Continuing Education Activity
Acne vulgaris is a chronic inflammatory disorder affecting the pilosebaceous unit, typically following a prolonged course. It is commonly triggered during adolescence by Cutibacterium acnes, a bacterial species, under the influence of normal circulating levels of dehydroepiandrosterone. This common skin disorder that can present with both inflammatory and non-inflammatory lesions. This activity aims to examine the causes, assessment, and treatment of acne vulgaris, emphasizing the importance of the interprofessional team in providing comprehensive care for patients affected by this condition.
Objectives:
- Identify the various types and severity levels of acne vulgaris through visual examination and patient history.
- Implement evidence-based treatment protocols for acne vulgaris, including topical and systemic therapies, according to individual patient needs.
- Communicate effectively with patients about the causes, triggers, and potential complications associated with acne vulgaris, as well as the importance of adherence to treatment plans.
- Collaborate with the interprofessional team to develop comprehensive treatment strategies and follow-up care for patients with severe or treatment-resistant acne vulgaris.
Introduction
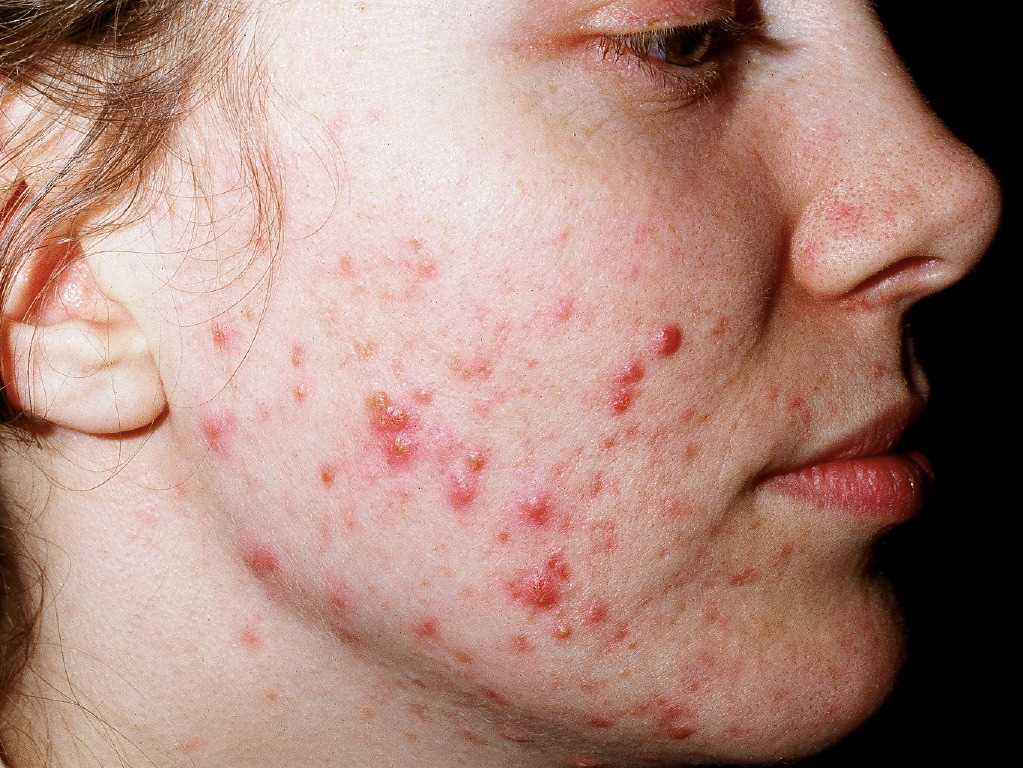
Acne vulgaris is a common cutaneous inflammatory disorder of the pilosebaceous unit, which runs a chronic course. The condition commonly manifests with papules, pustules, or nodules primarily on the face, although it can also affect the upper arms, trunk, and back. The pathogenesis of acne vulgaris involves the interaction of multiple factors that ultimately lead to the formation of its primary lesion, which is known as "comedo" (see Image. Acne Vulgaris). Although acne vulgaris is commonly observed among adolescents, it is not restricted to this age group and can affect individuals of various ages. The severity of this condition can vary, ranging from a mild presentation with only a few comedones to more severe forms characterized by disfiguring inflammatory manifestations, which can lead to hyperpigmentation, scarring, and adverse psychological effects.[1][2][3]
Etiology
Acne develops as a result of hypersensitivity of the sebaceous glands to normal levels of circulating androgens. This process is further exacerbated by the presence of Cutibacterium acnes (C acnes), a bacterial species, and subsequent inflammation.[4]
Proposed contributory factors for acne include:
- Use of medications such as lithium, steroids, and anticonvulsants.
- Exposure to excess sunlight.
