Continuing Education Activity
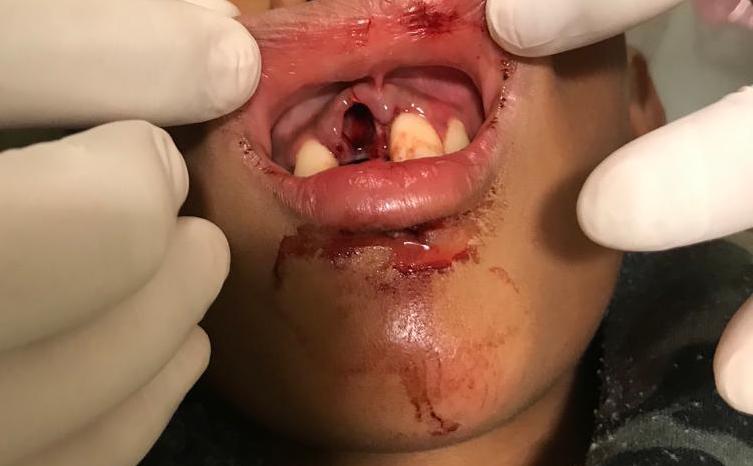
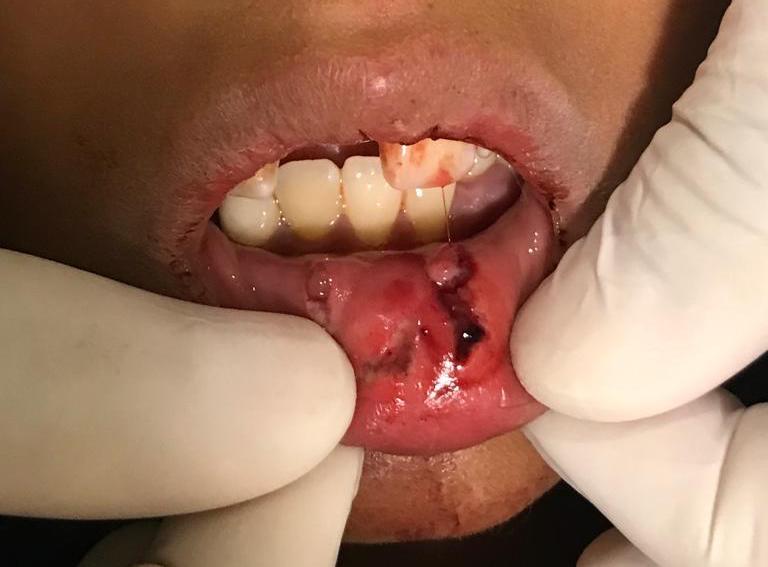
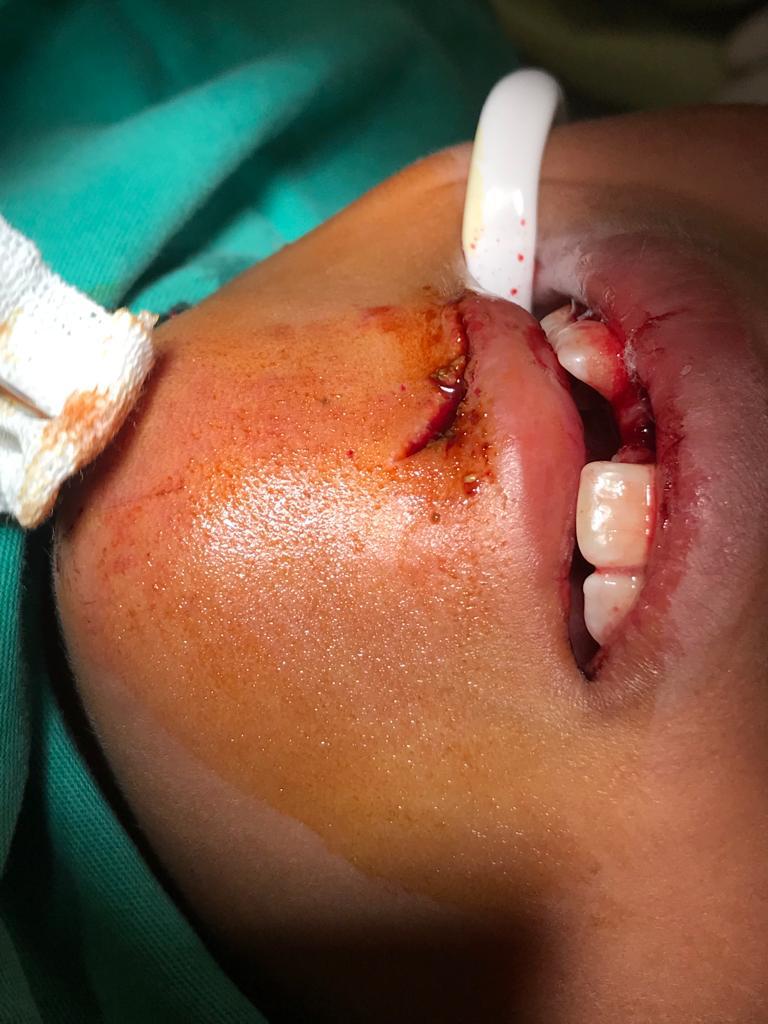
Dentoalveolar trauma injuries are caused by an external impact on the teeth, palate, mandible, maxilla, and gingiva. These injuries can result in anything from a tooth contusion to a total dislocation of the tooth from its socket, known as tooth avulsion. A significant amount of force is usually necessary for the avulsion of teeth, and other injuries to surrounding structures should be suspected. This activity reviews the evaluation, diagnosis, and management of tooth avulsion and highlights the role of team-based interprofessional care for affected patients.
Objectives:
- Describe the epidemiology of tooth avulsion.
- Review the treatment regime for an avulsed tooth.
- Explain the pathophysiology and histopathology of an avulsed tooth.
- Summarize the complications usually associated with tooth avulsion.
Introduction
Dento-alveolar trauma includes injuries caused by an external impact on the dentition and its surrounding structures. These injuries range from a simple contusion of the tooth to its total dislocation from the alveolar bone, termed tooth avulsion, a rare type of dental trauma. A significant amount of force is usually necessary for the avulsion of a tooth. Other injuries to the surrounding structures, such as alveolar bone fractures and gingival contusions, should be suspected.[1]
