Continuing Education Activity
Allergy is described as an exaggerated response from the body’s immune system to otherwise inert substances present in the environment. The usual symptoms are pruritus, flushing, rash, urticaria, swelling of the lips, tongue, and airway, (angioedema), nausea, vomiting, abdominal cramping, shortness of breath, wheezing and bronchospasm, stridor, syncope or collapse. This activity illustrates the etiology, pathophysiology, classification, and clinical symptomatology of allergy and highlights the role of health care providers in managing and educating the patients.
Objectives:
- Outline the etiology and pathophysiology of allergy.
- Review the clinical manifestations of allergy.
- Summarize the treatment and counseling strategies for patients with allergy.
- Describe how an optimally functioning interprofessional team would coordinate care to maximize patient education to achieve better clinical outcomes.
Introduction
Allergy is a broad topic and speaks to the body’s immune response to foreign substances common in the environment, and triggers a reaction from the body’s immune response described as hypersensitivity. Hypersensitivity is an inappropriate immune response to common, typically harmless antigens, manifesting as a continuum from minor (atopic dermatitis and rhinitis) to severe manifestations (anaphylaxis, anaphylactoid and asthma). The focus here will be anaphylaxis; other topics of atopic dermatitis and allergic asthma involve many of the same modulators, responses, and treatments.[1]
The most common triggers of anaphylaxis include foods, medications, insect stings, and allergen immunotherapies. Any substance that can trigger the degranulation of mast cells or basophils can induce anaphylaxis. The definition of allergy and anaphylaxis has varied in the past; in 2005, an interprofessional group of clinical experts was formed to improve recognition and designate criteria for the diagnosis of anaphylaxis. The incidence of anaphylaxis varies between 0.5 to 2% in the general population, and the rate has been increasing. The lifetime prevalence is 1.6%.[2]
Etiology
Anaphylaxis is the most severe form of a hypersensitivity reaction that has a rapid onset from minutes to hours. The reaction is caused by the activation of mast cells and basophils through the binding of cell membrane receptors to IgE antibodies. The activation of these cells causes the release of mediators from secretory granules such as histamine, tryptase, carboxypeptidase A, and proteoglycans. This reaction progresses to the activation of secondary substances like phospholipase A2, then cyclooxygenase and lipogenesis as well as arachidonic acid, platelet-activating factor, and tumor necrosis factor-alpha. These cytokines and chemokines create life-threatening symptoms, including bronchoconstriction, increased vascular permeability, and facial flushing. The reaction further progresses with the platelet-activating factor, which causes bronchoconstriction and vascular permeability. The activation of neutrophils by tumor necrosis factor and further recruitment of effector cells, and enhances chemokine synthesis. This severe rapid progression is life-threatening and leads to death without intervention to triggers either a reversal or stopping the process promptly, preventing secondary reactions.[3][4]
Common known triggers of anaphylaxis are bee stings, peanuts, (legumes), latex, and medications, but other substances can trigger this reaction. Therefore, an interprofessional approach to diagnosis is the recommendation. Patients may have anaphylaxis if they meet the criteria below
1. Acute onset of illness involving the skin, mucosal tissue, or both. This process is over in minutes to hours and can be in the form of generalized hives, pruritus, flushing, swollen lips, tongue, and uvula. In addition to these, there should be at least one of the following:
a) Respiratory compromise such as dyspnea, wheezing, bronchospasm, stridor, and decrease peak inspiratory effort and hypoxemia (which can be produced by the tissue edema and capillary leak in the lung tissue).
b) Reduced blood pressure or associated signs and symptoms of end-organ hypoperfusion (shock, hypotonia, syncope, incontinence).
2. Two or more of the following reactions that occur rapidly after exposure to a likely allergen (referred to in the literature as antigens, haptens, and mast cell receptor stimulants) for seconds or up to several hours.
a) Involvement of the skin-mucosal tissue signified by hives, itching to flushing, and swollen tissues such as lips, tongues, and uvula; other mucosal tissue can be affected as well from topical exposure and may not be as evident.
b) Respiratory compromise from dyspnea, swelling of the bronchus causing wheezing, bronchospasm, and stridor, or reduced peak expiratory flow and hypoxia.
c) Reduced blood pressure or associated symptoms of syncope.
d) Persistent gastrointestinal signs and symptoms such as cramping, vomiting, excessive salivation with due to inability to swallow secretions).
(Skin symptoms are absent or unrecognized in up to 20 percent of episodes, thus incorporating the other symptoms of gastrointestinal or the listed symptoms improve recognition of anaphylaxis and allergy).