- Use of occlusive wear, such as shoulder pads, headbands, backpacks, and underwire brassieres.
- Oil-based cosmetics and facial massage.
- Endocrine disorders, such as polycystic ovarian syndrome, and even pregnancy. A premenstrual flare-up in acne seems to follow edema of the pilosebaceous duct. This occurs in 70% of female patients.
- Genetic factors significantly influence the proportion of branched fatty acids found in sebum, with heritability estimates ranging from 50% to 90%.
- Repetitive mechanical trauma resulting from scrubbing affected skin with soaps and detergents.[5]
- Several studies have indicated that increased milk consumption and high glycemic load diets are associated with acne in adolescence. This could be attributed to the rich constituents of insulin-like growth factor (IGF) and natural hormonal components of milk.[6][7][8][9] However, no substantial evidence supports the common assumption that chocolate exacerbates acne.[10]
- Psychological stress is associated with increased acne severity, probably by stimulating stress hormones.[11][12]
- Insulin resistance may also have a significant role in acne, as individuals with insulin resistance have increased levels of IGF, which is linked to increased facial sebum excretion.[13] However, the association between body mass index and acne vulgaris is poorly understood, with contradictory results reported in various studies.[14][15]
Epidemiology
Acne vulgaris is commonly observed in adolescents and young adults. Its prevalence rates are estimated to range from 35% to over 90% among adolescents.[16] The natural course of this disease can commence as early as ages 7-12 (preadolescent acne) and resolve by the third decade of an individual's life. However, there are instances where acne can persist into adulthood or even develop for the first time during adulthood.
Adolescent acne is more common in males than in females. On the contrary, postadolescent acne predominantly affects females. Urban populations tend to be more affected by acne vulgaris than rural populations. Approximately 20% of the affected individuals develop severe acne, which results in scarring. Some evidence suggests that certain racial and ethnic groups may experience variations in the severity and prevalence of acne vulgaris. Asians and Africans are more likely to develop severe forms of acne. Whereas mild acne is more commonly seen in the White population. In general, people with darker skin also tend to develop hyperpigmentation.[17]
Acne can occasionally develop in neonates, but it tends to resolve independently in most cases without any specific treatment. Infantile acne, another variant of acne vulgaris, may begin in infancy. Acne that develops in children aged 1 to 6 is rare. However, it could be a sign of an underlying condition requiring additional evaluation.[18]
Pathophysiology
The pathogenesis of acne vulgaris involves the interaction of several host factors, including the stimulation of sebaceous glands by circulating androgens, dysbiosis of the pilosebaceous follicle microbiome, and cellular immune responses. In addition, other factors such as genetics and diet may also influence the development and progression of the disease. The microcomedo serves as the primary lesion and is the precursor for all clinical manifestations of acne vulgaris. It is characterized by a small, hyperkeratotic plug primarily composed of corneocytes and located in the lower region of the follicular infundibulum. Microcomedones gradually evolve and develop into other acne lesions, which include closed comedones (whiteheads), open comedones (blackheads), and inflammatory papules, pustules, and nodules. The progression of microcomedones into other types of acne lesions has been theorized to involve the following 4 primary pathogenic events:
- Increased sebum production (seborrhea)
- Follicular hyperkeratinization
- C acnes, formerly, Propionibacterium acnes (An anaerobic diphtheroid that naturally exists as part of the skin flora.)
- Inflammation
The gradual accumulation of keratinous material and sebum converts a micro comedo into a closed comedo. Through continuous distension, the follicular orifice gradually expands, resulting in the formation of an open comedo. Oxidized lipids and melanin within the comedo contribute to its characteristic dark black color. C acnes and its antagonizing cellular immune responses contribute to the development of inflammatory pustules and papules. Eventually, follicles rupture with the release of bacteria, keratin, and proinflammatory lipids into the surrounding dermis, exacerbating the inflammation with subsequent nodule formation.[19]
Role of Androgens
Most patients with acne vulgaris typically have normal androgen levels in their body. However, in certain conditions such as congenital adrenal hyperplasia, polycystic ovarian syndrome, and adrenal or ovarian tumors, excessive androgen production is produced in the body, ultimately leading to acne. This observation supports the significance of androgens in the development of acne. Furthermore, acne does not typically develop before an individual reaches adrenarche, which is the stage when levels of dehydroepiandrosterone sulfate (DHEAS), an adrenal androgen precursor, are high. However, there is an exception in infantile acne, a condition resulting from excessive androgen production by immature adrenal glands or gonads. Furthermore, it is noteworthy that individuals with androgen insensitivity, specifically men, do not experience the development of acne.[20]
The role of androgens in the development of acne involves various mechanisms, as listed below:
- The adrenal glands and the gonads secrete androgens.
- Sebaceous glands can also synthesize androgens through the conversion of DHEAS to testosterone via the action of several enzymes.
