Continuing Education Activity
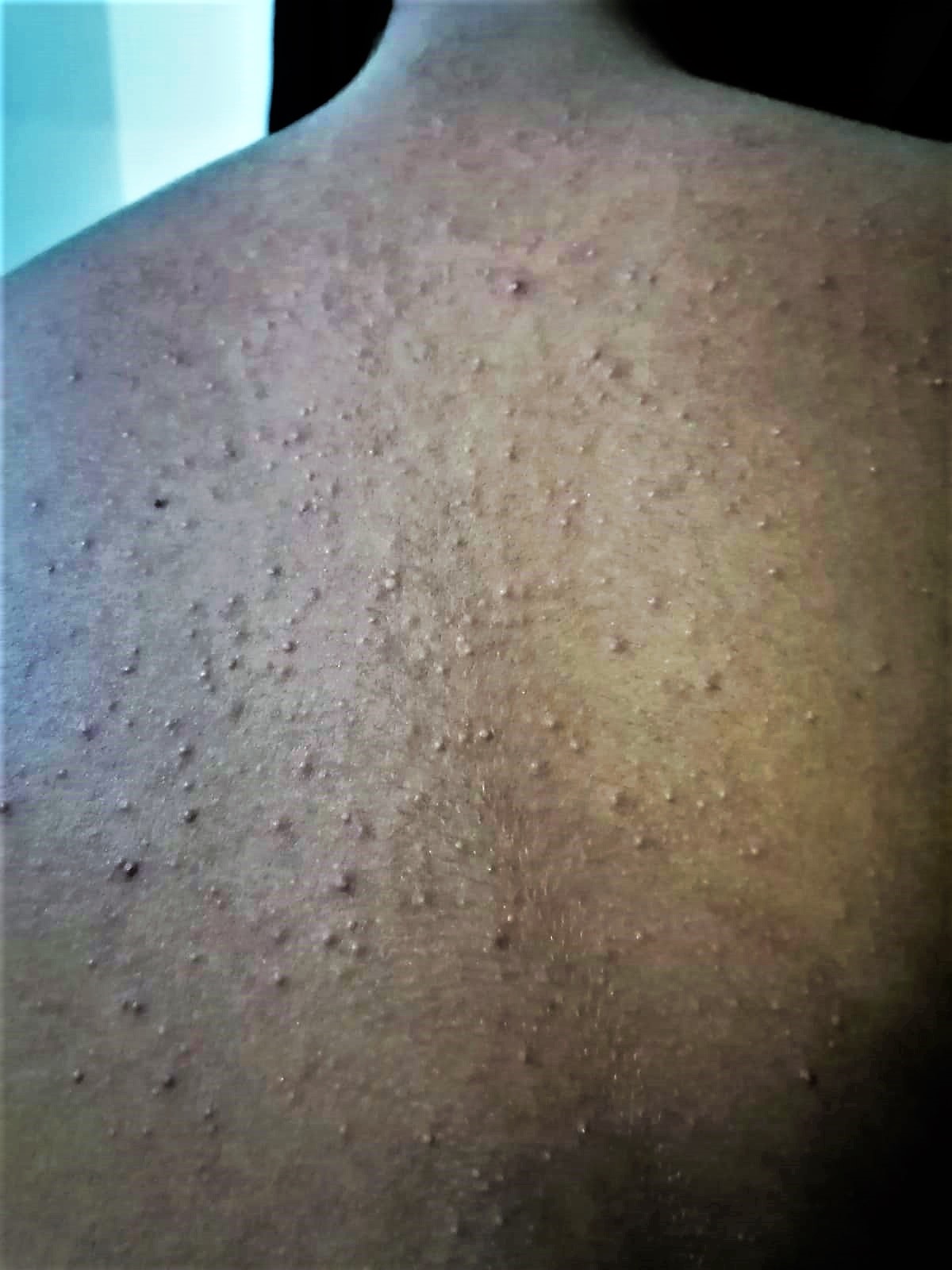
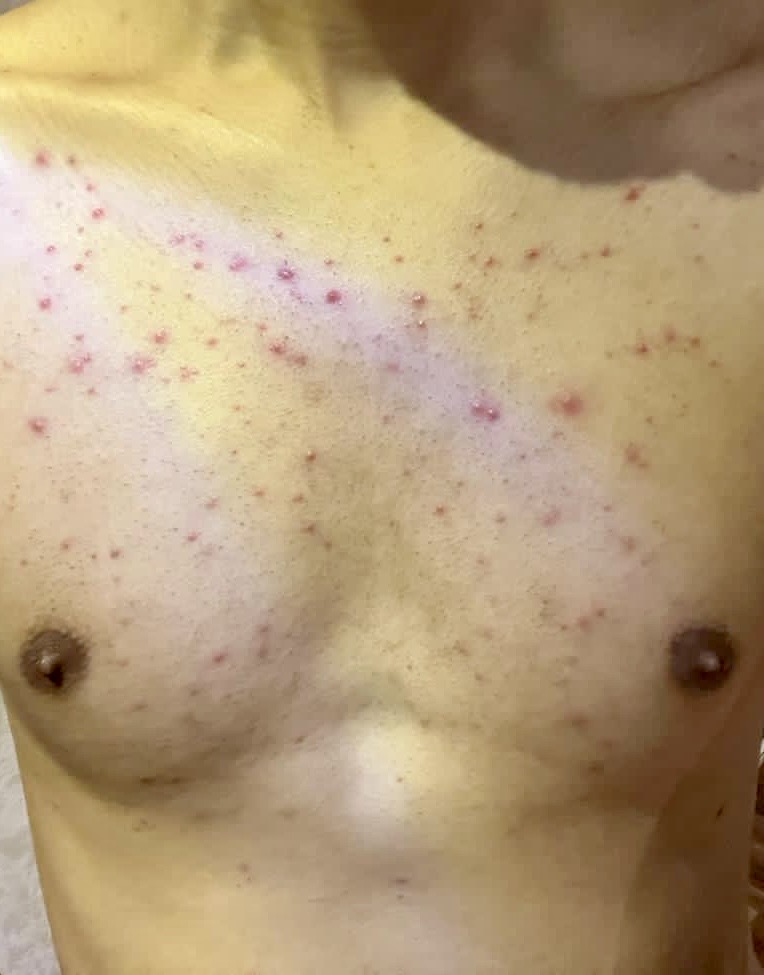
Acneiform eruptions are acne vulgaris-like dermatoses. There are papulopustular, nodular, and cystic lesions. Acne vulgaris is characterized by comedones, whereas acneiform eruptions clinically lack comedones. Acneiform eruptions demonstrate an acute onset and can affect any age group. Distinguishing between acne-like dermatoses and real acne can be difficult in clinical settings. Acneiform eruptions can display papules, pustules, nodules, and cysts, just like acne. Unlike acne, comedones are infrequent but can be seen in specific forms of acneiform eruptions.
Additionally, the sudden onset, propensity to affect people of all ages, uniformity of lesions, and dispersion outside the seborrheic regions distinguish acneiform eruptions from acne. Medications, hormonal and metabolic abnormalities, drug reactions, or genetic disorders may cause acneiform eruptions. In most cases, the diagnosis is clinical, but when there is doubt, one may obtain a biopsy or culture of any discharge. Withdrawal of the suspected medication is another way to make the diagnosis. The treatment of acneiform eruptions depends on the cause. This activity for healthcare professionals is designed to enhance the learner's competence when managing acneiform eruptions, equipping them with updated knowledge, skills, and strategies for timely identification, effective interventions, and improved coordination of care, leading to better patient outcomes.
Objectives:
Identify some of the etiologic factors that can contribute to the development of acneiform eruptions.