3. Reduced blood pressure alone after exposure to a known allergen for that patient as defined below:
a) Reduced blood pressure in adults is a drop in systolic to less than 90 or greater than a 30 percent drop from that person's baseline.
b) Reduced blood pressure in infants and children is the systolic blood pressure lower than normal for their age-specific rage or greater than 30 percent drop in systolic blood pressure:
(age [in years] x 2) + 70 mmHg up to 17 years of age (e.g., a child 1 month old; 1 month/12 months = (0.083 x 2) ==> 0.16 + 70 = 70.16)
Please note; once the age calculation reaches 90 mmHg, one can use the systolic pressure of 90 mmHg.
(This allows for the detection of anaphylactic reactions in which only one organ system is involved.)
Further, a response of resolved signs or symptoms to epinephrine for a known allergen would also be considered anaphylaxis.[5][6][7]
Epidemiology
Anaphylaxis has a prevalence between 0.5 and 2 percent in the general population for industrial nations, and there is an increasing rate of occurrence. The United States' lifetime prevalence is 1.6 percent. Allergic atopic dermatitis prevalence is 5 to 20 percent of children worldwide. In the United States, it is 11 percent. Allergic rhinitis prevalence is 10 to 30 percent in the United States. Rhinoconjunctivitis was found to be 8.5 percent for children 6 to 7 years of age and 14.6 percent for 13 to 14 years of age in the Study of Asthma and Allergies in Childhood. The study has found that the overall prevalence is increasing in the industrialized world. Atopy is the genetic predilection to produce IgE in response to exposure to allergens and may be related to an increased incidence.
Pathophysiology
Allergy pathophysiology is viewable through different mechanisms depending on the cause. The discussion then follows focusing on haptens (e.g., small-molecule drug reactions) that result from a direct effect. The hapten (drug) binds directly to mast cells of the immune system (also known as effector cells). This binding triggers the mast cell to degranulate, releasing histamines and chemotaxis creating symptoms of urticaria or anaphylaxis, referred to as a direct antigen response. Similar effects can occur with checkpoint inhibitors used in cancer treatment (melanoma and renal cell carcinoma) the mechanism is unclear.[8][9]
Immune drug reactions are rare because they are small molecular weight compounds with simple structures. B and T cell receptors do not easily recognize these structures. Medications can become immunogenic by the small structures covalently binding to larger macromolecules. These are host proteins on or inside of cells or in plasma, and they form a complex called a hapten. The haptens then bonded by a carrier complex (integrins or albumin). These complexes are presented to B Cells creating antibody responses and to T Cells creating responses through the human leukocyte antigen (HLA) molecules. Occasionally haptens are not formed from the medications themselves, but their metabolites form pro-haptens; this is the mechanism of penicillin and other beta-lactam antibiotics (cephalosporins, carbapenem, and monobactams). A similar mechanism occurs in the liver metabolism with cytochrome P450 enzymes forming metabolites the become pro-haptens. Sulfamethoxazole is an example when it metabolizes to sulfamethoxazole-hydroxylamine and then oxidized to sulfamethoxazole-nitroso, which stimulates both T and B cells. Other examples are phenacetin, halothane, phenytoin, carbamazepine, and lamotrigine.[10][11]
There is a concept of a direct immune response to medications and drugs or even biologic therapies that use proteins to stimulate a response. This concept involves the pharmacological interaction of drugs with immune receptors known as the p-i concept). The theory is that certain drugs in their naive state without processing or metabolism can stimulate T cells through T cell receptors (TCRs) or HLA molecules that are not their primary therapeutic targets. This stimulation is called “off-target” activity and explains genetic propensity through TCRs and HLA of individuals. A specific example is drugs that produce a drug reaction with eosinophilia and systemic symptoms/drug-induced hypersensitivity syndrome. (DRESS/DiHS) such as flucloxacillin and sulfamethoxazole). The mechanisms of p-i TCR and p-i HLA are different, but the concept is direct off-target induction of the immune system is the concept. In the p-i TCR model, a drug interacts with a TCR. Then a second interaction between the TCR and HLA molecules on APCs is required to stimulate a cellular proliferation, cytokine production, and cytotoxicity by the drug stimulated T Cells. Sulfamethoxazole, as an example, is a common public epitope, but another factor is required to induce it, such as a generalized viral infection.[12][13][14][15]