- Type I 5-alpha reductase in the sebaceous gland converts testosterone to 5-alpha-dihydrotestosterone (DHT).
- Sebaceous glands and the outer root sheath keratinocytes of the follicular epithelium have androgen receptors that bind DHT and testosterone. However, DHT has a greater affinity for these receptors than testosterone.
- Androgens stimulate sebaceous glands' growth and secretory function, leading to seborrhea and acne formation.
- Seborrhea provides a growth medium for C acnes from which they hydrolyze triglycerides in sebum, as a nutrient source, into free fatty acids and glycerol.
- The resulting anaerobic lipid-rich environment allows C acnes to thrive.
Role of C acnes
C acnes is widely considered a prominent commensal bacterium within the microbiome of the pilosebaceous follicles. The presence of C acnes can trigger both innate and adaptive immune responses, thereby contributing to the inflammatory responses observed in acne.[21] The population of C acnes can be categorized into 3 major divisions. One of these divisions, which includes an epidemic clone known as phylotype IA, is significantly associated with moderate-to-severe acne. The other 2 divisions, phylotypes II and III, are associated with normal skin health and opportunistic infections.[22]
The development of acne involves several factors associated with C acnes and the immune response as listed below:
-
The acne-associated strains of C acnes have been found to possess a heightened capacity to stimulate the pro-inflammatory cascade, specifically involving TH17 cells. These TH17 cells secrete cytokines such as interferon (IFN)-gamma and interleukin (IL)-17, which promote inflammation. In contrast, the strains associated with healthy skin have been shown to stimulate TH17 cells to produce the anti-inflammatory cytokine IL-10.[23]
-
Antibiotic resistance in acne has been linked to acne-associated strains of C acnes, which could form biofilms within the follicles.[24][25]
-
C acnes stimulate the innate immune response to produce IL-1 by activating the nod-like receptor P3 (NLRP3) inflammasome in human sebocytes and monocytes.[26][27]
-
It activates Toll-like receptor-2 on perifollicular macrophages, which triggers the release of more pro-inflammatory cytokines such as IL-8 and IL-12. These cytokines attract neutrophils that release neutrophil lysosomal enzymes that contribute to follicular rupture.
-
The pathogenicity of specific strains of C acnes, along with the variations in the host's inflammatory responses to the strains colonizing the skin, may contribute to the diversity observed in the prevalence and severity of acne.[28]
Role of Genetics
Genetics plays a substantial role in the development of acne, as mentioned below:
- Numerous studies have provided evidence supporting the genetic component of acne. Individuals with affected first-degree family members have a risk of developing acne that can be as high as 3 times greater compared to individuals without a family history of the condition.[15][29]
- Gene expression studies demonstrated the upregulation of matrix metalloproteinases 1 and 3, inflammatory cytokines (IL-8), and antimicrobial peptides (human beta-defensin 4 and granzyme B) in inflammatory acne lesions.[30]
- Compared to control samples, a significant increase in beta-defensin 2 immunoreactivity in the lesional and perilesional epithelium of acne, as observed in acne biopsies, occur. In addition, a relatively lesser increase in beta-defensin 1 immunoreactivity is observed.[31]
Histopathology
A dilated follicle can be observed with a keratin plug in typical acne lesions. In more advanced cases, the dilated follicle can lead to the formation of an open comedo. When the thin wall of a follicle ruptures, it can lead to the presence of bacteria and signs of inflammation within the surrounding area. In cases where large acne lesions are subjected to trauma, they can develop fibrosis and scarring as part of the healing process.
History and Physical
Acne occurs on the affected individuals' face, neck, chest, upper back, and upper arm areas, where large, hormonally responsive sebaceous glands are abundant. Acne presents as a variety of polymorphic lesions from grade 1 to grade 4, starting with comedones, as listed below:
- Grade 1: Also known as "comedones," and is categorized into two types, open and closed. Open comedones form when the pilosebaceous orifice becomes plugged with sebum and appears as papules with a central, dilated follicular orifice containing gray, brown, or black keratotic material. On the other hand, closed comedones form when keratin and sebum block the pilosebaceous orifice beneath the skin surface. They appear as dome-shaped, smooth papules that can be skin-colored, whitish, or grayish in appearance.
- Grade 2: Inflammatory lesions present as a small papule with erythema.
- Grade 3: Pustules.
- Grade 4: Many pustules coalesce to form nodules and cysts called nodulocystic acne.
