Continuing Education Activity
Angioedema is characterized by one or more areas of well-demarcated, non-pitting edema of deep subcutaneous tissues. It is primarily known to involve the face, lips, tongue, and oropharynx, but also, can also involve the genitals, distal extremities, and gastrointestinal mucosa. Immediate identification of angioedema is of the utmost importance due to the potential for rapid development and progression of life-threatening airway compromise. This activity eviews the evaluation and treatment of angioedema and highlights the importance of a cohesive interprofessional team in providing optimal care to patients with angioedema.
Objectives:
- Describe the evaluation of a patient with angioedema.
- Explain when airway intervention should be considered in patients presenting with angioedema.
- Describe the treatment of angioedema.
- Develop a cohesive, interprofessional team approach to evaluate and manage patients with angioedema.
Introduction
Angioedema is characterized by one or more areas of well-demarcated, non-pitting edema of deep subcutaneous tissues. Although known primarily to involve the face and intra-oral area, it can also involve the genitals, distal extremities, and intraabdominal gastrointestinal mucosa[1]. Immediate identification of angioedema is of the utmost importance due to the potential for rapid development and progression of life-threatening airway compromise due to either intraoral and/or laryngeal edema.
Etiology
There are several etiologies of angioedema, most notably angiotensin-converting enzyme inhibitor (ACEI) use. With tens of millions of people taking ACEIs, the incidence of ACEI angioedema is rising[2]. African Americans are at a much higher risk for ACEI angioedema, possibly due to lower endogenous bradykinin and increased sensitivity to ACEI-mediated increases in bradykinin.
Other etiologies include IgE-mediated allergic reactions (such as to food, drug, or environmental triggers), nonsteroidal anti-inflammatory drug (NSAID) use (including aspirin), and chemically-induced histamine release (most commonly opiates, highly cationic antibiotics, and muscle relaxants)[1]. A less common cause is hereditary angioedema (HAE) and acquired angioedema (AAE), both caused by a C1-inhibitor (C1-INH) deficiency.
HAE and AAE are rare. AAE is due to an acquired deficiency of (C1-INH), caused by either consumption (type 1) or inactivation (type 2)[3]. This increased catabolism can be related to an autoimmune disorder (e.g., systemic lupus erythematous) or a malignant tumor (e.g., lymphoma)[4]. Angioedema recurs unpredictably, lasting from two to five days. It not only presents with edema of the areas mentioned above, but it can also cause severe abdominal pain due to gastrointestinal mucosa edema. AAE recurrence is associated with various conditions such as different forms of lymphoproliferative disorders[5].
Epidemiology
Less than 1% - 2% of angioedema cases are characterized as either HAE or AAE, with HAE having been noted to be about ten times more common than AAE. While the prevalence of AAE is difficult to estimate due to its rarity and potential lack of recognition, some estimate it to be between 1:100,000 and 1:500,000. Specific triggers include trauma, medical procedures, emotional stress, menstruation, oral contraceptives, infections, and drugs, although flare-ups are unpredictable.
Other specific notable factors include more than 90% of patients developing AAE after 40 years of age, and that those suffering from AAE exacerbations have abdominal pain less than 50% of the time as compared to those with HAE having abdominal more than 80% of the time.
Pathophysiology
Angioedema’s underlying pathophysiology involves increases in vascular permeability and vasodilation that is histamine, bradykinin or complement-mediated, resulting in fluid extravasation into interstitial tissues. Active C1-INH is decreased through catabolism or binding that renders it inactive. The decrease of C1-INH causes deregulation of the complement pathway, leading to increased vascular permeability, mast cell degranulation, and increased bradykinin levels. Neutralizing autoantibodies to C1-INH are present in the majority of patients.
History and Physical
It is of utmost importance to obtain medication, food, and environmental exposure history with special attention to ACEIs and NSAIDs as possible causative factors. Also, find out if prior similar events have happened in the patient or family members. If no factors can be identified, then HAE/AAE should be considered. Distinguishing AAE from HAE can be challenging. However, there are characteristics in the patient’s history that can help distinguish HAE from AAE. Unlike HAE, AAE can be late onset (older than 40 years old). There will also be no family history of HAE, and there may be signs and symptoms that suggest an underlying malignancy[6]. Determination of C1 esterase and C4 levels allow differentiation of HAE and AAE from other causes of angioedema.