Differentiate acneiform eruptions from acne vulgaris.
Implement the treatment strategies for patients with acneiform eruptions.
Outline the role of a collaborative interprofessional team in improving the evaluation, management, and counseling for patients with acneiform eruptions.
Introduction
Acneiform eruptions are a group of disorders characterized by papules and pustules resembling acne vulgaris.[1][2] Distinguishing between acne-like dermatoses and real acne can be difficult in clinical settings. Acneiform eruptions can display papules, pustules, nodules, and cysts, just like acne. Unlike acne, comedones are infrequent but can be seen in specific forms of acneiform eruptions. Additionally, the sudden onset, propensity to affect people of all ages, uniformity of lesions, and dispersion outside the seborrheic regions distinguish acneiform eruptions from acne. Medications, hormonal and metabolic abnormalities, drug reactions, or genetic disorders may cause acneiform eruptions. In most cases, the diagnosis is clinical, but when there is doubt, one may obtain a biopsy or culture of any discharge. Withdrawal of the suspected medication is another way to make the diagnosis. The treatment of acneiform eruptions depends on the cause. Clinicians frequently erroneously treat patients for acne and exacerbate the condition.[1]
Etiology
Acneiform eruptions can develop due to infections, hormonal or metabolic abnormalities, genetic disorders, drug reactions, chemical contact, or friction and pressure.[3][4] Prolonged and increased excretion of causative substances might irritate the follicular epithelium and produce an inflammatory reaction. There are many causes for acneiform eruptions, including exposure to halogenated aromatic hydrocarbons and the use of antibiotics like macrolides and penicillin. Other drugs that induce acneiform eruptions include nystatin, isoniazid, corticotropin, naproxen, and hydroxychloroquine. Many organisms, like Proteus, Klebsiella, Escherichia coli, and Enterobacter infections, can also induce acneiform eruptions. Pityrosporum folliculitis, caused by Malassezia furfur, may also present on the trunk and upper extremities with pruritic eruptions. Infections that are known to cause acneiform eruptions include secondary syphilis, mycotic infections, cutaneous coccidioidomycosis, and Sporothrix schenckii.
Pathophysiology
The etiology of acneiform eruptions is multifactorial, with no singular underlying mechanism implicated. However, patient age, infections, occupation, habits, cosmetics, and medications may all contribute to the development of these eruptions. Because the observed lesions might not respond to conventional acne treatment, treatment approaches should be customized based on the identified causative agents. The following etiologies are common causes of acneiform eruptions.
Drug-induced Acne
This acne can occur due to several medications including corticosteroids, anticonvulsants (eg, phenytoin), antidepressants, antipsychotics (eg, olanzapine and lithium), antituberculosis drugs (eg, INH, thiourea, thiouracil, disulfiram, and corticotropin), antifungals (eg, nystatin and itraconazole), hydroxychloroquine, naproxen, mercury, amineptine, and chemotherapy. Acneiform eruptions are most frequently reported in individuals undergoing treatment with epidermal growth factor receptor inhibitors and mitogen-activated protein kinase inhibitors.[6] Antibiotics (eg, penicillins and macrolides) cause acute generalized pustular eruptions without comedones, and patients are often febrile with leukocytosis. Other antibiotic causes include co-trimoxazole, doxycycline, ofloxacin, and chloramphenicol. Acneiform eruption was found to be an adverse event associated with the recently approved 3 cystic fibrosis transmembrane conductance modulators (ie, elexacaftor, tezacaftor, and ivacaftor).[7] Compared to other cancer treatments, acneiform eruptions are less frequently observed with CTLA-4 inhibitors. However, healthcare professionals should know that this side effect may still occur in clinical practice.[8] There have been few reports in the literature regarding acneiform outbreaks caused by vitamin B12, with more cases reported in females than males. Possible causative variables of acneiform eruptions were postulated to include high-dose supplementation, prolonged periods of supplementing, or the concurrent use of vitamin B12 with vitamins B1, B2, or B6.[9][10][11]
Steroid acne presents as monomorphous papulopustules located mainly on the trunk and extremities, with less face involvement. Characteristically, lesions appear after the administration of systemic corticosteroids. Topical corticosteroids may also cause acneiform eruption over the skin under which the topical preparation is applied or around the nose or mouth in the case of inhaled steroids. This eruption typically presents as skin erythema along the distribution of corticosteroid application with pustules and inflamed papules. Ultimately, the lesions resolve once the corticosteroid is discontinued; however, prolonged and severe flares may result from "steroid dependency" after withdrawal. Athletes and bodybuilders ought to be questioned regarding their use of anabolic steroids.