The assessment of acne severity depends on multiple factors. The features that must be considered for a comprehensive evaluation of acne severity include the psychological impact of acne on the patient, clinical type of lesions, scarring, draining lesions, or sinus tracts, as well as the patient's response to treatment. Patients diagnosed with nodular inflammatory acne are classified as having severe acne. Similarly, individuals with inflammatory pustules and pustules accompanied by scarring, even in the absence of nodules, are also considered to have severe acne.[32]
The extent of skin involvement in acne varies greatly, ranging from a few small comedones to many inflamed nodules. Certain presentations are affected by the patient's characteristics. Young adolescents often present with comedones involving the forehead, nose, and chin (T-zone). As acne progresses, adolescents may develop inflammatory lesions in addition to comedones. It is common for adult women to experience acne, primarily on the lower face and neck, and these flare-ups are often associated with their menstrual cycles.[33]
Acne can leave various scars after healing, which may present as depressed scars or hypertrophic and keloidal scars. Depressed scars are either oval craters (boxcar scars), deep pits (ice-pick scars), or pits with sloped sides (rolling scars). The underlying reasons why some patients develop distressing scars from acne while others do not are still not fully understood. Acne is commonly associated with seborrhea. In cases where acne is associated with hyperandrogenism, additional symptoms may be present, such as hirsutism, acanthosis nigricans, irregular menstrual periods, and weight gain. Similar to other inflammatory skin conditions, acne vulgaris lesions may lead to the development of postinflammatory hyperpigmentation, which is more common in individuals with darker skin (phototypes IV to VI).
Some variants of acne vulgaris include:
- Acne conglobata: Acne conglobata is a rare but severe form of nodulocystic acne in young males. It usually presents with tender, disfiguring, double- or triple-interconnecting comedones, cysts, inflammatory nodules, and deep burrowing abscesses on the face, shoulders, back, chest, upper arms, buttocks, and thighs. Systemic symptoms are usually absent.
- Acne fulminans or acne maligna: Acne fulminans or acne maligna is a rare skin disorder presenting as an acute, painful, ulcerating, and hemorrhagic clinical form of acne. It may or may not be associated with systemic symptoms such as fever and polyarthritis. Acne fulminans also may cause bone lesions and laboratory abnormalities.
- Acne excoriée: Acne excoriée is a condition often seen in young women with an underlying psychiatric disorder. It presents with mild acne, including comedones, that are obsessively picked and excoriated, leading to scarring.
- Infantile acne: Infantile acne often commences between the ages of 3 and 6 months due to increased androgens produced by the immature adrenal gland in girls and the immature adrenal gland and testes in boys. Androgen levels revert to normal by the time a child attains the age of 1 or 2, with subsequent improvement in acne.
Acne vulgaris can be associated with certain rare syndromes, including:
- SAPHO syndrome (synovitis, acne, pustulosis, hyperostosis, and osteitis) with features of inflammatory arthritis or osteitis, particularly of the anterior chest wall.
- PAPA syndrome (sterile pyogenic arthritis, pyoderma gangrenosum, and acne).
Based on the natural history of the disease, its variants, and rare syndromes, comprehensive data on the patient's history should be collected, which include the following elements: age of onset and current age, medical history, medication history, family history of acne, menstrual history in females (associated with acne flares), signs of virilization in young children and females (hirsutism, male pattern hair loss, deepening of voice, or genital enlargement), systemic symptoms (including fever, myalgia, and arthralgia) especially in severe acne, skincare routine (use of comedogenic products), prior treatments and response, and psychological impact of the disease.
Skin examination should include an assessment of the lesion type and distribution. Lesions can be categorized as monomorphic, indicating drug-induced acne or pityrosporum folliculitis, or polymorphic, which coincides with the diagnosis of acne. It is also essential to look for signs of hyperandrogenism in females and young children (such as male pattern hair loss or hirsutism), postinflammatory hyperpigmentation, and scarring.
Evaluation
Acne vulgaris is typically diagnosed based on physical examination rather than laboratory tests. Laboratory or radiological tests are required for patients when their clinical evaluation indicates the presence of underlying hyperandrogenism or other specific conditions that require further testing. Skin biopsy is typically not required for diagnosis. However, in women of childbearing age, it is essential to inquire about their history of hirsutism or dysmenorrhea. If the history of hirsutism or dysmenorrhea is positive in women of childbearing age, it is advisable to order further tests to measure the levels of testosterone, luteinizing hormone (LH), follicle-stimulating hormone (FSH), and dehydroepiandrosterone (DHEA).[34]
The sudden onset of severe, recalcitrant acne should raise the suspicion of hyperandrogenism induced by either an ovarian or adrenal tumor. In this case, laboratory and imaging tests may be essential.