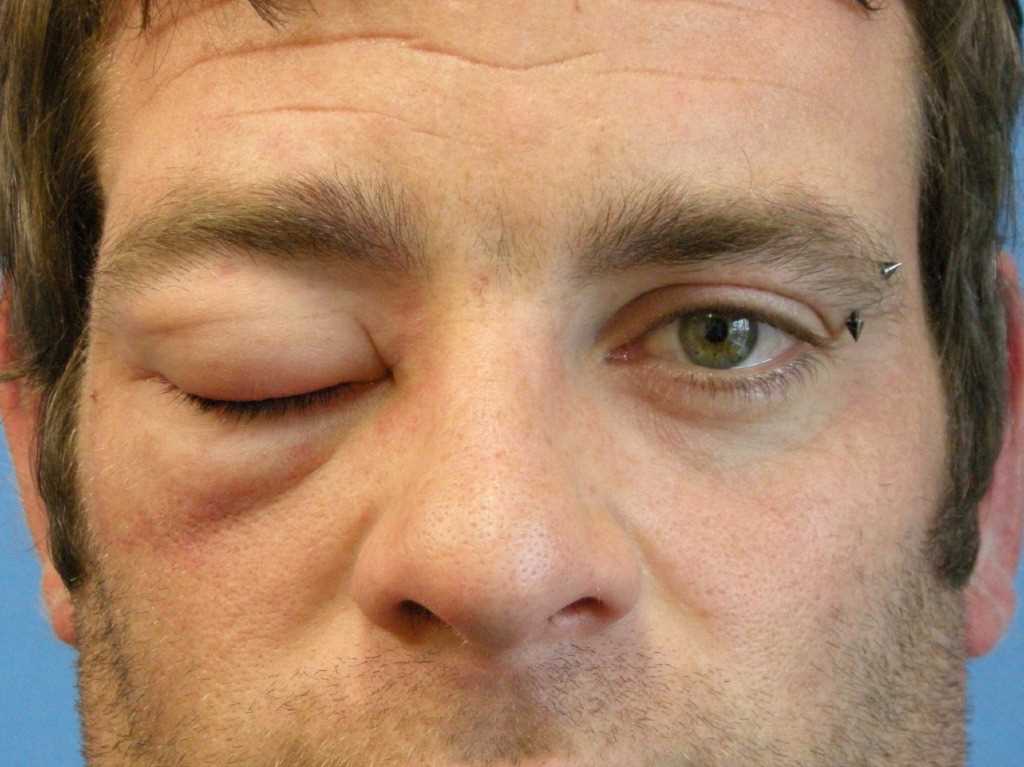
On physical exam, the hallmark of angioedema is localized, well-demarcated, non-pitting edema that most commonly involves the lips, tongue, face, and eyelids. It may also involve the larynx, genitals, and distal extremities. Urticaria may also be present. Angioedema can also cause recurrent, severe abdominal pains mimicking a surgical abdomen, which can lead to partial bowel resection[7].
It is always important to consider other possible diagnoses, like infection, a local reaction to insect bites, congestive heart failure, and renal or liver disease. Characteristics that suggest angioedema include rapid onset, an asymmetric distribution of edema, and absence of symptoms that point to other possible diagnoses.
Evaluation
Rapid assessment of the airway is critical. In one study, patient age as well as edema involving the oral cavity and/or the oropharynx, were predictive of the need for airway intervention while involvement of other sites, etiology and sex were not[8]. In another study, voice change, hoarseness, stridor, or dyspnea were highly predictive of impending airway compromise, and fiber-optic nasopharyngoscopy was shown to identify laryngeal involvement[9].
If definitive airway management is needed, direct laryngoscopy may be difficult or even impossible due to the inevitable distorted airway anatomy, making awake fiberoptic intubation an attractive alternative. Providers may consider preserving the patient’s respiratory effect during intubation with only mild sedation and no paralysis since the intubation has a high probability of being difficult. Because of this, advance preparation for cricothyrotomy is key in case airway securement becomes impossible.
Treatment / Management
Because initially, the cause of angioedema is likely to be unknown, the mainstays of initial medical management include supplemental oxygen, a parenteral H-blocker, a parenteral steroid, and intramuscular epinephrine. Unfortunately, in AAE standard regimens of epinephrine, corticosteroids and antihistamines do not have much effect and are not recommended for AAE. Administration of plasma-derived or recombinant C1-INH can resolve acute attacks, but some patients will become non-responsive[5].
Icatibant, a bradykinin B2 receptor antagonist, has been shown to provide symptoms relief in AAE and was well tolerated[10]. Ecallantide, a potent bradykinin pathway inhibitor, has also shown promise in the treatment of AAE, providing another alternative in the treatment of patients with resistance to C1-INH replacement[11]. If neither treatment is available, fresh frozen plasma (FFP) may be used. Although effective (at least in HAE), it at times will lack efficacy or even cause a sudden worsening of the patient’s symptoms. There is also the risk of viral transmission to consider[12]. Rituximab efficacy has been shown to be inconstant in AAE[13]. It is also important to consider that treatment of an underlying causative condition can result in improvement of AAE[4].
The emergency department course is varied and clinical evolution may reflect the natural course of the illness rather than an actual response to medical management. Therefore, frequent re-evaluation is essential to monitor for any sudden deterioration in clinical status. If a patient has persistent involvement of the tongue, intraoral cavity, or throat, if they have persistent or recurring airway edema, or if they have persistent signs and symptoms of anaphylaxis (e.g., hypotension, cardiovascular compromise, altered mental status) then they require admission to the hospital in an intensive care setting. However, if the angioedema is limited to the face and lips or there is localized tongue involvement with a fully visible soft palate, patients may be observed in the emergency department for four to six hours before discharge home if they are reliable with a good support system at home.
Differential Diagnosis
- Intestinal occlusion syndrome
- Hereditary angioedema
- Histamine-induced angioedema
Pearls and Other Issues
Symptoms of angioedema include angioedema of the face, laryngeal edema leading to difficulty with breathing, edema of the extremities and genitalia. Abdominal pain and bloating may occur together with hypotension.
Angioedema in the absence of urticaria indicates a bradykinin-mediated mechanism, most commonly C1-INH deficiency and may be hereditary or acquired.
Acquired angioedema may have underlying autoimmune connective tissue disease or a lymphoproliferative disorder.
Enhancing Healthcare Team Outcomes
The diagnosis and management of angioedema is best done with an interprofessional team that includes the emergency department physician, nurse practitioner, anesthesiologist, allergist, pharmacist and an intensivist. Time is of essence as the condition can rapidly lead to respirtaory distress.
Because initially, the cause of angioedema is likely to be unknown, the mainstays of initial medical management include supplemental oxygen, a parenteral H-blocker, a parenteral steroid, and intramuscular epinephrine. Unfortunately, in AAE standard regimens of epinephrine, corticosteroids and antihistamines do not have much effect and are not recommended for AAE. Administration of plasma-derived or recombinant C1-INH can resolve acute attacks, but some patients will become non-responsive[5]. Once the patient is stabilized, the cause of angioedema should be determined. The outcomes depend on the cause.