Occupational Acne, Acne Cosmetica, and Pomade Acne
Occupational acne is caused by contact with insoluble, follicle-occluding substances in the place of employment. Among the harmful substances are derivatives of coal tar, cutting oils, petroleum-based products, and chlorinated aromatic hydrocarbons. The clinical presentation primarily consists of comedones, although a few papules, pustules, and cystic lesions may be dispersed throughout exposed and normally covered regions. Facial acne that is predominantly comedonal, characterized by closed comedones, may also manifest in areas consistently exposed to hair products or follicle-occluding cosmetics (ie, acne cosmetica). The latter condition, pomade acne, is more prevalent on the forehead and temples.[12]
Chloracne
Chloracne formation is the result of halogenated aromatic hydrocarbon exposure. Typically, the onset of symptoms occurs multiple weeks following systemic exposure, which may occur through ingestion, percutaneous absorption, or inhalation. Insecticides, fungicides, herbicides, electrical conductors and insulators, polychlorinated naphthalenes and biphenyls, tetrachloroazobenzene, and tetrachloroazoxybenzene have all been implicated. Additionally, dibenzofurans, dibenzodioxins, polybrominated naphthalenes, and biphenyls have been identified. Comedo-like lesions and yellowish cysts, characterized by minimal inflammation, predominantly manifest in the retroauricular and malar regions of the head and neck, axillae, and scrotum. To varying degrees, the extremities, buttocks, and trunk are implicated. Significant scarring may accompany the healing of cystic lesions, and the condition may persist for years after exposure has ceased. Further observations might include hypertrichosis and a grayish discoloration of the skin.[13]
Acne Mechanica
Acne mechanica is caused by repetitive frictional and mechanical obstruction of the pilosebaceous orifice, resulting in comedo formation. Robust mechanical factors thoroughly described include chin straps, suspenders, helmets, and collars. Acne mechanica caused by orthopedic factors consists of eruptions in the axillae secondary to the use of crutches and amputee stumps due to friction from prostheses. A typical instance of acne mechanica is fiddler's neck, characterized by a distinct, hyperpigmented plaque that is lichenified and interspersed with comedones, resulting from repeated trauma caused by the positioning of a violin on the lateral neck. The primary clinical feature of acne mechanica is the geometrically distributed eruptions and linear areas of involvement.
Tropical Acne
Tropical acne is an acneiform follicular eruption caused by prolonged exposure to extremely high temperatures. This may manifest in tropical regions or due to working in extremely hot environments, such as among furnace workers. Tropical acne has historically resulted in substantial morbidity among troops. Manifestations often include trunk and pelvic involvement in nodulocystic acne that is significantly inflamed; secondary staphylococcal infection is a common complication.
Radiation Acne
Radiation acne is identified by comedo-like papules that develop in areas previously exposed to therapeutic ionizing radiation.[14] The lesions manifest as the acute phase of radiation dermatitis begins to subside. The ionizing rays induce epithelial metaplasia within the follicle, creating adherent hyperkeratotic plugs resistant to expression.[15]
Pseudoacne of the Nasal Crease
The transverse nasal crease is a horizontal line located in the lower part of the nose, marking the boundary between the alar cartilage and the triangular cartilage. Milia, cysts, and comedones can be found in a row along this fold. These acne-like lesions, or pseudoacne, are not influenced by hormones and develop in childhood shortly before puberty begins.