PilA model the drug binds preferentially to certain HLA molecules. There is a strong association with some HLA alleles. Thus, binding to them leads to T Cells stimulation by HLA drug complexes. The drug binding to the peptide-binding site in HLA has two possible consequences 1 HLA molecule acquires features of an allollele and makes a self HLA protein look like an Allo-HLA. 2 The drug binding to the peptide-binding site may be the presentation of an altered peptide repertoire. This happens in the endoplasmic reticulum(ER). The altered HLA molecule may allow the presentation of a different set of peptides to T Cells, Since T cells are tolerant to those HLA restricted peptides which they were exposed during development in the thymus, the alternate set of peptides may be interpreted as foreign by T cells and result in an autoimmune-like T cell reaction.[13]
- Examples of p-I TCR Sulfamethoxazole lamotrigine
- Examples of p-I HLA with interaction TCR carbamazepine
- Examples of p-I HLA predominantly main metabolite allopurinol - oxypurinol
- Lidocaine and mepivacaine
- Another p-I HLA radiocontrast agent iomeprol, flucloxacillin, and abacavir
The standard immune responses Gell and Coombs:
Type 1 immune reactions require a drug-specific immunoglobulin E(IgE), which requires a sensitization stage: The formation of drug-specific IgE normally requires coordinated actions of B cells and T Helper Cells the B cells process the hapten-carrier complex and present haptenized peptides to T cells. B and T cells interact via the HLA complex and the T cell receptor TCR and through CD40 on the B cells and CD40L on the T cell. This antibody form attaches to mast cells, and basophils surface sensitizing them then the effector stage the individual is re-exposed to the medication or substance cross-links on the sensitized mast and basophil cells resulting in sudden and widespread activation and release of an array of vasoactive mediators leading to what is called an immediate onset. Thus type one reactions are IgE immediate sensitivity reactions (humoral response activation).[17]
Type II (antibody-mediated cell destruction) are uncommon and involves antibody-mediated cell destruction; this involves IgG and occasionally IgM antibodies. The mechanism drugs or substances bind to surfaces of certain cell types (most often red blood cells or platelets and occasionally neutrophils and act as antigens forming macromolecule on the cell surface. Binding antibodies to the cells' surface results in the cells being targeted by macrophages for clearance.
Type III immune complex deposition) - This reaction is antigen-antibody complexes are present in the serum. The drug acts as a soluble antigen and binds to drug-specific IgG. The small immune complexes precipitate in various tissues. Examples include blood vessels (vasculitis) Joints(synovitis), renal glomeruli (glomerulonephritis). These immune complexes activate complement, and an inflammatory response ensues. These responses are dose sensitive. The higher the dose of the exposure, the greater the response.
Type IV (T cell-mediated) - The T cells are activated by the complexes directly, other cells can be activated, such as macrophages, eosinophils, or neutrophils. The response is not antibody-mediated. It is a direct cell response this generally is a cutaneous T Cell response as the primed memory effector cells, which react rapidly if immunogenic agents penetrate the skin barrier or reach the skin by diffusing from the circulation. The stimulation of cutaneous T cells may be further facilitated by close contact with various types of HLA expressing dendritic cells in the skin. This reaction is the manifestation of Steven Johnson Syndrome / toxic epidermal necrolysis SJS/TEN, drug reactions with eosinophilia and systemic symptom/ drug-induced hypersensitivity syndrome(DRESS/DIHS) or hepatitis. Type IV has subdivisions based on the P-I or haptens-peptide presentation.[16][17][14]
History and Physical
The patient usually presents with symptoms of rash, swelling of the lips/tongue, or collapsed. The review of the patient’s activity is vital in identifying the cause of the event or symptoms and the time of onset. How the patient treated these symptoms if the symptoms resolved but returned, and if there had been other events. Often patients cannot identify the cause of the symptoms immediately, and input from others present is necessary. In patients presenting with progressive symptoms as listed below on a continuous spectrum, anaphylaxis should be a consideration.
