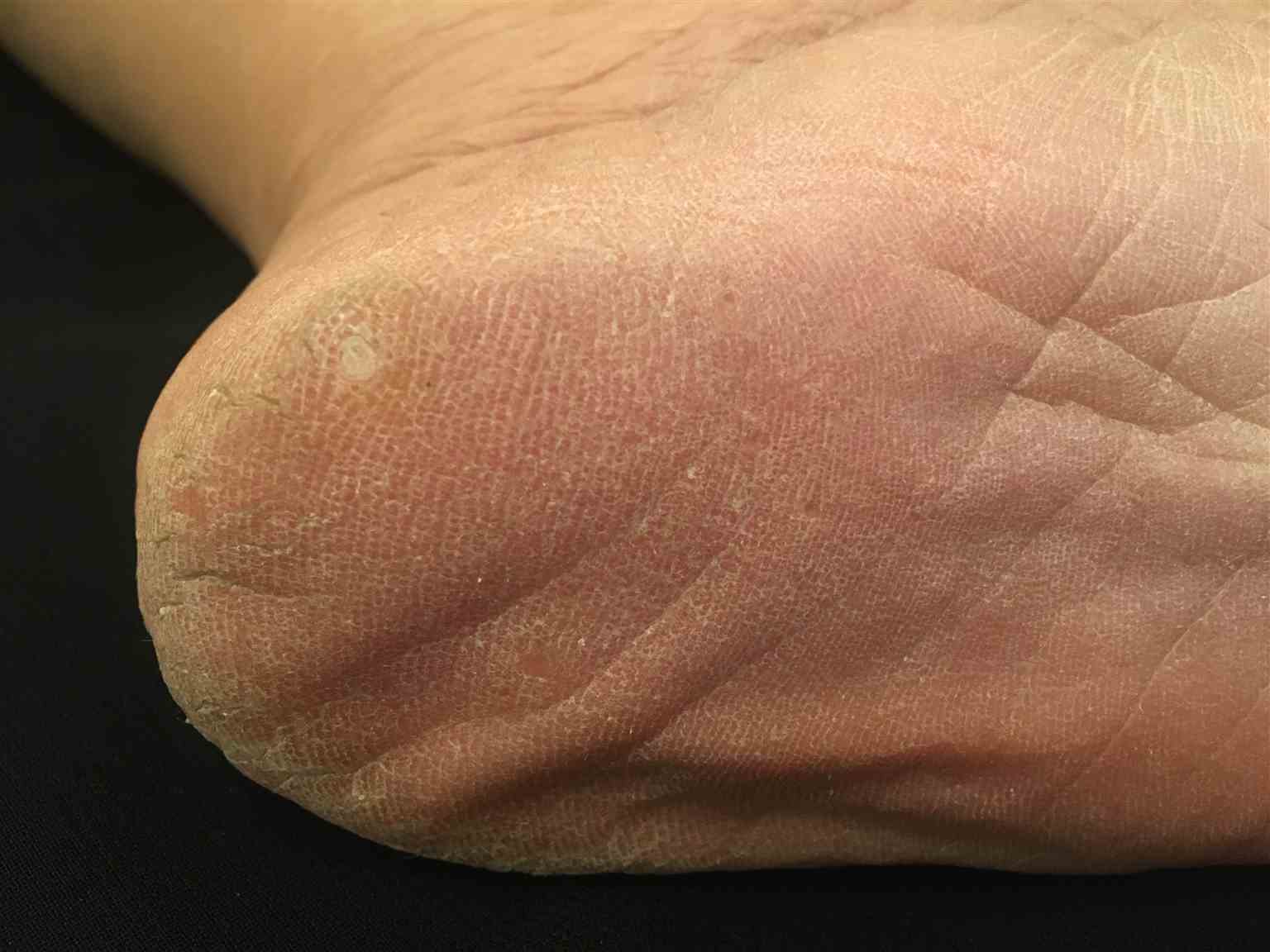
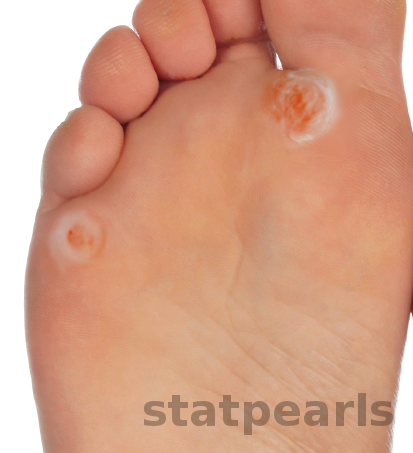
Corns usually present as flesh-colored dry, hard, rough papules with a whitish center (called the core). They are located over a bony prominence. They are painful on walking and standing but are asymptomatic to touch. As the overgrowth and thickening of keratin builds up, corns can grow and cause severe pain with ambulation.