Patients diagnosed with acne fulminans should undergo a comprehensive evaluation, including complete blood count, liver function tests, erythrocyte sedimentation rate, and C-reactive protein. This evaluation is particularly important for patients presenting with systemic symptoms. In addition, assessing serum cholesterol and triglyceride levels, performing a urine or serum pregnancy test for women, and considering radiographs when symptoms suggestive of joint or bone involvement are present are recommended. This thorough evaluation aims to assess the systemic involvement of acne fulminans and aids in preparing for isotretinoin therapy.[35]
Treatment / Management
The management of acne vulgaris, regardless of its severity, should commence with comprehensive patient counseling, encompassing discussions about the nature of the disease, proper skincare practices, and realistic treatment expectations. During patient counseling, it is essential to address the following points:
- The improvement of lesions may be delayed, and the primary objective of therapy is to resolve existing lesions and prevent the formation of new ones. At least 2-3 months of treatment compliance are needed to assess the efficacy of the treatment. The effective treatment response may involve a noticeable reduction of active lesions rather than complete clearance. This clarification helps to prevent patients from prematurely discontinuing their treatment process due to a perceived lack of efficacy.
- Long-term maintenance therapy is often necessary because most acne therapies are considered suppressive and not curative. The regular use of a topical retinoid can best achieve this.
- Responses to a treatment may vary from patient to patient. Therefore, it may be necessary to make adjustments to the treatment regimen to optimize both the tolerability and efficacy adjustment of the treatment.
- It is essential to promote the use of gentle skin cleansers instead of harsh soaps or scrubs, as soaps tend to have a higher pH level than the skin. This higher pH can lead to skin irritation and dryness. Aggressive scrubbing and picking of the skin should be discouraged as it may promote the development of new acne lesions and scarring.
- Selecting non-comedogenic skin products, such as gels and fluids, is essential to avoid blocking the pores.
- Various studies have reported associations between increased milk consumption and high glycemic load diets with acne vulgaris. However, there are currently no official recommendations for regulating the intake of these dietary factors in relation to acne. Nevertheless, discussions regarding the regulation of milk consumption and high glycemic load diets should be approached on a case-by-case basis.
Tailoring acne treatment should indeed take into consideration the severity of the acne.
I. Mild Acne Vulgaris
Acne vulgaris is considered mild when it presents with a few scattered comedones or small inflammatory papules without scarring. Additional features include a few lesions on either a single body area or in multiple body areas. It is also important to note the absence of nodules or their confluence. The primary treatment approach for mild acne vulgaris is topical therapy, which commonly involves the use of topical retinoids, topical antibiotics, and benzoyl peroxide.
Topical Retinoids
Topical retinoids are vitamin A derivatives that act by binding to retinoic acid receptors (RARs) and retinoid X receptors (RXRs) within the keratinocytes. Trifarotene is selective for only the RAR-gamma receptor. Tretinoin, tazarotene, and adapalene are topical retinoids that primarily act upon the RAR-beta and RAR-gamma receptors. Among them, tretinoin also targets the RAR-alpha receptor. Upon binding, the retinoid-receptor complexes are formed and transported into the cell's nucleus, activating the retinoid hormone response element, thereby stimulating the transcription of several regulatory genes. The significant outcomes of this process are the normalization of follicular keratinization and the loosening of the cohesiveness of the keratinocytes, thereby decreasing the formation of microcomedones.
Topical retinoids, such as tretinoin, tazarotene, adapalene, and trifarotene, should be included in the initial management for most patients with acne. These medications effectively target both comedones and inflammatory papules and pustules. For patients with predominantly comedonal acne, topical retinoids can be used as a monotherapy. They are also recommended for maintenance therapy after successful treatment. Patients with papulopustular acne can benefit from adding a topical antimicrobial agent such as benzoyl peroxide or topical antibiotic. Topical antibiotics should ideally be used in combination with benzoyl peroxide to minimize the risk of antibiotic-resistant bacteria emerging.
The topical retinoid should be applied once daily, preferably at night, due to the reported photolability of tretinoin.[36] However, adapalene and trifarotene are more stable in the presence of light.[37] Before applying retinoid, ensure that the skin is dry. A thin layer of the topical retinoid should be applied to the whole affected area rather than spot-treating individual lesions. A pea-sized amount of the medication is sufficient to cover the entire face. The frequency of application should be adjusted to minimize the risk of skin irritation. It is recommended to apply retinoids every other night or every third night. As tolerance improves, the frequency of application can be increased gradually over a few weeks until daily use is achieved. Similarly, the resulting irritation from topical retinoids can be reduced by using the lowest concentration and increasing it as tolerance develops. Alternatively, for individuals experiencing significant irritation, short-contact therapy with tazarotene can be considered, which involves applying tazarotene for up to 5 min daily and then rinsing it off with water.[38]
Some common adverse effects of topical retinoids are dryness, irritation, flaking of the skin, and sensitivity to sunlight due to skin thinning. However, these adverse effects can often be managed using non-comedogenic facial moisturizers and sunscreens.[39] It is important to note that topical retinoids are not recommended for use during pregnancy.