Replantation is the treatment of choice, and time management and appropriate storage of the avulsed tooth are crucial factors that will guarantee a good prognosis. Anti-resorption therapy is a newer technique that prevents the common inflammation that avulsed teeth experience after replantation, using a combination of antibiotics and corticosteroids. Splinting and systemic antibiotics are also included in the treatment regime of a patient with an avulsed tooth. Finally, follow-up appointments are of utmost importance, where the tooth will be assessed clinically and radiographically to confirm tooth vitality and rule out root resorption or ankylosis.
Etiology
The most common causes of dentoalveolar trauma include falls, especially in children, cycling, full-contact sports, traffic accidents, and assault. Dental trauma most frequently occurs at home, school, and sports centers.
Anatomic features that increase the likelihood of dentoalveolar trauma include protuberant upper teeth, overjet (over 3 mm), anterior open bite, malocclusion (Class II), incompetent lips, and mouth breathing.[2][3]
Epidemiology
The peak incidence of dental trauma occurs in the 7-11-year age group, with a male to female ratio of 2:1.[2][3] Permanent teeth are injured more than temporary (60% vs. 40%, respectively). A study of 800 children of 11-13 years of age found that just above half of them experienced dental trauma in permanent anterior teeth, with approximately 10% of respondents not remembering a history of trauma. In a study conducted on 1298 trauma patients that received treatment in an emergency room, 24% included dental injuries, of which two-thirds were tooth avulsions.
