Continuing Education Activity
The wrist is one of the most frequently splinted parts of the body, often after injury or surgery. Wrist splints provide rigid support to allow proper healing, decreased pain, and sustained alignment. The three most common types of wrist splint are volar, thumb spica, and sugar tong, each of which has its own indications. This activity reviews the varieties and indications of wrist splints and highlights the role of the interprofessional team in evaluating and treating patients who undergo surgery or sustain injuries to the wrist.
Objectives:
- Describe the anatomy of the wrist joint.
- Review the different types of wrist splints and their appropriate applications.
- Outline the technique of creating a wrist splint.
- Summarize complications that may arise from wrist splints and how to correct them.
Introduction
The wrist is a complex joint consisting of the distal radial and ulnar bones plus the eight carpal bones. The fibrocartilaginous complex is located between the carpal bones and the distal ulnar bone. Each of these structures has the propensity to get injured. The wrist can be injured during a fall, sporting activities, or from repetitive movements. Today, the use of a wrist splint has become invaluable for the treatment of many types of wrist injuries. The role of the wrist splints is to immobilize the wrist in a position to facilitate healing. This allows for edema to subside and the pain to decrease. There are many types of splining materials and pre-made splints on the market, each intended for a specific purpose.
Two common syndromes where a wrist splint is used are carpal tunnel syndrome and osteoarthritis (OA). The wrist splint is most commonly worn at night, but may also be worn during the day to improve the symptoms of the disorder. Many studies indicate that the use of a wrist splint for carpal tunnel syndrome can help decrease symptoms in just a few weeks. In OA, wearing a wrist splint at night showed reduced joint pain after 6 months of use.[1] The wrist splint can also be combined with physical therapy to create a marked improvement in symptoms.
Wrist splints can help correct minor orthopedic maladjustments through immobilization. These custom molded splints provide temporary alignment and allow swelling to subside prior to casting. There are a variety of materials and sizes that can be used and vary based on availability, cost, and/or personal preference. Common splint types include volar, dorsal, radial gutter (thumb spica), ulnar gutter, and sugar tong.
Clinical Significance
Wrist splints are widely used after surgery to decrease pain, promote proper healing, and ensure that the hardware or the reduced joint does not move. It is important to avoid wearing a wrist splint for prolonged periods as it can lead to a frozen joint.
No study has shown that one type of wrist splint is better than the other. It is all a matter of availability, affordability, and personal preference. After wearing a wrist splint, the joint does become stiff, and hence, some wrist exercise is recommended to regain the motion and strength. Individuals who have a wrist splint after surgery should speak to their physician before undertaking any exercise.
Anatomy and Physiology
The anatomy of the wrist joint is complex, composed of numerous bones, ligaments, tendons, and cartilaginous structures. Of note, there are 8 carpal bones: scaphoid, lunate, triquetral, pisiform, trapezium, trapezoid, capitate, and hamate. The articulations of the wrist are composed of the distal radius with the scaphoid and lunate carpal bones and with the distal ulna. The lunate is the most commonly dislocated of the carpal bones, while the scaphoid is most prone to fracture. The scaphoid can be palpated in the anatomical snuffbox, which is a small triangular area on the dorsal surface of the hand between the extensor pollicis longus (medially) and the extensor pollicis brevis and abductor pollicis longus (laterally). The major ligament of the wrist is the triangular fibrocartilage complex (TFCC), which keeps the wrist joint stable while pronating and supinating the arm. Each of these structures has the propensity to be injured and therefore is suitable for splinting.
Indications
The utilization of wrist splints may be either required or recommended. In situations such as during post-operative or post-reduction periods, the splint will be required to keep anatomical or near-anatomic alignment to allow for proper healing. For athletes, proper splinting can provide adequate protection in order to allow some of them to return to play while healing.[2] Conversely, for conditions such as sprain or strain, carpal tunnel, or osteoarthritis, the use of a wrist splint will reduce motion, diminish pain, and promote healing.
There are three main types of custom-molded splints that will be utilized for wrist injuries or pain, which are volar, thumb spica, and sugar tong. A volar splint is utilized for injuries involving carpal bones (excluding scaphoid and trapezium) and soft tissue injuries of the wrist. Thumb spica is utilized for suspected injuries to the scaphoid, de Quervain tenosynovitis, and injuries or pain of the thumb. Of note, a thumb spica should be performed for both confirmed and suspected scaphoid fractures, as the risk is high for avascular necrosis due to its blood supply. Confirmed or suspected scaphoid fractures require orthopedic follow-up for further monitoring and/or intervention. Sugar tong is utilized for acute injuries of the distal radius and ulna, as it will provide volar and dorsal support while limiting supination and pronation of the forearm.[3]
Contraindications
The decision to apply a wrist splint should involve evaluating the risks versus the benefits on a case by case basis. Some situations may arise that would warrant alternative management, ranging from withholding a splint entirely to immediate surgical fixation. A limited list of these situations may include: significant swelling of the extremity, burns overlying the fracture site that requires frequent dressing changes, underlying medical hardware that require frequent access (i.e., dialysis catheter, PICC line for medications), or open fracture.
