Continuing Education Activity
Volvulus occurs when portions of the bowel get entangled upon a mesenteric axis, which can cause impairment of the blood supply or result in complete or partial obstruction of the bowel lumen. This condition usually affects the colon. Colonic volvulus is rare in the United States and factors into about 4 percent of causes of large bowel obstruction, followed by cancer and diverticulitis. Of note, there are certain regions where colonic volvulus happens more frequently. In areas of the Middle East, India, South America, Africa, and Russia, colonic volvulus contributes to approximately 50 percent of all accounts of colonic obstruction. The regional areas listed above have been coined the "volvulus belt." Sigmoid volvulus occurs more frequently compared to cecal volvulus. This activity describes the evaluation and management of cecal volvulus and highlights the role of the interprofessional team in improving care for affected patients.
Objectives:
Determine the etiology of large bowel obstruction.
Determine the evaluation of large bowel obstruction.
Develop treatment considerations for cecal volvulus.
Communicate how coordination of the interprofessional team can lead to more rapid diagnosis of cecal volvulus and subsequently decrease associated morbidity and mortality in affected patients.
Introduction
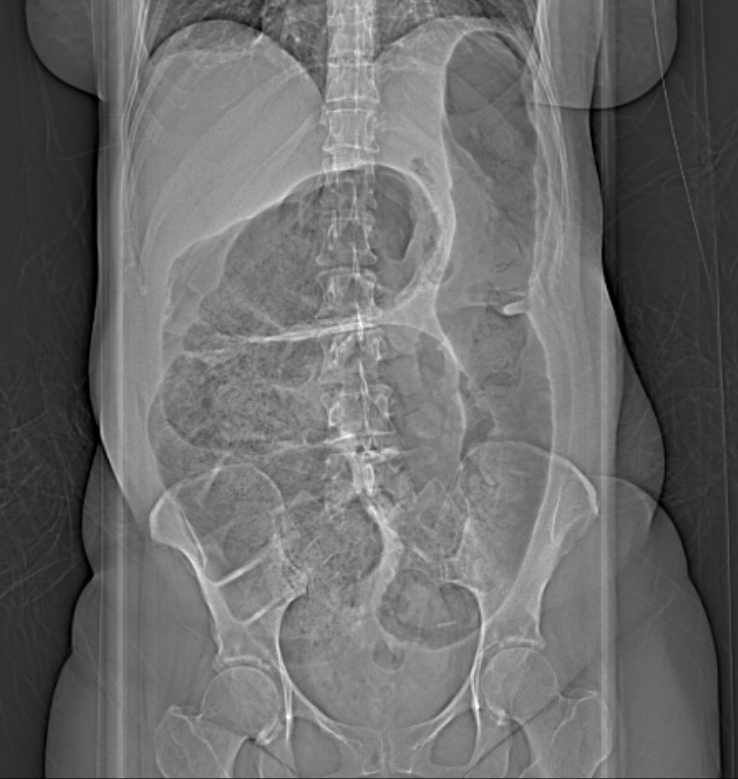
Volvulus occurs when portions of the bowel get entangled upon a mesenteric axis, which can cause impairment of the blood supply or result in complete or partial obstruction of the bowel lumen. This condition usually affects the colon. Colonic volvulus is a rare occurrence in the United States, attributing to approximately 4% of causes of large bowel obstruction, followed by cancer and diverticulitis. Of note, there are certain regions where colonic volvulus happens more frequently. In areas of the Middle East, India, South America, Africa, and Russia, colonic volvulus contributes to approximately 50% of all accounts of colonic obstruction. The regional areas listed above have been coined the "volvulus belt." Sigmoid volvulus occurs more frequently than cecal volvulus (see Image. Cecal Volvulus).[1][2][3]
Etiology
This condition occurs when redundant and loose mesentery twists around an axis. In terms of a cecal volvulus, the terminal ileum and right colon are involved. When a volvulus involves the cecum alone, it is also called a cecal bascule. This occurs when a highly mobile cecum traverses from a caudad to a cephalad direction.[4]
Epidemiology
United States
Colonic volvulus ranks below cancer and diverticulitis as a cause of large bowel obstruction.