Falls are the most common cause of dental trauma, followed by cycling accidents, full-contact sports, and assaults. Bemelmans reported that at least 32% of athletes involved in full-contact sports had experienced some form of injury to their dentition. The most high-risk sports for dental injury are ice hockey, football, lacrosse, rugby, martial arts, and skating. Helmets have not decreased the incidence of dental trauma, but mouth guards have. Dental trauma in younger children should always raise the suspicion of abuse.[4][5]
Pathophysiology
The periodontal ligament (PDL) is the soft tissue connecting the cementum that covers the roots of the teeth to the surrounding alveolar bone. When an external impact occurs on a tooth, the periodontal fibers can tear, allowing partial or total displacement of the tooth from the socket. The ensuing damage can lead to neuro-vascular disruption, as well as pulp necrosis. The maxillary central incisors are the most commonly affected teeth, followed by the maxillary lateral incisors. Often, more than one tooth is avulsed. Periodontal ligament fibers can desiccate rapidly in the open air. Even in a replanted tooth, the damaged periodontal ligament fibers can lead to bony resorption of the root. Root resorption will lead to crown fracture and loss of the tooth.[6][2][3]
Histopathology
The periodontal ligament fibers are torn when a tooth is avulsed, but the periodontal ligament cells remain viable on the root surface. Small and localized areas of cemental damage are usually seen due to the root scraping against the alveolar socket.[7]
History and Physical
A history of trauma to the tooth will reveal tooth avulsion, and the mechanism of injury can point to other injuries. History should include the length of time since tooth avulsion, the storage medium in which the tooth had been placed, and if the tooth is primary or permanent. By 14 years of age, a patient's primary teeth should all be replaced by permanent teeth.
Physical examination involves assessing the tooth socket for foreign material, and tooth fragments as these can prevent tooth replantation and evaluating the surrounding structures for other injuries such as lacerations, gingival contusions, and bone fractures. If a tooth suspected of avulsion is not found, aspiration, gastro-intestinal placement, or intrusion should be ruled out.
Evaluation
Imaging modalities, including extraoral and intraoral radiographs and CT scans, can aid in evaluating dental, alveolar, and surrounding fractures. Imaging is useful in identifying the intrusion of a missing tooth.
Treatment / Management
Replantation is the treatment of choice [8], although not always possible. The appropriate management of an avulsed tooth within the first 30 minutes and an organized treatment plan are essential to increase tooth survival. The treatment first aims to preserve tooth vitality or maintain a functional tooth in its alveolar socket to minimize growth retardation of the alveolar bone, which will be needed to place a dental implant in the future.[9]
Pre-replantation Procedures
Storage Media
Storing the avulsed tooth in an isotonic solution, such as milk, saline, or saliva, slows down cell death in the periodontal ligament of the root.[10] However, PDL cell death is unavoidable, and the storage in a solution is only a temporary but effective way of managing the tooth before replantation. Short-time storage in an isotonic solution has proven to provide the same or even higher healing results than replanting the tooth immediately.[11][12][11] Milk is the most frequently used and recommended storage solution due to its ready availability, appropriate pH, normal osmolarity, an abundance of nutrients, and growth factors.[9] It is worth noting that drinking water can damage the PDL due to its low osmolality.
Anti-resorption Therapy
It involves soaking the avulsed tooth in a storage solution containing antibiotics. Anti-resorption therapy is believed to prevent inflammation caused by necrotic cells and microbial contamination.[9] Different regimes have been suggested; one includes a storage solution with 800 µg doxycycline and 640 µg dexamethasone for 20 minutes.[9] In the meantime, the alveolus should be lightly irrigated with 0.9% physiologic saline solution and aspirated gently if a blood clot is obstructing it.
Tooth Replantation
The tooth should be aligned anatomically and replanted, applying firm pressure to the socket. Most teeth can be successfully replanted if the extraoral dry time is less than 30 minutes; after this period, the survival probability of the tooth diminishes - the periodontal ligament cells are irreversibly damaged after 30 to 60 minutes.
Post-replantation Procedures
Splinting
Once the tooth has been replanted, it should be immobilized with a semi-rigid splint (e.g., titanium trauma splint). Splinting immobilizes the replanted tooth and allows the damaged periodontal ligament fibers to reestablish connection from the alveolus to the cementum. The International Association of Dental Traumatology (IADT) guidelines indicate flexible splinting for all dental injuries. The splinting time is two weeks for avulsed teeth and four weeks if the avulsed tooth exceeded 60 minutes of dry time.[13] They do not give any specific splint type recommendation for alveolar fractures,[13] but they do recommend immobilizing the alveolar segment for four weeks.[13]
Systemic Antibiotics
It is advisable to prescribe the patient doxycycline for five days or amoxicillin in case of intolerance. In children under 50 kg, the regime includes an initial dose of 100 mg doxycycline on the first day and 50 mg on the four consecutive days.[14]
Follow up Appointment
The splint must be removed after two weeks, where the tooth will be clinically and radiographically examined. After removing the splint, the tooth’s mobility is checked, and a pulp vitality test should be performed, preferably pulse oximetry or electric testing.[15]
If the tooth is non-vital, a root canal treatment is indicated since there is no probability of revascularisation.[9] If the pulp is vital, an x-ray should be taken using an individualized holder. During the consecutive follow-up appointments (after one, three, and six months), a new x-ray will be taken to check for resorption. After this point, if there is no visible resorption, the patient is recalled every year for follow-up. In case of resorption, a root canal treatment is indicated.[16]
When the dry time is more than 60 minutes, the remaining PDL should be removed as it will become a stimulus for continued inflammation that accelerates infection-related resorption and ankylosis. The remaining PDL can be removed by gentle scaling and root planning, soft pumice prophylaxis, gauze, or soaking the tooth in 3% citric acid for 3 minutes. Fluoride treatment must follow this procedure as it slows down ankylosis and reduces the risk of resorption.