Equipment
Required materials include casting material (fiberglass, pre-padded casting material with fiberglass, plaster, etc), web roll (2” to 4”), elastic wrap (3”), stockinette (optional), shears or large scissors, sheets/chuck pads for draping, sling (if performing sugar tong splint), and a table/stand for supplies. If the splinting area does not have a sink available, one will also need a bucket or emesis basin.
Note: plaster and Ortho-Glass™ undergo an exothermic chemical reaction (heat release) when in contact with water. Using hot water will cause the material to harden faster while using cold water will cause the material to harden slower. Using warm water will give adequate time (approximately 10 minutes) to mold the splint while not causing you to stand for extended periods of time waiting for it to harden.
Personnel
Splinting a wrist can be performed by a single provider; however, having an additional person to aid in positioning is helpful. The assistant does not need to be a medical professional, as they will mainly be holding manual stabilization.
Preparation
As is true with all procedures, the key to success is adequate preparation. To fabricate a wrist splint, first, obtain all equipment as outlined above. If you do not have a sink available in your procedure room, fill a bucket or emesis basin with a few inches of warm water. Place a sheet or chuck pad on the floor and under the extremity to be treated. Using web roll, measure the length of the splint to be applied (see technique section below for lengths) and tear at the appropriate length. For plaster splints, tear three additional layers of web roll to be used as padding (optional for pre-padded). Using the measured web roll strip as a guide, cut the pre-padded casting material with fiberglass to size with shears/scissors or, if using plaster, cut 8 strips of equal length and layer on top of each other.[4] If using pre-padded casting material with fiberglass, stretch soft outer layer past the distal splint material or open and cut splint material 1 to 2 cm to avoid patient discomfort or injury when material hardens. Wrap web roll around the extremity, covering the area that will be in contact with the splint; be sure to apply additional layers to bony prominences, such as the radial styloid, ulnar styloid, and elbow. Open the elastic wrap and have within easy grasp from the fracture site. Submerge the pre-padded casting material with fiberglass or plaster in water, then remove excess by wringing out pre-padded casting material with fiberglass or milking plaster by running between two fingers from top to bottom. Place splint material between two layers of web roll padding and apply it to the patient as below.
Technique or Treatment
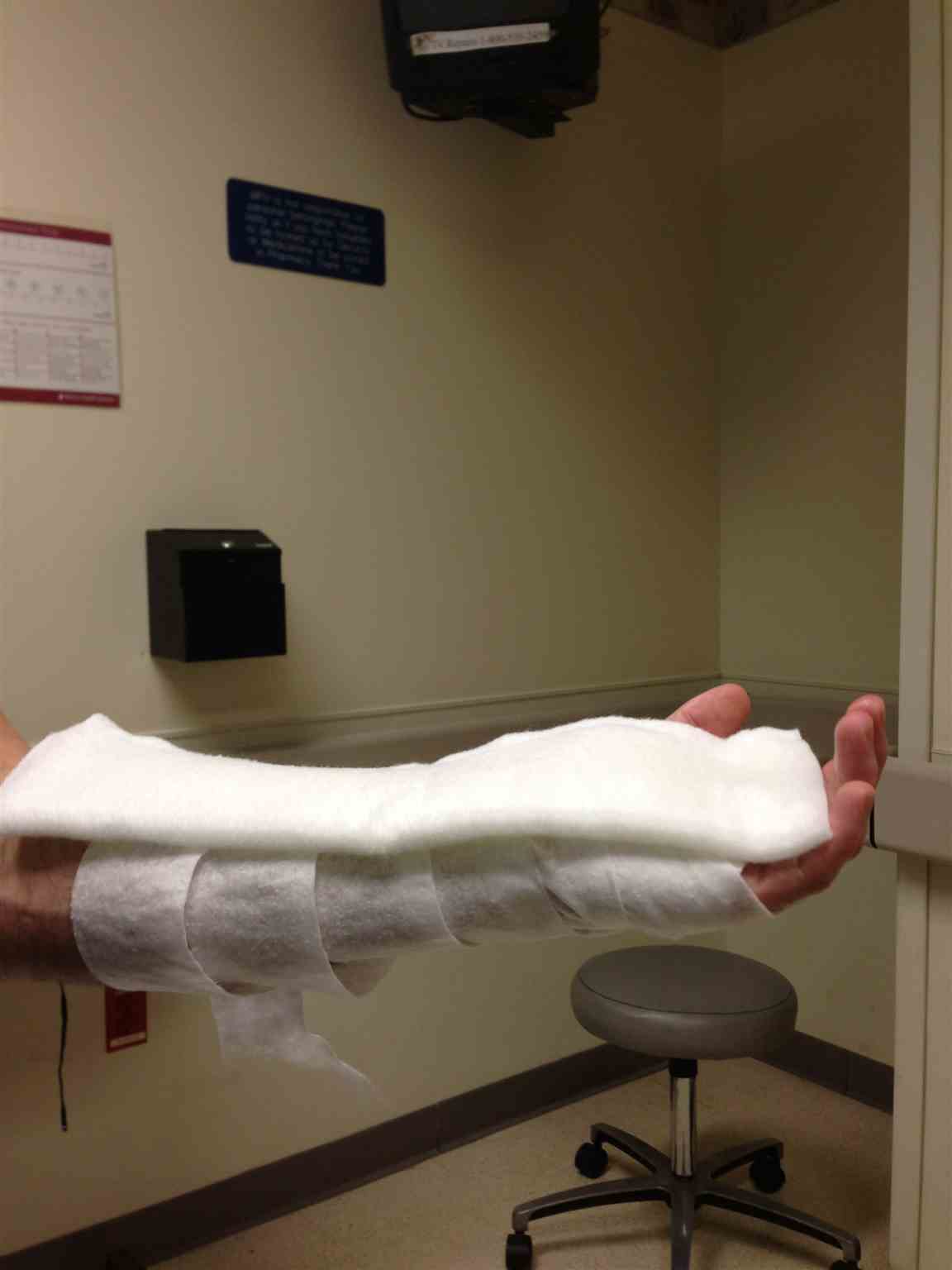
Volar splint: Apply splinting material to the volar (anterior) aspect of the forearm. The material should span from the 1 cm proximal to the transverse palmar crease to the proximal forearm.[5] Once applied, mold to the patient with the wrist slightly extended. Apply the elastic wrap to keep the splint in place, ensuring not to stretch while applying. Check fingertip movement, capillary refill, and sensation after applying a splint to rule out a neurovascular compromise.[6]
