Continuing Education Activity
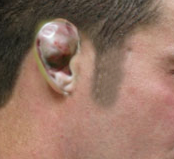
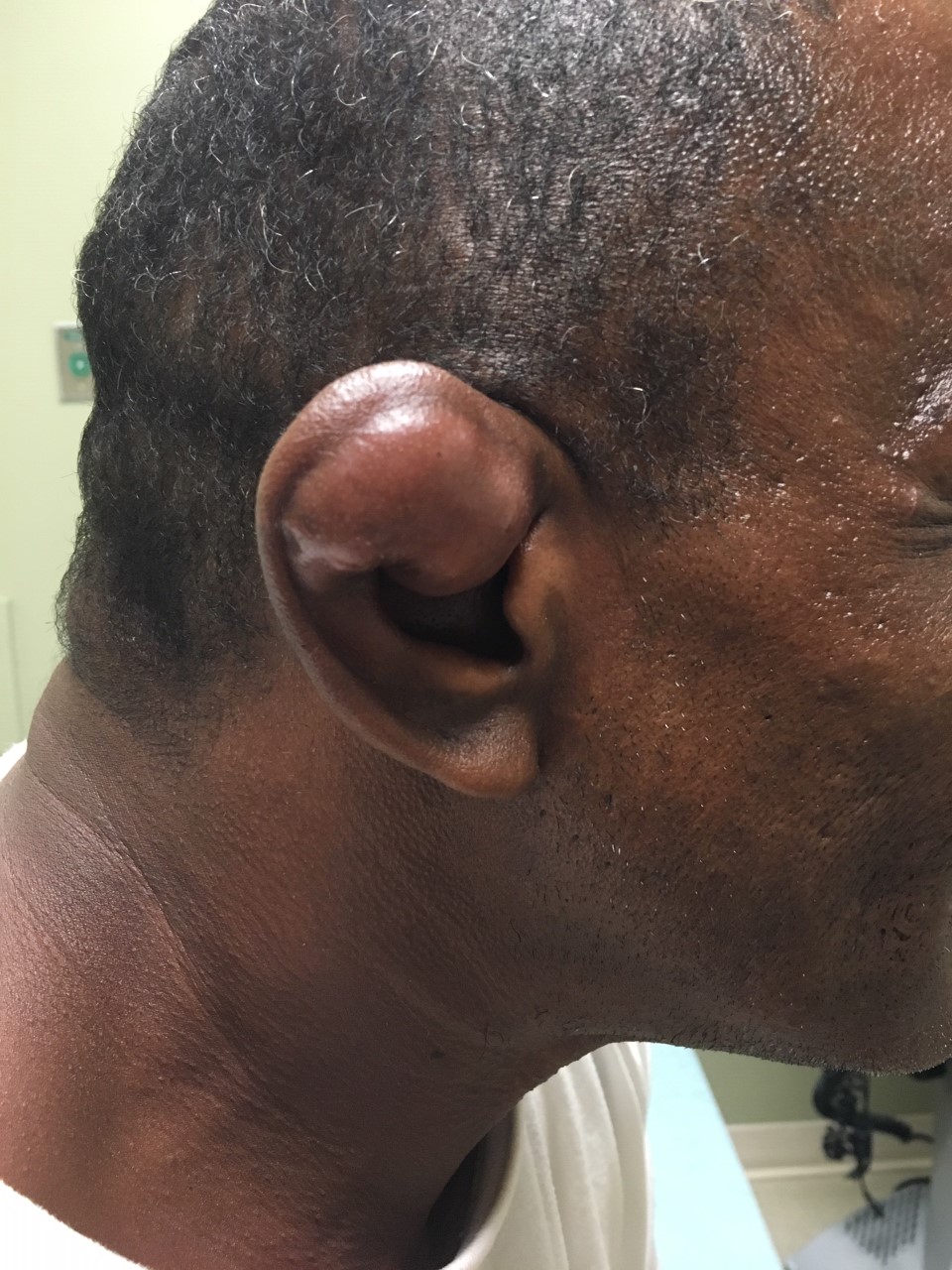
Cauliflower ear, also known as wrestler's ear or perichondrial hematoma, is a deformity caused by blunt trauma to the auricle. It occurs as blood accumulates in the pinna that can disrupt the blood supply of the healthy cartilage. The resulting fibrosis leads to the development of a cauliflower ear. This activity outlines the evaluation and management of the cauliflower ear and reviews the role of the interprofessional team in managing patients with this condition.