Benzoyl Peroxide
Benzoyl peroxide possesses both comedolytic and antimicrobial properties. It is available in various formulations and concentrations ranging from 2.5% to 10%. Typically, it is applied once daily, focusing on 1 or 2 small areas during the initial 3 days to test for any potential hypersensitivity reactions. Benzoyl peroxide should not be applied simultaneously with tretinoin due to its oxidizing effect on tretinoin. To avoid any reaction, benzoyl peroxide should be applied in the morning, whereas tretinoin should be applied in the evening.
Nonetheless, the microsphere formulation and polymeric emulsion of tretinoin, adapalene, and trifarotene are stable in the presence of benzoyl peroxide. It is important to note that skin irritation may occur with benzoyl peroxide use, particularly at high concentrations. It may also have a bleaching effect on clothing and hair.
Topical Clindamycin
Topical clindamycin is available in various formulations and in combination with either benzoyl peroxide or topical retinoids. It is typically applied once or twice daily. While using topical clindamycin, combining it with benzoyl peroxide is recommended to mitigate the risk of developing antibiotic resistance.[40] Although it is generally well-tolerated, some individuals may experience skin irritation as a possible adverse effect.
Topical Erythromycin
Topical erythromycin can be considered an alternative to topical clindamycin for treating acne. However, there has been an increased reporting of erythromycin resistance, making clindamycin the preferred choice. Therefore, when using topical clindamycin, combining it with benzoyl peroxide whenever possible is advisable.[41]
Azelaic Acid
Azelaic acid is a naturally occurring dicarboxylic acid with comedolytic, antimicrobial, and whitening effects due to its inhibition of tyrosinase enzyme, which is beneficial in patients with coexistent postacne hyperpigmentation.
Topical Salicylic Acid
Topical salicylic acid can be used as an alternative to topical retinoids for individuals who are unable to tolerate or obtain them.
In cases where patients do not initially respond to topical retinoids, benzoyl peroxide, and clindamycin, there are alternative topical therapies available, which include topical dapsone, topical minocycline, and clascoterone (the topical androgen receptor inhibitor).
II. Moderate-to-Severe Acne Vulgaris
Acne vulgaris is considered moderate to severe when presenting with prominent comedones, large inflammatory papules and pustules, and nodules with associated scarring, affecting multiple body areas. In assessing acne severity, it is essential to consider the psychological burden it may impose on individuals. Some cases may present with mild comedonal acne, but the acne causes significant psychological distress due to cosmetic concerns, thereby necessitating a more aggressive approach similar to moderate-to-severe cases. Topical and systemic therapies are the primary treatment options for moderate-to-severe acne vulgaris. Systemic therapies for acne include oral antibiotics (primarily tetracyclines), hormonal therapies (such as spironolactone or oral contraceptives for female patients), and oral isotretinoin. Systemic therapy is often combined with topical therapy, as discussed for mild cases, except for oral isotretinoin.
Oral Isotretinoin
Oral isotretinoin is a retinoid that combats acne vulgaris by counteracting the 4 pathogenic factors that contribute to the disease. Hence, it is well-accepted as a treatment for severe recalcitrant nodular acne associated with scarring.[41] Oral isotretinoin is typically prescribed as a monotherapy for severe acne vulgaris and is administered at a daily dosage of 0.5 to 1 mg/kg per day over several months. However, patients with severe acne vulgaris at a high risk of developing isotretinoin-induced acne flare may benefit from combining oral steroids at the start of treatment. Oral isotretinoin is teratogenic and therefore contraindicated during pregnancy. Patients taking isotretinoin should inform their healthcare providers about any plans for pregnancy, allowing for the discontinuation of isotretinoin at least 1 month before attempting pregnancy. Other adverse effects associated with the drug include myalgia, dry skin and mucous membranes, visual changes, hyperlipidemia, and elevation of hepatic transaminase levels. Patients taking isotretinoin should also refrain from donating blood while on the medication.
Oral Antibiotics
Oral antibiotics effectively inhibit the growth of C acnes within the pilosebaceous unit. Tetracyclines, in particular, have anti-inflammatory properties, making them the preferred antibiotic for treating acne vulgaris. If tetracyclines are ineffective or not well-tolerated by patients, other antibiotics (such as macrolides, cephalosporins, penicillins, and trimethoprim-sulfamethoxazole) may be considered alternatives.[41] To reduce the development of antibiotic resistance, it is necessary to limit the duration of the treatment to the shortest possible period (ideally, 3-4 months). This can be complemented by the concurrent use of a topical retinoid, which can aid in the discontinuation of the antibiotic, or by incorporating the use of benzoyl peroxide. Preferred tetracyclines for acne treatment include doxycycline, minocycline, and sarecycline. Doxycycline and other tetracyclines should not be prescribed to patients who are children aged less than 8 or pregnant women. Long-term treatment with oral antibiotics may lead to tooth discoloration in developing teeth. Moreover, doxycycline can cause gastrointestinal distress, esophagitis, and pseudotumor cerebri (idiopathic intracranial hypertension). Photosensitivity is also one of the adverse effects of oral antibiotics; therefore, sun protective measures are advised while on treatment with tetracyclines.