Multisystem involvement:
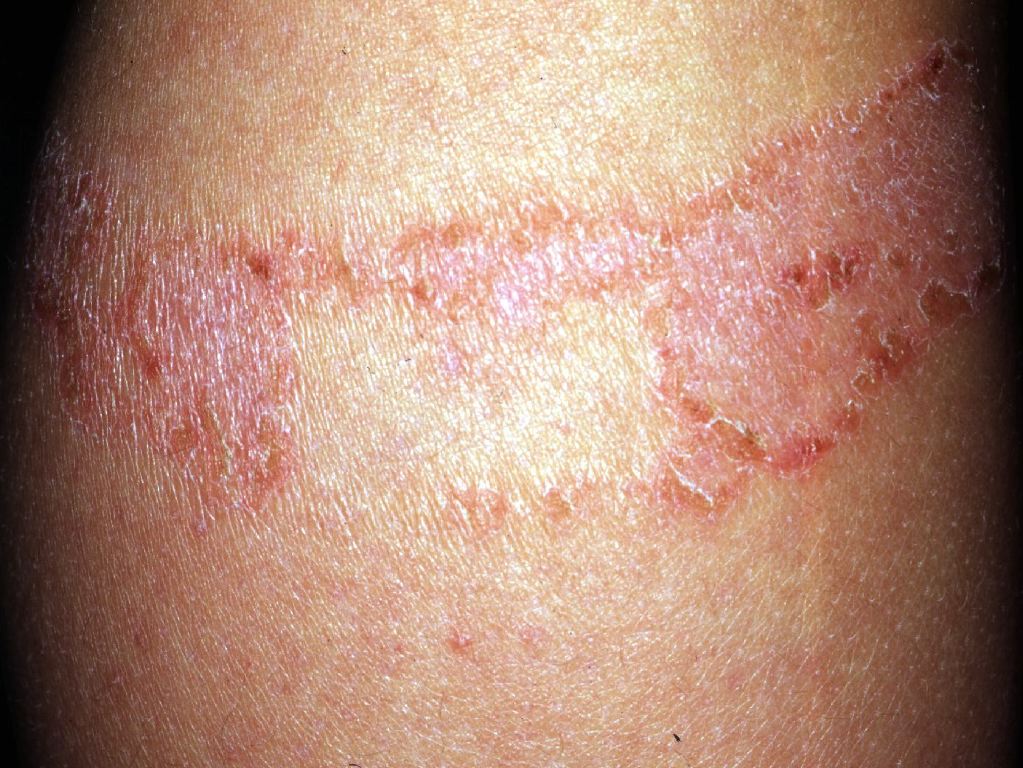
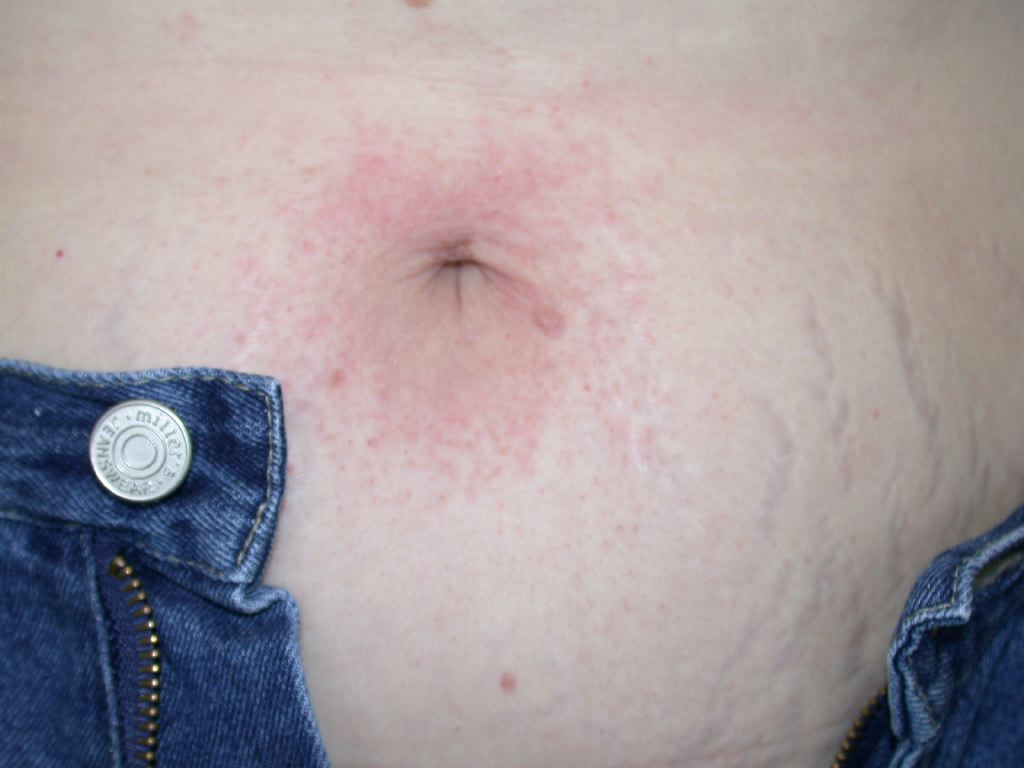
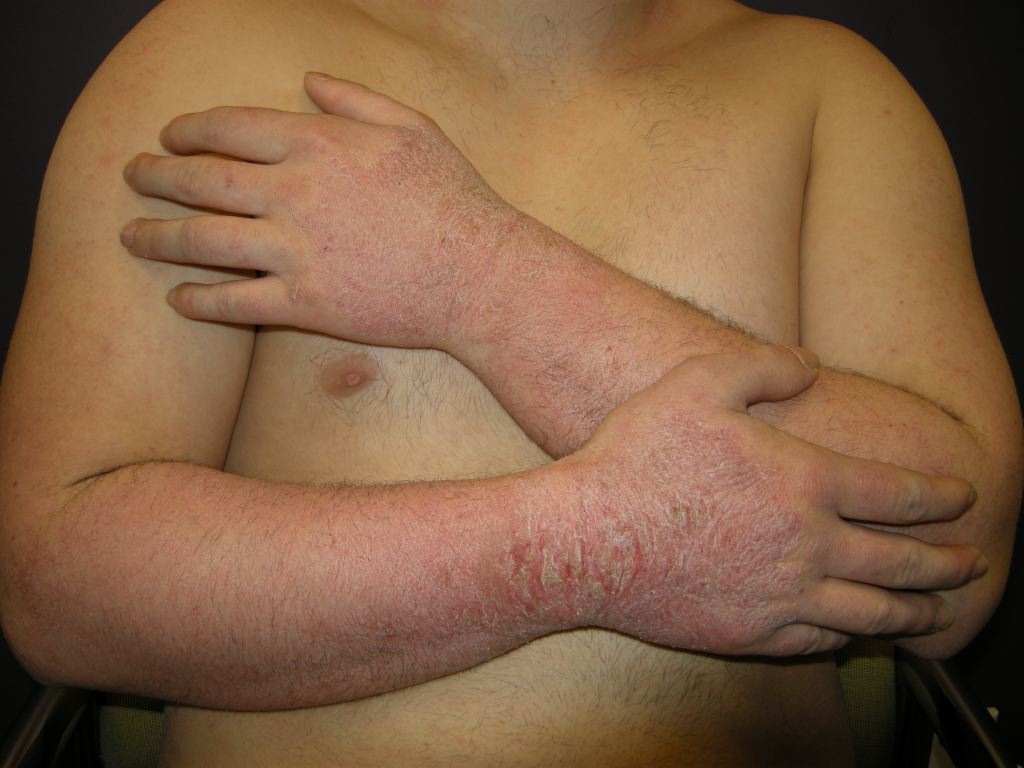
- Skin: (pruritus’, cutaneous flushing, and urticaria),
- Mucosa: (swelling of lips, tongue, conjunctiva, the fullness of the throat or difficulty swallowing),
- Lung/respiratory: (chest tightness, shortness of breath, wheezing, hoarseness, stridor, rhinorrhea),
- Gastrointestinal: (chest spasms with nausea and gaging/ wrenching, vomiting, abdominal cramping, diarrhea),
- Cardiovascular: (tachycardia, with above symptoms, syncope, collapse, hypotension), chest pain, palpitations,
- CNS: dysthymia, altered mental status, apprehension, a sense of impending doom, seizures, headache)
- Ocular: (periorbital itching, erythema, and edema, tearing, conjunctival erythema)
- Urinary or sexual organs: (bladder cramping, uterine cramps)
Children may exhibit behavior changes such as clinging, crying, become irritable, and cease to play. They may exhibit stridor showing laryngeal airway problems. The patients may state they self-treated the itch with over-the-counter antihistamines it went away and now has returned. Prior exposure to the substance is not always necessary, and the patient being on a particular medication with no prior reaction should not mislead the clinician from suspecting the medication as a cause. An example of this is ACE inhibitors producing angioedema.[18][19]
The clinician needs to be aware that anaphylaxis can have presentations of where the symptoms resolve, and then the patient develops a recurrence of symptoms with no additional exposure to the causative agent.; known as biphasic anaphylaxis. The patient can have a protracted anaphylactic reaction that lasts, hours, days, or weeks. Patients can also have delayed reactions from exposures where symptoms do not occur for hours. Reassessment and observation for 4 to 6hours is important as it allows for one to get pertinent history and physical assessment to determine the cause, prognosis, disposition, and needed education for the patient.[20]
Evaluation
Anaphylaxis is a clinical diagnosis. The chemical mediator measurements are not readily available to the clinician. They can retrospectively confirm the allergic reaction and support the diagnosis. Blood cell counts for the measurement of mast cells, and basophil mediators are also helpful if obtained soon after the onset of symptoms. Some suggest that serial tryptase levels be drawn at 15 minutes, 3 hours, 6hours and 