Objectives:
Describe the role of hematomas in the pathophysiology of cauliflower ear.
Identify the history of direct trauma in patients with cauliflower ear.
Summarize the use of emergency aspiration, compressive dressings, and surgery in the treatment of cauliflower ear.
Explain the importance of improving care coordination among the interprofessional team members to educate the patients on the adequate protection of the ear while playing contact sports for those at risk for developing cauliflower ear.
Introduction
Cauliflower ear is a deformation of the ear typically caused by direct blunt trauma to the auricle and surrounding tissue. Classically experienced by wrestlers or boxers, the condition can be seen in any activity where significant shearing or impact forces are experienced by the pinna, leading to an auricular hematoma. The hematoma then elevates the auricular perichondrium from the underlying cartilage, devascularizing the cartilage. The blood accumulates in the subperichondrial space and if left untreated can lead to necrosis, infection, and loss of cartilage. Cauliflower ear is the product of the fibrocartilage and fibrosis that occurs upon the destruction of the auricular cartilage once it loses its blood supply.[1][2][3]
Etiology
Description of cauliflower ear dates back to early Roman and Greek history. Literary and artistic collections from that time are littered with accounts describing the deformed or damaged ears of wrestlers, boxers, or other pugilists. Medical appreciation for the affliction has a similar storied past. Though case descriptions can be found in the works of Hippocrates, more formal research into the disease did not begin until the mid-1800s. At that time, there was thought to be a second idiopathic cause behind the cauliflower ear to go along with the more obvious relationship to direct trauma. The idiopathic hypothesis derived from observations of the elderly and mentally insane. It wasn’t until the late 20th century that the more conventional understanding of cauliflower developed, paralleling more modern advances in the physiology of trauma and wound healing.[4][5]
Epidemiology
The exact prevalence of the cauliflower ear is not easily described in the literature. In general, the higher-level the athlete in an at-risk sport (wrestling, boxing, martial arts, rugby, etc.), the higher the prevalence of the cauliflower ear. One study of national-champion-level Finnish martial artists described a prevalence of auricular hematoma of 96%, with cauliflower ear seen in 84% of men.[6]
Pathophysiology
Historically, researchers have debated the exact mechanism behind the formation of cauliflower ear. From a series of experiments conducted in the mid-1970s when weights were dropped on the ears of rabbits, researchers concluded hematomas in the intercartilaginous space were responsible for the deformity. However, further testing (and more rabbits), showed blood accumulation in the subperichondrial space was responsible for disrupting circulation to the anterior ear from the posterior auricular and superficial temporal arteries. This buildup leads to the necrosis of the ear’s healthy cartilage. The hematoma is then replaced by chondroblasts which form neocartilage. This process sets into action a cascade of fibrosis and contracture and the subsequent development of cauliflower ear.[7]
History and Physical
Patients present with a history of trauma to the affected ear, usually during contact sports like wrestling, boxing, rugby, or increasingly, mixed martial arts. The ear appears red due to hematoma, swollen, and warm, while the patient may describe any combination of difficulty hearing, tinnitus, vision changes, pain, and/or a headache. If there is no concern for more underlying severe cranial pathology, then the practitioner should continue directly to treatment. If there has been any loss of consciousness or other neurologic symptoms, the workup of these may take precedence over the auricular hematoma depending on the individual scenario.
The strong relationship between trauma causing auricular hematomas should make practitioners suspicious of those individuals presenting with the signs described above, but who deny having undergone any reported trauma. Especially where children and the elderly are concerned, it is crucial that the possibility of abuse be entertained and screened for through a careful history and exam.
Evaluation
Cauliflower ear is a clinical diagnosis that requires no formal testing or imaging, but practitioners should be alert to any signs of concussion in any patient with a history of head trauma.
Treatment / Management
The management and treatment of cauliflower ear can take many forms depending on when the patient presents and the size and scope of the deformity. It should be noted from the outset that the cauliflower ear is potentially avoidable through the appropriate covering and protection of the ear during contact sports. This protection reduces or eliminates the types of blunt, shearing forces the ear experiences altogether and subsequently, the formation of an underlying hematoma. According to studies of wrestlers, the use of protective headgear can reduce the prevalence of auricular hematomas by up to 50%.[8][9][10]
Any trauma to the head severe enough to injure the exterior ear mandates a thorough head and neck examination that includes the otoscopic inspection of the tympanic membranes, a cranial nerve examination, and a detailed neurologic examination. This helps ensure a more critical intracranial injury is not overlooked. If any focal deficits are noted, computed tomography of the head may be required.