Oral Hormonal Therapies
Oral hormonal therapies, such as oral contraceptives and spironolactone, are effective options for female patients seeking acne treatment. These therapies reduce the action of androgens on pilosebaceous units, which in turn decreases sebum production and helps alleviate acne symptoms. Hormonal therapy is an appropriate treatment option for various groups of females, including postmenarchal women dealing with severe acne vulgaris, women experiencing acne related to hyperandrogenism, and women with milder acne seeking contraception.[41] The treatment regimens for using oral contraceptives to manage acne vulgaris are similar to those used for contraception. However, only 3 oral contraceptives have been approved by the US Food and Drug Administration (FDA) for treating acne. These include ethinyl estradiol 20/30/35 mcg/norethindrone 1 mg, ethinyl estradiol 35 mcg/norgestimate 180/215/250 mcg, and ethinyl estradiol 20 mcg/drospirenone 3 mg. On the other hand, progestin-only contraceptives, which include low-dose oral pills containing androgenic progestins (such as norethindrone or desogestrel), are not considered effective and may exacerbate acne vulgaris. Treatment with oral contraceptives should be avoided in patients with underlying thrombophilic disorders or those having a history of thromboembolic events.[42]
Spironolactone is an oral anti-androgen that effectively blocks androgen receptors and inhibits androgen synthesis. This medication decreases the activity of 17-beta-hydroxysteroid dehydrogenase, possibly inhibits 5-alpha reductase, and potentially increases the levels of steroid hormone-binding globulin. The combined result of these actions is about a 50% reduction in sebum secretion.[43] The treatment with spironolactone can be initiated in patients with a daily total dosage of 25 or 50 mg, with subsequent dose escalation up to 100 mg per day, administered as a single daily dose or divided into 2 separate doses.[7] The adverse effects of this drug include breast tenderness, menstrual irregularities, minor gastrointestinal symptoms, hyperkalemia, orthostatic hypotension, and headache. Concomitant use of oral contraceptives can counteract some adverse effects, such as menstrual irregularities and breast tenderness.
III. Management of Complications
Managing complications in acne vulgaris involves various approaches to address specific issues that may arise. Here are some common complications and their corresponding management strategies:
- Postinflammatory hyperpigmentation can be managed by photoprotection, topical treatments (such as retinoids, azelaic acid, and hydroquinone), and superficial chemical peels (which use salicylic acid or glycolic acid).
- Postinflammatory erythema can be managed by pulsed-dye laser, fractional micro-needling radiofrequency, intense pulsed light, and topical application of 5% tranexamic acid.
- Ice-pick scars can be managed by chemical reconstruction of skin scars (CROSS) using trichloroacetic acid, punch elevation or excision, ablative fractional laser or erbium resurfacing, and filler injection.
- Rolling scars can be managed by subcision, needle-free pneumatic solution injection, and filler injection. A combination of ablative fractional laser with subcision can be effective for contoured scars.
- Boxcar scar can be managed by excision (if the scar is deep), erbium laser treatment, needle-free pneumatic solution injection, and filler injection.
- Hypertrophic scar or keloid can be managed by pulsed dye laser or intense pulsed light therapy, intralesional injection of triamcinolone, 5-fluorouracil or bleomycin, cryotherapy, radiotherapy, and surgical excision.
- Papular scars can be managed by controlled CO2 laser vaporization and light electrodesiccation of each papule.
Differential Diagnosis
The differential diagnoses for acne vulgaris vary widely and include those listed below.
- Rosacea can be differentiated from acne by the presence of comedones and the absence of telangiectasia.
- Perioral dermatitis is characterized by grouped erythematous papules in a perioral distribution, sparing the lip margin, unlike acne vulgaris.
- Demodex folliculitis presents as inflammatory papules and pustules. It is suspected when the patient fails to respond to acne or rosacea treatment.
- Facial angiofibroma in tuberous sclerosis appears as pink or red papules on the cheeks and nose of children.
- Pseudofolliculitis barbae appears as inflammatory papules, pustules, and scarring in the beard area of patients with tightly curved hair.
- Nevus comedonicus exhibits a grouped arrangement of comedones and typically appears at birth or in childhood.
- Sebaceous hyperplasia is characterized by small, umbilicated yellowish papules often found on the forehead and cheeks.