- Colonic volvulus causes make up approximately 5% of intestinal obstruction.
- Colonic volvulus causes constitute 10% to 15% of all cases of large-bowel obstruction. The most common location of large-bowel torsion is the sigmoid colon (80%), the cecum (15%), the transverse colon (3%), and the splenic flexure (2%).
International
In Africa and the Middle East, nearly 50% of large-bowel obstructions are caused by volvulus, usually of the sigmoid colon. Cecal volvulus is less common than sigmoid volvulus, accounting for 10% to 15% of all cases of volvulus, and it tends to affect women in the sixth decade of life.
Pathophysiology
Associated risk factors for colonic volvulus are advanced age, chronic constipation, and diets rich in high fiber. Cecal volvulus most commonly occurs in the second and third decades of life, compared to sigmoid volvulus, which occurs in the seventh and eighth decades. Patients who have psychiatric conditions or are institutionalized and taking psychotropic drugs have a higher incidence of colonic volvulus. The use of psychotropic drugs can cause hindered intestinal mobility and predispose patients to volvuluses.[5][6]
In general, there are 3 different types of cecal volvulus:
- Type 1: This cecal volvulus forms by a clockwise axial twisting or torsion of the cecum along the long axis. The location of the cecal volvulus is in the right lower quadrant.
- Type 2: This cecal volvulus develops from a twisting or torsion of a portion of the cecum and a portion of the terminal ileum. The location of the cecum gets displaced to an ectopic location (typically the left upper quadrant) and is relocated in an inverted orientation. Traditionally, but not in all cases, a type 2 cecal volvulus encounters a counterclockwise twist.
- Type 3: This cecal volvulus (also known as cecal bascule) is the upward folding of the cecum. There is no axial twisting like with type 1 and type 2.
Type 1 and 2, which involve axial torsion, account for approximately 80% of all cecal volvuli. Cecal bascules account for the remaining 20% of cecal volvuli.
History and Physical
Patients with colonic volvulus may present with an intestinal obstruction. Often, the symptoms are hard to differentiate from blockages caused by colon cancers. Common symptoms are acute onset of severe abdominal pain, constipation, obstipation, nausea, and vomiting. Often, a tympanitic and markedly distended abdomen is seen, and often, the distention is more impressive than other causes of bowel obstruction. When the wall of the distended bowel is placed under increased tension, the cecal volvulus may be associated with ischemia. Another cause of ischemia may be occlusion of the arterial blood supply to the mesentery caused by torsion. Ominous signs include tachycardia, rebound tenderness, and severe abdominal pain not improved with medical management.
Evaluation
Workup for a colonic volvulus includes a complete blood count (CBC) with differential, a comprehensive metabolic panel, and lactic acid. Laboratory findings may be useful; however, they are not diagnostic. A leukocytosis level, a left shift (pandemic), or metabolic acidosis may indicate systemic sepsis, bowel ischemia, or peritoneal infection. Electrolyte abnormalities may develop in the setting of a bowel obstruction and vomiting.
Radiographic imaging can help differentiate between a sigmoid and cecal volvulus from other abdominal pathologies. For a cecal volvulus, an abdominal x-ray reveals a dramatic dilation of the bowel extending from the right lower quadrant, moving upwards to the left upper quadrant of the abdomen (Figure 1). Usually, a patient with a cecal volvulus presents with small and large bowel obstructions, with the collapse of the distal large bowel, and with extensive dilation of the proximal small bowel. A definitive sign of a cecal volvulus is the upward displacement of the appendix with obstruction of the large bowel. Comparatively, a sigmoid volvulus shows findings of a bent inner tube sign with the apex of the volvulus located in the left upper quadrant.
Abdominal plain films are sufficient to diagnose a sigmoid volvulus; however, abdominal x-rays are less diagnostic for cecal volvulus. Thus, the additional imaging of a CT scan can help differentiate the approximate location of torsion. An abdominopelvic CT scan is diagnostic for a cecal volvulus in approximately 90% of the patients. About 10% of the time, patients are diagnosed with a cecal volvulus intraoperatively.[7] A mesentery torsion around the ileocolic vessels, as seen on a CT scan, is described as a "whirl sign" and is considered pathognomonic for diagnosing a cecal volvulus.