24 hours. If elevated at 24 hours, then referral to allergy/immunology specialists for evaluation of possible systemic mastocytosis or a mast cell activation syndrome is recommended. These patients with mast cell disorders can have hypotensive reactions to insect stings even in the absence of immunoglobulin E (IgE)-mediated allergy. Tryptase measurements have been assessed in patients presenting to the emergency department. A level of 12.4 ng/ml had a high specificity of 88 percent and a positive predictive value of (0.93) and low sensitivity of 28 percent and a negative predictive value (0.17). Anaphylaxis patients with hypotension were more likely to have elevated tryptase levels. Another marker is plasma histamine levels, which peak within 5 to 15 minutes of the onset of symptoms and decrease to baseline in 60 minutes; this is because histamine undergoes rapid metabolism by N-methyltransferase and diamine oxidase. The levels do correlate better with anaphylaxis than tryptase levels. As most patients arrive well beyond the 15 to 60 minutes window to emergency departments, measurement of histamine levels is not practical as they will be back to baseline. A 24-hour urine histamine collection started as soon as possible after anaphylaxis can be helpful. Future tests will focus on mature beta-tryptase over total tryptase and alpha tryptase.[21][22][23]
Treatment / Management
Patients can have spontaneous resolution of mild symptoms. Generally, the symptoms progress in severity. Prediction of how severe the reaction can be is not possible. Multiple factors determine severity. Further patients can have biphasic reactions where they have a recurrence of symptoms after resolution with no recurrent exposure. This has been reported in up to 15 percent of children; the reaction can become protracted where it lasts for days, and even weeks. These are instances with delayed hypersensitivity reactions develop anaphylaxis; these reactions occur hours after exposure to the allergen. If patients are untreated in any of these instances, the result can be fatal.[24][25]
Risk factors for severe outcomes include:
1. Asthma, chronic obstructive pulmonary disease (COPD), and interstitial lung disease: Patients with these conditions may have subacute reactions as a result of prescribed antihistamines, and steroids.
2. Cardiac and hypertensive patients, who are on alpha-blockers, beta-blockers, and ACE inhibitors block natural body compensatory mechanisms and require larger doses of epinephrine to treat the anaphylaxis.