Severe damage to the neurovascular bundle and the periodontal ligament can lead to replacement root resorption or inflammatory resorption. These complications can be anticipated and possibly prevented with disinfectants at the time of reimplantation and systemic antibiotics. Resorption complications may need a root canal.[2][17][3][18] If the extraoral dry time is over 90 minutes, soaking the tooth in agents such as fluoride may decrease resorption rates.
Immature teeth where the root has not yet wholly formed have a greater chance of revascularization after soaking in doxycycline. Primary teeth should not undergo replantation as this can damage the underlying permanent tooth germ.
Differential Diagnosis
Differential diagnosis of tooth avulsion includes complete tooth intrusion into the alveolar bone, subluxation, or lateral luxation. A 'missing tooth' needs to have intrusion, swallowing, or aspiration ruled out. These conditions can be distinguished by history and physical as well as by imaging modalities.
Prognosis
A study published by Karayilmaz et al., examining the long-term prognosis of avulsed teeth, concluded that the replantation of avulsed teeth is a highly successful procedure. However, the long and short-term prognosis is strongly affected by the dry time. In another study, the long-term survival of replanted avulsed teeth was only 20%, which was attributed to the lack of follow-up treatment.[17]
Complications
The major complications secondary to replantation of avulsed teeth include infections, tooth discolorations, fistulas, inflammatory root resorption, ankylosis of the root to the alveolus, apical periodontitis, pulp canal obliteration (PCO), and pulp necrosis (ultimately leading to tooth loss).
Resorption and ankylosis are associated more with the use of rigid splints as opposed to semi-rigid ones. Ankylosis can be especially problematic in young patients going through the facial growing phase as the surrounding structures will continue to develop, and the tooth will look submerged.
Tooth avulsion is associated with a high risk of loss of vitality, especially if the apex has completely developed. This may eventuate in pulp necrosis and inflammatory resorption of the root. If this goes unrecognized, periapical periodontitis may develop and can complicate the healing process and prognosis. Pulp canal obliteration is apparent weeks to months after replantation and is heralded by radiographic density in the pulp chamber and canal. Although it is thought to be a concomitant of healthy revascularization of the injured neurovascular bundles, approximately 15-25% of teeth with pulp canal obliteration develop pulp necrosis.[2][19]
Deterrence and Patient Education
Coaches, recreational leaders, and first responders should all know the initial management of an avulsed tooth. Patient and parental education and the early seeking of medical care can improve the prognosis and success of treatment. Using the right protective mouthguards in high-risk contact sports can reduce the incidence of potential injury.
Pearls and Other Issues
Tetanus immunization should be updated if necessary after tooth avulsion.
Dental follow-up is mandatory for further treatment after replantation.
Brushing teeth after every meal and using chlorhexidine 0.12% rinse twice daily can decrease infection rates.
Patients should be placed on a soft to chew diet for at least two weeks following tooth avulsion.
The success of replantation of the tooth is difficult to predict, and the patient and family should be warned that dental root resorption and tooth loss are possible.[20]
Enhancing Healthcare Team Outcomes
An avulsion is a rare type of dental trauma, emphasizing the need for professionals to regularly review the treatment protocols to increase a successful outcome. Keeping in mind that the treatment aims to maintain the tooth and bone until complete facial growth is achieved. The need for early replantation and the appropriate storage medium is less recognized by patients, parents, and medical professionals. It is necessary for primary care providers, nurse practitioners, and the general dentist to educate the public regarding the prognosis and success of replantation, how early treatment is essential, and that the preferred storage medium is a balanced salt solution or milk.