Thumb spica: Place the forearm in a neutral position (no pronation/supination). Apply splinting material to the radial side of the forearm, wrapping around the thumb. The material should span from just past the thumb IP joint to the proximal forearm. Once applied, mold to the patient with the thumb in a functional position (“soda can” grasp), and the wrist extended 20 to 30 degrees. Apply the elastic wrap to keep the splint in place, ensuring not to stretch while applying. Check fingertip movement, capillary refill, and sensation after applying a splint to rule out a neurovascular compromise.
Sugar tong: Place forearm in neutral position (no pronation/supination). If utilizing an assistant, have the patient rest their elbow on a table with their forearm elevated; if sole provider, the patient may rest the ulnar aspect of their forearm on a table to assist with splint adherence. Apply splinting material from the proximal palmar crease, wrapping around the elbow, and extending to the dorsal metacarpal pharyngeal joint. Once applied, mold to the patient with the wrist slightly extended. Apply the elastic wrap to keep the splint in place, ensuring not to stretch while applying. Check fingertip movement, capillary refill, and sensation after applying a splint to rule out a neurovascular compromise.
For pre-fabricated splints, such as those for carpal tunnel or OA, simply apply the splint according to the instructions on the packaging. Ensure that the splint is secure but do not overtighten. Always check fingertip movement, capillary refill, and sensation after applying a splint to ensure there is no neurovascular compromise.[7]
Complications
It is important to recognize the complications that may arise not only from performing wrist splinting but those which may occur due to the underlying injury as well. Compartment syndrome is a major complication resulting from increased pressure within fascial planes, which leads to impaired venous and lymphatic flow, which may be due to increased internal swelling or an excessively tight cast/splint. This is an emergency, and it is, therefore, crucial that patients be educated regarding the six signs and symptoms of compartment syndrome – pain out of proportion (early), paresthesia, poikilothermia, paresis, pallor, and pulselessness (late). If caused by internal pressure, treatment is an emergent surgical fasciotomy, whereas increased pressure due to a cast/splint is relieved by cutting the cast or loosening splint or elastic wrap. Improper positioning, splint fabrication, or lack of padding can cause pressure ulcers, lacerations, increased pain/swelling, and tendon rupture.[8] Improper alignment of a fracture may lead to poor healing and poor functional outcome and may require corrective surgery. Finally, excessively pressure exhibited onto the volar distal forearm can cause acute carpal tunnel syndrome.
Clinical Significance
Splints may be used to treat both acute and chronic orthopedic complaints. Proper splint application allows for pain relief, improved vascular and lymphatic flow, and alignment for healing.
Enhancing Healthcare Team Outcomes
Treatment of injured extremities involves a multidisciplinary team. A medical professional must first evaluate the extremity, be it a physician or NP/PA in primary care, emergency medicine, orthopedic surgery. A fracture should be excluded, which then involves a radiology tech to perform an x-ray and a radiologist to interpret the images. The extremity should be monitored, involving nurses for wound and splint checks. To improve functional outcomes, patients should start early physical therapy to increase range of motion and strength.[9][10]