Anaphylaxis treatment begins with triage and the removal from exposure, which can involve decontamination if topical agents are involved or clothing is contaminated. Removal of the patient's clothing and standard precautions by staff such as masks, gloves, and gown should take place. Hand washing by staff who may have used latex gloves or eaten peanuts may be necessary. ABC’s (airway, breathing, and circulation) of emergency care should have priority. Patients should have oxygen and intravenous administration of fluids. The patient should receive epinephrine intramuscularly (IM) (1 to 1000 dilution {1 mg/1ml} 0.3cc) 0.3 to 0.5 mg which can be repeated every 5 to 15 minutes as needed. Most patients should respond to 1 to 3 doses if symptoms persist, progress or the patient becomes hypotensive IV epinephrine should be started at 0.1 mcg/kg/minute by infusion device and titrated to maintain perfusion of body organs. Patients on beta-blockers should be given glucagon 1 to 5 mg over 5 minutes. Antiemetics should be given to treat vomiting often associated with glucagon administration. Histamine type 2 receptor blockers such as famotidine 20 mg IV or ranitidine at 50 mg IV should be administered. The glucocorticoid, methylprednisolone 125 mg, should be given.[26]
Weight-base dosing is recommended for pediatric patient populations. IM epinephrine is dosed at 0.01mg/kg and injected in the outer thigh. The maximum dose for children over 50 kg is 0.5 mg; this is done every 5 to 15 minutes for up to three doses if needed until obtaining an adequate response. After three doses, IV administration should begin 0.1 to 1 mcg/kg/minute titrated to effect. IV fluids should be 10 to 20 ml/kg infusion for hypotension and fluid replacement. H1 histamine blockers should be dosed at 1 mg/kg for diphenhydramine up to a maximum of 40 mg. H2 histamine blockers ranitidine is 1 mg/kg up to 50 mg and famotidine at 0.25 mg /kg iv not to exceed 40mg/day for patients 1 to 16 years of age. (If labs show renal dysfunction, consultation with the pharmacy is recommended for dosing based on creatinine clearance in both pediatrics and adults). Glucocorticoid administration methylprednisolone is 1 mg/kg up to a max of 125 mg.[1][26]
Respiratory symptoms of wheezing and bronchospasm can have treatment with aerosolized albuterol dosing for adults is 2.5 mg in 3 ml, and children o.15 mg/kg min dose; this does not affect mucosal edema/angioedema as this is an alpha-receptor control mechanism.