Treatment / Management
Treatment for cecal volvuli usually entails a surgical intervention. Other inventions, such as a barium enema or a colonoscopy, can offer a non-operative reduction of cecal volvulus. However, these modalities are rarely successful. For these non-operative treatments, there is a high risk of perforations and should not be attempted. Colonic necrosis can be missed up to approximately 20% to 25% of the time when non-operative modalities are used. Surgical treatment varies based on patient stability and findings seen intraoperatively. Intraoperatively, the surgeon ascertains if there is bowel compromise or if the bowel is viable. These findings help dictate appropriate surgical intervention.[2][8][3] Treatment options include the following:
- For patients who are stable with no bowel compromise, an ileocolic resection or a right hemicolectomy should be performed. In patients that receive an ileocolic resection, an additional colopexy is needed to tack the right remnant colon to the posterior peritoneum to minimize the recurrence of another volvulus.
- For patients who are hemodynamically unstable without bowel compromise, a cecopexy should be performed in conjunction with a cecostomy tube placement, or cecopexy can be done alone.
- For patients who are stable with bowel, the surgeon should proceed with a right hemicolectomy or ileocolic resection followed by an ileocolic anastomosis.
- For patients who are unstable with bowel, the surgeon should proceed with a right hemicolectomy or ileocolic resection with an ileostomy creation. Later, once the patient is stabilized, the ileostomy may be reversed.
Differential Diagnosis
The differential diagnoses for cecal volvulus include the following:
- Acute mesenteric ischemia
- Sigmoid diverticular disease
Prognosis
Cecal volvulus is not a benign disorder. If the treatment is delayed, it carries a mortality in excess of 30%. Most studies indicate that treatment should be within 24-72 hours after diagnosis. This much time is required for hydration and any investigations. Even after cecal volvulus is treated, patients have high morbidity due to a prolonged ileus, wound infection, respiratory failure, and bowel obstruction.[9]
Complications
Common complications after cecal volvulus treatment include:
- Wound infection
- Sepsis
- Anastomotic leak
- Colocutaneous fistula
- Pelvic or abdominal abscess
Postoperative and Rehabilitation Care
Patients often require a prolonged stay in the hospital. Most patients are elderly and frail. If the ileus is prolonged, they often require IV fluids for a few days. DVT prophylaxis and physical therapy are recommended.
Pearls and Other Issues
Key facts to keep in mind about cecal volvulus are as follows:
- Cecal volvulus is much rare compared to sigmoid volvulus.
- With cecal volvulus, the torsion is usually in a clockwise direction.
- Vascular compromise is more common in cecal volvulus compared to sigmoid volvulus.
- The plain x-rays are usually adequate for diagnosis.
- The options for treatment include endoscopic decompression, cecopexy, or a right hemicolectomy.
- With decompression alone, recurrence rates are very high.
Enhancing Healthcare Team Outcomes
There are no evidence-based studies on the diagnosis or treatment of cecal volvulus. The condition is not so common in North America, but since it carries a very high mortality, it is important that healthcare workers be aware of the disorder. An interprofessional team approach is recommended to ensure prompt diagnosis and treatment. Since most patients present in the emergency room, the triage nurse and the emergency physician must know the importance of timely admission and referral to a general surgeon. Because most patients have numerous comorbidities, the initial management is best done in a critical care unit. The patient must be hydrated and cleared for surgery by the internist. Depending on the patient's age and comorbidity, the type of procedure varies. Hence a gastroenterologist and a general surgeon must communicate to offer the patient the best treatment. Clinicians in the ICU need to monitor the vitals, abdominal girth, and urine output prior to surgery. A colostomy nurse should see the patient in case of an ileostomy or a colostomy.[3][10][11]
Outcomes
There are only small case series and isolated reports on outcomes of patients managed with cecal volvulus. For those who have delayed diagnosis, the outcomes are poor. Even those who undergo timely surgery have high morbidity as a consequence of their age. Laparoscopic surgery is preferred to open surgery, but sometimes the urgency of the situation may not allow it. No matter how one approaches the patient, the family must be fully informed of the potential complications, including recurrence and a stoma.[12]