The primary treatment for cauliflower ear is prevention. The best possible outcomes require early identification and management of the hematoma before cartilage death has occurred. Typically, this requires a patient be seen within the first six hours after the injury so that an emergency department provider can aspirate the underlying auricular hematoma and secure a bolster to prevent re-accumulation. This involves anesthetizing the distribution of the greater auricular nerve (often best achieved via a circum-auricular block) using lidocaine and epinephrine. This is followed by the insertion of an 18-gauge needle into the area of greatest fluctuance. If the patient is unfortunate enough to present outside the 6-hour period where aspiration is likely to be successful, a more invasive incision may be required to be sure to remove any blood that has begun to coagulate. Aspiration is always an appropriate first step, and if any palpable clot is still present, the needle incision can be gently probed with a hemostat or enlarged with a scalpel to allow bimanual expression of the clot before placing a bolster dressing.
By removing the pocket of blood, the perichondrium can reattach to the ear’s cartilage, preventing the loss of its valuable blood supply. Further aiding in the ear’s development of healthy cartilage, is the use of compressive dressings. A variety of compressive dressings are described in the literature including cotton bolsters, dental silicone, silicone rubber splints, or even auricular stents, but no one technique has been studied and deemed superior. Some sort of compressive bolster must be placed to eliminate the dead-space and re-appose the perichondrium or recurrence is assured.
Unfortunately, recurrence remains a frustrating complication of treating cauliflower ear. The most successful management of an auricular hematoma comes with the high likelihood that the blood will re-accumulate, particularly if no bolster was placed. These patients require close follow up to ensure there has been no re-accumulation (or to drain any re-accumulated fluid). Outpatient follow-up in three to five days after the injury is prudent.
For patients who present outside the window when auricular hematoma drainage is feasible, surgical intervention remains the mainstay of treatment. In general, surgical referral is appropriate for any patient with an existing cauliflower ear, where extensive fibrosis has already occurred. Once the surgery is settled upon, the exact approach can vary based on the degree and location of the underlying deformity. Some texts go so far as to classify the cauliflower ear into four distinct types, each requiring a unique reconstructive technique. The overall goal of surgery, however, remains the same regardless of surgical method, and that is to remove the damaging fibrocartilage without compromising the ear's structural integrity or its natural contours. If damage to the ear is so severe that simply removing the malformed cartilage does not equate to the desired cosmetic outcome, costal cartilage can be used to provide greater structural integrity. For these reasons, many plastic surgeons are loathed to operate on a mature cauliflower ear that is not causing obstruction of the external ear canal, simply advising protective headgear. This is especially true if the patient is continuing to engage in the high-risk activity.
Differential Diagnosis
- Acute (bullous) and chronic (granular) myringitis
- Otitis media with a perforation or ventilation tube present
Prognosis
If treated soon after the injury with appropriate drainage and bolster dressing, the prognosis is very good that the patient will not develop a cauliflower ear, or that the effects will be minimal. If the patient has a longstanding cauliflower ear and desires aesthetic improvement, the results are often extremely disappointing. This is a problem best prevented through protective sportswear, or through prompt recognition and treatment should it occur.
Complications
Recurrence is the major complication after the drainage of an auricular hematoma, abscess, or seroma, which can lead to a cauliflower ear if not appropriately managed. Complications of a cauliflower ear are typically aesthetic, though they can very occasionally be painful or lead to obstructive symptoms of the external auditory canal.
Consultations
If the physician is uncomfortable managing an auricular hematoma, seroma, or abscess, emergent consultation to an otolaryngologist, facial plastic surgeon, or plastic surgeon is required.
Enhancing Healthcare Team Outcomes
Patients with cauliflower ear may present to the emergency department physician, nurse practitioner, primary care provider or the sports physician. While the diagnosis is simple, the management can be difficult. In acute cases, aspiration is sufficient. The key is to educate the patient on prevention while playing sports. Unfortunately, recurrences are common if not managed appropriately. The cauliflower usually imparts poor aesthetics which cannot be reversed.[11][12]