Idiopathic Facial Aseptic Granuloma
Idiopathic facial aseptic granuloma is a painless nodule that resembles acne and usually forms on the cheeks of young children, with an average age of 3.5 years. Multiple lesions are infrequent. The histopathologic examination shows the presence of a lymphohistiocytic infiltration in the dermis, characterized by the presence of foreign body-type giant cells. Cultures are usually negative, and the lesions are unresponsive to antibiotic treatment. Typically, within a year, the lesions resolve spontaneously. Idiopathic facial aseptic granuloma has been suggested to be a type of childhood rosacea, as more than 40% of children exhibit at least 2 other clinical indications of rosacea (eg, recurring chalazions, facial flushing, telangiectasias, or papulopustules).
Childhood Flexural Comedones
This condition is identified by distinct, double-opening comedones found specifically in the axillae and, less frequently, in the groin area. Most patients exhibit a solitary lesion, and the average age of diagnosis is 6 years, with an equal prevalence among boys and girls. The condition may also be familial. No association with hidradenitis suppurativa, acne vulgaris, or precocious puberty has been identified.[16]
Treatment / Management
The treatment of acneiform eruptions is tailored to the underlying etiology. Exposure should be discontinued for acneiform eruptions due to organisms or medications. Minimizing contacts or friction will prevent occupational and mechanical acne. Protective clothing and the removal of the worker from unsuitable environments also help.[20] The traditional agents used to treat acne vulgaris seldom work in patients with acneiform eruptions, but using skin cleaners like salicylic acid or benzoyl peroxide to reduce oily skin may be suggested. Itching is a prevalent symptom in patients with acneiform eruptions so that these patients may benefit from the use of antihistamines. For nocturnal itching, first-generation antihistamines are recommended because they also induce sleep.
Over the years, the use of retinoids to treat acneiform eruptions has increased due to successful treatment. Both oral and topical retinoids have been used. These agents are known to decrease sebum production and rapidly resolve eruptions. These agents should not be prescribed to women of childbearing age because of their teratogenic potential. Some cases of acneiform eruptions may benefit from dapsone, as anecdotal reports have demonstrated that eosinophilic pustular eruptions have responded to a short course of dapsone.[21] Patients who have gram-positive organisms causing skin lesions may also benefit from doxycycline.
Oral tetracycline antibiotics are the most effective preventive treatment for acne-like skin rashes caused by EGFR inhibitors. These should be provided to appropriate individuals at the start of therapy and utilized with a comprehensive skincare regimen that includes moisturizers and the avoidance of irritants.[22] For fungal infections (eg, Pityrosporum folliculitis), topical antifungal agents such as ciclopirox, econazole, and ketoconazole can be helpful. Acneiform eruptions secondary to chloracne treatment are difficult as they may persist for years, even without further exposure. Some patients with eosinophilic pustular folliculitis may benefit from a short course of oral indomethacin. Lesions that fail to respond to indomethacin may be treated with cyclosporine.
Enhancing Healthcare Team Outcomes
Nurse practitioners, pharmacists, and primary care clinicians must know that not all facial lesions are due to acne. Acneiform eruptions have many causes and, in many cases, are caused by occupational exposure or certain medications. Erroneously treating these patients for acne often exacerbates the condition. Consult with a dermatologist is recommended for uncertain diagnoses. Clinicians should educate the public that acneiform eruptions are transient skin disorders with many causes. In many cases, simply removing the offending agent or limiting exposure to the organism can resolve the disorder. The prognosis for most patients is excellent, and there is usually no residual scarring. Patients should be warned not to scratch the lesions, which can lead to scars and keloid formation.