There are two main variants of corn:
- Hard corn ('heloma durum') – This is the most common type of corn, usually located over the lateral and dorsal aspect of the fifth toe as well as on the dorsal aspect of the interphalangeal joints of the lesser toes.
- Soft corn or interdigital corn ('heloma molle') – this lesion is a painful hyperkeratotic lesion, primarily seen in the interdigital web spaces, especially the fourth space. This location often leads to maceration of the corn, with sometimes the occurrence of a bacterial or fungal infection or ulceration.[4]
Some authors add to these two variants a third one, called seed corn, which manifests as multiple nonpainful keratotic plugs within plantar calluses in non-pressure-bearing areas of the soles.
Corns sometimes are difficult to distinguish from plantar warts. In corns, the plantar skin lines may be observed within the lesions, unlike plantar warts. Furthermore, if the physician exerts a digital pressure perpendicularly to plantar corn, this latter will come into contact with the bony prominence, and the patient will feel pain. This maneuver is generally nonpainful in the case of warts. Finally, the absence of capillary dotting, called "Auspitz's sign" after paring hard corns distinguishes them from plantar warts. Dermoscopy can also be an additional tool to distinguish corns and plantar warts.[10]
Evaluation
Dermoscopy may help make the diagnosis by showing areas of hyperkeratosis without vascular or hemorrhagic structures that are mainly seen in warts.[10]
Radiographs of the feet may help to show bony prominences contribute to corn formation.
Pressure studies of the feet can highlight areas of excessive plantar pressure associated with plantar corns.
Other tests, like fasting glucose level and rheumatoid factor, may be done to find the etiology of foot deformity in some patients.
Treatment / Management
The treatment aims to reduce the pain and discomfort resulting from corns.[11][12]
- The treating provider should perform a gentle paring of the lesion without drawing blood, utilizing scalpels. Removing the central plug under local anesthesia, if necessary, reduces the pressure on underlying dermal nerves, thus alleviating the pain. Patients should be advised to trim the previously treated lesions weekly, using an emery board or pumice stone, after immersing the feet in warm water for twenty minutes. Patients with diabetes should be very careful if they have peripheral sensory neuropathy causing diminished sensation of their skin: it is advisable for people with diabetes with corns and calluses to have their podiatrist par debride the callus safely, as attempting this on their own in the presence of sensory neuropathy may lead to excessive trimming and ultimately abrasion of the skin.
- Topical keratolytic medications may be applied to the corns, including salicylic acid 12.6% to 40% as a pad or a solution. A randomized control trial comparing standard parring of calluses to 40% salicylic acid plasters found that the salicylic acid treatment group resolved more corns by proportion, delayed the time to recurrence, reduced pain, and reduced corn size over six months than the standard parring treatment group.[13] Urea 20% to 50%, silver nitrate, and hydrocolloid dressings can also be used in this indication. These techniques are more effective for a few lesions of interest. Topical keratolytic agents may also facilitate lesion paring by softening the corns.
- Ablative laser therapy may also be used to treat corns instead of paring them with a scalpel. The carbon dioxide laser has been reported to be efficient by some authors. The 2,940 nm erbium-doped yttrium aluminum garnet laser has been used to treat corns with minimal thermal tissue damage. However, the recurrence of lesions may be observed in some patients, especially if the trigger factors are maintained.
- Any biomechanical abnormalities and/or deformities should be managed with appropriate conservative treatment. This involves proper footwear, orthotics, and soft cushions (silicon sheet, sheepskin), which reduce friction and improve comfort.
Management begins with prevention. Patients should avoid ill-fitting shoes and mechanical trauma to the affected area.
Surgical
Surgical management is directed toward the removal of the underlying cause of corns, such as bony prominences. Usually, surgery is indicated in case of failure of other conservative treatment modalities. Heloma durum caused by hammertoe deformities in the foot that have failed conservative measures, such as wider shoes, periodic parring of the callus, and toe crests, are candidates for either an arthroplasty or arthrodesis of the interphalangeal joints of the affected toes. However, on the 5th toe, an arthroplasty, or surgical removal of the head of the 5th proximal phalanx, will release the contracture and alleviate the pressure caused on the soft tissue, thereby decreasing the rubbing and callus formation.[14]
For heloma molle formation in the 4th interspace, the head of the proximal phalanx of one toe is often abutting the base of the proximal phalanx of an adjacent toe, causing the painful, soft corn formation. While toe arthroplasty may be an option to correct a heloma molle of the 4th interspace, a surgical syndactylization is also an option, where the soft tissue of the 4th and 5th toes are fused. Syndactylization is performed by excising the adjacent skin surfaces between the fourth and fifth toes: this helps to maintain the apposition of the two toes, and permanent syndactylism of the 4th interspace is achieved. Thus, the syndactylization will prevent the recurrence of the heloma molle.[15] Syndactylization is often utilized to provide stability to a flail toe secondary to digital arthroplasty and is often used in combination with 5th toe arthroplasty in the treatment of 4 interspace heloma molle.[16]
Differential Diagnosis
The differential diagnosis of a corn includes:
- Plantar wart
- Poroma
- Warty dyskeratoma
- Calcinosis cutis
- Gout and pseudogout
- Hypertrophic lichen planus
- Interdigital neuroma
- Lichen simplex chronicus
- Palmoplantar keratoderma
- Keratosis punctata of palmar creases
- Porokeratosis plantaris discreta
- Porokeratosis palmoplantar et disseminata
Prognosis
Although corns and calluses are chronic, recurrent issues, most of them gradually spontaneously remit when repeated friction or pressure causes them to be eliminated. Nevertheless, if corns do not resolve or if they start to cause severe pain, the patient should enlist the assistance of a podiatrist.