Treatment for patients with refractory hypotension to IV epinephrine should receive methylene blue which inhibits nitric oxide synthase and guanylate cyclase. Ideal dosing is not known. Dosing that has been used in cardiac surgery for treating profound vasodilation is 1 to 2 mg/kg given over 20 to 60 minutes. Other agents are non-adrenergic pressors such as vasopressin for hypotension. Extracorporeal membrane oxygenation is also useful in specialized treatment centers where it is available.[1][26]
Differential Diagnosis
The differential diagnosis of anaphylaxis can include many entities due to its variable presentation. These include vasovagal reactions when presenting with syncope and underlying arrhythmia, seizure, and its association with incontinence. The cardiovascular presentation of hypotension could include myocardial infarction, sepsis, and other causes of shock. The respiratory symptoms can include epiglottis, croup, laryngeal spasm, angioedema acquired and hereditary, foreign body air, and esophageal obstruction. Non-mediated IgE drug reactions, gastrointestinal conditions such as carcinoid with its release of vasoactive polypeptides, and mastocytosis with its systemic release of histamine and other chemotactic substances. The diagnosis is clinical as most patients do not present with isolated symptoms. Specific testing in the emergent setting helps to rule out other causes but should not delay treatment if suspected. Some have suggested testing for tryptase in the instance where one wants to identify a substance as the allergen, but it is not usually available in the emergency department. Tryptase is used to aid in the diagnosis; a normal level does not rule it out. Tryptase gets released from mast cells. It can present as elevated in mastocytosis. It has a higher normal concentration in children also, so it often proves unhelpful.[1]
These tests are generally normal as hypotension will not produce the substances for shock immediately, but as time progresses, it does. Other tests are in development, but as stated earlier, they are not available in most community hospital settings. These tests include variations of tryptase such as beta tryptase, histamines, and other mediators.
The clinician should consider anaphylaxis when:
Unexplained hypotension is present by its self without other explanation non-hypovolemic patients. One needs to consider patient baseline blood pressure.
Patients with unexplained causes of respiratory distress, skin, or gastrointestinal symptoms in combination (20 percent of patients may not have universally recognized symptoms).
The history is not explored sufficiently to look for symptoms of pruritus, flushing, hives, and shortness of breath preceding the patient’s presentation.[27][28]
Patients may be classified under previous terms of anaphylactoid reactions that occur due to the direct, or nonimmunologic release, of the mast and basophil cell mediators; these include contrast-mediated reactions, cold-induced exposure reactions, and exercise reactions.[29]
Foods contain a variety of substances that may not be recognized, such as popsicles containing legumes extracts which can trigger anaphylaxis in patients with peanut or legumes allergies. Thorough history considering all activity preceding presentations from minutes to several hours (up to 24 hours) is essential.[30][31][32]
Patients with psychiatric conditions may not be able to give sufficient information.
Special patient populations such as pregnant, socially disadvantaged (homeless, and low income), elderly even when healthy may be particularly vulnerable to outcomes due to a delayed presentation.[9]
Prognosis
Patients can have a spontaneous resolution from mild symptoms. Generally, the symptoms progress in severity. Prediction of how severe the reaction can be is not possible. Multiple factors can determine severity. Further patients can have biphasic reactions where they have a recurrence of symptoms after resolution with no recurrent exposure, which has been reported in up to 15 percent of children and 21 percent overall; the reaction can become protracted where it lasts for days and even weeks. There are instances with delayed hypersensitivity reactions that develop anaphylaxis' these reactions occur hours after exposure to the allergen. If patients are untreated in any of these instances, the result can be fatal.[9][33]
Risk factors for severe outcomes are patients with asthma, chronic obstructive pulmonary disease, and interstitial lung disease. Patients with these conditions may have subacute reactions if they have received pre-treatment with antihistamines and steroids. Cardiac and hypertensive patients, who are on alpha-blockers, beta-blockers, ACE inhibitors may require larger doses of epinephrine to treat the anaphylaxis.[34]
Complications
Anaphylaxis if unrecognized can result in death in minutes. A series of 164 cases of fatal anaphylaxis showed that the median time interval between onset of symptoms and respiratory or cardiac arrest was 5 minutes in iatrogenic anaphylaxis. The review also showed that the symptoms started within 15 minutes for insect venom stings and 30 minutes for food-induced reactions. Failing to recognize and treat quickly and appropriately with epinephrine leads to cardiac, circulatory, and respiratory compromise. Patients with underlying comorbidities such as heart disease can be at risk for complications from treatment. These patients should receive therapy because the risk of an adverse event from anaphylaxis is just as likely. Preparation for the complications from comorbidities requires anticipation and proper response. If myocardial ischemia occurs from epinephrine, then cardiac care treatment, with a consultation with a cardiologist, will be necessary. Airway protection for cases with severe asthma or chronic obstructive pulmonary disease (COPD) may be required.