- Adnexal tumors (such as trichoepithelioma, trichodiscoma, and fibrofolliculoma) appear as flesh-colored facial papules.
- Favre-Racouchot syndrome is commonly observed in older adults and is attributed to photodamage. It manifests as comedones in the upper lateral cheeks.
Prognosis
The overall prognosis of acne is generally good with appropriate treatment. While acne may not be life-threatening, it can have significant and lasting psychosocial effects. Individuals with acne and acne scars often experience increased levels of anxiety and depression. The acne scars can be challenging to correct effectively. A study from Sweden[44] suggests a potential association between acne in teenage boys and an increased risk of developing prostate cancer later in their lives.
Complications
The complications associated with acne vulgaris may include:
- Psychological effects, including depression, anxiety, and lowered self-esteem, may arise either from the visible appearance of the affected skin during an acne flare-up or from the resulting disfiguring scars.
- Acne fulminans is characterized by the acute eruption of large inflammatory nodules accompanied by ulcers and hemorrhagic crusts. This condition primarily affects male adolescents with preexisting acne. It can be triggered by isotretinoin therapy or may occur spontaneously, regardless of whether systemic symptoms are present. Accordingly, this condition is divided into 4 variants based on the presence or absence of systemic symptoms and whether it is induced by isotretinoin or occurs spontaneously. Isotretinoin-induced acne fulminans without systemic symptoms is the most common variant of this condition. Systemic symptoms can manifest as fever, malaise, bone pains, erythema nodosum, arthralgia, and abnormalities detected through radiological and laboratory tests. Potential laboratory abnormalities include leukocytosis, anemia, and an elevated erythrocyte sedimentation rate or C-reactive protein. Radiographs may reveal osteolytic lesions of the bone, particularly in the sternum, clavicles, sacroiliac joints, or hips.[35]
- Solid facial edema, or Morbihan's disease, presents with facial erythema and edema. This condition is characterized by periods of remissions and exacerbations; however, it often necessitates intervention to achieve resolution. Treatment options have shown success using isotretinoin, steroids, and clofazimine.
- Gram-negative folliculitis is observed in patients undergoing long-term systemic antibiotic treatment, particularly tetracyclines, for acne. Initially, these patients show a positive response to the antibiotic therapy. However, their acne worsens over time and becomes resistant to oral antibiotics treatment. The perinasal skin and central face are frequently affected in this condition, exhibiting inflammatory pustules and nodules. Culturing of the lesions typically reveals the presence of Gram-negative organisms, including Enterobacter, Klebsiella, Pseudomonas, Proteus, or Escherichia species.
Pearls and Other Issues
Although acne is unavoidable, it can be effectively controlled through various measures. Regularly washing one's face with a pH-balancing cleanser, such as benzoyl peroxide or salicylic acid face wash, can help manage acne symptoms. Avoiding high glycemic index foods and dairy-based products may help manage acne symptoms in some individuals. Managing stress levels is another important aspect of acne control.
For some individuals, underlying health conditions, such as polycystic ovarian syndrome, can contribute to acne. Early detection and treatment of such underlying causes are crucial for controlling acne and preventing disfigurement.
Although retinoids are highly effective acne treatment agents, their use in women of childbearing age is limited due to their teratogenic effects. To ensure safe use and address concerns, a registry has been established to monitor all individuals who are prescribed or dispensed retinoids, such as isotretinoin.
Outcomes
While most patients experience positive outcomes after acne treatment, some may develop residual scars. However, such scars can be minimized by educating the patient on the importance of refraining from manipulating the lesions and seeking timely professional care. When established, the treatment of acne scars is not optimal.[45]
Enhancing Healthcare Team Outcomes
The American Academy of Dermatology has evidence-based guidelines on the management of acne.[41] Therefore, all healthcare workers, including primary care providers and nurses, who are involved in managing acne must be familiar with these guidelines and understand how to stratify treatment based on individual needs. If a healthcare provider decides to use an oral contraceptive as a means to manage acne for their patients, they should follow the guidelines established by the World Health Organization (WHO). Finally, it is essential to note that determining the specific type of bacteria causing acne is generally of academic importance and should not significantly alter the treatment approach.
A consultation with a dermatologist is highly recommended if the acne is severe. The pharmacist should be fully aware of the adverse effects associated with medications (especially isotretinoin) and their potential teratogenic effects. The pharmacist should never dispense retinoids to a woman of childbearing age without consulting with the prescribing dermatologist or healthcare provider. The pharmacist should educate the patient on the potential teratogenic effects of retinoids and adhere to the iPLEDGE risk management program.[46][47] [Level V] Dermatology and plastic surgery nurses play an intricate role in patient care and management by actively participating in various aspects of the treatment procedure. They are involved in patient and family education, monitor the response to therapy, and provide valuable feedback to the healthcare team.