In a small 2021 study involving 39 patients, surgical versus conservative treatment were compared, and noted 100% "very good or excellent" satisfaction in the surgical group, in contrast to 28.6% of patients who underwent conservative treatment.[17] High patient satisfaction rate and 93% of patients (n= 62 feet) reported pain relief with the operative repair of 4th and 5th-digit corns.[18]
Complications
Complications to corns include the following:
- Ulceration and infection
- Pain
- Tinea pedis
- Septic arthritis
- Osteomyelitis
Complications secondary to surgical repair:
- Joint and toe stiffness
- Digital swelling
- Numbness
- Infection
- Floppy or flail toe
- Deformity recurrence
Postoperative and Rehabilitation Care
After most surgical procedures for corns, the patient is allowed to weight-bear as tolerated in a special surgical shoe. The exact time required to wear the surgical shoe depends on the exact procedure performed but ranges from two to six weeks. Typically the patient is not allowed to remove the dressing nor get the foot wet. During the recovery, pain medications may be required for the first few days. If the right foot has undergone surgery, the patient will not be allowed to drive. Sutures are normally removed around two weeks after surgery. Physically therapy is not typically required.
Consultations
The following specialties are involved directly or indirectly in the treatment plan for cases of corns.
- Podiatry
- Orthopedic surgery
- Dermatology
Deterrence and Patient Education
Corns are thick round skin lesions typically appearing on the toes. Repetitive rubbing or pressure (e.g., shoe) is the leading cause of corns. Corns have a hardened central core, whereas calluses do not. Certain deformities, such as hammertoes, can cause corns as the crocked toes rub on the shoes.
Numerous treatment options for corns exist, ranging from conservative to surgical approaches. Results and patient satisfaction are very good. Foot and ankle surgeons can provide the best treatment options when corns become exceptionally painful. The recurrence rate is high unless the underlying cause of the corn is not addressed. Due to the potential to create a wound or serious infection, it is best to avoid self-removal at home and use medicated corn pads.
Patients with peripheral neuropathies should try to avoid the application of plasters that contain salicylic acid because these plasters might cause sloughing of normal skin if placed incorrectly. Calluses and corns are not caused by viruses and are not contagious. Patients should be instructed to trim their nails and wear wider shoes to avoid any pressure or repeated trauma, which might lead to the development of corns.
Pearls and Other Issues
One of the frequent pitfalls seen in clinical practice by some dermatologists is using liquid nitrogen (cryotherapy) for treating cases of corns. Unfortunately, this can lead to aggravation of the problem, which can add more to the patient's suffering since liquid nitrogen damages normal skin surrounding the corn and does not help heal the lesion.
Despite effective conservative treatment, corns are often recurrent.[19]
Enhancing Healthcare Team Outcomes
The management of corns is best performed with an interprofessional healthcare team. Patients may be treated by a primary care physician, nurse practitioner or physician assistant, dermatologist, or podiatrist. The key in all cases is to eliminate the continuous pressure on the foot. The treating provider should refer the patient to a surgical podiatrist or an orthopedic surgeon to evaluate for underlying bony abnormalities in lesions that are recalcitrant to treatment or recurrent. Foot care nurses are often involved in the diagnosis and treatment of corns. They should educate the patient on proper foot care and follow-up to ensure resolution, also serving as a liaison point between the various clinical disciplines involved in caring for the patient. Pharmacists often recommend over-the-counter products and should also inform the patients on the appropriate use of these agents, recommending further clinical intervention from a clinician in severe or recalcitrant cases.
While most corns are minor lesions and can be effectively treated with good resolution, an interprofessional approach is still necessary to preclude complications and to ensure the best possible patient outcomes, allowing a full return to regular activity when the lesions have impacted their activities of daily living or limited recreation or sports participation. [Level 5]