Deterrence and Patient Education
Patients should receive education about anaphylaxis and the emergent treatment needed if recurrence happens. If the causative agent or allergen is known, the patient should be informed as to what it was and told to avoid future exposure. The patient should have training in the use of an epinephrine pen injector and the need to report to the emergency department as soon as possible after exposure. The patient should be made aware of early signs and symptoms of anaphylaxis itching, redness of the skin, hives, runny nose, and advance symptoms trouble breathing, wheezing, vomiting, swelling of the throat and esophagus, diarrhea, and feeling dizzy passing out. The patient may obtain a referral to an allergist/immunologist for further evaluation and treatment. Patients with high sensitivities such as the peanut or legume allergies need education on reading labels of food products. They should recommend allergy bracelets/rescue kits to patients with severe events. The rescue kit usually contains an epinephrine injector device and oral or injectable antihistamine.[35]
Pearls and Other Issues
The symptoms are pruritus, flushing, rash, urticaria, swelling of the lips, tongue, and airway, (angioedema), nausea, vomiting, abdominal cramping, shortness of breath, wheezing and bronchospasm, stridor, syncope, collapse, and progressive to hypotension which can be profound.[32][36]
The reactions are general IgE mediated.
The recognition of the condition needs to be early and treatment aggressive.
The drug treatment begins with epinephrine, if not hypotensive then progresses to IV in persistent, refractory, or progressive cases. Adjunctive therapies include H1 and H2 blocking agents like diphenhydramine and ranitidine; Glucocorticoids are also useful.
Special considerations for patient’s comorbidities need to be considered, such as the use of glucagon for beta-blocker toxicity and antiemetics for gastrointestinal symptoms.[37]
Treatments for those refractory cases include methylene blue, vasopressin, and extracorporeal membrane oxygenation.
Patients should receive an emergency action plan for when exposure or anaphylactic symptoms develop. This plan includes an epinephrine pen dispenser and activation of emergency medical services for transport to the hospital.
Education of the patient about lifestyle changes to avoid exposures is vital. Referral to an allergist for immune therapy and identification of possible allergens is indicated in patients with severe anaphylaxis and high risk for recurrence.[38]
Enhancing Healthcare Team Outcomes
The clinician should maintain a high index of suspicion of anaphylaxis and not hesitate to treat the patient presenting with suspected allergic reaction with epinephrine. Remember, hypotension or shock need not be present. The signs of two or more organ systems or one system with severe compromise need only be present. Noting early signs and symptoms is key to preventing complications.[33] The treatment of anaphylaxis can be complicated by patients on medications such as beta-blockers. The blood pressure specific for age should be known, especially for children and infants. The health care team (nurse practitioner, allergist, anesthesiologist, pulmonologist) need to realize patients may not always have the capacity to describe their symptoms of respiratory distress, especially when sedated. Skin lesions are absent up to 20 percent of all episodes, and one needs to be aware that a patient with a history of asthma or bronchospasm may be having anaphylaxis. Patient populations such as psychiatric, neurologic, and substance misusers may appear to present with side effects of medications or recreational drugs when it is an allergic reaction/anaphylaxis to a contaminant. Thus reassessment by health personnel is important. Having ancillary staff available to assist with airways such as respiratory, anesthesia, or a surgeon is helpful in case one needs a surgical airway due to upper airway angioedema. Educating the staff regarding recognition of anaphylaxis and prompt treatment is important in preventing adverse outcomes and under treatment.[39][40]
Given the potential lethality of anaphylaxis, all members of the health care team in addition to physicians, need to be aware and trained to recognize the symptoms and react accordingly. Nurses are often the first personnel to see the patient in the ED and may be called upon to assist with intubation in severe cases, as well as administering medication. They also need to be able to recognize adverse reactions to administered therapy and react appropriately, as well as informing the physician. Pharmacists need to verify all dosing quickly and accurately, particularly in pediatric cases with weight-based dosing and intervene if noting any anomalies. They also are invaluable resources for medication reconciliation and informing the team of adverse reactions to medications the patient may already be taking, such as beta-blockers. Only through interprofessional team collaboration between physicians, specialists, nursing, and pharmacists can outcomes be driven to their optimal result for patients. [Level V]